Mount Sinai Study Identifies Inflammatory Immune Pathway Driving Immunotherapy Resistance in Bladder Cancer
Study published in Cancer Discovery shows how simple blood tests may reveal why some tumors resist immune checkpoint inhibitor treatment

Researchers at the Icahn School of Medicine at Mount Sinai and the Mount Sinai Tisch Cancer Center have discovered a biological pathway that helps explain why some bladder cancers do not respond well to immunotherapy. Their findings, published in Cancer Discovery (10.1158/2159-8290.CD-25-1774), show that common signs of inflammation in the blood are linked to immune cells inside tumors that block the body’s ability to fight cancer.
The work reveals a previously unrecognized link between systemic inflammation in the blood and immune suppression inside tumors. The study was led by Nina Bhardwaj, MD, PhD, Director of Immunotherapy and Ward-Coleman Chair in Cancer Research at the Icahn School of Medicine; Matthew Galsky, MD, Director of Genitourinary Medical Oncology and Deputy Director of the Mount Sinai Tisch Cancer Center; and Diego Chowell, PhD, Assistant Professor of Artificial Intelligence and Human Health, and Immunology and Immunotherapy, at the Icahn School of Medicine.
The study’s first co-authors are Michelle A. Tran, PhD, an MD/PhD student at the Icahn School of Medicine at Mount Sinai; and Mount Sinai researchers Byuri Angela Cho, PhD; Sudeh Izadmehr, PhD; and Seung-Keun Yoo, PhD.
Immunotherapy has improved care for many patients with bladder cancer. Still, doctors do not fully understand why some patients respond to treatment while others do not. High levels of C-reactive protein (CRP), an inflammation marker in the blood, have long been linked to worse outcomes, but the biological connection between inflammation in the blood and the tumor itself has remained unclear.
The researchers found that high levels of CRP and another blood inflammation marker, interleukin-6 (IL-6), are linked to a specific group of immune cells inside tumors. These immune cells, called SPP1+ macrophages, can shut down cancer-fighting T cells. When this happens, immunotherapy drugs known as immune checkpoint inhibitors may not work as well.
“Immune checkpoint inhibitors have changed how we treat bladder cancer, but many patients do not have long-lasting responses,” said Dr. Bhardwaj, who is also Professor of Medicine (Hematology and Medical Oncology), and Urology, at the Icahn School of Medicine at Mount Sinai. “We found that common blood markers like CRP and IL-6 are not just general signs of inflammation. They reflect a specific immune process inside the tumor that may block treatment.”
The Mount Sinai scientists analyzed bladder tumor samples using advanced genetic tools. They built the largest single-cell atlas of bladder tumors to date and combined it with RNA sequencing data from multiple groups of patients treated with immunotherapy.
The researchers found that tumors from patients with high levels of IL-6 in their blood were more likely to contain SPP1+ macrophages. Further analysis revealed that these macrophages suppress T cells in part through IL-6-related signaling pathways. In contrast, the team identified another type of macrophage marked by CXCL9 that helps activate T cells and is linked to stronger immune responses.
“Our study shows that systemic inflammation can provide insight into what is happening inside tumors,” said Dr. Chowell. “Inflammatory signals in the blood reflect specific immune programs that suppress T cells and limit the effectiveness of immunotherapy.”
By connecting systemic inflammation in the bloodstream with immune dysfunction inside tumors, the study may point to a promising target for future therapies that could block or reprogram these macrophages, restore immune activity, and expand the number of patients who benefit from immunotherapy in bladder cancer and potentially other inflammation-driven cancers.
“For clinicians, these results suggest that commonly used blood tests may provide insight into what is happening inside a patient’s tumor before treatment begins,” Dr. Galsky said. “This framework may help identify patients who are more likely to have resistance to immunotherapy and support testing new combination treatment strategies.”
The findings also provide support for ongoing and future clinical trials studying drugs that target IL-6 signaling and related inflammatory pathways alongside immunotherapy. For patients, the research helps explain why some bladder cancers do not respond well to immunotherapy.
The research team is now continuing to study SPP1+ macrophages to better understand how they suppress the immune system and how future therapies might target or reprogram them. The research was supported by National Institutes of Health R01 and F30 awards.
Full study and complete list of authors: https://aacrjournals.org/cancerdiscovery/article/doi/10.1158/2159-8290.CD-25-1774/774912/A-tumor-promoting-inflammatory-SPP1-macrophage-IL
About the Icahn School of Medicine at Mount Sinai
The Icahn School of Medicine at Mount Sinai is internationally renowned for its outstanding research, educational, and clinical care programs. It is the sole academic partner for the seven member hospitals* of the Mount Sinai Health System, one of the largest academic health systems in the United States, providing care to New York City’s large and diverse patient population.
The Icahn School of Medicine at Mount Sinai offers highly competitive MD, PhD, MD-PhD, and master’s degree programs, with enrollment of more than 1,200 students. It has the largest graduate medical education program in the country, with more than 2,700 clinical residents and fellows training throughout the Health System. Its Graduate School of Biomedical Sciences offers 13 degree-granting programs, conducts innovative basic and translational research, and trains more than 560 postdoctoral research fellows.
Ranked 11th nationwide in National Institutes of Health (NIH) funding, the Icahn School of Medicine at Mount Sinai is among the 99th percentile in research dollars per investigator according to the Association of American Medical Colleges. More than 4,500 scientists, educators, and clinicians work within and across dozens of academic departments and multidisciplinary institutes with an emphasis on translational research and therapeutics. Through Mount Sinai Innovation Partners (MSIP), the Health System facilitates the real-world application and commercialization of medical breakthroughs made at Mount Sinai.
-------------------------------------------------------
* Mount Sinai Health System member hospitals: The Mount Sinai Hospital; Mount Sinai Brooklyn; Mount Sinai Morningside; Mount Sinai Queens; Mount Sinai South Nassau; Mount Sinai West; and New York Eye and Ear Infirmary of Mount Sinai.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.

Mount Sinai Study May Help Cancer Patients Keep Their Bladder
Feb 19, 2026 View All Press Releases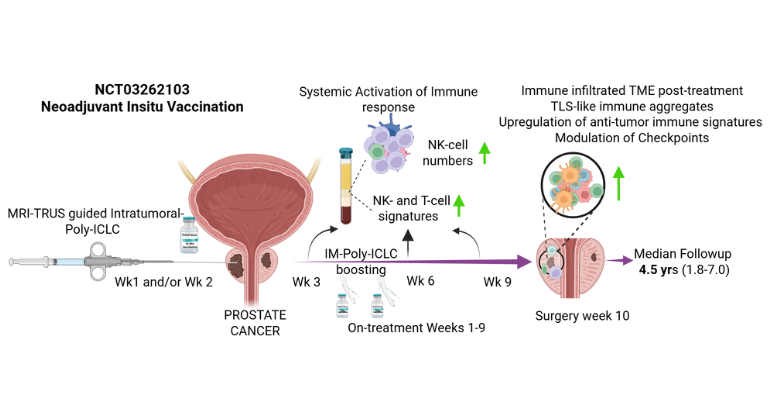
Early Clinical Trial Tests Immune-Boosting Therapy Before Prostate Cancer Surgery
Oct 30, 2025 View All Press Releases
Mount Sinai Researchers Engineer Rare Immune Cells to Create Powerful New Cancer Vaccine
Jul 21, 2025 View All Press Releases
Mount Sinai Study Advances Understanding of Personalized Vaccines for Bladder Cancer
May 12, 2025 View All Press Releases
Personalized Cancer Vaccine Proves Promising in a Phase 1 Trial at Mount Sinai
Mar 17, 2025 View All Press Releases
Mount Sinai Researchers Create AI Tool to Democratize Access to Cancer Immunotherapy
Jan 06, 2025 View All Press Releases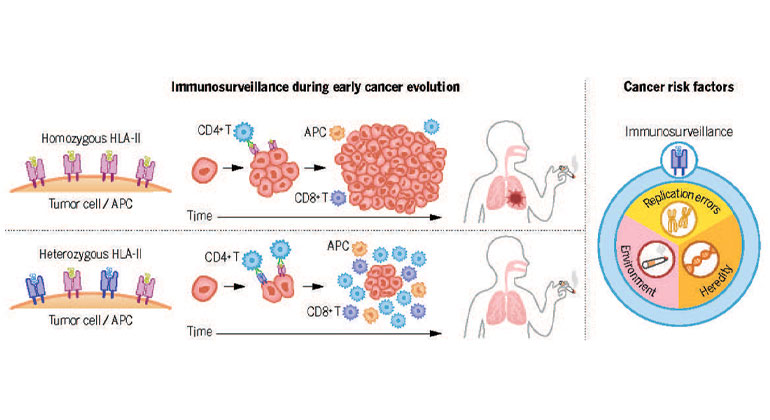
Study Reveals New Insights Into Immune System Role in Lung Cancer Risk
Feb 22, 2024 View All Press Releases
