Researchers Discover That Kidney Disease Gene Affects More Populations Than Previously Thought
Until now, studies on the APOL1 gene have primarily focused on African and African American populations
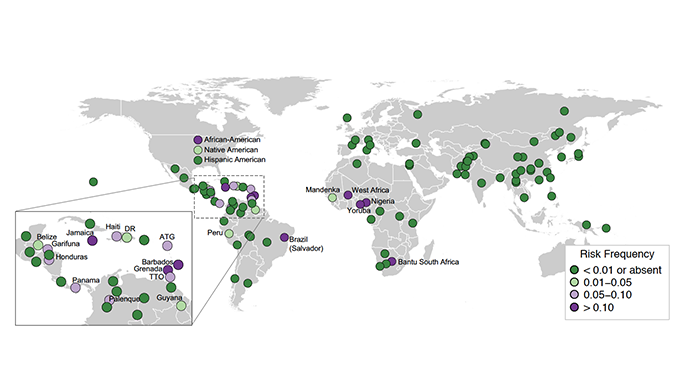
In the largest population genomics investigation to date, a team of researchers at the Icahn School of Medicine at Mount Sinai, Stanford University, and the University of Colorado have discovered that kidney disease risk variants of the gene APOL1, previously known to affect African and African American populations, are also found at appreciable frequencies in Caribbean and Latin American populations. Because these populations are historically under-studied and under-tested in connection with APOL1, the gene’s impact on these populations is currently unknown. The findings were described in a publication released today in The New England Journal of Medicine.
Risk variants in the APOL1 gene were first discovered in African Americans. Consequently, much of the research studies and clinical trials that followed have been heavily focused on self-reported African or African American populations. Knowing this, researchers in the study decided to link genetic and demographic data spanning more than 110 populations, leading to the discovery of APOL1 risk variants in other populations who share ancestry from Africa, such as those who are Hispanic or Latino.
“This finding is crucial in early detection of at-risk individuals who may not be indicated for genetic screening due to self-reporting of ethnic origins, but may still be at high risk due to the presence of APOL1 risk variants,” said Girish Nadkarni, MD, Assistant Professor of Medicine (Nephrology) at the Icahn School of Medicine and first author of the study. “It is important to more fully understand the global distribution of these variants based on country of origin and genetic ancestry rather than self-reported race/ethnic group.”
Knowing that the APOL1 risk is present in these populations could help physicians tailor treatment more closely to their needs, an example of the approach known as precision medicine. The team’s data also provides a centralized resource to help the medical community better understand at-risk kidney disease populations worldwide.
“APOL1 is the poster child for precision medicine, as the risk variants have a large impact on lifetime risk for not only kidney disease, but also early onset hypertension and cardiovascular disease,” said Eimear Kenny, PhD, Associate Professor of Genetics and Genomic Sciences at the Icahn School of Medicine at Mount Sinai, Director of the Center for Genomic Health, and senior author of the publication. “Here at Mount Sinai, we are leading national efforts to learn about the impact of APOL1 risk variants in routine clinical settings, and the gene is currently under intense scrutiny as a therapeutic target and across diverse populations.”
This study is supported by grants from the National Human Genome Research Institute and the National Heart, Lung, and Blood Institute.
N Engl J Med 2018; 379:2571-2572.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.