ENT/Head and Neck Surgery
Our Department of Otolaryngology–Head and Neck Surgery continues its innovative spirit in all facets of patient care, research, and education.
ENT-Head and Neck Surgery
Mount Sinai Health System’s Department of Otolaryngology–Head and Neck Surgery is internationally recognized for conservation laryngeal surgery, head and neck reconstruction, and accomplishments in the diagnosis and management of HPV-associated disease and robotic head and neck surgery.
This specialty report highlights:
- Incisionless endoscopic glomus tumor removal that yields reduced pain for patients
- Virtual reality that is being used to teach students skull base anatomy and how to prepare for surgeries
- Advances in vocal surgery boosting the confidence of transgender patients
- A unique procedure that removes a vascular malformation
- Transoral robotic surgery that tackles tonsil cancer without radiation
- Personalized genomic vaccines that fight cancer
Incisionless Endoscopic Glomus Tumor Removal Yields Reduced Pain for Patients
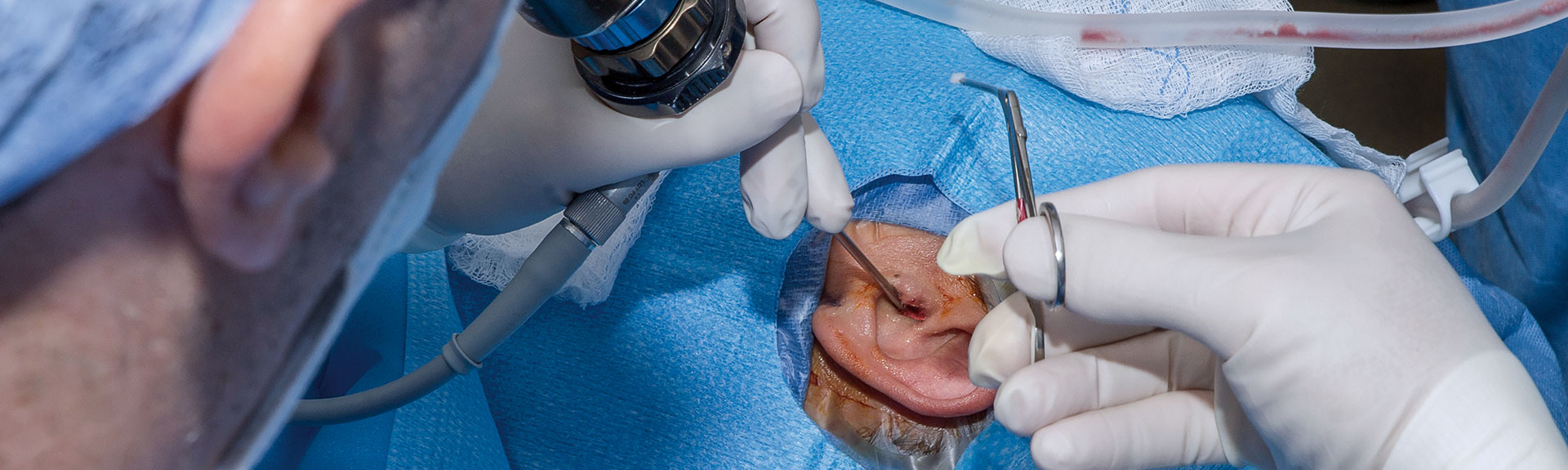
An observer catching sight of an endoscope in an otology operating room might have assumed that the case was an endoscopic tympanoplasty. However, George Wanna, MD, was actually performing an endoscopic removal of a glomus tumor. These benign, rare vascular tumors can initially present at the skull base and, over time, grow to be very large. Their removal is notoriously difficult and can be associated with complications, including swallowing issues that can lead to tracheostomy, facial nerve paralysis, and even death.
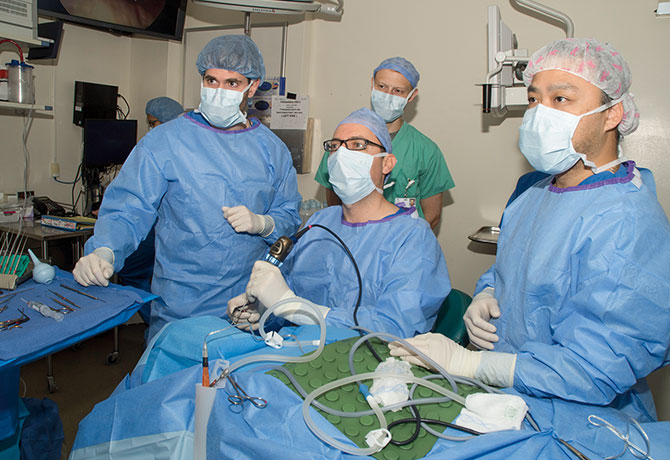
Endoscopic ear surgery was initially limited to perforations, cyst removal, and later, stapedectomy. The goals were to correct the problem without incisions in the ear, minimize the patient’s pain, enhance surgeons’ visualization, and expedite healing. For years, otologists shied away from endoscopic removal of vascular tumors, due to their rarity, complex nature, and risk of bleeding.
“I thought if I could find a tool that could suction and remove the tumor at the same time, then the bleeding would not be an issue, and surgeons could remove the tumor without patients enduring the pain and scarring associated with the surgery,” says Dr. Wanna, who is Professor and Site Chair of the Department of Otolaryngology – Head and Neck Surgery at Mount Sinai Downtown and Director of the Ear Institute at New York Eye and Ear Infirmary of Mount Sinai.
While at Vanderbilt University Medical Center, Dr. Wanna initiated aglomus tumor–removal study that entailed testing a suctioning/aspiration endoscope, which was entirely new to the market. “Five surgeries were performed at our center with no incision and no pain,” Dr. Wanna says of the clinical trial, which continued through his move to Mount Sinai. He was also the senior author of the first white paper published on endoscopic glomus tumor removal, “Utility of an Ultrasonic Aspirator in Transcanal Endoscopic
Resection of Temporal Bone Paraganglioma,” published in the Journal of Neurosurgery in February 2017, and was also an author of “Endoscopic Management of Middle Ear Paragangliomas: A Case Series” in Otology & Neurotology in March 2017.
“We at Vanderbilt and New York Eye and Ear Infirmary experienced a 100 percent success rate with all hearing improved and zero complications,” he says. “Patients no longer experienced the ringing and falsified sounds caused by these tumors.” Nationally, the study results yielded an 85 percent success rate, demonstrating that this was a safe, feasible, and effective surgical approach.
“The paradigm of this operation has changed,” Dr. Wanna says. “For those with large tumors, surgery has evolved from incisions and open surgery (possibly even two stages of surgery) to observation, partial resection, and radiation. But for smaller tumors, endoscopic removal will be adopted gradually across the country.”
So far, only a few centers nationwide treat these tumors endoscopically, but Dr. Wanna is confident that residents and fellows are surmounting a steep learning curve, and that the endoscopic approach for glomus tumor removal will become the gold standard of the future.
“Students love that what is difficult to see under the microscope can be seen clearly in high resolution on the monitor. And surgeons can explain the difference with endoscopic surgery to patients, who can visualize and understand the procedure; it greatly enhances your rapport with them. It makes the patient-physician experience wonderful.”
Immersive Virtual Reality Engages Students and Surgeons
Virtual reality (VR) may be most closely associated with the entertainment industry, but it is also being used at the Mount Sinai Health System to teach students skull base anatomy and how to prepare for surgeries. Led by Principal Investigators Raj Shrivastava, MD, and Alfred M.C. Iloreta, Jr., MD, as well as co-investigators Joshua B. Bederson, MD, Satish Govindaraj, MD, and Anthony Del Signore, MD, the IRB-approved study “Immersive Virtual Reality as a Teaching Tool for Neuroanatomy” was the first of its kind to evaluate medical students’ aptitude for skull base anatomy as well as their motivation and attitudes toward learning the material.
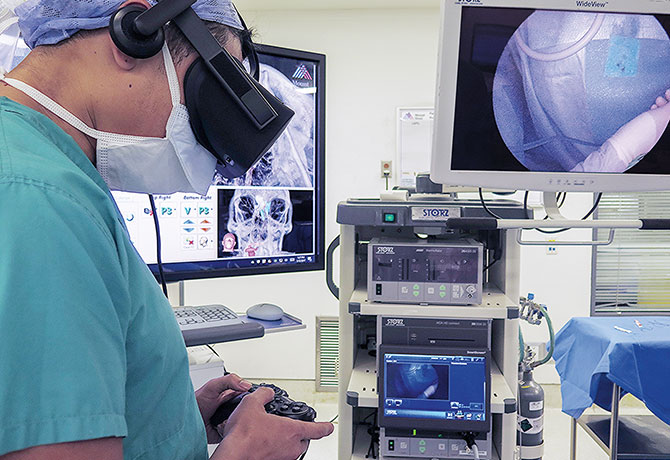
VR in the Classroom
For the purposes of the medical student study, images of normal cerebral anatomy were reconstructed from human Digital Imaging and Communications in Medicine (DICOM) files. The team merged CT and MRI imaging into a 3D VR format, which is compatible with the Oculus Rift + Touch Virtual Reality System. The ventricular system and cerebrovasculature were highlighted and labeled to formulate an interactive model. The study was performed as a randomized controlled trial of 66 students (33 each in the control and experimental groups), who studied pertinent neuroanatomical structures using either online textbooks or the VR interactive model. Their anatomy knowledge, educational experience, and motivation were then assessed.
The results demonstrated that there was no significant difference in anatomy knowledge between the two groups on pre- and post-intervention and retention quizzes. However, the VR group found the learning experience to be significantly more engaging and useful and scored significantly higher on the motivation assessment. This trial was the first study to examine the utility of next-generation immersive VR, such as the Oculus Rift, on medical student education.
VR as a Preoperative Planning Tool
Recognizing the complexity and delicate nature of many skull base tumors, Mount Sinai surgeons are using VR to ensure more precise preoperative planning and to mitigate the risk for complications. The Skull Base Surgery Center and the Department of Neurosurgery’s Simulation Core teams have taken Surgical Theater’s 3D mapping program to the next level, fusing multiple scans of individual patients’ heads and planning surgical pathways prior to procedures. This enables the team not only to practice the surgery before entering the OR but also to have clearer insights into the vascular structures that should be avoided when resecting tumors.
“Using high-resolution 3D reconstructions that enable us to simulate the surgical approach has allowed our team to anticipate any potential challenges during surgery, so we can provide our patients with the safest and most complete procedure possible,” Dr. Iloreta says.
VR in the OR
The pathology removed during skull base surgery is often surrounded by critical neuroanatomy, such as the internal carotid artery and the optic nerve. The Mount Sinai team can combine the virtualization of patient-specific anatomy with intraoperative neuronavigation. Our surgeons have access to live, real-time 3D visualization of the patient’s anatomy and the tumor’s location. “The fusion of leading-edge technologies has given us the capability to augment the view through our endoscopes and microscopes with digital reconstructions,” Dr. Iloreta says. “We have the potential to ‘see’ structures through bone or blood, to anticipate the position of critical structures, and to enhance our ability to teach other surgeons.”
To learn more about Mount Sinai’s Skull Base Surgery Center, visit www.mountsinai.org/skullbase.
Note: Dr. Bederson owns equity in Surgical Theater, LLC.
Advances in Vocal Surgery Boost Confidence of Transgender Patients
In response to a rapidly growing need, leaders at the Mount Sinai Health System recently established the comprehensive Center for Transgender Medicine and Surgery, which serves patients through all stages of their transitions. Mark S. Courey, MD, Chief of the Division of Laryngology and Director of the Grabscheid Voice and Swallowing Center of Mount Sinai, has been instrumental in ensuring that voice and communication needs are addressed for these patients. He advocates an interdisciplinary approach with close collaboration among otolaryngologists, speech-language pathologists, endocrinologists, primary care physicians, facial plastic surgeons, and psychologists.
Transgender individuals are often faced with incongruence between their voices and their identified gender. Their appearance, voice, and mannerisms form their initial presentation to the public. This discord can lead to decreased confidence and more pronounced psychological effects, such as depression.
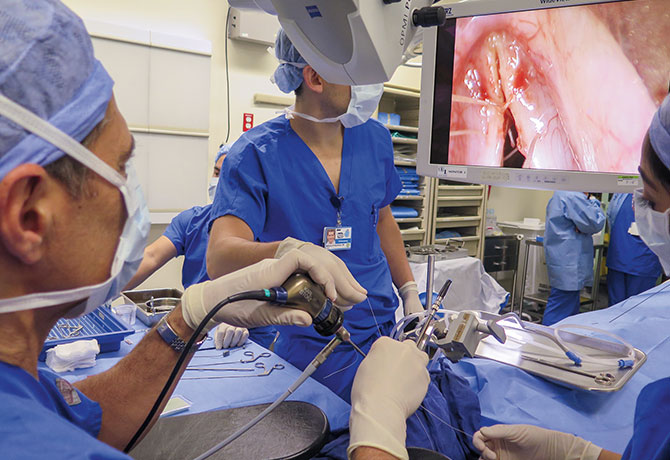
After patients have realized gains from hormonal therapies and behavioral changes in their vocal and communication mannerisms, surgical interventions such as Wendler glottoplasty, tracheal shave, and type 3 thyroplasty can improve those gains. “In my experience, this combined approach leads to more effective surgical outcomes,” Dr. Courey notes. “Patients are more likely to be satisfied with and maintain their end result from surgery if they have been successful with managing change in other areas."
Wendler Glottoplasty: Pitch-Raising Surgery
Today, the most common surgery to elevate pitch is the Wendler glottoplasty. This surgery is performed endoscopically with the mucosa removed in the anterior portion of the vocal folds, bilaterally. Extreme caution is used to create symmetric defects. Then the anterior 40 to 50 percent of the membranous vocal folds (20 to 30 percent of the entire vocal fold length) are sutured together through an endoscopic approach. The sutures must be placed symmetrically and the defect closed completely. Incomplete closure and asymmetric sutures can lead to prolonged healing and less-than-desirable outcomes with permanent vocal roughness.

“Placing the sutures symmetrically and tying them through the endoscope is a practiced skill that requires time to develop,” Dr. Courey says. “This is why it can be beneficial for these patients to see a surgeon experienced in these procedures.”
Other procedures such as the FemLar require open surgical approaches. The Wendler glottoplasty seems to produce similar results in pitch elevation without significant risks such as infection, swelling, or bleeding, with accompanying airway obstruction. Also, with the Wendler procedure, there is no external incision or scar on the neck.
Tracheal Shave: Modification of the Adam’s Apple
The appearance of the prominent male Adam’s apple, also known as the laryngeal or thyroid prominence, depends on the thickness of the patient’s neck. Typically, the thinner the neck, the more prominently the Adam’s apple stands out. Tracheal shave is commonly performed to reduce the size of this area by carefully removing only that portion of the thyroid cartilage that is visible and does not support the anterior attachment of the vocal folds. This procedure can be problematic when even experienced surgeons attempt to reduce the thyroid prominence to achieve an optimal external appearance: overly aggressive resection can lead to detachment of the vocal folds and loss of voice.
“I have seen this in my practice through referrals from experienced surgeons,” Dr. Courey says. “To avoid this potentially devastating complication, I visualize the vocal folds during the procedure, using a flexible endoscope through the laryngeal mask airway. Then I place a needle through the thyroid cartilage to determine the level of the vocal folds from the outside and then remove only the portion of the cartilage above the vocal folds. Sometimes, to achieve an optimal appearance, you need to contour the remaining portion of the cartilage. This ensures that the vocal folds are not detached and that voice is preserved.”
Type 3 Thyroplasty: Pitch-Lowering Surgery
Although most transgender men obtain enough lowering of vocal pitch through hormone-replacement therapies and behavioral modifications, some patients choose to avoid hormones for health reasons. Type 3 thyroplasty can be very effective in lowering their pitch. This is a standard Isshiki approach. However, careful consideration needs to be exercised, as the female larynx is smaller than the average male’s. Cartilage resection and anterior commissure retrusion need to be adjusted to account for this difference. Otherwise, the vocal folds can become too relaxed and the patient can lose vocal volume.
Dr. Courey cites the case of a transgender man who sought voice surgery in order to feel more comfortable in his law-enforcement job. “Prior to the surgery, the patient was not confident in his voice and felt it detracted from his ability to perform his duties,” Dr. Courey notes. “The patient was happy with his outcome. This conservative approach led to rapid healing with preserved volume and the ability to return to work confidently as a law-enforcement officer.”
Mount Sinai Student Wins First-Place Poster Award
Rocco Ferrandino, an Icahn School of Medicine at Mount Sinai medical student, won the first-place poster award for Head and Neck Surgery at the American Academy of Otolaryngology annual meeting in September 2017.
His research involves hospital readmissions in patients undergoing parathyroid surgery. He shares the honor with Yue Ma, MD, and Scott Roof, MD, residents at The Mount Sinai Hospital; Marita Teng, MD, residency program director for the Department of Otolaryngology; and Girish Nadkarni, MD, MPH, his nephrology mentor.
Unique Procedure Removes Vascular Malformation
For 16-year-old Ethan Garcia, it all started in October 2013, when his mother noticed a growth the size of a golf ball protruding from his right cheek. Thinking it was a tooth abscess, Ethan’s mom took him to a dentist, who prescribed an antibiotic to cure what she thought was an infection in Ethan’s saliva glands. Although the swelling initially went away, it returned a few weeks later and would not respond to any further treatments with antibiotics prescribed by Ethan’s pediatrician. In fact, the medication only made it worse.
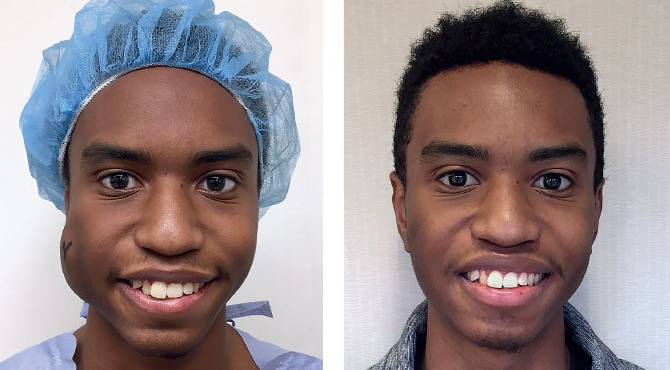
The doctors at Ethan’s local hospital concluded that it was a muscle mass or a mass of veins, and referred Ethan to an ENT specialist. However, it proved difficult to find one with the right expertise. “From January to December of 2014, my family and I were stagnant,” Ethan recalls. “We didn’t know which doctor to go to.” The swelling typically flared up in the morning, and although ice helped, eating was painful. “My friends would ask why my cheek was swollen; I wouldn’t know what to tell them because I didn’t know what it was. I didn’t want anybody to look at me because I felt that my face looked deformed and uneven,” he says.
Ethan and his family continued their search for the right specialist until finally, in the fall of 2015, he was referred to Gregory Levitin, MD, Director of Vascular Birthmarks and Malformations for the Mount Sinai Health System, and one of only a few surgeons in the country able to treat this condition.
“Reviewing Ethan’s MRI, I recognized the problem right away,” Dr. Levitin says. “It was an extensive lympho-venous malformation of the right midface that by this point had gotten quite large. Only a surgical intervention would help Ethan.”
Dr. Levitin operated on Ethan in December 2015 at New York Eye and Ear Infirmary of Mount Sinai. The operation lasted almost five hours but was a success. “Ethan’s condition had progressed to the point where the malformation was putting pressure on the facial nerve branches that control the face. I knew going in that this would be a challenging case, especially with the risk of bleeding, so we made sure to take our time separating the normal tissue from the vascular malformation.”
The surgical procedure was unique in its use of intraoperative facial-nerve monitoring, a state-of-the-art technique that provides real-time assessment of the facial-nerve function throughout the operation, even alerting the surgeon to any stretch or compression from tissues nearby.
“In the past, we would advise patients that the surgical risk to the facial nerve was up to 50 percent, leading some patients not even to consider surgery,” Dr. Levitin adds. “Using this technique, I can confidently remove these types of lesions with less than one percent risk of injury to the nerve. This was the case for Ethan: after five hours, we got it just right.”
“When I awoke after surgery I was in so much pain but saw a beautiful sight: my family, the nurses, and Dr. Levitin,” Ethan recalls. “After the surgery I felt a resurgence of confidence inside me. And when I resumed classes for the spring semester, my friends noticed that my lump was gone and my face was symmetrical again. Today, looking into the mirror, I feel completely normal, as if I never had the surgery.”
Transoral Robotic Surgery Tackles Tonsil Cancer Without Radiation
Tameka Ferdinand first experienced a burning sensation in her throat after eating tart candy. When it persisted, the Queens, New York, resident headed straight to her primary care physician, who referred her to a Mount Sinai–affiliated ear, nose, and throat physician, William Portnoy, MD.
Shortly after Thanksgiving of 2016, Dr. Portnoy gave Ms. Ferdinand, who is in her 50s, the bad news from her biopsy: she had HPV-related tonsil cancer. “I literally sat on my bed and started planning my funeral,” Ms. Ferdinand recalls. “And I wondered how I was going to tell everyone.”

Dr. Portnoy referred her to Raymond Chai, MD, a head and neck surgeon at Mount Sinai-Union Square, who scheduled her for a PET-CT scan and conducted an exploratory procedure to determine whether she was a candidate for transoral robotic surgery (TORS).
“I relayed to Ms. Ferdinand that she had a large mass arising from the tonsil and involving the inferior portion of her soft palate,” Dr. Chai says. “But the good news was that she was an excellent candidate for TORS and we felt that with the procedure, there was a high likelihood that we could deintensify therapy for her.”
Surgery, including a neck dissection, took place at Mount Sinai Beth Israel on a Friday in January 2017, and Ms. Ferdinand returned home on Sunday. Without TORS, she would have required high-dose chemoradiation or spent up to two weeks in the hospital following open surgery. She was swallowing liquids the day after surgery and resumed a normal dietroughly two weeks afterward.
The best news of all followed. “I was told the surgery was so successful, I would not require chemotherapy or radiation as a follow-up treatment,” she declared, smiling broadly. “I thank God for all three of my doctors: my PCP, Dr. Portnoy, and Dr. Chai—they are godsends,” Ms. Ferdinand says.
“This was a journey of enlightenment and I don’t take any more days for granted. I live each day to the fullest now. Thank you to my physicians and the entire staff at Mount Sinai-Union Square and Mount Sinai Beth Israel. I am grateful to be alive to tell my story!”
Personalized Genomic Vaccines Fight Cancer
When tumor cells appear in a cancer patient, the immune system is mobilized to attack and kill them through the action of white cells called killer T cells. Despite the initial immune response, tumors become highly adept at escaping the immune system. Fortunately, new immune-based therapeutics, in particular checkpoint inhibitors, demonstrate clinical efficacy in several solid malignancies, including head and neck cancer, by reinvigorating and expanding killer T cells that recognize neoantigens in tumor cells and target these cells. These agents are available as part of The Tisch Cancer Institute’s Solid Tumor Program at the Icahn School of Medicine at Mount Sinai.

Unfortunately, not all patients respond to checkpoint inhibitors, and therefore Mount Sinai researchers are exploring novel strategies to combat this problem. Physicians with the Personalized Medicine Program at The Tisch Cancer Institute have initiated a phase I proof-of-concept study, a fully personalized multipeptide therapeutic vaccine designed to target tumor-derived neoantigens for individual patients. The investigational vaccine is based on the Personalized Genomic Vaccine (PGV) platform, which utilizes tumor sequencing technologies to identify tumor-specific neoantigens for specific patients.
The goal of this therapy is to induce a robust antitumor immune response and minimize the risk of nonspecific immune activity. If effective, it would represent a significant contribution to the fields of tumor immunology and medical oncology.
The first patient enrolled in this trial had head and neck cancer and has almost completed his vaccine cycle. There is early evidence that the vaccine has generated immunity in this patient. Should this trial prove to be safe and elicit immunity in additional patients, it will demonstrate the utility of the PGV therapeutic vaccine design platform and pave the way for further cancer type–specific trials to demonstrate therapeutic efficacy.
Message from the Chair: Eric Genden, MD, FACS
The year 2017 was one of innovation at the Department of Otolaryngology – Head and Neck Surgery. Clinical innovations in the areas of otologic and skull base surgery, as well as personalized vaccine therapy, have had a positive impact on the care of our patients. George Wanna, MD, Site Chair of Otolaryngology for Mount Sinai Downtown and Director of the Ear Institute and Center for Hearing and Balance, is using high-resolution endoscopy to manage disease and tumors of the middle ear and lateral skull base. Dr. Wanna and Maura Cosetti, MD, have demonstrated the unique advantages that this technique provides for the management of middle ear cholesteatoma and vascular tumors of the skull base.
 Innovation and technology have also had a positive impact on education. Led by Alfred M.C. Iloreta, Jr., MD, virtual reality is now being used for learning complex skull base anatomy. No longer are students and resident trainees dependent on two-dimensional learning tools. Virtual reality headsets provide students with the ability to navigate the anatomy in a way that has not been previously possible. This program appears to increase students’ aptitude and learning motivation and can be used as a platform for planning surgery.
Innovation and technology have also had a positive impact on education. Led by Alfred M.C. Iloreta, Jr., MD, virtual reality is now being used for learning complex skull base anatomy. No longer are students and resident trainees dependent on two-dimensional learning tools. Virtual reality headsets provide students with the ability to navigate the anatomy in a way that has not been previously possible. This program appears to increase students’ aptitude and learning motivation and can be used as a platform for planning surgery.
Finally, the Department launched a personalized multipeptide therapeutic vaccine designed to target tumor-specific neoantigens with the goal of inducing a robust antitumor immune response and minimizing the risk of nonspecific immune activity.
As the Icahn School of Medicine at Mount Sinai enters its 50th anniversary year, we remain steadfast in our commitment to our patients, our trainees, and our faculty, with the goal of developing and refining the innovative treatments of the future. I invite you to peruse the detailed information in this year’s Specialty Report and thank you for taking the time to do so.
Dr. Isidore Friesner Professor and Chair
Department of Otolaryngology – Head and Neck Surgery
Senior Associate Dean for Clinical Affairs
Icahn School of Medicine at Mount Sinai