Mount Sinai's The Louis Armstrong Center for Music and Medicine Celebrates 30th Anniversary With a Commemorative Conference
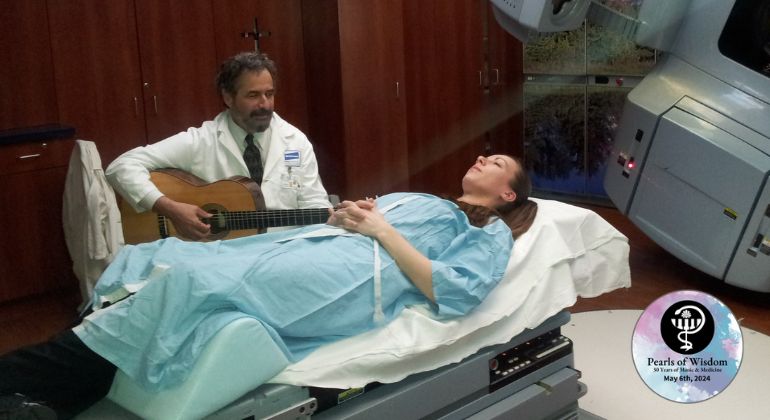
The Louis Armstrong Center for Music and Medicine at Mount Sinai is celebrating its 30th anniversary.
Launched with support from the Louis Armstrong Educational Foundation, the Center created a new model of integrating music and medicine in patient care and has served patients and families in various settings throughout the Mount Sinai Health System and overseas. The Center provides continuity of care for patients in the inpatient and outpatient settings, and has launched a research lab through AMEND (Assessment of Music Experiences in Navigating Depression) which is supported by the National Endowment for the Arts in partnership with Carnegie Hall's Weil Music Institute.
The Center held a commemorative conference—Pearls of Wisdom: 30 Years of Music and Medicine—to mark 30 years of practice and impact that discussed influential trends in disease management such as the inclusion of healing breath, oncology, AI, and diversity. Conference Chair Kristen Stewart, MA, LCAT, MT-BC, the Center’s Assistant Director, joined other experts, including a keynote by Brian Harris, director of Med Rhythms, and a research overview by Sheri Robb, PhD, a National Institutes of Health (NIH) supported researcher at Indiana University who has been studying music therapy in children with cancer for many years. Conference sponsors include the Renee Fleming Foundation, Marshalls Speakers, the MJS Foundation, and the International Association for Music and Medicine.
Joanne Loewy, DA, is a Professor of Family Medicine and Community Health at the Icahn School of Medicine at Mount Sinai and Director of the Center. The clinic's Medical Director, Stephan Quentzel, MD, oversees psychiatric care and provides supervisory support to the Armstrong team of music therapists, including Andrew Rossetti, PhD, LCAT, MT-BC; Christopher Pizzute, MA, LCAT, MT-BC; Samantha Sancho, MA, MT-BC, LCAT-LP; administrative coordinator Shantelena Mouzon; and research coordinator Andee Dooley, MS, BC-DMT, LCAT.
"We are one of the only Centers in New York City that provides integrative care for patients and musicians of all professions and calibers," says Dr. Quentzel, who partners with the Mount Sinai Behavioral Health Center to refer patients in need of psychiatry care, services, and evaluation.
“The clinic serves patients of all ages and diagnoses, while providing graduate students with the opportunity to provide direct patient care with guidance from experienced, licensed music therapists who guide them in caring for vulnerable populations such as musicians, neuro-divergent children, teens with depression, and aging adults with multiple social stressors and mental health needs,” says Dr. Loewy.
“Students quickly learn how to leverage hospital and community resources implementing music with medicine in a care-model that emphasizes a multidisciplinary approach” says Ms. Stewart.
The clinic provides a rich training ground for graduate students who complete 1,080 hours of clinical training as part of their second year graduate studies. The music therapists also extend music therapy services to children in the New York City public schools through the Asthma Initiative Program.
Since its inception in 1994, the Center’s music therapists have co-authored numerous papers in leading academic journals along with doctors and nurses who play a significant role in the care continuum. The research encompasses topics relevant to the health care needs of the most vulnerable patient populations, such as newborn babies and patients in medical intensive care units. The research has focused on strategies for mitigating the chronic burden of stress among their patients. This year, thanks to NIH funding, the Center will study the impact of music therapy in metabolomic pathways that indicate chronic stress in Black pregnant women during their first trimester. Additional focus is given to practice development such as population-based care in neonates and pediatrics, older adults and clinic-based mental health population.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.