Mount Sinai Study Finds Wearable Devices Can Detect COVID-19 Symptoms and Predict Diagnosis
Wearable devices can identify COVID-19 cases earlier than traditional diagnostic methods and can help track and improve management of the disease, Mount Sinai researchers report in one of the first studies on the topic. The findings were published in the Journal of Medical Internet Research on January 29.
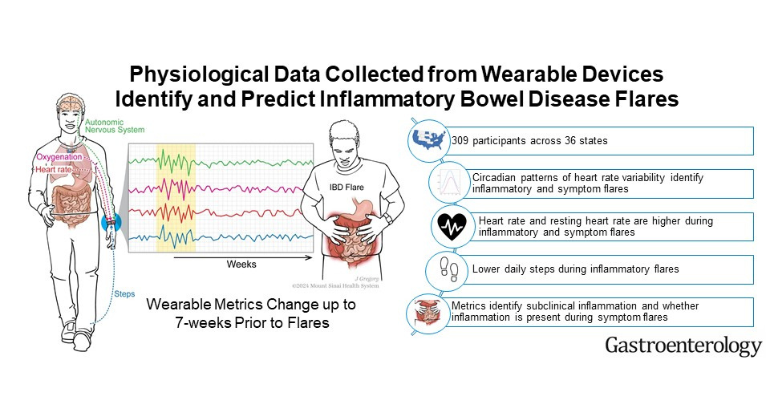
The Warrior Watch Study found that subtle changes in a participant’s heart rate variability (HRV) measured by an Apple Watch were able to signal the onset of COVID-19 up to seven days before the individual was diagnosed with the infection via nasal swab, and also to identify those who have symptoms.
“This study highlights the future of digital health,” says the study’s corresponding author Robert P. Hirten, MD, Assistant Professor of Medicine (Gastroenterology) at the Icahn School of Medicine at Mount Sinai, and member of the Hasso Plattner Institute for Digital Health at Mount Sinai and the Mount Sinai Clinical Intelligence Center (MSCIC). “It shows that we can use these technologies to better address evolving health needs, which will hopefully help us improve the management of disease. Our goal is to operationalize these platforms to improve the health of our patients and this study is a significant step in that direction. Developing a way to identify people who might be sick even before they know they are infected would be a breakthrough in the management of COVID-19.”
The researchers enrolled several hundred health care workers throughout the Mount Sinai Health System in an ongoing digital study between April and September 2020. The participants wore Apple Watches and answered daily questions through a customized app. Changes in their HRV—a measure of nervous system function detected by the wearable device—were used to identify and predict whether the workers were infected with COVID-19 or had symptoms. Other daily symptoms that were collected included fever or chills, tiredness or weakness, body aches, dry cough, sneezing, runny nose, diarrhea, sore throat, headache, shortness of breath, loss of smell or taste, and itchy eyes.
Additionally, the researchers found that 7 to 14 days after diagnosis with COVID-19, the HRV pattern began to normalize and was no longer statistically different from the patterns of those who were not infected.
“This technology allows us not only to track and predict health outcomes, but also to intervene in a timely and remote manner, which is essential during a pandemic that requires people to stay apart,” says the study’s co-author Zahi Fayad, PhD, Director of the BioMedical Engineering and Imaging Institute, Co-Founder of the MSCIC, and the Lucy G. Moses Professor of Medical Imaging and Bioengineering at the Icahn School of Medicine at Mount Sinai.
The Warrior Watch Study draws on the collaborative effort of the Hasso Plattner Institute for Digital Health and the MSCIC, which represents a diverse group of data scientists, engineers, clinical physicians, and researchers across the Mount Sinai Health System who joined together in the spring of 2020 to combat COVID-19. The study will next take a closer look at biometrics including HRV, sleep disruption, and physical activity to better understand which health care workers are at risk of the psychological effects of the pandemic.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with 48,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 9,000 primary and specialty care physicians and 11 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals, Best in State Hospitals, World Best Hospitals and Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2024-2025.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.