AI Can Help Doctors Make Better Decisions and Save Lives
Study suggests real-time alerts for declining health speed up treatment and reduce hospital deaths
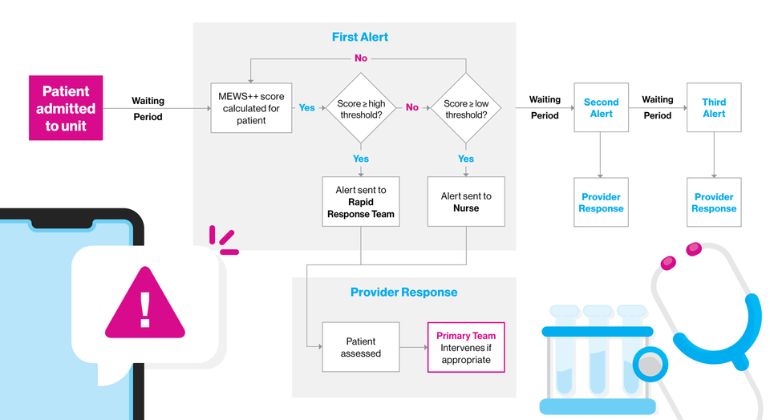
Flow chart showing the study notification protocol. The logic and provider response for the second and third alerts are identical to the first alert.
Credit: Mount Sinai Health System
Deploying and evaluating a machine learning intervention to improve clinical care and patient outcomes is a key step in moving clinical deterioration models from byte to bedside, according to a June 13 editorial in Critical Care Medicine that comments on a Mount Sinai study published in the same issue. The main study found that hospitalized patients were 43 percent more likely to have their care escalated and significantly less likely to die if their care team received AI-generated alerts signaling adverse changes in their health.
“We wanted to see if quick alerts made by AI and machine learning, trained on many different types of patient data, could help reduce both how often patients need intensive care and their chances of dying in the hospital,” says lead study author Matthew A. Levin, MD, Professor of Anesthesiology, Perioperative and Pain Medicine, and Genetics and Genomic Sciences, at Icahn Mount Sinai, and Director of Clinical Data Science at The Mount Sinai Hospital. “Traditionally, we have relied on older manual methods such as the Modified Early Warning Score (MEWS) to predict clinical deterioration. However, our study shows automated machine learning algorithm scores that trigger evaluation by the provider can outperform these earlier methods in accurately predicting this decline. Importantly, it allows for earlier intervention, which could save more lives.”
The non-randomized, prospective study looked at 2,740 adult patients who were admitted to four medical-surgical units at The Mount Sinai Hospital in New York. The patients were split into two groups: one that received real-time alerts based on the predicted likelihood of deterioration, sent directly to their nurses and physicians or a “rapid response team” of intensive care physicians, and another group where alerts were created but not sent. In the units where the alerts were suppressed, patients who met standard deterioration criteria received urgent interventions from the rapid response team.
Additional findings in the intervention group demonstrated that patients:
- were more likely to get medications to support the heart and circulation, indicating that doctors were taking early action; and
- were less likely to die within 30 days
"Our research shows that real-time alerts using machine learning can substantially improve patient outcomes," says senior study author David L. Reich, MD, President of The Mount Sinai Hospital and Mount Sinai Queens, the Horace W. Goldsmith Professor of Anesthesiology, and Professor of Artificial Intelligence and Human Health at Icahn Mount Sinai. "These models are accurate and timely aids to clinical decision-making that help us bring the right team to the right patient at the right time. We think of these as ‘augmented intelligence’ tools that speed in-person clinical evaluations by our physicians and nurses and prompt the treatments that keep our patients safer. These are key steps toward the goal of becoming a learning health system."
The study was terminated early due to the COVID-19 pandemic. The algorithm has been deployed on all stepdown units within The Mount Sinai Hospital, using a simplified workflow. A stepdown unit is a specialized area in the hospital where patients who are stable but still require close monitoring and care are placed. It's a step between the intensive care unit (ICU) and a general hospital area, ensuring that patients receive the right level of attention as they recover.
A team of intensive care physicians visits the 15 patients with the highest prediction scores every day and makes treatment recommendations to the doctors and nurses caring for the patient. As the algorithm is continually retrained on larger numbers of patients over time, the assessments by the intensive care physicians serve as the gold standard of correctness, and the algorithm becomes more accurate through reinforcement learning.
In addition to this clinical deterioration algorithm, the researchers have developed and deployed 15 additional AI-based clinical decision support tools throughout the Mount Sinai Health System.
The Mount Sinai paper is titled “Real-Time Machine Learning Alerts to Prevent Escalation of Care: A Nonrandomized Clustered Pragmatic Clinical Trial.” The remaining authors of the paper, all with Icahn Mount Sinai except where indicated, are Arash Kia, MD, MSc; Prem Timsina, PhD; Fu-yuan Cheng, MS; Kim-Anh-Nhi Nguyen, MS; Roopa Kohli-Seth, MD; Hung-Mo Lin, ScD (Yale University); Yuxia Ouyang, PhD; and Robert Freeman, RN, MSN, NE-BC.
About the Icahn School of Medicine at Mount Sinai
The Icahn School of Medicine at Mount Sinai is internationally renowned for its outstanding research, educational, and clinical care programs. It is the sole academic partner for the eight- member hospitals* of the Mount Sinai Health System, one of the largest academic health systems in the United States, providing care to a large and diverse patient population.
Ranked 13th nationwide in National Institutes of Health (NIH) funding and among the 99th percentile in research dollars per investigator according to the Association of American Medical Colleges, Icahn Mount Sinai has a talented, productive, and successful faculty. More than 3,000 full-time scientists, educators, and clinicians work within and across 44 academic departments and 36 multidisciplinary institutes, a structure that facilitates tremendous collaboration and synergy. Our emphasis on translational research and therapeutics is evident in such diverse areas as genomics/big data, virology, neuroscience, cardiology, geriatrics, as well as gastrointestinal and liver diseases.
Icahn Mount Sinai offers highly competitive MD, PhD, and Master’s degree programs, with current enrollment of approximately 1,300 students. It has the largest graduate medical education program in the country, with more than 2,000 clinical residents and fellows training throughout the Health System. In addition, more than 550 postdoctoral research fellows are in training within the Health System.
A culture of innovation and discovery permeates every Icahn Mount Sinai program. Mount Sinai’s technology transfer office, one of the largest in the country, partners with faculty and trainees to pursue optimal commercialization of intellectual property to ensure that Mount Sinai discoveries and innovations translate into healthcare products and services that benefit the public.
Icahn Mount Sinai’s commitment to breakthrough science and clinical care is enhanced by academic affiliations that supplement and complement the School’s programs.
Through the Mount Sinai Innovation Partners (MSIP), the Health System facilitates the real-world application and commercialization of medical breakthroughs made at Mount Sinai. Additionally, MSIP develops research partnerships with industry leaders such as Merck & Co., AstraZeneca, Novo Nordisk, and others.
The Icahn School of Medicine at Mount Sinai is located in New York City on the border between the Upper East Side and East Harlem, and classroom teaching takes place on a campus facing Central Park. Icahn Mount Sinai’s location offers many opportunities to interact with and care for diverse communities. Learning extends well beyond the borders of our physical campus, to the eight hospitals of the Mount Sinai Health System, our academic affiliates, and globally.
-------------------------------------------------------
* Mount Sinai Health System member hospitals: The Mount Sinai Hospital; Mount Sinai Beth Israel; Mount Sinai Brooklyn; Mount Sinai Morningside; Mount Sinai Queens; Mount Sinai South Nassau; Mount Sinai West; and New York Eye and Ear Infirmary of Mount Sinai.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.