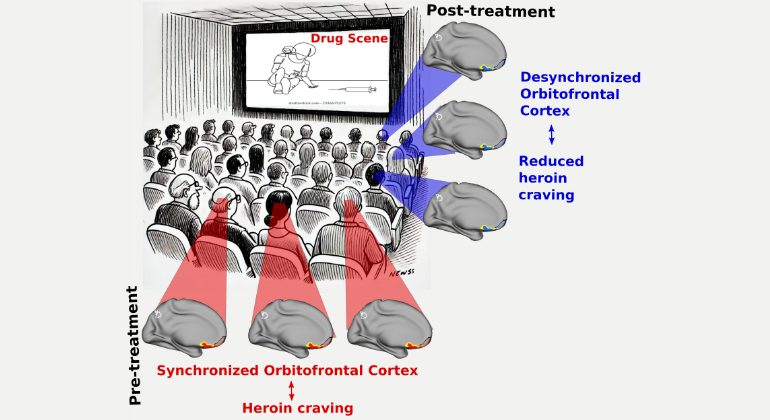
Dysregulation of the Brain’s Reward Learning System Is Identified by Scientists as a Potential Driver and Treatment Target for Cocaine Addiction
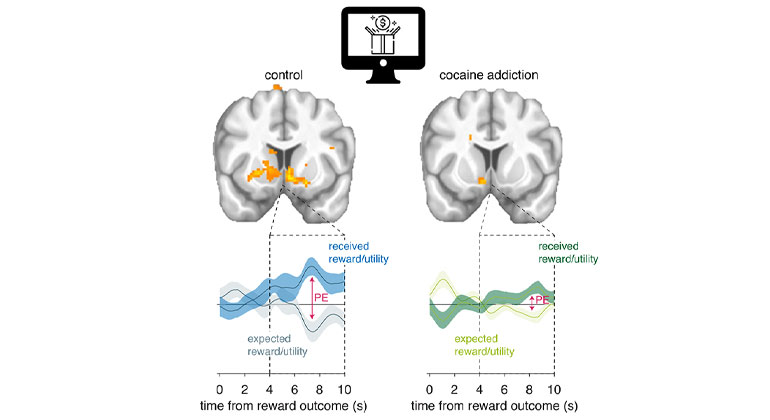
A Mount Sinai-led team of researchers has shed new light on the ways in which cocaine addiction dysregulates the normal function of dopamine neurons and thus the brain’s ability to process and respond to reward-related information, making it more difficult for individuals to change their addictive behaviors.
Their insights into the neural mechanisms that mediate and maintain continued cocaine use, reported in the journal Neuron, could potentially lead to interventions to modify and even prevent this addiction.
“Previous research, mostly in animal models, has suggested that chronic cocaine use degrades the normal functioning of dopamine, a neurotransmitter widely implicated in reward, motivation, and learning,” said Rita Z. Goldstein, PhD, the Mount Sinai Professor in Neuroimaging of Addiction at the Icahn School of Medicine at Mount Sinai and senior author of the work.
“In people with chronic cocaine addiction we observed a striking reduction in the way their reward system—a set of connected regions along the brain’s dopamine pathways—responds to the outcomes of the person’s decisions,” Dr. Goldstein added. “Instead of signaling clearly when an unexpected reward was received and broadcasting this information throughout the brain to inform future decisions, the signal was attenuated, making it harder to learn from experience and modify decision-making to obtain better outcomes. This finding could potentially inform therapeutic strategies to target addictive cocaine use behaviors, which are especially difficult to change since this system is not functioning properly.”
The study was designed to investigate whether people with chronic cocaine use disorder demonstrate differences in how their brains process and represent prediction “errors”—discrepancies between what an individual expects to receive as a reward and what they actually receive. This difference is used as a “teaching signal” by the brain to guide learning and adaptive decision-making.
For their study, researchers used a simple decision-making task inspired by studies of dopamine neurons in animal models to measure different kinds of reward responses in the ventral striatum, a brain region that receives dense dopaminergic inputs. The results showed that prediction error responses in the ventral striatum reflected “utility” prediction errors—errors that incorporate an individual’s subjective experience of reward as informed by their unique preferences for risk and uncertainty. Importantly, utility prediction error responses were found to be significantly reduced in people with cocaine addiction, who were generally more risk-tolerant, especially those who began using cocaine in early adolescence.
“Our work firmly establishes that compared to non-addicted individuals, and despite generally intact reward expectations, people with cocaine addiction demonstrate weaker responses to actual rewards in the brain’s reward system, particularly the ventral striatum,” explains Anna Konova, PhD, Assistant Professor of Psychiatry at Rutgers University and first author on the study. “This is important because these responses are crucial for the fidelity of the prediction error signal as a teaching signal. A reduced reward signal may contribute to addictive behavior by diminishing an individual’s ability to respond to the harmful effects of a drug, or the value of other, healthier alternatives to drug use.”
Researchers suggest that understanding the precise mechanisms of prediction error alterations that drive addiction could lead to novel, targeted interventions designed to restore the aberrant teaching signal. More specifically, their study points out that therapeutic strategies that aim to boost the impact of one’s decisions—namely the perception of received rewards—could be valuable for normalizing prediction error signaling and the ability of the individual to learn from their addiction experiences.
“We’ve gone further than any prior study to characterize the mechanistic source of prediction error disruptions in people with clinically defined cocaine disruption and believe researchers can build on these findings to explore innovative new treatments and prevention strategies,” said Dr. Goldstein. She also serves as Director of the Neuroimaging of Addictions and Related Conditions (NARC) Research Program at Icahn Mount Sinai.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.