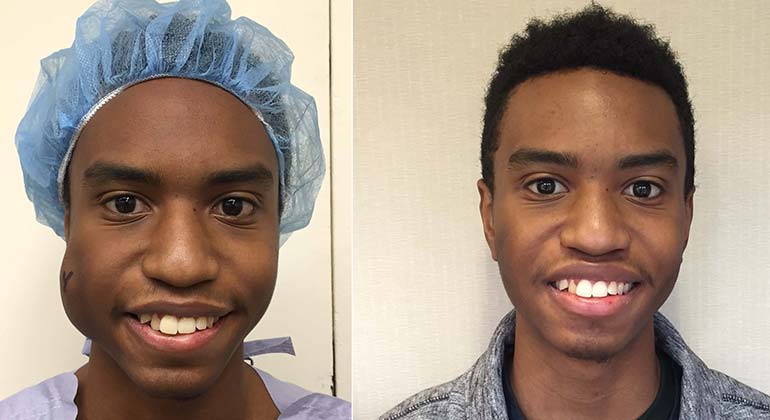
Venous Malformation: A Life-Changing Surgery
For 16-year-old Ethan Garcia, it all started in October 2013, when his mother noticed a growth the size of a golf ball protruding from his right cheek. Thinking it was a tooth abscess, Ethan’s mom took him to a dentist, who prescribed an antibiotic to cure what she thought was an infection in Ethan’s saliva glands. Although the swelling initially went away, it returned a few weeks later and would not respond to any further treatments with antibiotics prescribed by Ethan’s pediatrician. In fact, the medication only made it worse.
The doctors at Ethan’s local hospital concluded that his condition was probably caused by a muscle mass or a mass of veins and referred Ethan to an ENT specialist for further testing. Ethan ended up going to several ENT specialists. Given Ethan’s unusual condition, some of the specialists were unsure about its cause, while others were unwilling to take on such a difficult and complicated surgical case. In the end, Ethan was told that he should just watch it for now, as the risk of surgery outweighed the benefits.
“From January to December of 2014, my family and I were stagnant. It was so frustrating because we didn’t know which doctor to go to,” Ethan recalls, adding that the swelling typically flared up in the morning, and although ice helped, eating was painful. “My friends would ask why my cheek was swollen; I wouldn’t know what to tell them because I didn’t know what it was. I didn’t want anybody to look at me because I felt that my face looked deformed and uneven.”
Ethan and his family continued their search for the right specialist with the experience to treat his case. Finally, in the fall of 2015, he was referred to Gregory Levitin, MD, Director of Vascular Birthmarks and Malformations for the Mount Sinai Health System.
“Reviewing Ethan’s MRI, I recognized the problem right away,” Dr. Levitin says. “It was an extensive lympho-venous malformation of the right midface that by this point had gotten quite large. Only a surgical intervention would help Ethan.”
Dr. Levitin operated on Ethan in December 2015 at New York Eye and Ear Infirmary of Mount Sinai. The operation lasted almost five hours but was a success.
“Ethan’s condition had progressed to the point where the malformation was putting pressure on the facial nerve branches that control the face,” Dr. Levitin says. “I knew going in that this would be a challenging case, especially with the risk of bleeding, so we made sure to take our time separating the normal tissue from the vascular malformation.”
The surgical procedure was unique in its use of intraoperative facial-nerve monitoring, a state-of-the-art technique that provides real-time assessment of the facial-nerve function throughout the operation, even alerting surgeons to any stretch or compression from tissues nearby.
“In the past, we would advise patients that the surgical risk to the facial nerve was up to 50 percent, leading some patients not even to consider surgery,” Dr. Levitin adds. “Using this technique, I can confidently remove these types of lesions with less than one percent risk of injury to the nerve. This was the case for Ethan: after five hours, we got it just right.”
“When I awoke after surgery I was in so much pain but saw a beautiful sight: my family, the nurses, and Dr. Levitin,” Ethan recalls. “After the surgery I felt a resurgence of confidence inside me. And when I resumed classes for the spring semester, my friends noticed that my lump was gone and my face was symmetrical again. Today, looking into the mirror, I feel completely normal, as if I never had the surgery.”