Osteoarthritis
Hypertrophic osteoarthritis; Osteoarthrosis; Degenerative joint disease; DJD; OA; Arthritis - osteoarthritis
Osteoarthritis (OA) is the most common joint disorder. It is due to aging and wear and tear on a joint.

You used to take for granted that you could play a whole game of tennis or basketball without pain. But years of wear and tear have left their mark on your joints, and now your knees and hips hurt so much you can barely bend them. The pain you're feeling may be due to osteoarthritis, a problem many of us face as we get older. We all start out life with a thick layer of cartilage that cushions our joints in the space where the bones meet. That cartilage allows us to twist our legs to kick a soccer ball, or jump to shoot a basket. But years of running, jumping, and climbing stairs can wear out that cushion, leaving the bones rubbing painfully against each other. By age 70, just about everyone feels some pain and stiffness from osteoarthritis, especially when they get up in the morning or after they've overused the joint. You're more likely to have osteoarthritis if you're overweight. It's similar to what happens when you put extra weight on your bed. Eventually, you'll push on the springs so hard that you'll wear them out. The same is true for your joints. People who've had joint injuries or who have played certain sports are also more likely to get osteoarthritis. When you see your doctor about joint pain and stiffness, he'll check how well the joint moves and look for swelling around it. You probably won't be able to move the joint all the way. And when you do move it, it's likely to hurt and may make a cracking sound. An x-ray can confirm that you've lost cartilage around the joint. Unfortunately, there's no cure for osteoarthritis. But there are treatments to relieve the pain, including physical therapy, knee taping, special low load exercise programs, such as swimming, cycling, walking or stretching, and Tai chi in particular can be great for flexibility and strength. Over-the-counter medicines like topical Capsaicin, oral acetaminophen, aspirin, ibuprofen, and naproxen may help. Mud pack therapy may increase the benefit of whatever else you're doing. Your doctor may recommend getting a steroid injection into the joint to both relieve pain and reduce swelling. Another method, which injects artificial joint fluid into the knee, can relieve pain longer term, for up to six months. If the joint damage is really bad, you may need surgery to trim off damaged cartilage or to replace the affected joint in the knee, hip, shoulder, or elbow with an artificial joint. This is called joint replacement surgery, and is quite common for the both damaged hip and knee joints. Although it may hurt to move, staying active can help keep your joints healthy. Exercising can also help you lose the weight that's putting pressure on your sore joints. Ask your doctor to recommend a physical therapist, who can teach you exercises that strengthen the muscles supporting your joints. Osteoarthritis is different in everyone. Some people can get around fine with it while others have trouble doing even the simplest tasks, like bending down to get the morning paper. Before your joints get so stiff and painful that they limit your lifestyle, talk to your doctor about treatment and prevention options that can help you get around more like you used to.
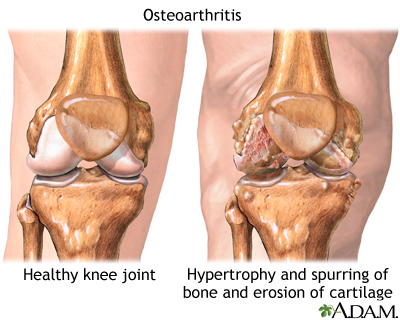
Osteoarthritis is a chronic disease of the joint cartilage and bone, often thought to result from wear and tear on a joint, although there are other causes such as congenital defects, trauma and metabolic disorders. Joints appear larger, are stiff and painful and usually feel worse the more they are used throughout the day.
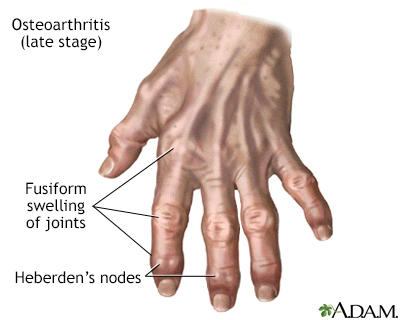
Osteoarthritis is associated with the aging process and can affect any joint. The cartilage of the affected joint is gradually worn down, eventually causing bone to rub against bone. Bony spurs develop on the unprotected bones causing pain and inflammation.

Osteoarthritis is the most common form of arthritis and is associated with the aging process. Even from the outside, you can see that the knee of an older person looks considerably different than that of a younger person. Let's take a look at the joint itself to see the differences. Osteoarthritis is a chronic disease, a disease that persists for a long time. It causes the deterioration of the cartilage within a joint. For most people, the cause of osteoarthritis is unknown, but metabolic, genetic, chemical, and mechanical factors play a role in its development. Symptoms of osteoarthritis include loss of flexibility, limited movement, and pain and swelling within the joint. The condition results from injury to the cartilage, which normally absorbs stress and covers the bones, so they can move smoothly. The cartilage of the affected joint is roughened and becomes worn down. As the disease progresses, the cartilage becomes completely worn down and the bone rubs on bone. Bony spurs usually develop around the margins of the joint. Part of the pain results from these bone spurs, which can restrict the joint's movement as well.
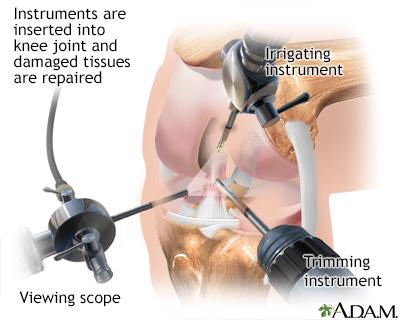
Arthroscopy allows for the visualization of the interior of a joint through the use of optic instruments. Surgery can now be performed on larger joints using direct visualization and miniaturized techniques. After this procedure, the person can often go home the same day.
You used to take for granted that you could play a whole game of tennis or basketball without pain. But years of wear and tear have left their mark on your joints, and now your knees and hips hurt so much you can barely bend them. The pain you're feeling may be due to osteoarthritis, a problem many of us face as we get older. We all start out life with a thick layer of cartilage that cushions our joints in the space where the bones meet. That cartilage allows us to twist our legs to kick a soccer ball, or jump to shoot a basket. But years of running, jumping, and climbing stairs can wear out that cushion, leaving the bones rubbing painfully against each other. By age 70, just about everyone feels some pain and stiffness from osteoarthritis, especially when they get up in the morning or after they've overused the joint. You're more likely to have osteoarthritis if you're overweight. It's similar to what happens when you put extra weight on your bed. Eventually, you'll push on the springs so hard that you'll wear them out. The same is true for your joints. People who've had joint injuries or who have played certain sports are also more likely to get osteoarthritis. When you see your doctor about joint pain and stiffness, he'll check how well the joint moves and look for swelling around it. You probably won't be able to move the joint all the way. And when you do move it, it's likely to hurt and may make a cracking sound. An x-ray can confirm that you've lost cartilage around the joint. Unfortunately, there's no cure for osteoarthritis. But there are treatments to relieve the pain, including physical therapy, knee taping, special low load exercise programs, such as swimming, cycling, walking or stretching, and Tai chi in particular can be great for flexibility and strength. Over-the-counter medicines like topical Capsaicin, oral acetaminophen, aspirin, ibuprofen, and naproxen may help. Mud pack therapy may increase the benefit of whatever else you're doing. Your doctor may recommend getting a steroid injection into the joint to both relieve pain and reduce swelling. Another method, which injects artificial joint fluid into the knee, can relieve pain longer term, for up to six months. If the joint damage is really bad, you may need surgery to trim off damaged cartilage or to replace the affected joint in the knee, hip, shoulder, or elbow with an artificial joint. This is called joint replacement surgery, and is quite common for the both damaged hip and knee joints. Although it may hurt to move, staying active can help keep your joints healthy. Exercising can also help you lose the weight that's putting pressure on your sore joints. Ask your doctor to recommend a physical therapist, who can teach you exercises that strengthen the muscles supporting your joints. Osteoarthritis is different in everyone. Some people can get around fine with it while others have trouble doing even the simplest tasks, like bending down to get the morning paper. Before your joints get so stiff and painful that they limit your lifestyle, talk to your doctor about treatment and prevention options that can help you get around more like you used to.
Causes
Cartilage is the firm, rubbery tissue that cushions your bones at the joints. It allows bones to glide over one another when the joint moves. When the cartilage breaks down and wears away, the fragments of the cartilage or the bones rub together. This often causes the pain, swelling, and stiffness of OA.
As OA worsens, bony spurs or extra bone may form around the joint. The ligaments and muscles around the joint may become weaker and stiffer.
Before age 55, OA occurs equally in men and women. After age 55, it is more common in women.
Other factors can also lead to OA.
- OA tends to run in families.
- Being overweight increases the risk for OA in the hip, knee, ankle, and foot joints. This is because extra weight causes more wear and tear.
- Fractures or other joint injuries can lead to OA later in life. This includes injuries to the cartilage and ligaments in your joints.
- Jobs that involve kneeling or squatting for more than an hour a day, or involve lifting, climbing stairs, or walking increase the risk for OA.
- Playing sports that involve direct impact on the joint (football), twisting (basketball or soccer), or throwing also increase the risk for OA.
Medical conditions that can lead to OA or symptoms similar to OA include:
- Bleeding disorders that cause bleeding in the joint, such as hemophilia
- Disorders that block the blood supply near a joint and lead to bone death (avascular necrosis)
- Other types of arthritis, such as long-term (chronic) gout, pseudogout, or rheumatoid arthritis
Symptoms
Symptoms of OA often appear in middle age. Almost everyone has some symptoms of OA by age 70.
Pain and stiffness in the joints are the most common symptoms. The pain is often worse:
- After exercise
- When you put weight or pressure on the joint
- When you use the joint
With OA, your joints may become stiffer and harder to move over time. You may notice a rubbing, grating, or crackling sound when you move the joint.
"Morning stiffness" refers to the pain and stiffness you feel when you first wake up in the morning. Stiffness due to OA often lasts for 30 minutes or less. It can last more than 30 minutes if there is inflammation in the joint. It often improves after activity, allowing the joint to "warm up."
During the day, the pain may get worse when you are active and feel better when you are resting. As OA gets worse, you may have pain even when you are resting. And it may wake you up at night.
Some people might not have symptoms, even though x-rays show the physical changes of OA.
Exams and Tests
Your health care provider will examine you and ask about your symptoms. The exam may show:
- Joint movement that causes a crackling (grating) sound, called crepitation
- Joint swelling (either due to fluid in the joint or the bones around the joints feeling larger than normal)
- Limited range of motion
- Tenderness when the joint is pressed
- Normal movement is often painful
Blood tests are not helpful in diagnosing OA. They can be used to look for alternative conditions, such as rheumatoid arthritis or gout.
An x-ray will likely show:
- Loss of the joint space
- Wearing down of the ends of the bone
- Bone spurs
- Bony changes near the joint, called subchondral cysts
Treatment
OA cannot be cured, but OA symptoms can be controlled. OA will most likely get worse over time though the pace with which this occurs varies from person to person.
You can have surgery, but other treatments can improve your pain and make your life much better. Although these treatments cannot make the OA go away, they can often delay surgery or make your symptoms mild enough to not cause significant problems.
MEDICINES
Over-the-counter (OTC) pain relievers, such as acetaminophen (Tylenol) or a nonsteroidal anti-inflammatory drug (NSAID) can help with OA symptoms. You can buy these medicines without a prescription.
It is recommended that you should not take more than 3 grams (3,000 mg) of acetaminophen a day. If you have liver disease, talk with your provider before taking acetaminophen. Over the counter NSAIDs include aspirin, ibuprofen, and naproxen. Several other NSAIDs are available by prescription. Talk with your provider before taking an NSAID on a regular basis.
Duloxetine (Cymbalta) is a prescription medicine that can also help treat long-term (chronic) pain related to OA.
Injections of steroid medicines into the arthritic joint often provide significant short to medium-term benefits from the pain of OA.
Other medicines that may help include:
- Pills, such as glucosamine and chondroitin sulfate
- Capsaicin skin cream to relieve pain
LIFESTYLE CHANGES
Staying active and getting exercise can maintain joint and overall movement. Ask your provider to recommend an exercise routine or refer you to a physical therapist. Water exercises, such as swimming, are often helpful.
Other lifestyle tips include:
- Applying heat or cold to the joint
- Eating healthy foods
- Getting enough rest
- Losing weight if you are overweight
- Protecting your joints from injury
If the pain from OA gets worse, keeping up with activities may become more difficult or painful. Making changes around the home can help take stress off your joints to relieve some of the pain. If your work is causing stress in certain joints, you may need to adjust your work area or change work tasks.
PHYSICAL THERAPY
Physical therapy can help improve muscle strength and the motion of stiff joints as well as your balance. If therapy does not make you feel better after 6 to 12 weeks, then it likely will not be helpful.
Massage therapy may provide short-term pain relief but does not change the underlying OA process. Make sure you work with a licensed massage therapist who is experienced in working on sensitive joints.
BRACES
Splints and braces may help support weakened joints. Some types limit or prevent the joint from moving. Others may shift pressure off one portion of a joint. Use a brace only when your provider or therapist recommends one. Using a brace the wrong way can cause joint damage, stiffness, and pain.
ALTERNATIVE TREATMENTS
Acupuncture is a traditional Chinese treatment. It is thought that when acupuncture needles stimulate certain points on the body, chemicals that block pain are released. Acupuncture may provide significant pain relief for OA.
Yoga and Tai chi have also shown significant benefit in treating the pain from OA.
S-adenosylmethionine (SAMe, pronounced "Sammy") is a manmade form of a natural chemical in the body. It may help reduce joint inflammation and pain.
SURGERY
Severe cases of OA might benefit from surgery to replace or repair damaged joints. Options include:
- Arthroscopic surgery to trim torn and damaged cartilage
- Changing the alignment of a bone to relieve stress on the bone or joint (osteotomy)
- Surgical fusion of bones, often in the spine (arthrodesis)
- Total or partial replacement of the damaged joint with an artificial joint (knee replacement, hip replacement, shoulder replacement, ankle replacement, and elbow replacement)
Support Groups
Organizations that specialize in arthritis are good resources for more information on OA.
Outlook (Prognosis)
Your movement may become limited over time. Doing everyday activities, such as personal hygiene, household chores, or cooking may become a challenge. Treatment usually improves function.
When to Contact a Medical Professional
Contact your provider if you have symptoms of OA that get worse.
Prevention
Try not to overuse a painful joint at work or during activities. Maintain a normal body weight. Keep the muscles around your joints strong, especially the weight-bearing joints (knee, hip, or ankle).
References
Hunter DJ. Osteoarthritis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 241.
Kolasinski SL, Neogi T, Hochberg MC, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the hand, hip, and knee. Arthritis Care Res (Hoboken). 2020;72(2):149-162. PMID: 31908149
Misra D, Kumar D, Neogi T. Treatment of osteoarthritis. In: Firestein GS, Budd RC, Gabriel SE, Koretzky GA, McInnes IB, O'Dell JR, eds. Firestein & Kelley's Textbook of Rheumatology. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 106.
Version Info
Last reviewed on: 4/10/2022
Reviewed by: David C. Dugdale, III, MD, Professor of Medicine, Division of General Medicine, Department of Medicine, University of Washington School of Medicine, Seattle, WA. Internal review and update on 07/09/2023 by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
