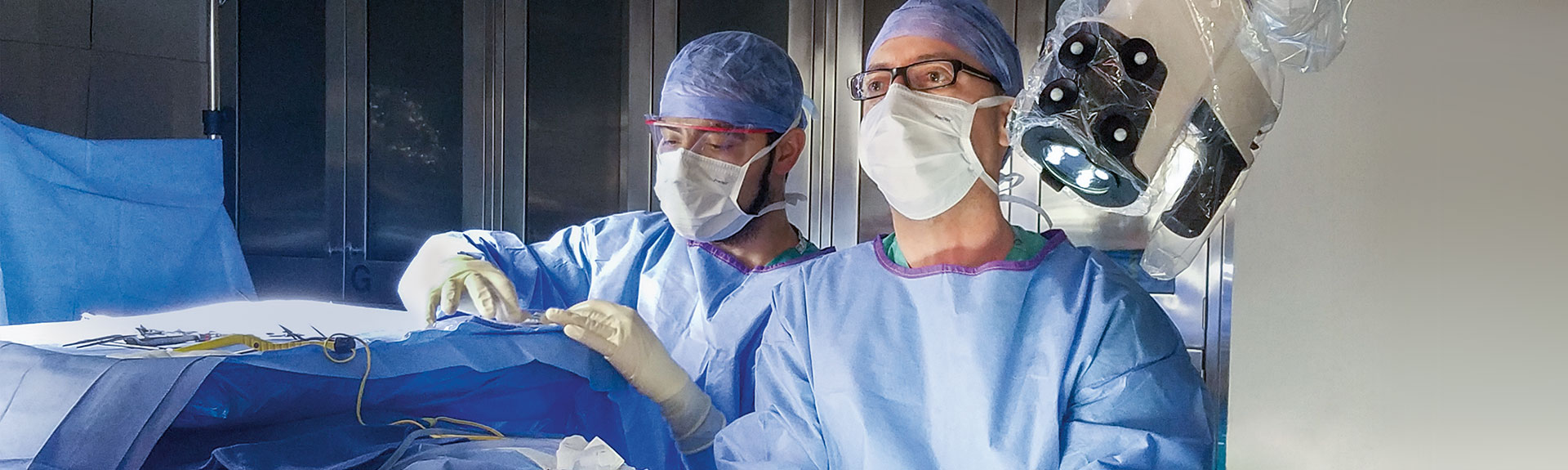
ENT/Head and Neck Surgery
Our Department of Otolaryngology–Head and Neck Surgery continues its innovative spirit in all facets of patient care, research, and education.
ENT-Head and Neck Surgery
Mount Sinai Health System’s Department of Otolaryngology–Head and Neck Surgery is internationally recognized for conservation laryngeal surgery, head and neck reconstruction, and accomplishments in the diagnosis and management of HPV-associated disease and robotic head and neck surgery.
This specialty report highlights:
- Surgeons perform the world’s first complete mastoidectomy with robotic arm technology
- The Quarterback Trial: Treating oropharynx cancer with reduced-dose chemoradiation
- SEES: A contemporary approach to the evaluation and management of dysphagia
- 3D printing and immersive simulation that improves surgical planning for skull base surgeries
- Using multilevel sectioning to detect lymph node metastases in papillary thyroid cancer patients
- Residency program receives top ranking
- Educating physicians in the virtual classroom
- Message from the Chair: Eric Genden, MD, FACS
Surgeons Perform World’s First Complete Mastoidectomy With Robotic Arm Technology
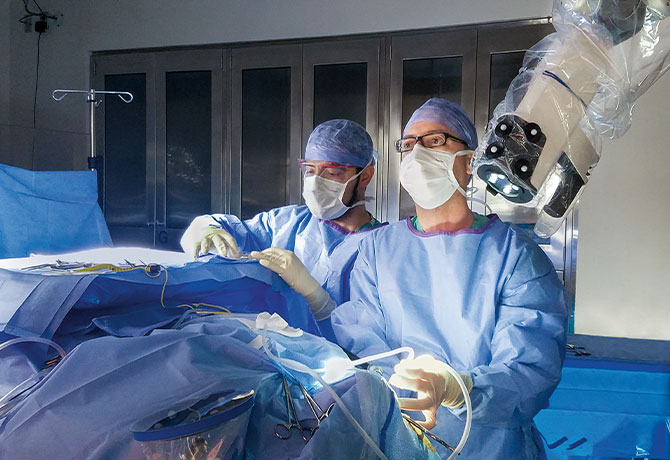
Skull base surgeons at the Mount Sinai Health System have performed the world’s first mastoidectomy using the Synaptive Medical Modus V, becoming some of the first in the nation to use the robotically controlled digital microscope for skull base surgery. Known as the exoscope, the device offers safe, high-resolution visualization, increased mobility and flexibility, and a compact design. George Wanna, MD, Professor and Site Chair of Otolaryngology – Head and Neck Surgery at Mount Sinai Downtown and Chief of Otology-Neurotology for the Mount Sinai Health System, recognized the vast benefits of using the device, as well as the advantages of scaling it to neurotology.
“The exoscope is a wonderful tool for multidisciplinary neurosurgery and neurotology surgeries,” says Dr. Wanna. “Performing a mastoidectomy with the exoscope allows great visualization of the anatomy and a unique opportunity for teaching and collaboration.”
The exoscope facilitates a multidisciplinary experience by allowing both neurosurgeons and ENTs to see high-quality images in real time and to be actively engaged during both the otolaryngology and neurology portions of surgery.
In addition to the mastoidectomy, surgeons at Mount Sinai have used the exoscope in multiple skull base cases, including vestibular schwannoma resections using suboccipital craniotomy and translabyrinthine approaches, temporal lobe encephalocele repairs, and superior canal dehiscence repair. No intraoperative complications were encountered and none of the procedures required abandonment of the exoscope. In April 2018, research from Mount Sinai’s initial case series was presented at the American Neurotology Society. Otology & Neurotology published an article detailing the case in its February 2019 issue. The findings presented the exoscope as a formidable alternative to the binocular operating microscope for lateral skull base procedures due to its ability to maximize visualization without compromising surgical exposure or patient safety.
“I believe this technology also has potential applications with anterior skull base cases,” says Dr. Wanna. “This is an exciting time in our field. I hope technological advances like this will optimize patient care and outcomes, which is our ultimate goal.”
Minimizing Surgeon Fatigue With the Exoscope
Complex lateral skull base surgery and otology procedures rely heavily on high-precision surgical techniques through a limited access point. Using the traditional binocular operative microscope, surgical techniques in neurotology became more sophisticated and successful for a wider range of procedures. However, use of these microscopes forces surgeons into ergonomically uncomfortable postures for several hours while operating through small “keyhole” corridors. Frequent periods of readjustments and refocusing are required, as the narrow depth of field can be quite limiting.
The introduction of the exoscope enriches the benefits of the microscope, but mitigates its limitations. In addition to heightened visualization, the exoscope’s longer focal length and compact configuration considerably increase the working space for surgeons and their instruments, along with providing improved ergonomics and increased degrees of freedom for adjustment while operating. Setup and mobility of the technology are swift, thus contributing to efficiency and a slight reduction of surgery duration. One limiting factor of the exoscope was decreased depth perception.
Elevating Academic Training Using the Exoscope
The exoscope projects real-time 3D rendering of the anatomy onto a large monitor. This enables pointing and visualization unmatched by the microscope, which has a limited view available only to the lead surgeon. Observers in the operating room have the same anatomical visualization as the lead surgeon, allowing residents to immediately familiarize themselves with the intricacies of each case type without awaiting the opportunity to be behind the microscope.
“This technology is a game changer for residency education with complex cases,” notes Jonathan Garneau, MD, Chief Resident, Otolaryngology – Head and Neck Surgery at The Mount Sinai Hospital. “I foresee this as an essential teaching tool in the future.”
The Quarterback Trial: Treating Oropharynx Cancer With Reduced-Dose Chemoradiation
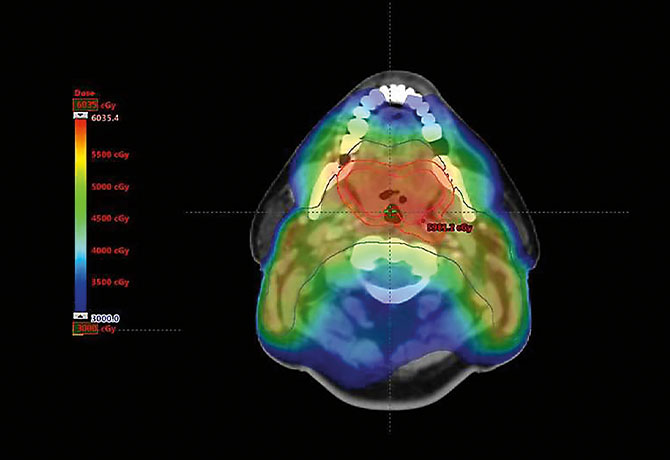
Physicians at the Head and Neck Cancer Research Program of the Icahn School of Medicine at Mount Sinai are conducting a broad clinical research study to create the safest and most effective therapy for patients with locally advanced HPV-positive oropharynx cancer (HPVOPC). This radical, multidisciplinary study aims to reduce short- and long-term side effects of radiation therapy in patients through the use of reduced-dose chemoradiation (rdCRT) after induction chemotherapy (IC). Participants receive approximately one-quarter less radiation than the average therapy dosage, earning the study the moniker the Quarterback Trial.
It is well established that locally advanced HPVOPC has a significantly better locoregional control and leads to better response and survival rates compared to non-HPVOPC after chemotherapy and radiotherapy. The Quarterback Trial compares rdCRT after IC to standard-dose chemoradiation (sdCRT) after IC in a 20-person randomized trial of volunteers with locally advanced HPVOPC. Each volunteer had a smoking history of less than 20 pack-years and had smoked less than one cigarette each day in the past five years. Participants were not eligible for Mount Sinai’s robotic surgery trial for low- and intermediate-risk operable cancer patients, as their disease was more advanced and surgery may have led to a significant reduction in function.
Eight volunteers were administered sdCRT with 7,000 centigray (cGy), and 12 were administered rdCRT with 5,600 cGy. All patients had positive molecular testing for HPV in their tumor. Sixteen were found to be HPV16 positive, while four had other high-risk variants. As of the end of the third quarter of 2018, patients have been followed for a minimum of three and a half years and an average of more than four and a half years. The three-year progression-free and overall survival rates are 87.5 percent for those who were administered sdCRT (seven of eight participants) and 83.3 percent (log-rank test p=0.85) for those who were administered rdCRT (10 of 12 participants) for both measures. All three cancer failures were local or regional, and two of the three occurred in non-HPV16 high-risk variants, representing 50 percent of the patients with variants. All failures were in the first eight months after the start of treatment.
Researchers at the Head and Neck Cancer Research Program performed quality-of-life assessments which demonstrated significantly better outcomes among the rdCRT patients compared to sdCRT patients. Specifically, dysphagia, xerostomia, and pain returned to baseline significantly more rapidly in the reduced-dose subjects. Late effects have not been evaluated yet. These results were reported in abstracts at the American Society of Clinical Oncology (ASCO) meetings in 2017 and 2018.
“We concluded that rdCRT patients had similar progression-free and overall survival rates as compared to those receiving sdCRT,” says Marshall Posner, MD, Professor of Medicine (Hematology and Medical Oncology), and Otolaryngology, and Medical Director, Head and Neck Medical Oncology, at the Icahn School of Medicine. “These results support the clinical benefit of rdCRT as a treatment option with comparable survival to the sdCRT and with better quality of life.”
Currently, Dr. Posner and his team are conducting a second study, known as Quarterback II, in which all eligible patients are treated using rdCRT. Future modifications of this trial are being planned that will explore even lower-dose rdCRT and proton-beam technology.
“We hope to identify biologic and genetic markers from the patients entered into these trials to predict who would benefit from rdCRT and to improve therapy for our patients,” says Dr. Posner.
SEES: A Contemporary Approach to the Evaluation and Management of Dysphagia
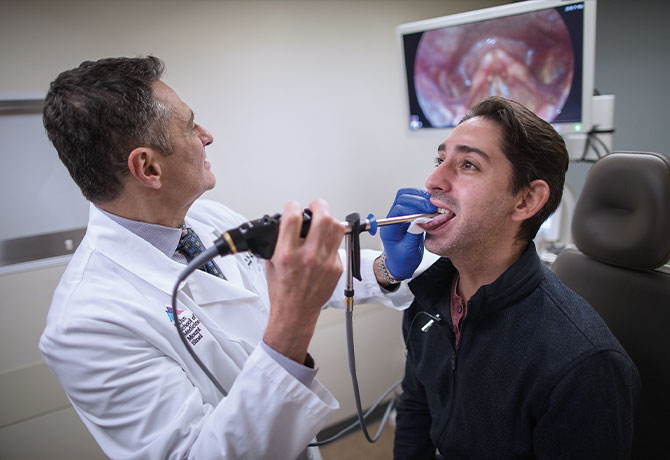
At The Grabscheid Voice and Swallowing Center of Mount Sinai, Mark S. Courey, MD, and his team are expediting the evaluation and management of patients with difficulty swallowing and reducing overall cost by using a new technique termed “static endoscopic evaluation of swallowing” (SEES). This in-office instrumental evaluation was developed and correlated against the gold standard modified barium swallow (MBS) by Dr. Courey, who is Director of The Grabscheid Voice and Swallowing Center and Chief of the Division of Laryngology within the Department of Otolaryngology – Head and Neck Surgery. SEES can be used in addition to or instead of the more traditional flexible endoscopic evaluation of swallowing (FEES).
Dysphagia impacts 1 in 25 adults in the United States each year, with prevalence increasing with age. As many as 68 percent of patients living in long-term care facilities are affected by the condition. It is estimated that patients with dysphagia increase hospital costs by $4,200 per year per patient and outpatient expenditures by $7,200 per patient compared to their age-equivalent peers. Studies have also found that management of the condition reduces the risk of aspiration pneumonia, the number one event leading to increased morbidity and mortality.
The SEES Evaluation
During studies conducted at the University of California, San Francisco, Dr. Courey found that SEES is a well-tolerated addition to the standard otolaryngologic evaluation, providing valuable information about the status of swallowing in patients with dysphagia-related problems.
Performed in a single office visit, the evaluation begins with an indirect transoral endoscopy, during which pre-swallow patterns of secretion pooling, pharyngeal strength, and laryngeal function are assessed. Next, an assessment of solid food swallowing is conducted by removing the scope and having the patient consume a dry, solid substance, like a graham cracker. The rigid endoscope is reinserted to assess the absence and quantitative presence, as well as location, of post-swallow pooling, penetration, and/or aspiration. Finally, an assessment of liquid swallowing of single sips and clinically appropriate liquid boluses is conducted. The endoscope is removed during swallowing and reinserted after to assess the post-swallow residue, penetration, and/or aspiration.
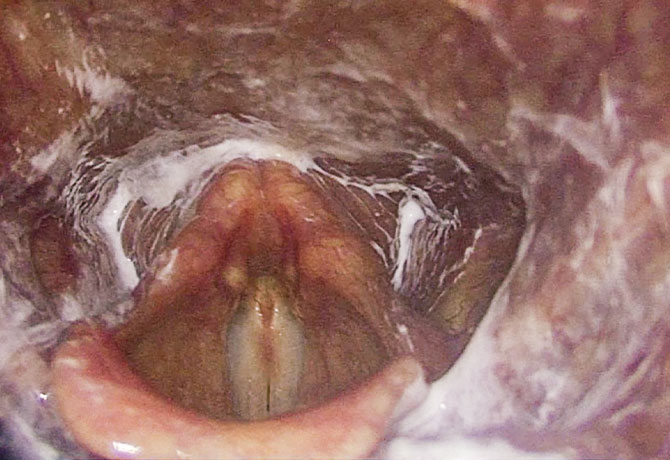
Unlike FEES, the SEES evaluation allows the detection of penetration and aspiration without invasive instruments or local anesthesia, which can affect swallow function. Additionally, it reduces the scheduling time and travel burden for patients who may need to return for radiographing if undergoing MBS.
Who Needs Evaluation for Dysphagia
Patients with dysphagia often present with vague symptoms such as unexplained cough, throat clearing, globus, and/or vocal changes. Clinicians must be astute when managing patients with these overlapping complaints and many may benefit from evaluation of swallowing function in addition to laryngeal function. Often, the entire speech mechanism, oropharynx, and hypopharynx must be examined for changes in structure and function.
The evaluation of patients with dysphagia starts with a careful problem-focused history. Meal length as well as alterations in diet should be documented. Meal times longer than 30 minutes are problematic, as patients often lose interest in eating as meal time extends. Clinicians should also note if choking or coughing is experienced more with certain substances, or if the patient has eliminated certain substances from his/her diet. Difficulty with liquids indicates a problem with swallow control or timing of swallow reflexes, while difficulty with solids usually indicates weakness of the muscles involved in swallowing.
After collecting a focused history, the clinical evaluation of swallowing includes a thorough examination of the speech mechanism, assessment of oro-motor control, testing of rapid alternating movements, testing of tongue strength in all directions, and assessment of hyolaryngeal elevation for completeness and rapidity of movement. Finally, the patient is asked to swallow a small liquid bolus while the clinician documents coughing or the development of a rough or wet voice quality indicative of laryngeal penetration or aspiration.
The Benefits of SEES
While clinical evaluation is important, it is no better than flipping a coin. Studies indicate that this form of testing of swallowing is only 50 percent sensitive in identifying laryngeal penetration or aspiration. This makes instrumental evaluation essential for the accurate diagnosis and management of patients with dysphagia. SEES is a simple and effective tool that can be used in the office to accurately characterize patterns of dysphagia.

Dysphagia is a variable and often multifactorial condition that disproportionately affects aging populations, those with neurologic illnesses, and patients with a history of head and neck cancer treatment. Although the ability to enjoy meals with family and peers is recognized as a major determinant in overall quality of life, few treatments are recommended or performed to help patients with significant loss of swallow function. The management of these patients begins with a thorough history and instrumental evaluation that is used to guide treatment and the adoption of safe swallow habits.
“We have developed SEES as a quick and accurate instrumental swallow assessment tool to assist with directing specific follow-up care plans for patients with dysphagia,” says Dr. Courey. “SEES may obviate the need for more expensive and time-consuming testing, and can be performed by any otolaryngologist to accurately assess patients with complaints of dysphagia.”
3D Printing and Immersive Simulation Improves Surgical Planning for Skull Base Surgeries
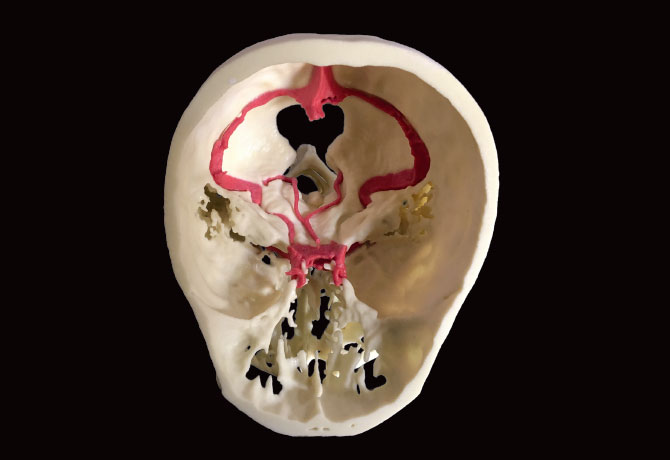
Neurosurgery and Otolaryngology teams at the Icahn School of Medicine at Mount Sinai have found success using 3D models to plan for the endoscopic approach to complex, minimally invasive skull base surgeries. Surgical planning is crucial during these procedures. Appropriate and effective surgical planning that uses 3D models has the potential to decrease general anesthesia time and allows surgeons to optimize preoperative planning and surgical efficiency to operate with greater certainty.
Prior to surgery, Mount Sinai teams use digital 3D models to highlight important bony landmarks and vessels in cases of odontoidectomy, Meckel’s cave mass, and skull-based adenoid cystic carcinoma. Surgeons simulate and analyze different surgical approaches using the digital models. The images are rotated or aspects are made semitransparent in order to see behind vessels or other structures that may be critical during a procedure. This real-time feedback allows for critical views to be replicated and important anatomy to be pictured. Most notably, it provides surgeons with the ability to accurately plan their approach and improve surgical efficiency. The digital models are then used to determine whether printed models would be beneficial for the tactile evaluation of surgical approach and adequate length of endoscopic tools, such as the high-speed drill.
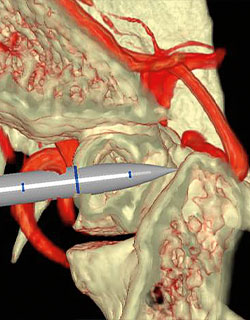
Preoperatively, patient-specific segmented structures generated from radiological imaging and representative 3D models are printed within 72 hours. Structural models are printed at one-to-one scale in full color using a ProJet 660 3D printer (Rock Hill, South Carolina, 3D Systems). Costs for full-color models were less than $500 per patient. The models allow surgeons to test various approaches, tools, and operative positioning in a patient-specific atmosphere.
Intraoperatively, Surgical Theater’s 3D imaging technology, the SuRgical Planner (SRP) and Surgical Navigation Advanced Platform (SNAP), are used to create and simulate the previously tested otolaryngology and neurosurgical skull base approaches with a 3D model of the patient’s anatomy and pathology.
Outside of surgery, the models could be used as an instructional tool for residents. Although a time-consuming process, the use of 3D reconstruction and printing in the surgical planning of complex, minimally invasive surgery allows for more efficiency and safety, especially for unconventional pathologies and surgical approaches. As navigation with 3D imaging and 3D printing becomes more widely available, it should be considered during the surgical planning for endoscopic endonasal approaches to lesions associated with obscured or difficult anatomy.
Using Multilevel Sectioning to Detect Lymph Node Metastases in Papillary Thyroid Cancer Patients
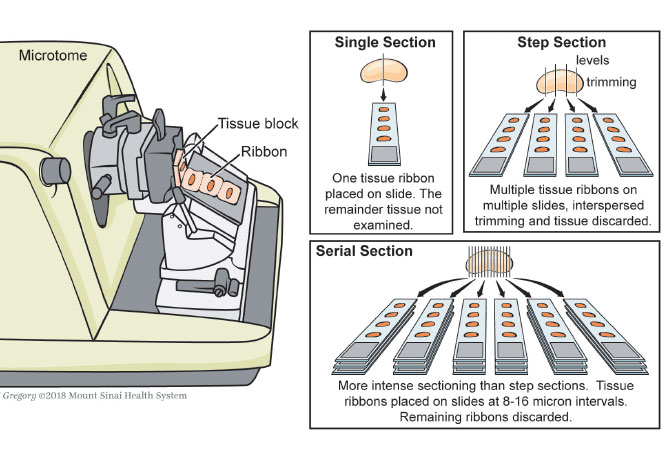
Based on results from a retrospective study, a team led by Mark Urken, MD, Chief of the Division of Head and Neck Surgical Oncology at Mount Sinai Downtown-Union Square, has proposed using the multilevel sectioning method as a standardized protocol in patients with papillary thyroid cancer on the cusp of intermediate-risk classification. The study aimed to determine whether intensified, multilevel sectioning increased the detection of micrometastases in intermediate-risk patients and found that the method ensured more consistent and accurate staging and risk stratification.
In accordance with American Thyroid Association guidelines, intermediate-risk papillary thyroid cancer patients may be considered for further treatment with radioactive iodine. One classification factor for intermediate risk is the presence of micrometastases in more than five lymph nodes. Determining the number of involved nodes is complicated by the extent of lymph node sectioning performed on intermediate-risk patients by the pathologist as well as the lack of standard sectioning protocol for patients on the cusp of intermediate-risk classification.
The team studied 17 patients who underwent total thyroidectomy for primary treatment of papillary thyroid carcinoma from January 2010 to August 2017 at Mount Sinai. Each patient had five or more lymph nodes excised during thyroidectomy and no more than five positive lymph nodes determined on initial pathologic analysis.
Using the multilevel protocol, new lymph nodes were identified in 6 of 17 patients. Multilevel sectioning yielded an additional 1.1 lymph node ± 0.9 SD per patient, compared to conventional sectioning (19.2 lymph nodes ± 14.9 SD vs. 18.1 lymph nodes ± 14.0 SD respectively; p=0.03, paired t-test). In total, 12 lymph nodes with metastatic disease were found. Six were found in lymph nodes newly identified using the multilevel sectioning method and six were found in lymph nodes previously deemed negative by conventional sectioning. For three patients, the revised number of positive lymph nodes reclassified them as intermediate risk.
In accordance with these findings, surgeons should alert pathologists as to which patients may be on the cusp of low to intermediate risk. This will enable clinicians to be highly selective in their recommendations to administer radioactive iodine therapy, and ensure that patients with metastatic disease receive optimal treatment.
Residency Program Receives Top Ranking

The Mount Sinai Hospital and New York Eye and Ear Infirmary of Mount Sinai’s combined Otolaryngology Residency Program at the Icahn School of Medicine at Mount Sinai was ranked sixth nationally in the field by physician social networking platform Doximity. In 2018, Marita Teng, MD, Associate Professor of Otolaryngology, and Residency Program Director for the Department of Otolaryngology, facilitated the merging of this training program which currently educates 35 residents.
Educating Physicians in the Virtual Classroom

The Department of Otolaryngology – Head and Neck Surgery, the Department of Academic Informatics and Technology, and the Office of CME at the Icahn School of Medicine at Mount Sinai have forged an innovative initiative with Coursera.org, an online learning platform. The initiative provides continuing medical education (CME) courses to busy physicians as well as on-demand access to high-quality MOOCs (massive open online courses).
“Increasing demand for the virtual classroom, coupled with Coursera’s more than 36 million learners worldwide, is what drew Mount Sinai to Coursera’s MOOC pedagogy,” said Paul Lawrence, MFA, Senior Associate Dean and Vice President of Academic and Research Informatics at the Icahn School of Medicine at Mount Sinai.
In 2015, Satish Govindaraj, MD, Associate Professor, Otolaryngology, Icahn School of Medicine at Mount Sinai, and Chief of Rhinology and Skull Base Surgery, Mount Sinai Health System, hosted the inaugural CME-accredited course on Coursera On Demand MOOC titled, “Acute and Chronic Rhinosinusitis: A Comprehensive Review.” Since then, the Department has launched the following courses:
- “HPV-Associated Oral and Throat Cancer: What You Need to Know,” hosted by Eric Genden, MD, MHCA, FACS, Chair of Otolaryngology – Head and Neck Surgery for the Mount Sinai Health System (CME-accredited)
- “Voice Disorders: What Patients and Professionals Need to Know,” hosted by Mark S. Courey, MD, Division Chief of Laryngology and Director of The Grabscheid Voice and Swallowing Center of Mount Sinai (CME-accredited)
- “Intro to Hearing Loss,” hosted by Maura Cosetti, MD, Director of the Cochlear Implant Program at the Ear Institute of New York Eye and Ear Infirmary of Mount Sinai (non-CME)
Each course contains at least four modules, followed by a brief quiz. Participants may take the course at no cost, pay $49 for the official Coursera certificate, or pay a total cost of $79 for the Coursera certificate and CME certificate.
“The flexibility of taking multiple remote modules versus attending a full course at once is a game changer for engagement, attendance, and learning outcomes,” noted Mr. Lawrence.
Message from the Chair: Eric Genden, MD, FACS
This past year, the Icahn School of Medicine at Mount Sinai celebrated its 50th anniversary, marking decades of groundbreaking research and clinical innovation. Galvanized by this significant milestone, physicians and scientists within the Department of Otolaryngology – Head and Neck Surgery powered 90 investigative studies at the Head and Neck Cancer Research Program. This denotes the largest volume of research activity in the Program’s 25-year history. The Ear Institute at New York Eye and Ear Infirmary of Mount Sinai, which observed its 10th anniversary in 2018, also led various pioneering efforts in otology.

George Wanna, MD, Site Chair at Mount Sinai Downtown, Chief of Otology-Neurotology for the Mount Sinai Health System, and Director of the Ear Institute, performed the first mastoidectomy using the Synaptive Medical Modus V, a high-resolution, robotically controlled digital microscope that enhances visualization as well as the surgical work space. Physicians at the Head and Neck Cancer Research Program advanced the Quarterback Trial, which uses reduced-dose chemoradiation in an attempt to decrease the side effects of radiation therapy in patients with locally advanced HPV-positive oropharynx. After completing a retrospective study on total thyroidectomy patients, pathologists and researchers at Mount Sinai Downtown-Union Square have proposed using the multilevel sectioning method as standard protocol.
Strides were also made with 3D printing and its role in planning complex skull base surgeries. Additionally, static endoscopic evaluation of swallowing (SEES)—a new technique for the evaluation and management of dysphagia—is evolving into the gold standard at The Grabscheid Voice and Swallowing Center of Mount Sinai.
With the adoption of these emerging technologies and investigations, our faculty and trainees are invigorated about the future. Thank you for perusing the detailed information in this year’s Specialty Report.
Dr. Isidore Friesner Professor and Chair
Department of Otolaryngology – Head and Neck Surgery
Senior Associate Dean for Clinical Affairs
Icahn School of Medicine at Mount Sinai