Big Data Reaps Big Rewards in Drug Safety
Systems biology approach suggests existing drugs could be combined to reduce adverse effects.
Using the Food and Drug Administration’s Adverse Event Reporting System (FAERS), a hospital electronic health records database, and an animal model, a team of researchers at the Icahn School of Medicine at Mount Sinai report that by adding a second drug to the diabetes drug rosiglitazone, adverse events dropped enormously. That suggests that drugs could be repurposed to improve drug safety, including lowering the risk of heart attacks.
The research is published online October 9 in the journal Science Translational Medicine.
The approach is part of an emerging strategy known as systems pharmacology that integrates computer science, mathematical models, and animal models to examine how drugs work in cells. Systems pharmacology shows that most drugs act by binding to targets that are part of complex networks within cells.
"Big data systems have a wealth of data, and when studied appropriately, can point to potentially safer combinations," said the study’s lead author, Ravi Iyengar PhD, Dorothy H. and Lewis Rosenstiel Professor, Department of Pharmacology and Systems Therapeutics, and Director, Systems Biology Center, at the Icahn School of Medicine at Mount Sinai. "As an end in themselves, big data analyses must be considered preliminary, but findings can point to potentially safer combinations that can subsequently be tested in clinical trial," said Dr. Iyengar. "We may be able to use FDA-approved drugs to prevent adverse events."
In this study, investigators studied how drug combinations act through networks within cells, focusing on the diabetes drug rosiglitazone, an effective drug in controlling blood glucose. However, rosiglitazone has a serious side effect, increased heart attacks, which has restricted its use markedly.
Since most patients with diabetes take more than one drug and the FDA Adverse Event Reporting System (FDAERS) is freely available, investigators analyzed data from the FDAERS to see if second drugs could lower the rate heart attacks. In addition, investigators compared their results with Mount Sinai’s electronic health records system.
Compared with many other commonly used second drugs, "we found that the drug exanatide, often given along with rosiglitazone to get better control of blood glucose, also very substantially reduced the heart attack rate in rosiglitazone users," said Dr. Iyengar. Using these findings, the investigators made some predictions of how these beneficial drug interactions might work in diabetic mice, finding that the heart attack rate declined.
"The beneficial effects of rosiglitazone and exanatide are not unique," explained Dr. Iyengar. "We found nearly 19,000 other drug combinations in the FDA database, where the second drug appears to reduce a wide range of side effects of the first drug. Other beneficial effects were demonstrated when lisinopril was added to a statin, where the rate of statin-associated rhabdomylosis, a kind of muscle tissue wasting, declined; when an H2 antagonist was added to SSRIs, it reduced completed suicide.
The research team stressed that the results are a valid starting point for developing clinical trials of safer drug combinations. To further drug safety, they urge researchers and clinicians to contribute to big databases, such as the Food and Drug Administration’s Adverse Event Reporting System.
The research was supported by the National Institute of General Medical Sciences: NIGMS (grants GM071558, and GM 007280) of the National Institutes of Health.
Co-authors include Evren U. Azeloglu, PhD, Juan J. Badimon, PhD, Ludovic Benard, PhD, Yibang Chen, PhD, Chiara Giannarelli, MD/PhD, Joseph Goldfarb, PhD, Omri Gottesman, PhD, Roger J. Hajjar, MD/PhD, Mohammad U. Zafar, MD, and Shan Zhao, PhD from the Icahn School of Medicine at Mount Sinai; and Tomohiro Nishimura, PhD, from Keio University, Tokyo, Japan.
About the Systems Biology Center New York
Systems Biology Center New York is a trans-disciplinary center that uses systems approaches to study pathophysiological processes and drug action at Mount Sinai, a National Institute of General Medical Sciences National Center for Systems Biology. We are a highly collaborative group of researchers both basic and clinical, and educators from several universities in the New York area. Center investigators have expertise in genomics, biochemistry and molecular biology, proteomics, in cell biology and visualization of signaling reactions live cells, in tissue/organ physiology and pathophysiology, clinical imaging and in pharmacology. At the computational level we have expertise in statistical models, graph-theory network based analyses, mathematical biology and dynamical modeling including ODE, PDE and stochastic models. Melding the expertise of various disciplines, we work at various scales of biological organization to make substantive contributions to the emerging fields of systems pharmacology and precision medicine.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
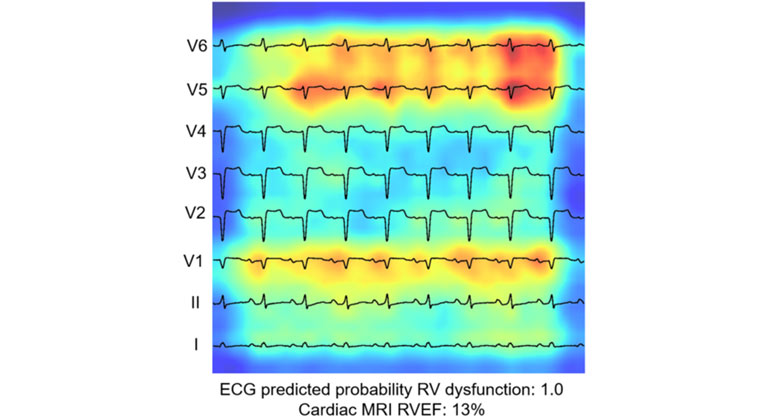
AI-Driven Study Redefines Right Heart Health Assessment With Novel Predictive Model
Jan 04, 2024 View All Press Releases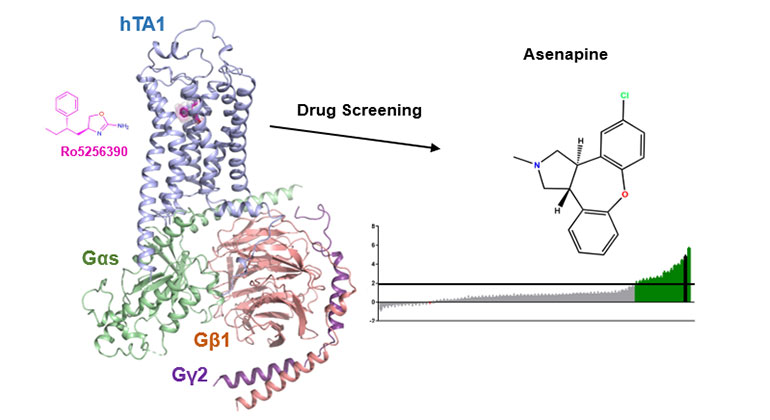
Demystifying a Key Receptor in Substance Use and Neuropsychiatric Disorders
Jan 02, 2024 View All Press Releases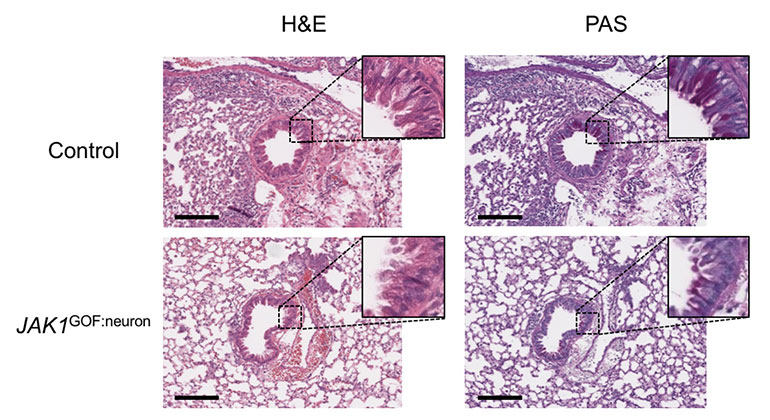
New Insights Revealed On Tissue-Dependent Roles of JAK Signaling in Inflammation
Dec 21, 2023 View All Press Releases