Gene Therapy Halts Progression of Pulmonary Hypertension in a Large Animal Pre-Clinical Study
Scientists have used a novel gene therapy to halt the progression of pulmonary hypertension, a form of high blood pressure in the lung blood vessels that is linked to heart failure, according to a study led by Roger J. Hajjar, MD, Professor of Medicine and Director of the Cardiovascular Research Center at the Icahn School of Medicine at Mount Sinai. The study was published online this week, and will appear in the May 3 issue of the Journal of the American College of Cardiology (JACC).
Pulmonary arterial hypertension (PAH) is a rare, rapidly progressing disease that occurs when blood pressure is too high in vessels leading from the heart to the lungs. There is currently no cure for PAH, and about 50 percent of people who are diagnosed will die from the disease within five years. The high pressure is caused by abnormal remodeling of the lung blood vessels that sometimes leads to failure of the right ventricle and premature death. Thickening and narrowing of pulmonary vessels is seen with all types of pulmonary hypertension and is triggered by abnormal calcium levels within the vascular cells. The sarcoplasmic reticulum calcium ATPase pump (SERCA2a) regulates intracellular calcium in vascular cells and prevents them from proliferating in the vessel wall.
“There is considerable need for new treatments that improve functional capacity, symptoms, and survival,” said Dr. Hajjar. “This treatment with gene therapy offers a novel method of treating a deadly disease that disproportionately affects young adults and women,” he said. Female patients make up about 72 percent of the total population of patients with PAH.
“The therapeutic potential of using gene therapy to treat pulmonary hypertension by delivery of aerosolized adeno-associated virus carrying SERCA2a to directly target vascular remodeling through the overexpression of the SERCA2a protein is very significant,” said co-senior study author Jane A. Leopold, MD, of Brigham and Women’s Hospital, Harvard Medical School. “In addition, as other novel targets are identified by deep phenotyping of patients with pulmonary hypertension in the National Institutes of Health/National, Heart, Lung, & Blood Institute-funded Pulmonary Vascular Disease Phenomics (PVDOMICS) study, they may be viable candidates for aerosolized gene transfer using adeno-associated viral vectors.”
There were two primary objectives for this study, which was conducted by Mount Sinai and research teams from Brigham & Women’s Hospital in Boston, MA, and Centro Nacional de Investigaciones Cardiovasculares Carlos III in Madrid, Spain. First, scientists wanted to learn if it is feasible to deliver a therapeutic gene called SERCA2a in aerosol form to damaged blood vessels of the lung using an engineered adeno-associated virus as a “vector.” Second, they wanted to see if there was a sustained beneficial impact, and if the transferred genes effectively slowed or stopped the vascular changes in the airways that are the hallmark of PAH and other forms of pulmonary hypertension.
Previously, the novel aerosol inhalation technique used to deliver the SERCA2a gene in this study had proven effective in a rodent model. However, the current study is the first to explore this approach in a large animal—specifically, a Yorkshire swine model that closely resembles PH in humans.
In the study, 20 pigs were divided into two groups, half of which received the aerosolized viral vector carrying the SERCA2a gene and half a saline spray. Two months after the gene delivery, scientists performed tests to see if the new therapeutic genes were present and functioning in the vessels of the animals’ lungs, and whether the transfer was producing the desired effects. When they examined the animals, they found that that heart and lung function had improved and abnormal cellular changes causing PH were reduced.
“I’m excited that there is a potential new treatment for patients with this deadly disease,” Dr. Hajjar said. “By tailoring the gene therapy, it looks like we can halt the proliferation of smooth muscle cells in the blood vessels. This should help restore function and improve survival in human patients.”
Dr. Hajjar said that additional animal studies focusing on long-term efficacy and safety are warranted before advancing this approach, known as airway gene delivery, to human clinical trials. That’s because the current study involved a small number of animals, and they were assessed just eight weeks after gene delivery. Nevertheless, he said, airway gene delivery appears to modify fundamental pathophysiology, and therefore might offer therapeutic benefit to humans with a variety of pulmonary vascular diseases.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.
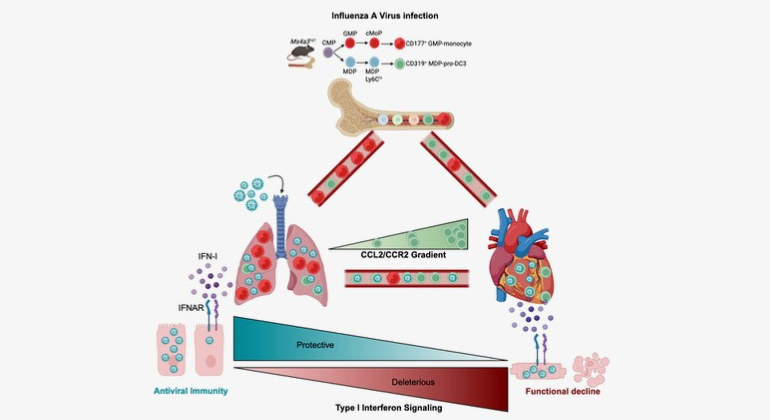
Mount Sinai Scientists Uncover Link Between Influenza and Heart Disease
Feb 09, 2026 View All Press Releases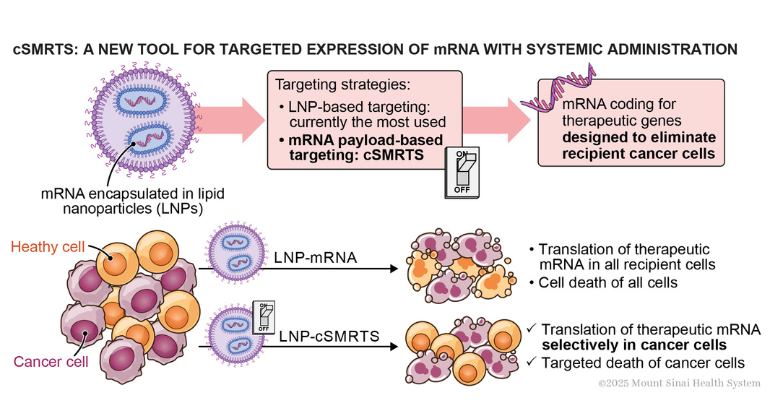
Scientists Develop a Smarter mRNA Therapy That Knows Which Cells to Target
Dec 15, 2025 View All Press Releases