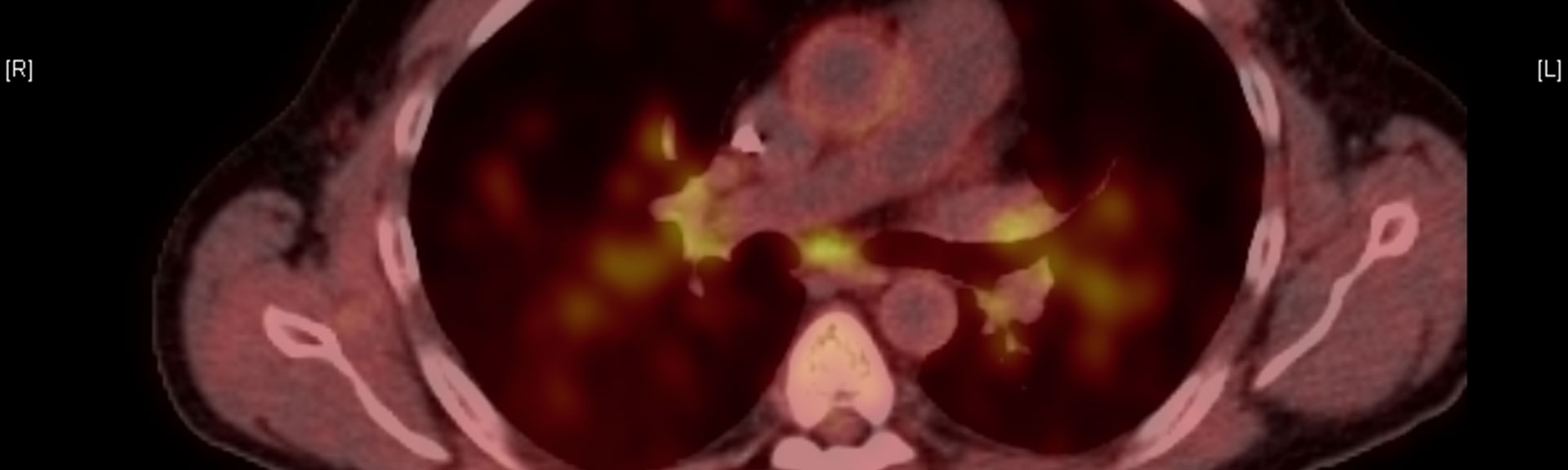
Catherine and Henry J. Gaisman Division of Pulmonary, Critical Care and Sleep Medicine
We provide state-of-the-art consultation, diagnostic testing and clinical and multidisciplinary care to patients with simple and complex respiratory and respiratory-related diseases
Catherine and Henry J. Gaisman Division of Pulmonary, Critical Care and Sleep Medicine
With the opening of a permanent home on our campus for the Mount Sinai – National Jewish Health Respiratory Institute, we have created a model for delivering patient-centered, multidisciplinary, state-of-the-art care for patients with simple and complex respiratory diseases.
This specialty report highlights:
- Our long tradition of sarcoidosis research and treatment and two complex cases solved through urgent teamwork
- Our lung cancer research program, which has identified key molecular pathways activated in the progression of adenocarcinoma from indolent tumor to metastatic tumor—an increasingly important focal area
- Innovative efforts in off-label device use, including the placement of lung valves to treat surgical leaks and a fully portable positive pressure ventilator that helped treat a difficult case of tracheomalacia
- A clinical trial of an interleukin 4 receptor alpha blocker that may provide a more effective way to block cytokines in asthma patients with underlying type 2 inflammation
- The new Mount Sinai Center for Integrative Sleep Medicine, which will unify clinical and research information from outpatient and inpatient sleep studies across the Mount Sinai Health System
A Creative Fight Against Sarcoidosis
Complex Cases Are Solved Through Urgent Teamwork
It is not often that sarcoidosis poses a challenge for Louis DePalo, MD, Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine at Mount Sinai. But in cases of neurosarcoidosis and cardiac sarcoidosis, it takes an urgent response, a team approach, and some out-of-the-box thinking to achieve success.
Noam Jacknis can testify to that. In 2011, the now 31-yearold began experiencing symptoms such as dizziness, lower back pain, and vomiting. Sent by his doctor for a range of tests, including MRIs and lumbar puncture, the presumed diagnosis was a central nervous system malignancy, and he was referred to a Mount Sinai neurologist for a lymph node and brain biopsy. When those tests revealed sarcoidosis, Dr. DePalo was called in.
It was clear that an aggressive regimen of steroids was required to treat the neurosarcoidosis and prevent any loss of function, but there was a complication: Mr. Jacknis has type I diabetes. Not only would Dr. DePalo have to partner with Mr. Jacknis’s endocrinologist to manage his blood sugar, he would also need to address the risk of infection and neuropathy. He decided to utilize a second agent in Mr. Jacknis’s treatment: Remicade® (infliximab)—a monoclonal antibody historically used to treat Crohn’s disease, colitis, arthritis, and psoriasis.
“There were some clinical data that supported using it in this situation, and we had some success with it with other patients,” Dr. DePalo says. “By using Remicade, we could minimize the steroids used and mitigate their side effects, but because it was off-label and expensive, we had a six-month battle with the insurers to get it approved.”
Dr. DePalo and his team eventually were able to induce remission, although Mr. Jacknis suffered one relapse. But he is now married and has started a family, which he says would not have been possible without Dr. DePalo.
Unlike Mr. Jacknis, Roy Rutledge did not appear to have an urgent case of complex sarcoidosis during his first consultation with Dr. DePalo in April 2014. A beach volleyball enthusiast, the 55-year-old had been experiencing shortness of breath and more colds than usual, and his heart rate had crashed during a February 2014 colonoscopy. He also had been diagnosed with pneumonia and was experiencing pain that made it impossible for him to lie down.

Mr. Rutledge underwent a series of tests, including a renal ultrasound, X-ray, and chest CT scan, but no one was able to explain his pain or why his condition had not improved. On the suggestion of a relative, Mr. Rutledge reached out to Dr. DePalo.
Although Mr. Rutledge’s X-ray and CT scan were somewhat atypical, Dr. DePalo was inclined to agree that this was a case of lower left lobe pneumonia—until Mr. Rutledge began experiencing arrhythmias and more pronounced chest pains. Dr. DePalo ordered an EKG that revealed a heart block.
“Abnormal X-ray, nodules, heart block—it was starting to look like sarcoidosis,” Dr. DePalo says. “We did an MRI of the heart and then a catheterization and a myocardial biopsy of the right ventricle that confirmed the diagnosis. The majority of the time, this type of biopsy is negative, so we used our imaging studies to help direct it.”
Meanwhile, Mr. Rutledge’s condition progressed very quickly to the point where he developed complete heart block, necessitating the placement of a pacemaker and defibrillator by Mount Sinai’s cardiac team. Determined to preserve cardiac function, Dr. DePalo began an aggressive regimen of steroids and, after much back and forth with insurers, Remicade to limit the side effects of the steroids. “Much like neurosarcoidosis, the stakes are higher than with a skin or even a lung sarcoid. If you don’t hit it fast and hard, there is a risk that the heart could burn out and the patient would be forever disabled or require a transplant,” Dr. DePalo says.
Like Mr. Jacknis, Mr. Rutledge experienced one relapse requiring a second round of treatment. But now, off all treatments and with an implantable cardioverter defibrillator maintaining his heart rate, Mr. Rutledge is playing beach volleyball again, proving that the right treatment at the right time from the right team can go a long way to getting someone back in the game.
Identifying Indolent Lung Cancer Gene
Studies Could Help Differentiate Among Tumors
A scientist at The Mount Sinai Hospital is leading a multisite research project on the molecular differences among nonsmall-cell lung adenocarcinomas that could be a game changer in the treatment of patients with lung cancer.
Using genomic techniques, Charles A. Powell, MD, Director of the Mount Sinai – National Jewish Health Respiratory Institute, is identifying differences in the cell genomics and pathways in early adenocarcinomas that are indolent versus those that are more aggressive and invasive.
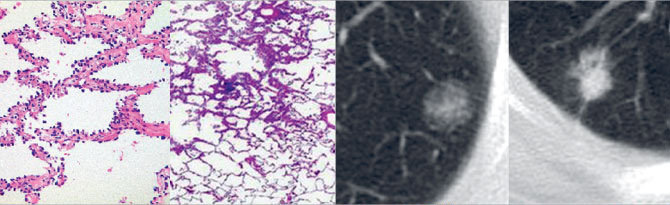
Lung adenocarcinoma has the potential to progress from a pathological in-situ lesion (left)
Through research, Dr. Powell and his colleagues have been able to demonstrate an association between the state of a tumor and amplification of gene copy numbers. Some of these genes offer opportunities for diagnostic testing and therapeutic treatment that can retard or reverse progression of these tumors.
Using fluorescent in-situ hybridization (FISH), where dyes are attached to parts of chromosomes and studied under a fluorescent microscope, Dr. Powell and his colleagues have observed that two genes in particular do show amplification in invasive human lung adenocarcinomas: cyclin-dependent kinase 4 (CDK4) and mouse double minute 2 homolog (MDM2).
“We’ve gone on to use cells in the labs to examine the mechanisms associated with these observations,” Dr. Powell notes. “For that, we’ve manipulated the copies and expressions of these genes themselves and have changed their behavior. We’ve subsequently demonstrated in preclinical trials that we can use MDM2 inhibitors, some of which are now clinically available, to inhibit these pathways and retard their aggressive tendencies.”
These findings, Dr. Powell notes, suggest that certain subsets of early-stage lung cancer are indolent to the point where they can be observed instead of treated—a radical change from the historic approach of aggressive treatment for all lung adenocarcinomas.
“We’re becoming more comfortable with observing these early-stage tumors through a screening program, rather than moving immediately to do a resection. We save patients the inherent, albeit small, risks of that procedure, and I think that’s helping very much to improve the quality of care that patients can receive.”
It is also a game changer in that it brings molecular markers into the realm of early lung-cancer diagnosis, which is typically done using clinical and imaging data. “That’s relevant for tumors that may look the same at the level of imaging but may be different at the level of their particular biology,” Dr. Powell says. “This application can further refine assessments in terms of predicting the biological behavior of a particular tumor.”
Funded by a National Institutes of Health grant, the study includes researchers from Cornell University and Vanderbilt University, as well as colleagues from the Departments of Radiology, Thoracic Surgery, Pathology, and Genomics at the Mount Sinai Health System. Dr. Powell says the grant program will continue as he and his colleagues work to bring into human clinical trials the inhibitors that demonstrated efficacy in the preclinical trials and animal models they have developed. They will also look for other biomarkers that could be used in the diagnosis of various biological subtypes of lung adenocarcinoma.
“There are very few biomarkers that have successfully made the jump to such an application. That’s in large part due to the complexity of the cancer and the heterogeneity of both the patients and the tumors. CDK4 and MDM2 could be amongst the first gene copy targets to make that leap, but we think there are more, and that’s what we will be looking for.”
New Use for Lung Valves
Device Aids Patients With Leaks After Surgery
The Mount Sinai Health System is using endo-bronchial valves to improve healing times and eliminate the need for additional surgery in patients who experience prolonged air leaks after lung surgeries.
Timothy Harkin, MD, an Associate Professor of Medicine and Thoracic Surgery at the Icahn School of Medicine at Mount Sinai and Director of Interventional Pulmonology, says the valves, developed by Spiration® for use in patients with emphysema, are FDA approved only for humanitarian use for persistent lung air leaks—those lasting approximately five to seven days—following lobectomy, segmentectomy, or lung-volume reduction surgery.
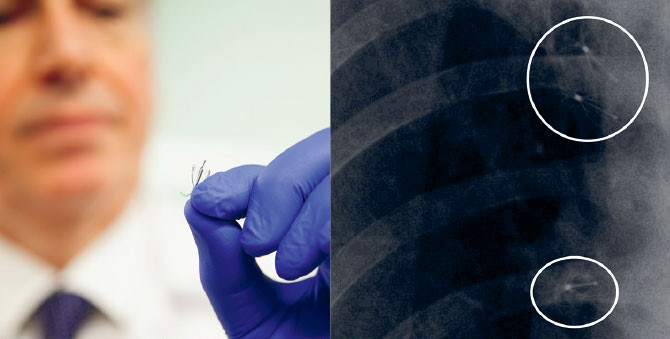
Using a bronchoscope and catheter, Dr. Harkin inserts the valves, which resemble tiny umbrellas, into the airway that supplies the part of the lung where the leak occurs. Dr. Harkin says the valves have an 80 percent efficacy rate, typically failing due to spontaneous rupture of the underlying lung disease or the presence of collateral ventilation.
One instance of collateral ventilation involved a patient with a persistent air leak after a segmentectomy in the right upper lobe. Although Dr. Harkin had occluded that lobe, the air leak did not stop entirely.
“We decided to occlude an area in the middle lobe,” Dr. Harkin says. “The leak stopped 100 percent. Sometimes, you achieve 90 percent improvement, but once we determined it was collateral ventilation and put the valve in there, it worked like a charm.”
Dr. Harkin performs approximately three to five valve implant procedures annually, and each must receive internal review board approval. The majority of the procedures he performs are off-label, involving patients with spontaneous ruptures. Generally, the valves are removed within six to eight weeks, but there are exceptions, such as among patients with advanced metastatic cancer who have a life expectancy of months.
“We believe there is a real benefit to patients being able to go home or into hospice without a chest tube, which improves their quality of life significantly in their remaining time,” Dr. Harkin says.
Dr. Harkin would like to see the valves receive FDA approval for all types of air leakage, such as those affecting patients with emphysema or asthma or those who are on mechanical ventilation.
Asthma and an IL-4 Alpha Blocker
Trial Examines New Approach to Disrupt Disease Pathways
Mount Sinai researchers are studying an interleukin 4 receptor alpha blocker to see whether it can benefit patients with severe asthma who have underlying type 2, or eosinophilic, inflammation of the airways.

“If you block one or the other cytokine individually, you do not completely block activity in the axis, because the receptors have different subunits, and thus blocking either of the mediators themselves does not completely block signaling in the joint pathway,” Dr. Rogers says.
“Dupilumab blocks a subunit that is common to the receptor for both IL-4 and IL-13, so it may be a more complete blocker of both cytokines than drugs that block IL-4 or IL-13 individually.”
Although the blocker is anticipated only to be effective for asthma patients with underlying type 2 inflammation, Dr. Rogers says the clinical trial was open to anyone with severe asthma whose current therapies are failing. The study will be monitoring patients with type 2 asthma in particular to see whether commonly available biomarkers predict their response to the drug.
“Any manufacturer would be pleased to see that a therapy was effective in a broader population than anticipated, so Sanofi-Regeneron is allowing patients to participate regardless of their biomarker status,” Dr. Rogers says. “The common type 2 inflammation biomarkers used in clinical practice are peripheral blood eosinophil counts and fraction of exhaled nitric oxide, but we will also be looking at other potential blood markers that are not currently as well validated clinically.”
Patients participating in the study will receive either a dupilumab or placebo injection every second week—one in the clinic during monthly visits and one that they will administer at home. Using handheld electronic diaries, participants will keep records of their symptoms and the other asthma medications they are taking, and they will record their lung function with peak flow meters between and during clinic visits. They will also be monitored for side effects through ongoing tests of basic organ function. At the end of the clinical trial, patients who received the placebo and completed all of the study requirements will have access to the therapy.
In addition to focusing on asthma, the development program for the dupilumab therapy includes clinical trials for two other allergy and respiratory targets: chronic rhinosinusitis (specifically nasal polyps) and eczema.
“The diseases for which the manufacturer is developing the therapy are actually often interrelated,” Dr. Rogers says. “For example, there are patients who have severe allergies and also have severe eczema and asthma. Even though we already have some advanced therapies for these patients, not everybody responds to them. This therapy offers the potential of another way to treat them without the risk of damage from oral corticosteroids.”
The success of the clinical trial would also confirm the value of molecular phenotyping in determining optimal asthma treatment, particularly for a subset of patients who have not traditionally benefited from conventional therapies.
“Asthma is such a common illness that it probably has a prevalence of anywhere between 7 and 10 percent of the population. Approximately 5 to 15 percent of those patients are very severe and don’t respond to treatment, so you are looking at millions of people who could ultimately be helped.”
How Sleep and Disease Interact
Studying Links Among Apnea, Heart, and Brain Function
Most of us spend one-third of our lives sleeping, but we have very little understanding about how sleep affects us or how it interacts with various diseases. These are the mysteries David M. Rapoport, MD, Professor of Medicine in the Division of Pulmonary, Critical Care and Sleep Medicine, is working to unravel as Research Director of the Mount Sinai Integrative Sleep Center.

One of several recent high-profile hires at the Center, Dr. Rapoport, together with his colleagues, is exploring the causes, epidemiology, treatments, and consequences of sleep disruption due to sleep apnea—defined as brief or prolonged pauses in breathing. His own interests include developing new ways to deliver continuous positive airway pressure, or CPAP, the most widely used treatment for sleep apnea, which involves a blower and a mask worn at night; identifying new treatments for sleep apnea other than CPAP; and understanding the causes and treatment of an infrequent variety of sleep apnea that occurs in the obese—the obesity hypoventilation syndrome. These patients don’t breathe enough while asleep but may not have complete stoppages like apneics. They need a breathing machine and special settings different from CPAP.
Among other interesting studies are those led by Indu Ayappa, PhD, involving a cohort of World Trade Center first responders who exhibit an extraordinarily high incidence of sleep apnea compared to the general population.
“Our main goal is to better understand what happened to cause sleep apnea in this cohort, not only so that we can treat them but also because there are generalizable lessons to be learned that we could apply in other situations involving first responders or air pollution,” Dr. Rapoport says.
One observation is that many in this cohort have chronic rhinosinusitis, but tests to date, including measurements of daytime nasal-passage resistance, have not found a strong relationship between apnea and chronic rhinosinusitis. A more encouraging observation is that the sleep apnea experienced by this cohort is mainly positional apnea.
Dr. Rapoport says that his team has been training patients to change sleep position using Night Shift, a vibro-tactile positional therapy device manufactured by Advanced Brain Monitoring. “More than one-third of these patients are nearly cured by sleeping on their sides,” he notes.
The Center is also involved in studies on how apnea affects heart and brain function. Neomi Shah, MD, MPH, is leading the heart studies, looking at whether treating heart failure first is more effective than first treating central sleep apnea, a condition where the brain stops sending signals to the muscles that control breathing. She is also following a group of patients who recently have had small heart attacks to see whether obstructive sleep apnea contributes to heart failure or is a marker of other risk factors, such as hypertension.
Perhaps their most interesting observation to date is that mild obstructive sleep apnea may decrease the severity of a heart attack. “Clearly, the apnea predisposes you to have the attack, but the theory is that the intermittent cessation of breathing may be training the muscle to be resistant to the total lack of oxygen that occurs when you cut off a blood vessel,” Dr. Rapoport says.
Andrew W. Varga, MD, PhD, is leading the research on how sleep disruption impacts brain function. One study is looking at the consequences of apnea-related sleep disruptions to determine the role they play in memory and learning deficits, and particularly how this might affect the development of Alzheimer’s disease.
“Certain proteins, such as amyloid beta, are thought to be involved in the degeneration of the brain that we call Alzheimer’s disease,” Dr. Rapoport says. “During the day, they build up in the brain, but at night they drop down. Disrupting sleep interferes with this process, so there’s a very exciting possibility that we may have found something that explains the association between sleep disorders such as apnea and the progression of this disease.”
Compact Device Keeps Airway Open
Novel Treatment for Tracheomalacia That Mimicked COPD
Dorothy Frontiero had always been active, enjoying jogging, skiing, and tennis. But 15 years ago, the 83-yearold Raleigh, North Carolina, resident began experiencing shortness of breath during exercise, which gradually worsened to the point where she found herself gasping for air just walking around her house.
Ms. Frontiero consulted a wide range of specialists who each offered different diagnoses for the underlying cause of her condition, including mitral valve disease, asthma, chronic obstructive pulmonary disease (COPD), and sleep apnea. Treatments were recommended and pursued, but nothing seemed to help. Frustrated with the lack of clarity and progress on her shortness of breath, Ms. Frontiero reached out for help to The Mount Sinai Hospital in March 2016.
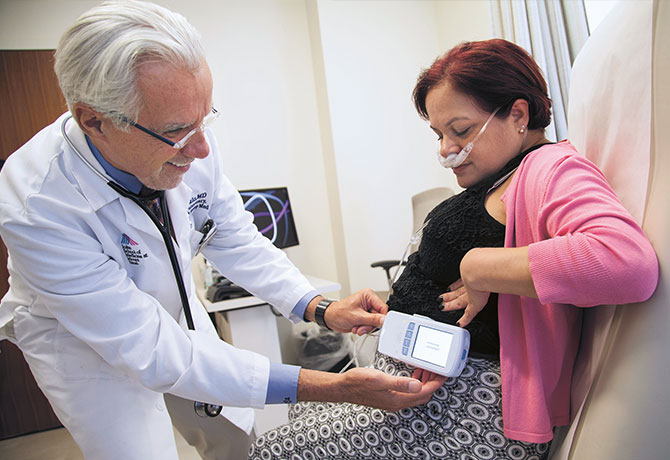
After reviewing eight years of medical records, Louis DePalo, MD, Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine at Mount Sinai, launched a multidisciplinary evaluation of Ms. Frontiero’s breathing problems, collaborating with experts at the Mount Sinai – National Jewish Health Respiratory Institute in asthma, allergies, sleep, cardiology, and ENT. A series of tests ensued, including those to check for sleep apnea and to evaluate inspiratory and expiratory force and pressure, as well as a dobutamine stress echocardiogram. But apart from finding signs of weakened muscles, Dr. DePalo was no closer to discovering the source of her breathing problems. He began thinking about conditions that mimic COPD and asthma and ordered a chest CT scan to look for tracheomalacia, a condition in which the trachea collapses during periods of increased airflow.
“Most CT scans are done with the lungs fully inflated, but that doesn’t help for tracheomalacia, because the airway is dilated and looks totally normal,” Dr. DePalo says. “We decided to do an expiratory maneuver and discovered that there was a dynamic airway collapse.” A 3D reconstruction of the trachea further confirmed the new diagnosis and helped illustrate the nature of the problem for Ms. Frontiero.
Treating Ms. Frontiero’s acquired tracheomalacia proved challenging for several reasons. For one, she was considerably overweight, but she also had kyphosis, which had not been addressed or treated. Although the kyphosis in itself presented obstacles to her recovery, Ms. Frontiero’s weight and shortness of breath created a vicious cycle that complicated treatment until Dr. DePalo suggested a novel solution: the Life2000™ system. Developed by Breathe Technologies mainly for end-stage COPD patients, Life2000 is a fully positive pressure ventilator that not only has a low profile on the face but is also compact enough that it can be worn on the hip.
“We had done a couple of inpatient trials, and based on those, I thought it would work for her,” Dr. DePalo says. “But it wasn’t covered by Medicare because it was a new technology and was going through the regulatory process. We were able to source a device and provide training and technical support. Now, when she breathes in, her airway is not closing off, and that means she’s able to do more physical activity.”
Ms. Frontiero is participating in a local pulmonary rehabilitation program and has regained mobility to the point where she has been able to enjoy extended walks with her husband. Relieved that she is finally making progress, Ms. Frontiero is looking forward to continuing to be a patient of the Mount Sinai – National Jewish Health Respiratory Institute.
Message from the Chief: Charles A. Powell, MD
The last few years have been extraordinary for the Division of Pulmonary, Critical Care and Sleep Medicine at the Mount Sinai Health System.

The Mount Sinai – National Jewish Health Respiratory Institute opened its permanent home on the Mount Sinai campus in late 2016. With the Institute, we have created a model for delivering patient-centered, multidisciplinary, state-of-the-art care for patients with simple and complex respiratory diseases. For out-of-town referrals, we provide comprehensive multiday visits for the evaluation and treatment of undiagnosed respiratory diseases. For all patients, we provide an interdisciplinary team with physicians from Gastroenterology, Cardiology, Otolaryngology, and Rheumatology.
We also have the largest sarcoidosis program in the Northeast, directed by Adam Morgenthau, MD, and a long tradition of sarcoidosis research and treatment. In this report you will read about two complex cases that were managed by the Clinical Director of the Respiratory Institute, Louis DePalo, MD.
Also in this report, we feature the achievements of our lung cancer research program, which has identified key molecular pathways that are activated in the progression of adenocarcinoma from indolent tumor to metastatic tumor—an increasingly important focal area as efforts to detect early-stage lung cancers with chest CT screening begin to pay off.
We are pleased to present our innovative efforts in off-label device use, including the placement of lung valves to treat surgical leaks and a fully portable positive pressure ventilator that helped treat a difficult case of tracheomalacia.
Our ongoing research programs include a clinical trial of an interleukin 4 receptor alpha blocker that may provide a more effective way to block cytokines in asthma patients with underlying type 2 inflammation.
Finally, we write about the new Mount Sinai Center for Integrative Sleep Medicine. Under the direction of two world-renowned recruits, David Rapoport, MD, and Omar Burschtin, MD, this center will unify clinical and research information from outpatient and inpatient sleep studies across the Mount Sinai Health System.
This is just the tip of the iceberg of what’s being done in the Division of Pulmonary, Critical Care and Sleep Medicine at Mount Sinai. I’d be happy to answer any questions; you can reach me anytime directly via email at charles.powell@mssm.edu.
Charles A. Powell, MD, Janice and Coleman Rabin Professor of Medicine
Chief, Catherine and Henry J. Gaisman Division of Pulmonary, Critical Care and Sleep Medicine
CEO, Mount Sinai – National Jewish Health Respiratory Institute
@CAP_MSNJHRI
Division of Pulmonary, Critical Care and Sleep Medicine
Download the Winter 2017 Specialty Report