Mount Sinai Researchers Find Gene Therapy Improved Left Ventricular and Atrial Function in Congestive Heart Failure by up to 25 percent
Intracoronary Delivery of Gene Vector Was Safe and Improved Heart Function in a Large Animal Model
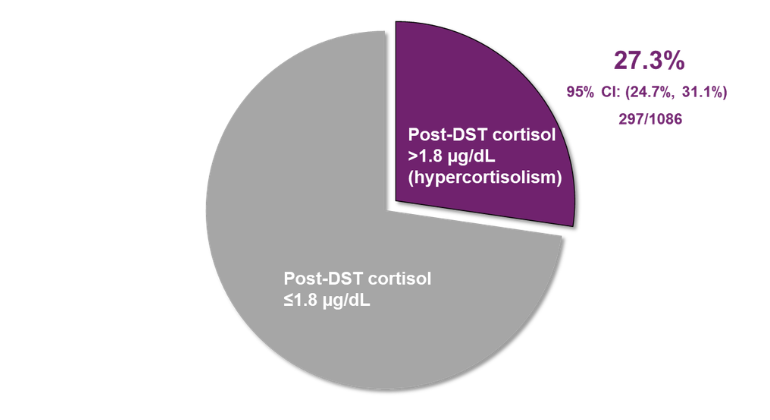
Heart function improved by up to 25 percent in a trial using gene therapy to reverse cardiac damage from congestive heart failure in a large animal model, Mount Sinai researchers report. This is the first study using a novel vector for gene therapy to improve heart function in non-ischemic heart failure.
The results of the study will be published online in the Journal of the American College of Cardiology on Monday, September 25, at 2 pm.
In heart failure, a weakened or damaged heart no longer pumps blood effectively. This potentially fatal disease affects almost 6 million Americans, according to the American Heart Association, and is a major cause of morbidity and mortality, especially in elderly patients. Despite this toll, there has been little progress toward any kind of cure. Novel therapeutic approaches, such as gene therapy and cell therapy, hold the promise of complementing or replacing existing therapies for congestive heart failure.
“Mount Sinai has performed pioneering work on gene therapy over the last decade, and this study shows that gene therapy is now a viable option for treating congestive heart failure,” said the study’s senior author, Roger Hajjar, MD, Director of the Cardiovascular Research Center and the Arthur and Janet C. Ross Professor of Medicine at the Icahn School of Medicine at Mount Sinai. “There is a critical need to explore new therapeutic avenues and approaches.”
This study featured two independent experiments. The first established the safety of administering a therapeutic gene delivery vector, BNP116, created from an inactivated virus over three months, into 48 pigs without heart failure through the coronary arteries via catheterization using echocardiography. The second experiment examined the efficacy of the treatment in 13 pigs with severe heart failure induced by mitral regurgitation. Six pigs received the gene and 7 received a saline solution.
The researchers determined that the gene therapy was safe and significantly reversed heart failure by 25 percent in the left ventricle and by 20 percent in the left atrium. Heart failure often results in enlarged hearts, and the team found a 10 percent reduction of heart size in the affected animals. Heart failure in the cohort of pigs treated with saline worsened.
The research team plans to study the same gene therapy in a human trial starting next year. The gene vector has been approved by the Food and Drug Administration for clinical treatment.
This study was supported by NIH P50 HL112324, R01 HL119046, R01 HL117505, R01HL128099, R01 HL129814, R01HL131404, & R43HL108581 (R. J. H.), HL26057, & HL64018 (E.G. K) and a Transatlantic Leducq Foundation grant. The Gene Therapy Resource Program (GTRP) of the National Heart, Lung, and Blood Institute, National Institutes of Health provided some of the gene vectors used in this study. K.I is supported by a grant from American Heart Association 17SDG33410873.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.

Mount Sinai’s Roxana Mehran, MD, Named President of the American College of Cardiology
Mar 30, 2026 View All Press Releases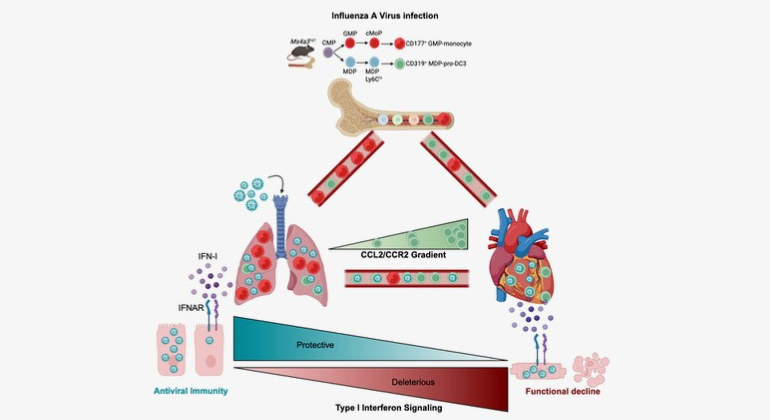
Mount Sinai Scientists Uncover Link Between Influenza and Heart Disease
Feb 09, 2026 View All Press Releases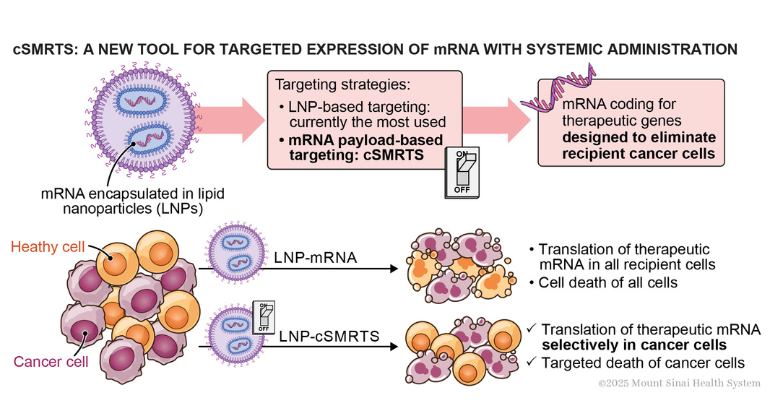
Scientists Develop a Smarter mRNA Therapy That Knows Which Cells to Target
Dec 15, 2025 View All Press Releases