Multi-omics Approach Offers New Insights into Peanut Allergy Severity
Findings could improve diagnostics and lead to new treatments
Researchers at the Icahn School of Medicine at Mount Sinai have identified novel genes associated with the severity of peanut allergy, as well as ways in which these genes interact with other genes during allergic reactions.
The findings, published December 12 in the Journal of Allergy and Clinical Immunology, could lead to better treatments for peanut allergy.
Peanut allergy varies widely in severity and is the leading cause of fatal food-related anaphylaxis. The tests used to determine the existence of a peanut allergy don’t offer any clues as to whether an individual ingesting a peanut could experience a minor rash, major swelling, or life-threatening issues such as difficulty breathing or cardiovascular complications.
The study’s senior author, Supinda Bunyavanich, MD, MPH, Associate Professor of Genetics and Genomic Sciences, and Pediatrics, and Associate Director of the Elliot and Roslyn Jaffe Food Allergy Institute at Mount Sinai, was especially curious about why the severity of reactions varies so much, both as a clinician-scientist and as a mother of a child with a peanut allergy.
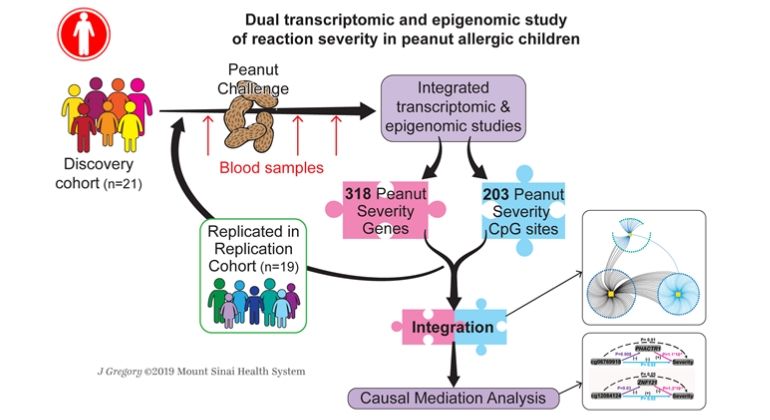
To help address this question, Dr. Bunyavanich and her team used novel multi-omic approaches (the study of the role, relationships, and actions of a system-wide measure of a given molecular type) to identify genes and networks of activity that might be driving the severity of peanut allergy reactions. The approaches included transcriptomics, the study of gene expression across the genome, and epigenomics, the study of reversible modifications to DNA that affect gene expression.
The study involved 21 children ages 7-17 with peanut allergy, who were given gradually increasing doses of peanut until they displayed an allergic response. The scientists drew blood from the participants at three times: before they ate, as they reacted, and after their reaction. The team confirmed their findings from the initial cohort by repeating the study in another 19 children.
Taking blood samples at multiple times allowed the team to analyze both the transcriptome and epigenome (which can tell scientists which genes are turned on or off through a process called methylation) as the children reacted. Using this genome-wide approach, they identified more than 300 genes and 200 CpG sites (areas where DNA can be activated or inactivated by methylation) associated with reaction severity. Combining these data using integrative networks, the team also characterized key interactions between gene expression, CpG sites, and reaction severity.
Not only did they identify novel genes associated with the severity of peanut allergy, but they also managed to characterize ways in which these genes interact with other genes and CpG sites during allergic reactions to regulate biological processes. “It was very exciting to apply multi-omics to uncover how genes and methylation sites interact to affect reaction severity in these peanut allergic kids,” says Anh Do, PhD, lead author of the study and postdoctoral fellow in the Bunyavanich Lab.
Among the insights is that while the findings support recognized roles for adaptive immunity in allergy, they also suggest that neutrophil (a type of white blood cell)-mediated immunity plays a prominent role in reaction severity. “We know neutrophil-mediated immunity is part of immune responses, and this study suggests it may play a central role in the severity of peanut allergic reactions,” said Dr. Bunyavanich.
Additionally, one of the reaction severity drivers the team identified, the gene ARG1, can be inhibited by arginase inhibitors, a type of drug under study for many diseases. This study’s finding suggests it may be a potential target for treating peanut allergy as well.
Dr. Bunyavanich hopes future studies will identify biomarkers that can predict who is likely to have severe responses without having to expose them to peanuts first. But in the meantime, she states that this study “hopefully challenges people to think about food allergy with a broader lens.”
This study was supported by the National Institutes of Health (R01AI118833, U19AI136053, U19AI066738 and U01AI066560) and the Mindich Child Health and Development Institute at Mount Sinai.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.
Mount Sinai Researchers: Why COVID-19 May Be Less Common in Children Than Adults
May 22, 2020 View All Press ReleasesAirway Microbiome and Host Interact Differently in Children with Severe Asthma
Mar 12, 2020 View All Press Releases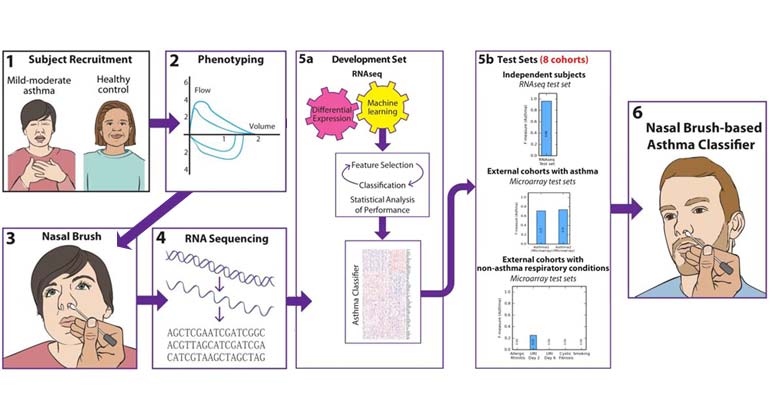
Mount Sinai Team Diagnoses Asthma With Nasal Brush Test
Jun 11, 2018 View All Press Releases