
Catherine and Henry J. Gaisman Division of Pulmonary, Critical Care and Sleep Medicine
We provide state-of-the-art consultation, diagnostic testing, and clinical and multidisciplinary care to patients with simple and complex respiratory and respiratory-related diseases.
Catherine and Henry J. Gaisman Division of Pulmonary, Critical Care and Sleep Medicine
Compassionate, seamlessly coordinated care and groundbreaking research go hand in hand at the Mount Sinai Health System.
This specialty report highlights:
- Easing the transition to adulthood
- Monoclonal antibodies show promise for severe asthma
- Seventy years of experience with sarcoidosis
- ED and ICU collaborating in acute lung injury trials
- A new textbook that gives the basics of ventilation
- The Respiratory Institute continuing to grow
- Message from the Chief: Charles A. Powell, MD
Easing the Transition to Adulthood

The transition to adulthood is typically a complicated rite of passage for any adolescent to navigate, but it is even more challenging for young people with a pulmonary condition, who must leave the doctor they’ve known their whole life to start seeing an adult specialist.
“Patients are often reluctant to leave the comfort of a lifelong physician because of what they see as an arbitrary rule,” says Alfin Vicencio, MD, a Professor of Pediatrics at the Icahn School of Medicine at Mount Sinai. “Given that many children’s hospitals are freestanding, patients are essentially shifting to an environment that is unfamiliar to them with the added risk that there will not be a good continuance of care. That can lead to psychological discomfort, causing patients to feel alienated or become lost to care.”
That has not been the case at the Mount Sinai Health System, which has long set standards for successful pediatric-to-adult pulmonary care transitions. This legacy inspired Dr. Vicencio to make his own transition to Mount Sinai in 2012. As Chief of the Division of Pediatric Pulmonology and Vice Chair for Clinical Affairs and Strategy for the Department of Pediatrics at the Icahn School of Medicine and Mount Sinai Kravis Children’s Hospital, he has considerable insight into what makes Mount Sinai unique in addressing the uncertainty and reluctance often associated with pulmonary patient transitions.
“In my experience, pediatric and adult specialists rarely cross paths,” says Dr. Vicencio. “Here, interaction is actively pursued, and that is enabled in large part by the fact that this is an integrated health care system. That encourages communication and collaboration among our specialists, enabling us to make progress in helping patients make this shift.”
Dr. Vicencio says that progress is exemplified by the hospital’s joint bronchoscopy program. “I have always been interested in bringing high-level adult procedures into the pediatric population,” he says. “Mount Sinai’s shared bronchoscopy suite, equipment, and expertise enabled our specialists to work together to the point where our pediatric specialists now have the capacity to perform these practices on their own.”

Mount Sinai has also distinguished itself from other New York health systems in that young cystic fibrosis, severe asthma, and sleep disorder patients are able to continue receiving care in the same space once they become adults. “Having a shared facility removes a significant psychological barrier to making this change,” says Patricia Walker, MD, a Co-Director of the Cystic Fibrosis Center at Mount Sinai Beth Israel and an Assistant Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine. “Patients feel confident because they get to interact with the same staff at the same location.”
“We can also introduce patients to the adult specialists who will eventually take over their care,” says Maria Berdella, MD, Director of the Mount Sinai Cystic Fibrosis Pediatric Program and an Assistant Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine. “Additionally, we have a nurse practitioner who helps our adolescent patients learn the fundamentals of self-care.”
Transitions are even more straightforward for Mount Sinai patients with sleep disorders, according to Jason Bronstein, MD, an Assistant Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) and Pediatrics at the Icahn School of Medicine. “Because I specialize in both pediatric and adult sleep medicine, I am essentially transitioning them to myself,” he says. “But there are instances where I need to transition a patient to an adult pulmonologist or another specialty. Our integrated system means I have access to providers with a background in both adult and pediatric care, and they have access to my patients’ medical records, which ensures there are no gaps in therapeutic treatments.”
Mount Sinai researchers are also making significant headway in enhancing pediatric-to-adult transitions by exploring pulmonary disease onset and progression. One study, conducted by the Mount Sinai Institute for Exposomic Research and published in the May 2018 edition of The Journal of Allergy and Clinical Immunology, is the first to demonstrate that increased prenatal exposure to air pollution and maternal stress significantly increases the risk for developing childhood wheeze, childhood asthma, and impaired lung function.
“The more we learn about the development of chronic pulmonary diseases in adulthood, the more we understand that many have their origins early in life, including during pregnancy,” says the study’s lead author, Alison Lee, MD, MS, an Assistant Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) and Pediatrics at the Icahn School of Medicine. “By identifying the environmental exposures that increase the risk for developing or exacerbating existing respiratory illness, we have the potential to reduce those exposures and decrease disease in both childhood and adulthood.”
Dr. Lee’s work exemplifies Mount Sinai’s continued innovations in pediatric-to-adult pulmonary patient transitions, says Charles A. Powell, MD, Chief of the Division of Pulmonary, Critical Care and Sleep Medicine. “By embedding research into our clinical programs, we are able to offer patients more therapeutic options to help them better manage their disease regardless of age or stage,” he says. “The mission of the Mount Sinai – National Jewish Health Respiratory Institute is to improve lung health across the age continuum through innovative clinical programs and research. At Mount Sinai, we are fortunate to have colleagues with a shared vision and the institutional commitment and resources to deliver this unique model of care to adults and youths.”
Monoclonal Antibodies Show Promise for Severe Asthma
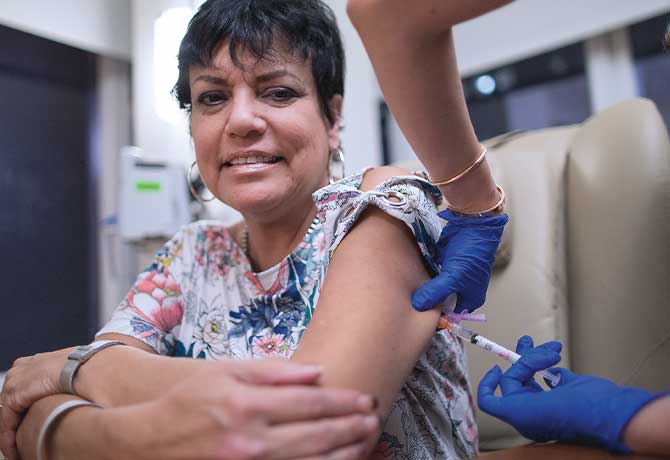
Approximately 5 to 10 percent of asthma patients have a severe form not controlled by standard inhaled therapies. They often require repeated courses of oral corticosteroids for acute flares of asthma, or chronic oral corticosteroids that put them at risk for steroid-related health complications. But new advanced therapies are demonstrating considerable promise in controlling asthma, and the Mount Sinai – National Jewish Health Respiratory Institute has positioned itself as a leader in offering these therapies to patients.
One therapy, omalizumab, a monoclonal antibody to immunoglobulin E (IgE), blocks one of the central features of the allergic asthma pathway and is effective in patients with severe allergic asthma. For patients who do not respond to or are not eligible for anti-IgE therapy, there are antibodies that inhibit the interleukin-5 pathway and block the production and migration of eosinophils to the airway, either by acting directly on the cytokine (mepolizumab or reslizumab) or at its receptor (benralizumab).
Linda Rogers, MD, an Associate Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine at Mount Sinai and Director of Mount Sinai’s Clinical Asthma Program, notes that these biologics have enabled patients to either reduce their daily dose of oral corticosteroids or completely stop taking them, in addition to reducing the frequency of asthma exacerbations.
“Oral corticosteroids target multiple pathways, so it is very much a broad approach to treatment,” Dr. Rogers says. “But patients are at a high risk of side effects such as osteoporosis, infections, cataracts, diabetes, and high blood pressure. On the other hand, monoclonal antibodies target specific pathways involved in eosinophilic and type 2 inflammation to reduce the need for oral corticosteroids, and thus reduce the risk of steroid-related complications.”
Patients who have uncontrolled symptoms or two or more exacerbations per year, or who are oral corticosteroid dependent, should be considered for advanced asthma therapies. At the Mount Sinai Therapeutic Infusion Center, these patients receive targeted therapies under medical supervision. “Because we have a large volume of patients, we have a cohort that has cycled through multiple drugs, and we are studying a variety of patient characteristics to better understand predictors of response to therapy,” Dr. Rogers says.
The ability to more accurately target which of the new therapies is best for a particular patient may soon be possible, Dr. Rogers says.
She cites a new partnership between Mount Sinai, Sema4, and Sanofi that will use systems biology approaches to understand differential responses to therapy and enable better selection of treatments.
Moreover, another class of biological treatments for asthma, anti-interleukin-4-receptor alpha (dupilumab), was recently approved by the U.S. Food and Drug Administration. The Mount Sinai – National Jewish Health Respiratory Institute Asthma Program participated in phase III clinical trials of this drug.
Dr. Rogers says the asthma program, in collaboration with Timothy Harkin, MD, an Associate Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine, and the interventional pulmonology program, will make bronchial thermoplasty available for severe asthma patients. Bronchial thermoplasty is a technique that uses radio frequency energy to ablate airway smooth muscle in order to improve the airway hyperreactivity that is a feature of asthma.
“This is an exciting time to be working in asthma,” Dr. Rogers says. “We hope that with all of these new options, we will be able to help patients who have previously been unable to get their asthma under control.”
With Sarcoidosis, 70 Years of Experience
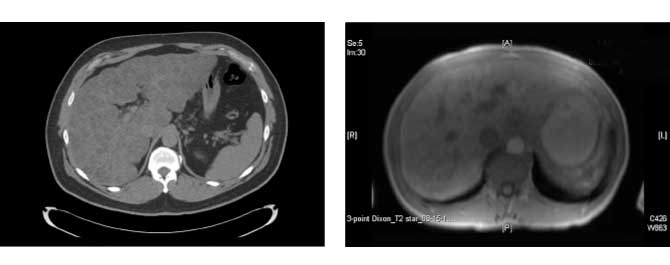
Adam Morgenthau, MD, does not hesitate when asked what has made the Mount Sinai Health System’s Sarcoidosis Program one of the largest in the world.
“For more than 70 years, we have seen the most complex, severe, and chronic cases, and that is invaluable because there are very few data to guide us in our decision making for this enigmatic disease,” says Dr. Morgenthau, an Associate Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine and the Director of Mount Sinai’s Sarcoidosis Program.
“The ability to achieve positive patient outcomes comes down to experience, training, and practice, and we have those,” says Dr. Morgenthau.
Established in 1948 by Louis Siltzbach, MD, Mount Sinai’s Sarcoidosis Program has enrolled 18,000 patients to date, and it continues to grow at a vigorous pace, welcoming approximately 40 new patients each week at the Mount Sinai – National Jewish Health Respiratory Institute and the Sarcoidosis Center. Patients receive comprehensive treatment through a multidisciplinary approach that includes consultations with specialists in fields such as cardiology, dermatology, and neurology.
“Most of our patients have multi-organ disease, which means they are seeing as many as five different doctors,” Dr. Morgenthau says. “That creates a significant risk for fragmentation in care. But we have access to these specialists at Mount Sinai, so we are able to oversee and direct patient care to ensure there are no gaps.”
The Sarcoidosis Program has distinguished itself in many ways over the years. It has been a leader in the use of immunomodulatory medication therapies to reduce the side effects of prednisone, and has developed several unique protocols, tools, and criteria for diagnosing and assessing the disease. These include the noninvasive Kveim-Siltzbach diagnostic skin test, an algorithm that greatly reduces uncertainty in making a diagnosis, and a sarcoidosis severity score that facilitates care management decisions. “Our goal is to administer exceptional patient care in a standardized fashion that also accommodates patients’ preferences, allowing for individualized treatment plans,” Dr. Morgenthau says.
Treatment plans typically incorporate a range of resources and initiatives to engage patients in managing the disease and its symptoms. One particularly successful initiative is the Program’s patient-run support group, which provides a forum for patients, family members, and caregivers to share experiences, advice, and news about advances in sarcoidosis diagnoses and therapies.
“The support group is an opportunity for patients to engage with their health care providers outside the context of the traditional consultation,” Dr. Morgenthau says. “It’s an invaluable opportunity to better understand their perspectives and concerns, and use this information to enhance care delivery.”
Inspired by the considerable progress that the Mount Sinai Sarcoidosis Program has made in terms of patient care over the past seven decades, Dr. Morgenthau sees room for continued improvement. Drawing on Mount Sinai’s status as a National Institutes of Health Center of Excellence for research in sarcoidosis, he is looking to increase the Program’s participation in research and clinical trials. Dr. Morgenthau will be conducting data analysis for a retrospective study of patients with hepatic sarcoidosis to determine whether features of the liver histology correlate with disease severity and outcomes. He will also serve as a co-investigator for a phase III clinical trial that will explore his hypothesis that the drug KIACTA (eprodisate disodium) can attenuate the development of granulomatous inflammation in sarcoidosis.
“I want to develop a research infrastructure that complements our robust clinical program,” Dr. Morgenthau says. “I am also interested in developing more concentrated multidisciplinary care that enables patients to see multiple specialists on the same day. Through these efforts, we will remain on the cutting edge in providing patient care.”
ED and ICU Collaborate in Acute Lung Injury Trials

Mortality rates related to acute respiratory distress syndrome (ARDS) have remained high since the syndrome was first defined more than 50 years ago. The Mount Sinai Hospital is helping to advance ARDS research and clinical care as the only Manhattan-based hospital participating in the Clinical Trials Network for the Prevention and Early Treatment of Acute Lung Injury (PETAL).
Funded by the National Heart, Lung, and Blood Institute, PETAL is a network of 12 clinical centers (each comprising several hospitals) and one clinical coordinating center that is designing and conducting randomized controlled clinical trials of new treatments and practices that could improve outcomes among patients at risk for ARDS. Mount Sinai has distinguished itself among participating hospitals, in part through the highly collaborative relationship of its emergency department (ED) and intensive care unit (ICU). Kusum Mathews, MD, a PETAL co-investigator at Mount Sinai, has helped to lead the implementation of the network’s four clinical trials to date.
“To work on clinical trials spanning the patient’s hospital course, it is crucial that the ED be on the same page as the ICU,” Dr. Mathews says. “Because we have a long history of research-based collaboration at Mount Sinai, we were able to integrate our departments’ research infrastructure to facilitate patient recruitment and enrollment. We also established a joint approach to protocol implementation and training to ensure we follow the same procedures and that we maintain the same standard of care when we transfer patients from the ED to the ICU.”
Mount Sinai has also distinguished itself among PETAL hospitals as a leader in health informatics and data mining through EPIC, its electronic medical records system. In one study, LOTUS FRUIT, a multicenter prospective observational cohort feasibility study assessing ventilation practices, Mount Sinai was one of only five participating hospitals that had the capability to efficiently identify intubated patients and extract data for analysis using electronic medical records.
“As in many clinical trials, there was a lot of data to be collected and analyzed in that study,” Dr. Mathews says. “That poses significant limitations in the number of patients you can enroll if you are handling data manually, and you can lose some of the granularity that is vital in answering research questions. Mount Sinai is a research and data powerhouse. We have a depth of expertise in data gathering, extraction, and analysis that has led to better care for our patients, and that has enabled us to be a successful partner in the PETAL Network.”
Dr. Mathews says Mount Sinai is actively working within the PETAL Network to incorporate more health informatics capacity into future studies, and is partnering with participating hospitals to determine how they can enhance their data query and extraction capabilities.
She adds that Mount Sinai’s participation in PETAL has garnered considerable attention, and the strong research infrastructure facilitates successful collaboration in other multicenter clinical trials.
“I think our participation in PETAL demonstrates that we have the research capacity and academic focus to support these studies,” Dr. Mathews says. “We are committed to being at the forefront of interventions that will lead to better patient outcomes in cases involving ARDS.
New Textbook Gives the Basics of Ventilation

When Hooman Poor, MD, could not find a clear, concise resource to help his residents, fellows, and medical students comprehend the functionality and applications of mechanical ventilation, he decided to create one.
Published by Springer in both paperback and Kindle editions in summer 2018, Basics of Mechanical Ventilation takes a unique approach to outlining the essentials of mechanical ventilation. Dr. Poor, Assistant Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) and Cardiology at the Icahn School of Medicine at Mount Sinai, uses the mechanics of spontaneous breathing as a starting point to provide insights into the anatomy of a ventilator- delivered breath, the modes that control how the device functions, the best practices for management of disease states such as acute respiratory distress syndrome, and the safest ways to wean patients off mechanical ventilation. Dr. Poor also created a series of simple diagrams to illustrate and enable comprehension of key mechanical ventilation concepts and equipment functionality.
“There are a lot of very informative textbooks written on this topic,” Dr. Poor says. “I read many of them during my residency and fellowship and found most were extremely long and dense, with content that medical students might not comprehend. I wanted to create something approachable that facilitates a deep understanding and appreciation of how a ventilator works. The result is a textbook that I wish had existed when I was a trainee.”
In describing the mechanisms and theories of mechanical ventilation, Dr. Poor addresses various issues and misconceptions regarding its use. Many arise from the lack of consistent and clear nomenclature for ventilator operation and modes. For example, Dr. Poor has noted that the prevailing wisdom regarding volume-controlled ventilation is that the ventilator does all the work of breathing, which is not necessarily the case. He has also observed considerable confusion around the term “assist-control,” which is assumed to be a mode that always provides full ventilatory support to patients. But it is really just a hybrid triggering algorithm that delivers an “assist” breath if triggered by the patient, or a “control” breath if the patient does not trigger a breath within a specified time frame.
“Because there is no consistent language when discussing ventilators, it is hard for fellows, residents, and medical students to grasp the concepts behind mechanical ventilation, and it leads to confusion, which can impact patient outcomes negatively,” Dr. Poor says.
The textbook also explains the underlying interactions between a ventilator and a critically ill patient, which have become particularly acute as current guidelines recommend using as little sedation as possible for patients receiving mechanical ventilation.
“Because patients are now awake, they are using their respiratory muscles and are participating in the breathing process,” Dr. Poor says. “Their breathing and the ventilator need to be coordinated and synchronous; otherwise, the patient can become very agitated and uncomfortable, and paradoxically, the effort to breathe may actually increase. By focusing on this interaction and addressing ventilation misconceptions, this textbook will enable physicians to make informed decisions about clinical applications, which will lead to positive outcomes.”
Dr. Poor says it took approximately three years of work to complete the textbook, which draws on several sources for theories and best practices, as well as his own expertise in mechanical ventilation and his five years of experience as an instructor at the Icahn School of Medicine. He also provided early drafts to medical students, residents, and critical care fellows to solicit their feedback, and the questions they asked during rounds also informed the content.
“My goal was that a fourth-year medical student would be able to understand everything in this textbook,” Dr. Poor says. “I hope those who read it will have a deeper understanding of how a ventilator works, ultimately improving patient care for critically ill patients.”
Respiratory Institute Continues to Grow

It did not take long for the Mount Sinai – National Jewish Health Respiratory Institute to earn a reputation as the leader in cutting-edge diagnosis and treatment of simple and complex lung diseases among pulmonary patients in the New York City area.
“We opened the Respiratory Institute in mid-2015 with a multidisciplinary approach and staff, and as of 2017, we were averaging 22,000 patient visits per year,” says Charles A. Powell, MD, Chief of the Division of Pulmonary, Critical Care and Sleep Medicine at the Mount Sinai Health System. “That is a huge growth from the 8,500 patient visits we were able to accommodate at our single-specialty practice at The Mount Sinai Hospital, and it has made us the largest respiratory practice in the city.”
Combining National Jewish Health’s extensive clinical and research expertise in lung diseases with Mount Sinai’s experience in genomic health population research and bench research in immunology, the Respiratory Institute is setting standards for pulmonary disease research, clinical expertise, and outcome-driven care. It is also, to Dr. Powell’s knowledge, the first multidisciplinary respiratory-focused partnership in the country.
“We have pulmonologists working alongside cardiologists, thoracic surgeons, rheumatologists, and allergists,” says Dr. Powell, who is the Janice and Coleman Rabin Professor of Pulmonary Medicine at the Icahn School of Medicine at Mount Sinai. “That is unique. We have embedded nurse educators and social workers who are not only able to help our patients adjust to life with respiratory disorders, but are also available to answer any subsequent questions patients have about their disease or treatment. Those are just a few reasons why patients and their referring providers are increasingly choosing us.”
Under Dr. Powell’s leadership, the Institute has established itself as an early adopter of innovative diagnostic tools and therapies. These include fiber-optic laryngoscopy, used to evaluate respiratory disease symptoms in patients with chronic cough, severe asthma, chronic obstructive pulmonary disease (COPD), and lung fibrosis. Another diagnostic device is ResTech, a minimally invasive esophageal probe that enables same-day diagnosis and treatment of symptoms such as chronic cough and reflux. Through the Mount Sinai Therapeutic Infusion Center, the Respiratory Institute is offering advanced therapy options to patients whose asthma is not controlled by conventional inhaled therapies. And it has partnered with Itamar Medical in the development of a next-generation version of WatchPAT— an easy-to-use watch-like portable sleep diagnostic device.
Recognizing that research enables clinical innovation, Dr. Powell and his colleagues at the Respiratory Institute are also advancing the science of respiratory disease diagnosis and treatment. He is collaborating with David Yankelevitz, MD, a Professor of Radiology at the Icahn School of Medicine, on a National Institutes of Health R01-funded study to identify key biological pathways that distinguish aggressive lung cancers from indolent early-stage lung cancers. Other projects include a collaboration involving Dr. Yankelevitz and Sidney Braman, MD, a Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School Medicine, that included analysis of CT scans of COPD patients to predict acute exacerbations and develop patient phenotypes, and multiple clinical trials being led by Maria Padilla, MD, a Professor of Medicine (Pulmonary, Critical Care and Sleep Medicine) at the Icahn School of Medicine, that could result in new approved therapies for patients with idiopathic pulmonary fibrosis.
All this activity and growth has necessitated the opening of a second location at Mount Sinai Union Square, which, based on preliminary data, is expected to average 14,000 patient visits each year. It has also inspired Mount Sinai and National Jewish Health to partner with the Thomas Jefferson University Hospital in Philadelphia to launch a similarly structured Respiratory Institute there, under the leadership of Jesse Roman, MD.
“The strategy is to eventually take what we have developed here at the Institute, and implement the same model at other locations,” Dr. Powell says. “That will mean better approaches to diagnosis and treatment, and better outcomes for patients not just regionally, but also nationwide.”
Message from the Chief: Charles A. Powell, MD
Compassionate, seamlessly coordinated care and groundbreaking research go hand in hand at the Mount Sinai Health System.

We illustrate that in this year’s cover story, which details how Mount Sinai expertly manages the transition from pediatric to adult care for a variety of conditions, from asthma to cystic fibrosis to sleep issues. As an integrated health care system that sees pediatric and adult patients on the same campus, we encourage interactions between pediatric and adult specialists to ease each child’s transition into adulthood and adult care.
That kind of seamless coordination is a hallmark of the Mount Sinai – National Jewish Health Respiratory Institute, now the largest respiratory institute in New York City, which I have had the honor of leading since 2015. The Institute has not only successfully combined National Jewish Health’s expertise in lung diseases with Mount Sinai’s strengths in genomics and immunology, but also puts pulmonologists side by side with other specialists for a smoother and more satisfying patient experience.
Our Sarcoidosis Program offers not only advanced therapies like immunomodulation, but also a successful patient-run support group in which patients and caregivers can share experiences and advice.
We continue to offer the most advanced therapies and clinical trials to our patients, including monoclonal antibodies and bronchial thermoplasty for uncontrolled asthma, and we are one of 12 clinical centers in the PETAL network conducting clinical trials for acute respiratory distress syndrome.
When it comes to ventilation, we literally wrote the book; Hooman Poor, MD, published Basics of Mechanical Ventilation in the summer of 2018.
Another important focus of our Division is developing young physician- scientists into academic leaders. In the past year, three of our junior faculty secured their first NIH independent investigator R01 awards, a key milestone in academic research career development. Neomi Shah, MD, Alison Lee, MD, and Andrew Varga, MD, demonstrate how bright, motivated physician-scientists thrive in the rich research environment of the Icahn School of Medicine at Mount Sinai and are positioned to be among the next generation of leaders in academic medicine.
As always, I’d be happy to answer any of your questions at charles.powell@mssm.edu.