
Rehabilitation Center
The Mount Sinai Health System has enabled us to provide the best imaginable rehabilitation medicine services to thousands of individuals with disability and painful conditions caused by either injury or disease.
Rehabilitation Center
The Mount Sinai Health System’s Rehabilitation Center strives to provide comprehensive rehabilitation services for people with disability and to educate others about their diverse needs while conducting groundbreaking research to enhance patient health, mobility, self-care skills, quality of life, and integration into the community.
This specialty report highlights:
- A 37-year-old patient with paraplegia who returned to his job, stays fit at the gym, and recently completed his sixth marathon.
- The Mount Sinai Injury Control Research Center’s five-year study, funded by the U.S. Centers for Disease Control and Prevention, of the relationship between traumatic brain injury and criminal behavior
- A pilot study exploring the safety and feasibility of using a powered exoskeleton for persons with multiple sclerosis (MS)
- A report on the Sports Medicine program in the Mount Sinai Health System, a robust interdisciplinary program that has become a leader in research and fellowship training
- The story of a mergers and acquisitions attorney who became a paralysis advocate, co-founding New Yorkers to Cure Paralysis, following a spinal cord injury
Coordinated Care and Innovative Programs Help Patient Regain Skills
Yannick Benjamin is a 37-year-old sommelier at The University Club in Midtown Manhattan. He co-founded and is the development director of a nonprofit organization, travels internationally, stays fit by exercising at the gym five days a week, and recently completed his sixth marathon. Mr. Benjamin is also paraplegic, and he credits many of his achievements to The Mount Sinai Hospital’s Department of Rehabilitation Medicine.
 In October 2003, Mr. Benjamin was involved in a traumatic car accident on a New York City highway. He fractured his T6 vertebra, which left him with paralysis below the waist. Following spinal surgery, he began two months of inpatient rehabilitation at Mount Sinai, where he learned how to use a wheelchair and to adapt to his new situation, including performing such daily activities as transferring properly in and out of his wheelchair, showering, using the bathroom, and getting up after falls.
In October 2003, Mr. Benjamin was involved in a traumatic car accident on a New York City highway. He fractured his T6 vertebra, which left him with paralysis below the waist. Following spinal surgery, he began two months of inpatient rehabilitation at Mount Sinai, where he learned how to use a wheelchair and to adapt to his new situation, including performing such daily activities as transferring properly in and out of his wheelchair, showering, using the bathroom, and getting up after falls.
At Mount Sinai, a team effort—together with innovative programs—provides patients like Mr. Benjamin with the skills and encouragement to resume an active life. Physicians, therapists, nurses, social workers, and psychologists offer coordinated care so that patients can reach their maximum recovery potential. And unlike facilities where patients of all ages and with various types of surgeries and injuries rehabilitate together, Mount Sinai has a separate section, with 25 beds and dedicated staff, for patients with spinal cord injuries (SCI).
In July 2015, the Mount Sinai Rehabilitation Center was accredited by the Commission on Accreditation of Rehabilitation Facilities for achieving a pattern of practice excellence for its Spinal Cord System of Care (see box, page 5). Mr. Benjamin commends the physical therapists for the passion they bring to their work and the nurses for providing “phenomenal” care as well as patience, compassion, positive attitudes, diligence, and the capacity to understand his challenges.
It was at Mount Sinai that Mr. Benjamin met Alex Elegudin, a college sophomore at the time, who was also rehabilitating from a C6-level SCI. Their bond led them to co-found Wheeling Forward, a nonprofit organization that provides advocacy, mentorship, and support services to enable people with disabilities to experience life to the fullest. Mr. Elegudin, now a successful patent attorney, is president of the organization.
Once patients are discharged from Mount Sinai, they stay connected through a large range of fitness and education programs designed to address SCI patients’ physical, emotional, and social needs. The Spinal Cord Injury Peer Mentoring Program establishes partnerships between those with recent SCI and former patients who have successfully coped with these injuries over the long term. Since the program began, more than 100 people have been trained as mentors and matched with 130 partners.
The Do-It! Program helps people with SCI to reconnect with the community by offering classes to promote health, wellness, and self-advocacy. The Peak Performance class uses chair yoga, seated tai chi and qigong, breathing exercises, meditation, and guided imagery to teach participants how to improve their health.
Since its inception in 2003, Mount Sinai’s Spinal Cord Injury Life Challenge Program has organized trips enabling nearly 300 individuals with SCI to skydive, surf, kayak, hang glide, and ski. “It’s a very empowering program,” says Avniel Shetreat-Klein, MD, PhD, Assistant Professor of Rehabilitation Medicine.
Today, Mr. Benjamin lives independently in New York City and dedicates much of his time to Wheeling Forward, where, in addition to fundraising, he teaches a modified spin class to individuals with paraplegia. Through his determination and creativity, Mr. Benjamin has additionally fulfilled his professional aspiration of becoming a sommelier: he created a special tray that lets him carry wine glasses while seated in his wheelchair.
“I tell people who sustain a spinal cord injury never to give up and never to lose faith in themselves,” Mr. Benjamin says. “Don’t lose the passion for life that you had before your accident. Whatever you were doing before, by thinking outside the box and being creative, you can make it happen again.”
Advancing the Study of Traumatic Brain Injury and Criminal Behavior
Although it has long been recognized that a relationship exists between traumatic brain injury (TBI) and criminal behavior, this relationship has not been studied in a large sample of youth offenders. The Mount Sinai Injury Control Research Center (MS-ICRC) is examining this issue in great detail in a five-year study funded by the U.S. Centers for Disease Control and Prevention.
By using the Brain Injury Screening Questionnaire that was developed at Mount Sinai, investigators are screening more than 4,300 youth in jail or on parole in Texas to determine the relationship between TBI and violent or antisocial behavior.
Preliminary data analysis reveals, unsurprisingly—as this is the case in adult prison populations—that 27 percent of these young people have a history of one or more TBIs. The more significant finding, to date, is that the majority sustained their TBIs prior to the onset of their criminal behavior. Those who sustained their injury prior to their first criminal encounters also had more DSM diagnoses and reported more symptoms, meaning that they were more emotionally, physically, and cognitively distressed. In addition, this group of adolescents was more likely to commit violent crimes—and crimes of a sexual nature—than those without a TBI or whose TBI came after the onset of their criminal behavior.
To potentially help these adolescents take a better path in life, the MS-ICRC developed, in cooperation with the staff of the El Paso Juvenile Justice Center, an intervention to teach them to better understand their emotions, solve problems more effectively, and think of the consequences of their actions before they act. This program is currently being pilot tested at the El Paso center, where 300 youth have gone through the 12-week program. Although the study is still ongoing, data reveal that six months following program completion, recidivism had dropped by more than 50 percent among the participants.
Wayne Gordon, PhD, Director of the Brain Injury Research Center of Mount Sinai and the Jack Nash Professor and Vice Chair of Research and Mentoring, Department of Rehabilitation Medicine, is the principal investigator of the study, which also involves a team of collaborators at the El Paso Juvenile Justice Center.
The Brain Injury Research Center of Mount Sinai has an annual budget of more than $3 million in federal grants. Its research portfolio encompasses a range of important areas, including aging with TBI and interventions to improve fatigue and emotional regulation in individuals with TBI. To learn more about the Center and its research, visit www.tbicentral.org.
A Law Career and Travel Resumed, and New Role in Advocacy Pursued, After Skiing Accident
Nancy A. Lieberman knew she was in trouble as soon as she lost control of her skis and landed in a thicket of trees while on a family vacation in 2007 in Colorado. She heard her neck snap and lay in the snow yelling for help until she was found. She was flown to a nearby hospital while her husband and eight-year-old son, unaware of what had happened, waited to meet her for lunch.
The accident fractured her neck and injured her spinal cord, resulting in total and permanent paralysis of both her legs and trunk. After several surgeries and rehabilitation, she regained some use of her arms and now has limited use of her fingers.
 Ms. Lieberman’s injuries led to severe medical complications, including dangerously fluctuating blood pressure. She was placed on a ventilator for three weeks. While she recovered in Colorado, her family selected The Mount Sinai Hospital for her transfer. “They absolutely picked the right place because of all of my complications,” she says. “I needed a full-service hospital.”
Ms. Lieberman’s injuries led to severe medical complications, including dangerously fluctuating blood pressure. She was placed on a ventilator for three weeks. While she recovered in Colorado, her family selected The Mount Sinai Hospital for her transfer. “They absolutely picked the right place because of all of my complications,” she says. “I needed a full-service hospital.”
About a year after her accident, Ms. Lieberman returned to her position as a partner in the law firm Skadden Arps, where she specializes in mergers and acquisitions, and where she remains at the top of her professional game. In 2015, she was one of 75 attorneys named to the National Law Journal’s list of Outstanding Women Lawyers and one of 50 women selected worldwide by Harvard Law School as an honoree for its International Women’s Day celebration. In 2013, Ms. Lieberman was named a Dealmaker of the Year by The American Lawyer for her work on two important pharmaceutical deals.
 She and her family continue to travel, and vacations have taken them on safari in Botswana; to Morocco, where she rode a camel; and to London. As a director of the Pacific Council on International Policy, she visited the Great Hall of the People in Beijing, where she ascended the 62 marble steps by resourcefully using the stone dividers as ramps. “Unfortunately, no one has yet written a book called ‘Paraplegia for Dummies,’” she says. “So you have to be creative and come up with solutions for day-to-day challenges.”
She and her family continue to travel, and vacations have taken them on safari in Botswana; to Morocco, where she rode a camel; and to London. As a director of the Pacific Council on International Policy, she visited the Great Hall of the People in Beijing, where she ascended the 62 marble steps by resourcefully using the stone dividers as ramps. “Unfortunately, no one has yet written a book called ‘Paraplegia for Dummies,’” she says. “So you have to be creative and come up with solutions for day-to-day challenges.”
She believes that there is a lack of advocacy on behalf of people with paralysis. “Spinal cord injury is not what I’d call a ‘popular’ medical condition, like cancer or heart disease,” she says. “It doesn’t affect a wide enough cross section of the population or an empowered constituency to get the attention it needs. There’s not as much funding as you would think.”
 Therefore, she has taken on the advocacy role herself. When she learned that New York State improperly cut $8.5 million per year in mandated funding for spinal cord research, she co-founded New Yorkers to Cure Paralysis. The group led the effort to successfully restore funding, and Governor Andrew M. Cuomo subsequently appointed Ms. Lieberman to the New York State Spinal Cord Injury Research Board. In that position, she conferred with scientists at the National Institutes of Health and the California Institute of Regenerative Medicine to learn about best practices for the state to adopt when selecting research projects to fund.
Therefore, she has taken on the advocacy role herself. When she learned that New York State improperly cut $8.5 million per year in mandated funding for spinal cord research, she co-founded New Yorkers to Cure Paralysis. The group led the effort to successfully restore funding, and Governor Andrew M. Cuomo subsequently appointed Ms. Lieberman to the New York State Spinal Cord Injury Research Board. In that position, she conferred with scientists at the National Institutes of Health and the California Institute of Regenerative Medicine to learn about best practices for the state to adopt when selecting research projects to fund.
Years after the accident, Ms. Lieberman feels fortunate to be living in New York City with access to Mount Sinai. “It’s a place where I feel people really care,” she says. “I’m grateful that there’s a place where people like me can go to get their lives back.”
Expanding Uses for Powered Exoskeletons
The Mount Sinai Hospital’s Department of Rehabilitation Medicine Bionics Research Program continues to grow. In 2015, the Department launched a pilot study—possibly the first—to explore the safety and feasibility of using a powered exoskeleton, the ReWalk™, for persons with multiple sclerosis (MS). To date, the study has enrolled 14 participants with the goal of examining adverse events, tolerability, ease of learning, and patients’ ability to walk with the device.
This study builds on previous research at Mount Sinai that examined the clinical benefits of the ReWalk and Ekso™ exoskeletons for use in spinal cord injury by patients who have use of their arms. Both devices have powered leg attachments that enable individuals to stand upright, walk, and return to sitting. Motors power movement at the hips and knees, and a battery-operated computer coordinates that movement into a walking pattern.

The secondary outcomes being explored in the MS pilot study, called “Feasibility of ReWalk Exoskeleton-Assisted Walking for Persons with Multiple Sclerosis,” include a range of physical-function and quality-of-life measures such as changes in fatigue, sleep, mood, and pain interference. In 2015, investigators shared preliminary results with the New York City chapter of the National MS Society in the presentation “Powered Exoskeletons in MS Rehabilitation: Fantasy or Future?” They also presented their findings as part of an exoskeleton symposium at the American Congress of Rehabilitation Medicine Annual Conference.
Researchers continue to study the usability of walking with the Ekso- and ReWalk-powered exoskeletons for those with spinal cord injury. Since the inception of the Bionics Research Program in July 2012, Mount Sinai has provided more than 860 walking sessions to 57 study participants (mostly outpatients), with good outcomes. Beyond experiencing walking, participants also recorded beneficial secondary changes, including reduced pain and muscle spasticity, improved bowel and bladder function, and sleep.
In 2015, architect Robert Woo, who has had paraplegia since a workplace injury in 2007, became the first person in the United States to be certified to purchase the new ReWalk Personal 6.0 System for use at home. Mr. Woo had participated in a 2013 study with the Ekso device at The Mount Sinai Hospital’s Rehabilitation Center, as part of a clinical trial led by Allan J. Kozlowski, PhD, Assistant Professor of Rehabilitation Medicine at the Icahn School of Medicine at Mount Sinai.
In 2016, researchers are preparing to test the safety and feasibility of the Ekso robotic exoskeleton in inpatient rehabilitation. In separate studies, researchers will examine the implementation of the Ekso for locomotor training for persons with spinal cord injury and with stroke.
Robust Sports Medicine Program Gets Athletes Back Into the Game
Sports Medicine in the Mount Sinai Health System is a robust interdisciplinary program that involves physical medicine and rehabilitation, orthopaedics, radiology, neuropsychology, and emergency medicine.
The medical team, led by Joseph Herrera, DO, the newly appointed Chair of the Department of Rehabilitation Medicine at Mount Sinai Beth Israel, treats elite professional athletes as well as student athletes in the New York City area, and has excellent return-to-play outcomes. As one of only 16 accredited sports medicine programs in the United States that are housed within Rehabilitation Medicine departments, Mount Sinai Beth Israel’s program has also become a leader in research and fellowship training.
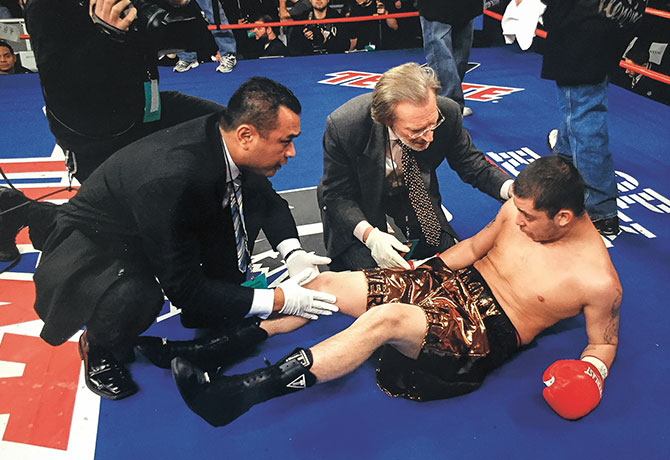
Physicians and staff treat a wide range of musculoskeletal injuries and disorders, focusing on spinal disc herniation, sciatica, and cervical and lumbar conditions. They oversee competitors at the New York City Marathon and other New York Road Runner events and the New York City Golden Gloves and other USA Boxing events, and are the doctors for the football, soccer, and men’s and women’s basketball teams of the Globe Institute of Technology in Manhattan. They also work with high schools in the area, treating shoulders, lower back, neck, and concussions, and have taken a leading role in the Mount Sinai Play Safe program, which provides medical treatment and education about pediatric concussions.
Mount Sinai Beth Israel’s medical staff are at the forefront of research on regenerative medicine, including the use of platelet-rich plasma and stem cells for musculoskeletal injuries, and are leaders in employing ultrasound-guided musculoskeletal and neuromuscular injections. The textbook Atlas of Ultrasound-Guided Musculoskeletal Injections, edited by Dr. Herrera and Mount Sinai colleagues, is one of the most widely used and referenced texts in the field. Dr. Herrera’s research interests include the use of the Wii gaming system to treat shoulder tendinopathy, AposTherapy for back and knee pain, regenerative medicine, and spinal interventions.
Dr. Herrera, who serves as Associate Professor of Rehabilitation Medicine at the Icahn School of Medicine at Mount Sinai, additionally has helped build a highly selective, nationally renowned fellowship program that trains two fellows each year. Four full-time physiatrists—who together conduct more than 19,000 patient visits and perform more than 3,500 interventional procedures per year—actively participate in didactic and clinical education for the fellows.
Excellence in Spinal Cord and Brain Injury Care
The Mount Sinai Rehabilitation Center is accredited by the Commission on Accreditation of Rehabilitation Facilities (CARF) for 17 programs across the continuum, including Spinal Cord System of Care, Brain Injury, Stroke, Amputation Specialty Program, and the Comprehensive Inpatient Rehabilitation Program.
The Center is the only CARF-accredited program in New York City for both spinal cord injury and brain injury and is the first program in New York State to achieve CARF accreditation in post-amputation care.
Message from the Chair: Kristjan T. Ragnarsson, MD
Last spring, I announced my plans to step down on June 30, 2016, as the Chair of the Department of Rehabilitation Medicine after serving 30 years in that position. It has been a privilege for me to have worked with outstanding colleagues and staff members at this great academic medical institution.
The Mount Sinai Health System has enabled us to provide the best imaginable rehabilitation medicine services to thousands of individuals with disability and painful conditions caused by either injury or disease. A search committee, headed by Joshua B. Bederson, MD, Chair of Neurosurgery, has been established and includes chairs of key clinical departments and institutes, as well as top administrative leaders.
 During the search, departmental activities continue with vigor. Our clinical mission remains to provide comprehensive rehabilitation services for persons with disability and help them to return to all areas of community life. We also strive to educate the public and professionals about the diverse needs of people with disability, while conducting groundbreaking research to enhance the health, mobility, self-care skills, quality of life, and community integration of our patients.
During the search, departmental activities continue with vigor. Our clinical mission remains to provide comprehensive rehabilitation services for persons with disability and help them to return to all areas of community life. We also strive to educate the public and professionals about the diverse needs of people with disability, while conducting groundbreaking research to enhance the health, mobility, self-care skills, quality of life, and community integration of our patients.
Unfortunately, many individuals do not recover from disabling conditions despite remarkable advances in medical and surgical care and promising developments in research. Our goals for those patients is to enable them to return to what they did best before the onset of their disability, whether resuming their family roles or making use of their special talents.
Among the features in this Report, we profile two extraordinary individuals who sustained severe spinal cord injuries resulting in profound disability. Yet, through their comprehensive rehabilitation at Mount Sinai and their own hard work, they have successfully carried on with their remarkable careers. They are among the thousands who have overcome disability by using their talents for their own benefit and that of our society.
Kristjan T. Ragnarsson, MD, is the Dr. Lucy G. Moses Professor and Chair of the Department of Rehabilitation Medicine, Mount Sinai Health System.
Rehabilitation Medicine
Download the Winter 2016 Specialty Report