Mary: Autopsies Save Lives
Date Published: January 13, 2020
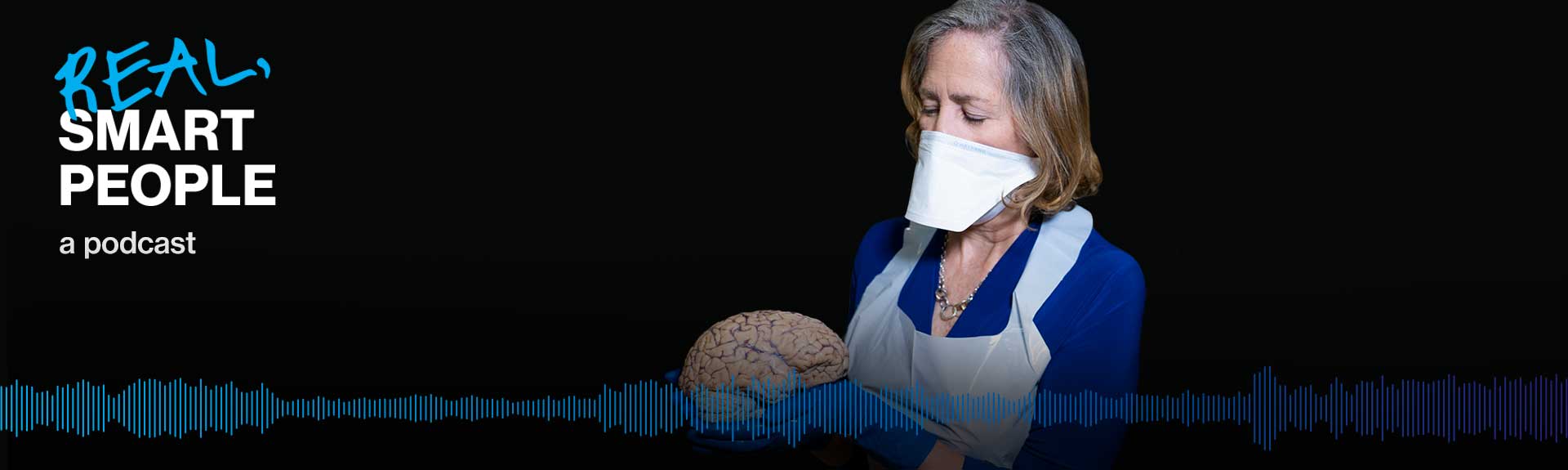
Neuropathologist Mary Fowkes, MD, PhD, on what she learned about COVID-19 from performing autopsies on pandemic victims.
Early in the pandemic, when little was known about the SARS-CoV-2 virus, neuropathologist Mary Fowkes, MD, PhD, volunteered to perform autopsies on COVID-19 victims. Wearing a full-body protective suit and often working alone, she painstakingly examined the virus’s impact on the brain. What she and her team found shocked her—significant blood clots in the brain and vital organs. The discovery led to the increased use of blood thinners in COVID-19 patients.
Dr. Fowkes died on Nov. 15, 2020 of an acute heart attack. An autopsy did not reveal the presence of COVID-19.

Dr. Fowkes in a pressurized air purifying respirator (PAPR) suit to perform autopsies.


Podcast Transcript
Dr. Fowkes: 00:00
I love to hike. I love to be outdoors. I love animals. I love to fish. I absolutely love to fish. I'll get up at any time in the morning—I'd get up in the middle of the night to go fishing. It's kind of like the autopsy stuff. I don't know. I just find it really exciting.
I'm Dr. Mary Fowkes. I'm Director of the Neuropathology Division, as well as the Autopsy Service here at the Icahn School of Medicine.
I have always been good at dissecting things from even when I was little. I've always been the one that filleted the fish and was the go-to person—if there was a medical, an animal that was hurt, I was the go-to person to bring the animal to. Oh, and my grandmother had a stuffed skunk in her attic. And I just thought that was the coolest thing. So that probably started me on the path. Pathology is like being a detective. You can investigate what's going on with the patient. And we have the gold standard of diagnosis. We have the best answer for trying to help the patient. And I like that. I like being able to help patients.
So now we're in the basement of the hospital. Most morgues or autopsy suites are in the basement, just by convention.
Producer: 01:29
Why is that?
Dr. Fowkes: 01:30
They get us out of the way. So this patient had a prior stroke affecting the right frontal lobe and right temporal lobe. So we're going to cut it and see if we can identify evidence of the stroke. Sometimes people have a hard time dealing with things that are not what they expect. So just leave the room, sit down, collect yourself. Nothing to be ashamed of. But I don't want people passing out.
People have this perception that it's gory and bloody. And it's how it's portrayed on TV, in some horror movie, you know, blood shooting everywhere. And it's not like that. And in most instances, if you talk to families and you explain to them that an autopsy is done very carefully with surgical-like incisions, and we can sometimes provide important information for families relating to inheritable diseases, patients usually want to have an autopsy.
Okay so I'm going to cut this. If you approach things systematically, look at the vessels, you look at the cranial nerves, and try not to focus on lesions that you immediately see when you cut the brain. So your eye is drawn to things that are interesting, but you have to systematically look at everything so that you don't miss things.
I've always thought that autopsies were important, but then when COVID hit, it just hit me so hard how important they can be. I was one of four pathologists here at Mount Sinai that were willing to volunteer to do the COVID autopsies, despite the risk. I didn't tell my kids. My daughter didn't know until one of my colleagues posted a picture of me in a full PAPR. I told my kids I wasn't doing autopsies. I wasn't doing the general autopsy, I was just doing the brains. So I felt like I kind of wasn't totally lying.
The first time that I did a COVID autopsy, I learned very quickly that you have to go slow and calm when you're working with a PAPR. It's like a space suit. You're not gonna breathe what's in the room. You're gonna only breathe what's gone through the machine. But I had one incident where it started going off in the middle of doing the brain removals. "Beep beep beep beep." And then if it continues to not be working properly, where the air is not coming into the hood properly or into the suit properly, it has a continuous beep, "Bzzz." That's when I really started getting nervous. Then I realized, yes, I can still breathe. Does that mean that it's not protecting me from the air that's in the room? So I finished the work that I was doing. I waited the 15 minutes. I took off the hood and then I went home and see if you come down with symptoms.
We did a total of 102 COVID cases and we've done at least four more now that are post-COVID. We found that the lungs were severely affected and we found blood clots throughout the body, but most importantly within the brain. So patients with strokes. That was shocking. And we made sure that the clinical team here at Mount Sinai was aware that concern about blood clots needed to be followed in these COVID patients. I'm really not that talented. I'm not that smart. I have my faults. But I work really, really hard and I pull it off.
So I am seeing some changes here. There's a stroke in the right side of the brain. It's an area of gray discoloration, softening, and it's knocking out portions of the white matter. It's about maybe two centimeters front to back in measurement. So it's a pretty big stroke.
I think that autopsies are phenomenal. I don't understand why more clinicians don't push for them. We've had people say, "We didn't want to put the patient through an autopsy." Well, the patient's dead. The autopsy's gonna help the living. It's the last gift that a patient can give to their family. And it makes the family feel better most of the time. It provides this little glimmer of good out of something that is really hard. So, if I had a billboard in Times Square, I would put, "Autopsies save lives." Because they do.
Dr. Carlos Cordon-Cardo: 06:56
One, two, three. I'm Carlos Cordon-Cardo. I'm the Professor and Chair of the Department of Pathology at the Icahn School of Medicine at Mount Sinai. We are saddened and shocked by the passing of our esteemed and beloved colleague Mary Fowkes, who passed peacefully at her home of an acute heart attack. The autopsy didn't reveal any COVID disease. She was truly heroic in her efforts during COVID-19, where the findings from autopsy changed clinical care at Mount Sinai with national and international repercussions during the first surge of 2020. She was cherished by the residents, fellows, staff, and all faculty members. A friend to all, she was always helping others and always with a smile. We will miss her teaching, her brilliance and great sense of humor. We will miss her gentle character. We will miss an outstanding colleague and mentor. We will miss a friend.
