Mount Sinai Selected to Serve as Capacity Building Center and Center of Excellence as Part of the National Cancer Institute’s New Serological Sciences Network
More than $7.3 million in funding will help with serological testing efforts and research into immunology of COVID-19
Researchers from the Icahn School of Medicine at Mount Sinai will receive more than $7.3 million from the National Cancer Institute (NCI) as part of the NCI’s new Serological Sciences Network (SeroNet), one of the largest coordinated national efforts to study immunology and SARS-CoV-2, the virus that causes COVID-19. Mount Sinai was selected as one of only four Capacity Building Centers and one of eight Centers of Excellence as part of this new network.
SeroNet is a major component of NCI’s response to the pandemic and is included in an emergency Congressional appropriation of $306 million to the Institute to develop, validate, improve, and implement serological testing and associated technologies. Through the involvement of more than 25 universities, cancer centers, and laboratories working in partnership with NCI, the National Institute of Allergies and Infectious Diseases and the Frederick National Laboratory, members of SeroNet will work to rapidly deploy serological testing to the American public and to improve our understanding of the immune response to SARS-CoV-2 and mitigate the pathogen’s spread.
“Mount Sinai is at the forefront of cutting-edge research and treatment on COVID-19. Our innovation, creativity, and exceptional staff have found ways to adapt and continue to excel in our drive to translate scientific discovery into practice that will improve public health,” says Dennis S. Charney, MD, Anne and Joel Ehrenkranz Dean of the Icahn School of Medicine at Mount Sinai, and President for Academic Affairs of the Mount Sinai Health System. “We are thrilled to join the National Cancer Institute in this collective endeavor to fight this virus that has affected so many around the world.”
As one of the four SeroNet Capacity Building Centers, Mount Sinai will receive more than $3.46 million from the National Cancer Institute so a multidisciplinary team of Mount Sinai researchers and clinicians can assist with SeroNet’s effort to rapidly deploy and expand SARS-CoV-2 serological testing capacity and practice in the community.
Mount Sinai’s serology testing platforms and operations are uniquely poised to provide a solid translational engine capable of the capacity building SeroNet is committed to accomplishing, said Carlos Cordon-Cardo, MD, PhD, Irene Heinz Given and John LaPorte Given Professor and Chair of Pathology, Molecular and Cell-Based Medicine at the Icahn School of Medicine at Mount Sinai.
“We have a proven track record of accomplishment in implementing, validating, reliably performing, and maintaining high-throughput SARS-CoV-2 serology testing, having developed a highly sensitive and specific antibody test that was one of the very first to receive emergency use authorization by the U.S. Food and Drug Administration and the New York State Department of Health during the early stages of the pandemic,” said Dr. Cordon-Cardo, who will lead Mount Sinai’s capacity-building efforts for SeroNet. “We are extremely grateful to the National Cancer Institute for recognizing our excellence in this arena and for selecting Mount Sinai to assist them in this effort.”
Mount Sinai researchers also received $3.9 million to lead a SeroNet Center of Excellence to study lung cancer patients’ vulnerability to developing severe COVID-19 symptoms and their increased chances of dying from the disease. This is one of eight centers of excellence funded by the NCI as part of the SeroNet initiative. The center of excellence that Mount Sinai is leading will analyze blood samples to determine lung cancer patients’ antibody response when they contract COVID-19 and when they receive a COVD-19 vaccine. Researchers will also study possible changes in lung tumor cells and noncancerous lung cells in lung cancer patients who have COVID-19. The project will study 1,000 patients with lung cancer and 1,000 patients without lung cancer to determine if there are differences in antibody responses related to age, gender, tobacco history, and race or ethnicity.
“Our overall hypothesis is that lung cancer patients have a weaker antibody response to COVID-19 and that their lung tissue and tumor cells may play a role in their body’s response to infection, which could explain the aggressive course and high fatality rate that we’ve seen,” said Fred R. Hirsch, MD, PhD, Executive Director of the Center for Thoracic Oncology at The Tisch Cancer Institute at Mount Sinai and co-primary investigator of the lung cancer project. “Our U54 Serologic Center will determine whether COVID-19 infection or vaccines will give similar antibody responses in patients with lung cancer compared to patients without lung cancer.”
Dr. Hirsch and Adolfo García-Sastre, PhD, Director of the Global Health and Emerging Pathogens Institute at Mount Sinai, are primary investigators of the lung cancer project and will oversee the center, which also includes researchers from the University of Texas Southwestern, University of Colorado, University of Maryland, and Vanderbilt University.
“The nation’s top researchers in academia, government, and private industry have come together in an unprecedented effort to fight the pandemic,” said Dinah Singer, PhD, deputy director of the National Cancer Institute. “Though SeroNet, we are examining the immune response to the coronavirus to speed delivery of testing, treatments, and vaccine development for COVID-19. What we learn could be applied immediately and will provide invaluable to public health beyond the current pandemic.”
In April 2020, the Mount Sinai antibody test was one of the first to receive emergency use authorization for qualitative use (detection of the presence or absence of antibodies) from both the U.S. Food and Drug Administration and the New York State Department of Health. The Mount Sinai antibody test detects the presence or absence of SARS-CoV-2 antibodies in addition to measuring the titer (level) of antibodies a person has produced. It utilizes not one, but two virus antigens: the full-length spike protein and its receptor-binding domain (RBD), which is correlated with antibody neutralization, as described in a recent paper published in Nature Medicine. The test was used recently in a study by researchers at the Icahn School of Medicine at Mount Sinai that found most people with COVID-19 mount a robust antibody response that is stable for at least three months.
Created by a team of internationally renowned scientists and clinicians at the Icahn School of Medicine at Mount Sinai, the Mount Sinai antibody test is a serological enzyme-linked immunosorbent assay (ELISA) that utilizes both the spike protein and the RBD, which are necessary for viral entry into cells. The toolkit needed to set up the Mount Sinai antibody test has since been shared with hundreds of research laboratories worldwide and has been used by Mount Sinai on more than 68,000 people to determine whether they were exposed to SARS-CoV-2, and to understand their antibody titers both in the initial response to SARS-CoV-2 and over time.
Through SeroNet, Mount Sinai faculty involved in serological testing and immunology research will interact closely, collaborate, and share data, resources, and samples with colleagues at NCI, across the United States and abroad.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.
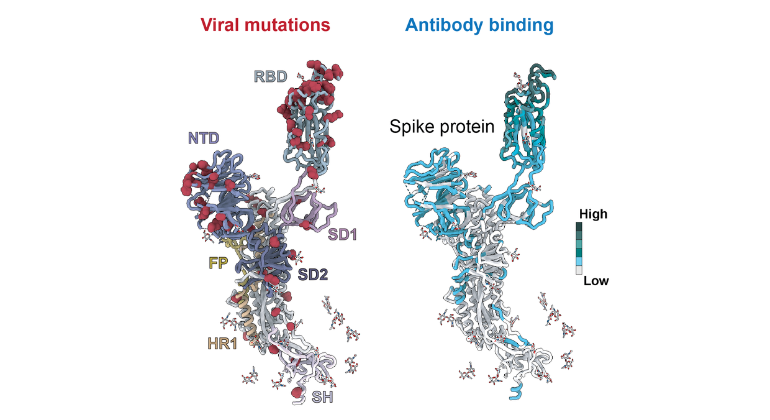
Scientists Uncover How COVID-19 Variants Outsmart the Immune System
Nov 21, 2025 View All Press ReleasesMost People Mount a Strong Antibody Response to SARS-CoV-2 That Does Not Decline Rapidly
Oct 28, 2020 View All Press Releases