Scientists See Signs of Traumatic Brain Injury in Headbutting Muskox
Preliminary results from Mount Sinai study may contradict consensus on whether ramming animals experience brain damage and provide insights into human injuries
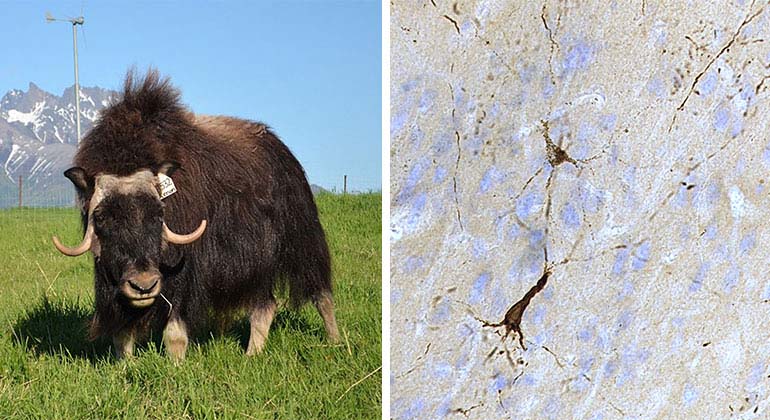
Do Headbutting Muskox Experience TBI? Scientists Icahn Mount Sinai saw signs of traumatic brain injury in headbutting muskox. Credit: Musk Ox Farm, Palmer, AK TBI Hallmarks in Muskox Brains Scientists at Icahn Mount Sinai discovered hallmarks of TBI in muskox brains which had been treated with antibodies against phosphorylated tau protein. Credit: Hof lab, Icahn Mount Sinai, N.Y., N.Y.
Scientists at the Icahn School of Medicine at Mount Sinai saw for the first time hallmarks of concussions and other head trauma in the brains of deceased headbutting animals—muskoxen and bighorn sheep. The results published in the journal Acta Neuropathologica may contradict the commonly-held belief that ramming animals do not suffer brain injuries and support the notion that studies on animals with brains evolutionarily similar to those of humans may help researchers understand and reduce traumatic brain injuries.
“Death and disability caused by traumatic brain injury is a widespread problem that needs better solutions,” said Nicole Ackermans, PhD, postdoctoral fellow at Icahn Mount Sinai and the study leader. “We showed that animals which regularly engage in headbutting may actually suffer the kind of traumatic brain injury seen in humans. This opens the possibility that by studying these animals we could learn a lot about traumatic brain injury.”
Dr. Ackermans and her colleagues studied the brains of three deceased muskoxen from Greenland and four bighorn sheep, which were obtained from parks in Colorado and Utah and the Buffalo Zoo in New York.
Part of the reason for obtaining brains from these horned animals is that they are known to engage in violent head-to-head collisions, usually in mating and social hierarchy rituals. For instance, male muskoxen often reach speeds of up to 30 miles an hour before impact. Although a few studies have observed symptoms of traumatic brain injury (TBI), such as acting dazed, none have directly tested whether the brains of muskoxen and other ramming animals show any damage.
The other reason is that bovids—such as cows, sheep, buffalo, gazelles, and the animals in the study—have gyrencephalic, or folded, brains, which are also seen in humans.
“Our lab tries to use evolution to help solve medical mysteries,” said Patrick R. Hof, MD, Professor of Neuroscience at Icahn Mount Sinai and senior author of the study. “One of the difficulties of TBI research is that most of it is performed on smooth, rodent brains. We thought that studying the brains of ramming bovids might provide a better model for understanding TBI in humans.”
When they first arrived, the animals’ brains looked healthy, and brain scans showed that the overall structure of each animal’s brain was intact.
To look for signs of TBI damage, the researchers then cut the brains into thin slices and treated the slices with antibodies made to detect phosphorylated tau proteins found in humans or mice. This form of tau is a hallmark of damage that is often seen in the brains of Alzheimer’s disease patients, or in people who have suffered TBIs, including chronic traumatic encephalopathy (CTE).
When they looked at the brains under a microscope, they saw that one of the antibodies stained muskoxen brains at easily detectable levels, whereas the bighorn sheep brains had lightly detectable levels of staining by a different antibody.
“At first we were surprised. One of the challenges with these kinds of studies is that we don’t know whether antibodies used on human and rodents will work on bovid brains,” Dr. Ackermans said. “The fact that we detected these antibodies was important. It suggested that the brains of these animals, especially the muskoxen, sustain TBI-like damage."
Further analysis supported the idea. For example, the prefrontal cortex of the muskoxen brains had high levels of tau protein tangles, especially near the surface of the cortex.
“This pattern is sometimes seen in the brains of people who suffer from CTE,” Dr. Ackermans said. “Our results open the possibility that these animal’s brains undergo chronic, repetitive damage, as seen in some TBI patients.”
In contrast, when the researchers looked at brain slices from an Alzheimer’s disease patient, they saw a more even and widespread staining pattern.
Curiously, an old female muskox had much more—about 20 times more—staining than the older male and five times more staining than another female. This is the opposite of what the researchers hypothesized, as males are known to ram each other harder and more often than females.
“This study left us with many interesting questions, like: Why did the female muskox brains appear to have more damage than the male ones? Is this because of differences in skull anatomy? Why did the brains of bighorn sheep have so little damage? And is it possible to harness the knowledge we gain from these animals to develop better treatments for TBI?” said Dr. Ackermans.
This work was supported by the Swiss National Science Foundation (P2ZHP3_191255) and the Office of Naval Research (N00014-20-452 1-2762; N00014-17-1-2737).
Article
Ackermans, N.L.; Evidence of traumatic brain injury in headbutting bovids, Acta Neuropathologica, May 17, 2022, DOI: 10.1007/s00401-022-02427-2
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.