Integrated, Multi-“omic” Studies of Asthma Could Lead to Precision Treatment
Mount Sinai researchers’ review of asthma classification efforts highlights the importance of multidimensional data for stratifying a complex disease
Carefully designed, integrated multi-“omic” studies could accelerate the use of precision medicine for asthma patients, according to researchers from the Icahn School of Medicine at Mount Sinai. In an invited review article published today in the Journal of Allergy and Clinical Immunology, Scott R. Tyler, PhD, and Supinda Bunyavanich, MD, MPH report that numerous studies have shown the value of applying transcriptomics and other “omic” approaches (the study of the role, relationships, and actions of a system-wide measure of a given molecular type) for defining asthma subtypes—but they also cite the need for more studies aimed at pulling together these disparate data streams for a more comprehensive view of the disease.
Asthma is a highly heterogeneous disease, presenting with a broad range of symptoms. According to the American Lung Association, more than 26 million Americans have asthma. It is the third most common cause for hospitalization among children. Much effort has gone toward establishing clinical and molecular subtypes—known as endotypes—of asthma in order to better understand the disease and hone treatment recommendations for patients in each group.
“Endotypes are important for physicians and biomedical researchers because they organize the way we think about asthma, which manifests in many different ways across patient populations,” said Dr. Bunyavanich, faculty allergist/immunologist and Associate Professor of Pediatrics and of Genetics and Genomic Sciences, at the Icahn School of Medicine at Mount Sinai. “By strategically integrating clinical and molecular data, it should be possible to identify meaningful endotypes that both enhance our mechanistic understanding of asthma and guide our clinical care of asthma toward the best treatments for each subtype. This is important for optimizing patient outcomes.”
The review covers several types of omic studies that have been applied to asthma already, including transcriptomics, epigenomics, metabolomics, proteomics, and microbiome analysis. But, as the authors note, each approach captures only one dimension of the disease biology. More complex studies that integrate multiple layers of data have begun, but additional work is needed.
“We are in the early stages of these more sophisticated and comprehensive analyses of asthma, but the growth in available patient cohorts, data repositories, technology, and analytical tools gives us confidence that this kind of approach is rapidly becoming more feasible,” said Dr. Tyler, a postdoctoral fellow in the Bunyavanich Lab at Mount Sinai. “As this concept gains traction, it will be essential for researchers to ensure careful study design and implement rigorous methodology for the most reliable results for future use in precision medicine.”
The Bunyavanich lab is funded by the National Institutes of Health (NIH) R01 AI118833 and NIH U19 AI136053
Paper cited: Scott R. Tyler and Supinda Bunyavanich. Leveraging -Omics for Asthma Endotyping. Journal of Allergy and Clinical Immunology. DOI 10.1016/j.jaci.2019.05.015
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.
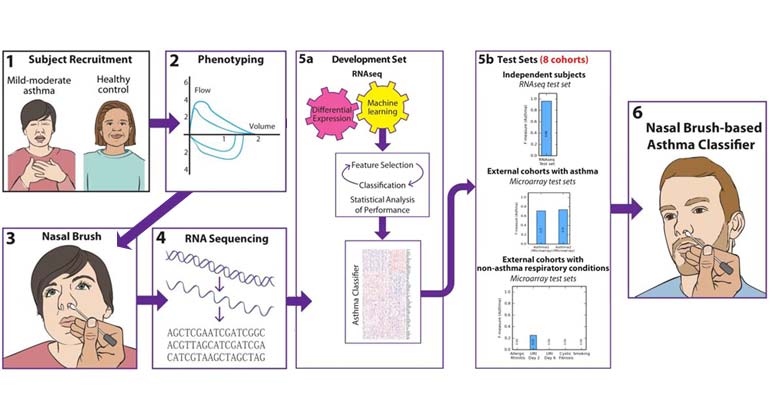
Mount Sinai Team Diagnoses Asthma With Nasal Brush Test
Jun 11, 2018 View All Press Releases