
Calm Through Chaos
Date Published: April 1, 2020
Jessica Montanaro, MSN, RN, Assistant Nursing Care Coordinator, Surgical Trauma ICU, Mount Sinai Morningside, describes what it's like to treat COVID-19 patients, and explains how nurses and colleagues in her unit are banding together to meet an unprecedented challenge.

Jessica Montanaro, MSN, RN, with a team of nurses at Mount Sinai Morningside.

Jessica Montanaro, MSN, RN, ICU Nurse at Mount Sinai Morningside.
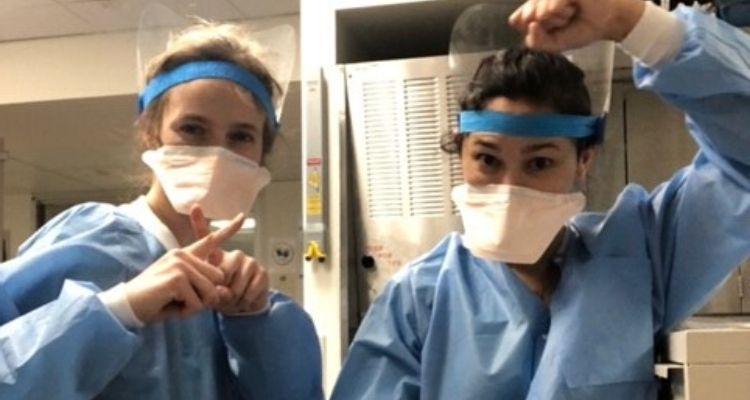
Nurses at Mount Sinai Morningside.
Podcast Transcript
Host: 00:00
From the Mount Sinai Health System in New York City, this is Road to Resilience. I'm Jon Earle. Each episode we bring you interviews with resilient people and scientists who study resilience. This is our second episode on resilience during the coronavirus pandemic. It's an interview with an ICU nurse at one of Mount Sinai's Manhattan hospitals. Before this interview, I knew intellectually that frontline workers are heroes in this fight. But until I spoke to Jessica Montanaro, I didn't feel it. Listening to Jessica helped me feel the viciousness of the disease. It helped me feel the sacrifices that frontline workers are making. And it helped me feel the incredible bonds between people in the trenches, bonds that are helping them cope. I think you're going to feel the same way. Jessica, thank you so much for making the time to talk to us. We really appreciate it.
Jessica Montanaro: 00:52
Thank you for having me.
Host: 00:54
So I understand you've been a nurse for a long time. Can you just tell us a little bit about your background?
Jessica Montanaro: 00:58
Yeah, so I've been a nurse for 18 years and all of my work has been in the hospital. I've always had secondary jobs, maybe teaching or in other facilities, but my primary main job has always been in the hospital as a nurse.
Host: 01:14
You've been a nurse with some of the sickest patients, right? In the surgical intensive care unit and medical intensive care unit. Is that correct?
Jessica Montanaro: 01:23
Yes, when I started my career, I started in telemetry nursing, on a regular telemetry floor--
Host: 01:31
And what is that?
Jessica Montanaro: 01:32
So that's where you monitor patients with cardiac issues and heart rhythms, et cetera. And then I moved into oncology nursing and from there I've spent the last eight years in critical care.
Host: 01:47
The picture I have in my head is of you racing around putting out fires, saving lives all day. Is that accurate?
Jessica Montanaro: 01:57
Yeah, I would say--I mean, I'm not going to say that every day looks like that. I will tell you every day since coronavirus looks like that. But, I think particularly because of the type of unit we are and the types of patients we get, especially in a New York City trauma ICU. We can be very, very busy. Are there days where maybe we don't get admissions and we have, you know, our patients and we're managing it. Yeah, of course.
Host: 02:27
Tell me about how coronavirus has changed your work.
Jessica Montanaro: 02:33
If I had to tell you that when it first started last week, my answer would have been very different than what I will probably answer for you today, because I think with this--it is changing on not even just a daily basis, but on more of a maybe even hourly basis. I actually just got done saying last night to my husband when I was coming home from my shift that I don't know how this will not change the nurses and the physicians that I'm working with forever. It is something I've never seen before. It is an intensity level and a stress level that I've never experienced nor have a lot of my colleagues that I've worked with. I've been asking them, and a lot of them have been in critical care for up to 20 plus years.
Host: 03:23
What explains that intensity?
Jessica Montanaro: 03:26
So I think it is number one, the amount of critical care patients that we're getting. So we're a 24-bed unit. So even though we might be full, and that's not always the case, let's say we had 24 patients in the ICU prior to corona. Not all of them will be intubated and requiring that almost one-to-one type nursing to keep them alive. And that's what I'm finding is happening with this. Is that we are full, everyone is on a ventilator, everyone is requiring four to five critical-care drips that need to be managed sometimes minute by minute. And the second thing is that these patients are decompensating so fast.
Host: 03:12
They're deteriorating.
Jessica Montanaro: 04:13
Deteriorating, decompensating. One minute they can be okay. And then out of the blue, another minute they are requiring emergency, life-sustaining interventions. So they're changing very fast. You know, we have a very big unit physically, and I feel like when I'm standing in the hallway, you can see all the way down between all our whole unit. It's very large, and I'll be standing at one end and then I see 10 people running to a room on the other end. And we're running down there and we just get that taken care of, and then you see 10 more people going a different direction to another room. And then we're running over there to see what's going on. So it's been that type of environment, I would say.
Host: 04:56
That sounds incredibly stressful. I can't even imagine.
Jessica Montanaro: 05:00
Yeah, absolutely.
Host: 05:03
Tell me about your first COVID patient.
Jessica Montanaro: 05:05
The first patient that we actually had when I came onto a shift was intubated and then we got our second patient actually of that day. And when he came into us from the floor, he was on the floor, COVID-positive, sick, and he was screened into the ICU because they were concerned about his breathing. And he looked terrified. And he would call me by name. He would say, "Jessica, are you done taking my blood?" And, "That's a lot of blood you're taking." He would say, "Jessica, are you going to help me breathe? I can't breathe." And while I was taking care of him in that room, he received a phone call from his daughter, who was in her 20s, who was calling to confirm to him that she had just tested positive. And so not only was he now concerned for his breathing and what was happening to him, but you could just see this whole wave of worry that just came over him now for his daughter. We got him settled, and I made sure his cell phone was hooked up right next to him and that he had it so he could talk to his family. And he just touched my heart in a way, because he was scared and he was talking to me. And when I came in the next day for my shift, he was intubated because he obviously decompensated with his breathing and he required a breathing tube. And he was on, like, four critical care drips and he just broke my heart because he changed so fast.
Host: 06:39
I guess I want to pivot now to how you and your staff are doing. I know there are many aspects of that. One of them was the feeling of being around COVID patients. And you told me that the first time that you were in a room with a COVID patient was kind of a unique experience. Can you share that?
Jessica Montanaro: 07:02
I would say that my staff and I—it's not new for us to care for patients who are requiring high levels of respiratory isolation for various diseases. But for me, personally, when I went into that room, I had my PPE on and we closed the door and it became very real. It became very, like, "Wow, this is a virus that we don't know anything about that I could contract." And it became very real and it's almost surreal. And I think obviously now where we are going from having two to having 24, being in and out of these rooms—it becomes surreal. But it's almost becoming, like, normal putting on this PPE and taking it off and going in and out of these rooms. And sometimes you just stop and you realize what you're dealing with and it's immobilizing for a few minutes, but you have to keep moving.
Host: 08:00
Is it okay if I ask you about your colleague who passed and how you responded to that?
Jessica Montanaro: 08:08
Yeah. Yesterday was a tough day. We had to send one of our top leadership physicians home who was sick. And then we got notified that one of our colleagues at our sister hospital, at Mount Sinai West, who was in his forties, who was a manager actively taking care of these patients to assist his staff, had died on a ventilator due to corona. And it was devastating. I think it stopped us in our tracks. The nurses, I guess, were notified on Facebook or something. And so they started sending it out. And as we were receiving this notification that this happened, one of the nurses came to me and said, "We have to gather together." And so we stopped around mid-afternoon and we gathered the entire team and we recognized this heroic nurse who lost his life. And we had a moment of silence for him in our unit. I don't think anybody was right after that to be honest with you.
Host: 09:14
You mean that they were shaken?
Jessica Montanaro: 09:17
Yeah, it just—it sends it home in a very real way, into a surreal world that we're living in. That our colleagues are being sent home sick and that they're dying now and we are in the middle of it. I likened it to a war last night to someone I was speaking to. I actually, I try to be strong because I also am the clinical leader of the unit and I need to make sure that my nurses are okay. So I often check in with them, and we're handing out water and we're doing "emotional temperature checks," if you will. I had a nurse who had a full-on panic attack the day before, and I just sat her in the office and I let her leave the floor for about an hour and a half, and we had her patients covered. And we're checking in with each other. And so yesterday when that happens, after our moment of silence, I actually sent a text out to one of our fellows who I'm close with who has been struggling with this. And actually my text said, "I need a pep talk." And he's the one that actually likened it to a war. He's like, "It's like when you're in war, in the trenches, next to your buddy, and you see them, you know, die next to you." That's what he was likening it to. But we're just kind of leaning on each other right now.
Host: 10:38
Did that help you, that metaphor?
Jessica Montanaro: 10:42
I think it just is the reality of what it is. I think what helped me was that he can relate. And that nobody's sugarcoating anything among each other, which is good. You know, we're trying to stay positive, but we're also trying to acknowledge the realism of what's happening in a very surreal kind of environment right now. And so I appreciated that he didn't just say, "Oh, it's all gonna be okay." You know, he was, he could just relate to me on a very real level and put it in that metaphor for me.
Host: 11:14
You mentioned earlier that you felt like this experience is changing everybody in an indelible way.
Jessica Montanaro: 11:22
Oh, for sure. I guess what I mean is, if you go into critical-care nursing, you are going into it expecting that you're gonna see deaths, that you're going to see critical illness, you're going to see things, especially in a trauma ICU where we work. Trust me, I have seen my fair share of horrible, sad, sad, sad, sad things. And I'm seeing nurses who have seen all that stuff have to really stop and emotionally take a minute or 30, who are just finding their own coping mechanisms to get through this because the amount of patients we're seeing at the same time, the amount of critical illness and the amount of decompensation is just something that we don't get inundated with all at the same time at once. It's like—we train in our ICU, like most ICUs do, but especially in New York City, for mass casualty incidents, right? So with a mass casualty incident, you would expect that, okay, this horrible event happens and you get maybe 20 plus patients, but, okay, now we figure out what to do with them and we go through a short period of intensity and then we start to figure this out. And it might be horrible. But with this, there's no end in sight. They keep showing up, they keep decompensating, there's emergencies being called overhead constantly. There's intubations happening all over the place. If one patient is passing away, there's another one waiting to fill the bed. And so that's the part that's not, it's not stopping.
Host: 13:00
What are the coping mechanisms that you're using and that your colleagues are using?
Jessica Montanaro: 13:05
I know that nurses are just eating for a few minutes and kind of taking that few minutes or pulling their colleagues aside and saying, "Hey, just checking in. You okay? Do you need anything?" I know that for me, I'm on several text-thread messages with my staff, and we just kind of let it all out there. Whether we're happy or sad or we're angry or, whatever the emotion is. And I was pretty angry the other night when I came home. And I just was kind of sharing my anger in this group. And the messages that I was receiving back from my friends who were in my unit was just, "Vent away. We're here. Just say it." And I'm just being allowed to express what we have to and say what we have to.
Host: 13:53
There's something else you said when we last spoke that helped me to put everything into context but also kind of gave me hope, and it was the mantra that you use.
Jessica Montanaro: 14:04
Actually I got it from my sister. We were on a text thread and I was just expressing to my family how serious this is and what we're going through inside. I call it, "a look on the inside." And my sister was like, "Calm through chaos." And I was like, "Oh, I like that. Calm through chaos." And so I kinda tried to make that my mantra and I shared that with my staff in an email. Calm through chaos. That was last week. I'm not saying that it doesn't hold true today. But I will tell you that on my way into work, I often try to listen to some positive affirmations and I'll say that to myself. And I have every single intention of living that when I get into work. But when I get there, it's so chaotic, the level of stress. You just walk in and it hits you in the face. It's hard to not get swept up by that. So maybe midday I'll look at one of my colleagues and I'll be like, "Okay, I'm regrouping internally," and I'll say that to myself, "calm through chaos." I probably should put a sign up in the unit somewhere that says that, "calm through chaos."
Host: 15:09
Jessica, when you look to the future right now, what do you see?
Jessica Montanaro: 15:13
Honestly, right now I don't see an end. I can't see the end where we come through this, not to say we won't come through it, but in the beginning I think I was saying more like, "We'll get through this." And we will. But right now I don't see what that end looks like because just yesterday there were discussions happening about how we were going to double up our rooms and put two critically ill patients in one room on one ventilator. So that's where I think we're still at. We're definitely not talking about a resolution. We're not talking about an ending. So I don't know how I can answer that other than right now we're just in the middle of it.
Host: 15:51
Jessica, I really can't thank you enough. This has been so eye-opening and so powerful, and I'm just in awe of you guys. I know "thank you" isn't enough. And I know you have a weird relationship to hearing people say "thank you" right now—
Jessica Montanaro: 16:02
I really do! It's so weird. It's like, I appreciate it, and I know we appreciate it, but it's almost like this is what we were born to do. I think I said to you before, like, when I describe who I am, I'm a mother, I'm a wife and I'm a nurse. And nursing isn't something I do; it's part of who I am. So to me, this is just my calling. So when people say "thank you," it's obviously appreciated, but it's awkward because this is what my calling is and I was destined to give this away to people. And I just wanted to say that this is not an individual "me." I'm trying to bring the experiences and the voices of my amazing, awesome comrades, who are working alongside me. Because without them I wouldn't be where I am right now. So we are definitely a team. So I know you're hearing my voice, but this is really about the team right now.
Host: 16:50
Thank you. Thank you for telling us that. And thank you for your work. And thank you for this interview. And please enjoy—I know this is your day off—please enjoy the rest of your day off. Thanks for giving us some of your time.
Jessica Montanaro: 17:03
Thank you very much. Thank you all.
Host: 17:07
Jessica Montanaro is an assistant nursing care coordinator at Mount Sinai Morningside. Road to Resilience is a production of the Mount Sinai Health System in New York City. It's produced by Katie Ullman, Ncci Hudson and me, Jon Earle. Lucia Lee is our Executive Producer. If you enjoy this episode, please leave us a rating and a review on Apple podcasts or wherever you're listening. It helps other people find the show and keeps us resilient. Thanks. That's all for this episode. Thanks so much for listening. We'll be back with more soon and until then, stay safe and be well.
