Study Provides Further Evidence That Immune Cell Dysregulation is a Driver of COVID-19 Severity
Maintenance of reparative lung macrophages may be a viable therapeutic strategy for the treatment of SARS-CoV-2 and other inflammatory lung diseases
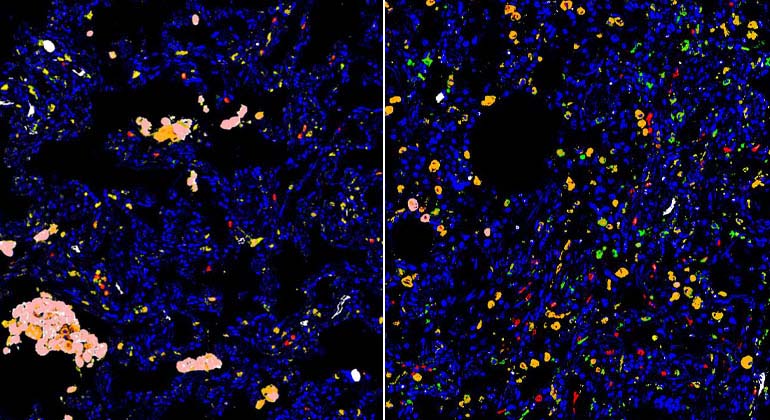
Immunohistochemistry staining of lung autopsy tissue sections showing decrease in Alveolar Macrophages (pink) in COVID+ lungs (Right) compared to COVID- control (Left). Credit: Science Translational Medicine
In one of the largest single-center COVID-19 cohort studies to date, researchers at the Icahn School of Medicine at Mount Sinai, using samples collected during the peak of the pandemic in New York City, have identified a key driver of COVID-19 disease severity.
The findings, published in the September 14 edition of Science Translational Medicine, suggest that lung damage is linked to the loss of immune cells called macrophages that normally reside in the lung and organize tissue repair, followed by an influx of new macrophages from the blood into the lung that cause inflammation. Blocking the entry of inflammatory macrophages and preventing the loss of reparative lung resident macrophages may be a therapeutic strategy for treating SARS-CoV-2 and other viral lung diseases.
Nearly three years since the start of the COVID-19 pandemic in late 2019, the virus continues to fuel a worldwide health crisis.
“Despite the development of vaccines that prevent disease, and therapies to treat COVID-19 and other infections, these critical viral diseases remain a major unmet need in medicine,” said lead author Steven Chen, a recent MD/PhD graduate in the laboratory of Miriam Merad, MD, PhD, a senior author of the study and Director of the Marc and Jennifer Lipschultz Precision Immunology Institute (PrIISM) at the Icahn School of Medicine at Mount Sinai. “Our study sought to identify drivers of disease severity and mortality in order to identify therapeutic strategies that could halt the progression of severe lung viral infections.”
In the study, blood and lung fluid samples of healthy controls and 583 COVID-19 patients admitted to Mount Sinai were collected as part of the Health System’s COVID-19 Biobank. The cohorts were longitudinally followed from March through December 2020.
The investigators used serum proteomics and immune cell phenotyping to compare the two groups' systemic immune responses and identify potential disease severity drivers that could predict which patients were most at risk and guide new treatment protocols. They found that COVID-19 severity was linked to a shift in the specialized functions of different macrophage populations in the lung. This may partly explain why older adults, who have fewer reparative lung resident macrophages to start with and can produce more inflammatory blood-derived macrophages, may be predisposed to severe disease, say the researchers.
The researchers emphasize that the study highlights the need to improve measurements of the immune system in patients. “Clinically available immune tests are very limited, which is unfortunate because understanding the composition of immune cells circulating in the blood, and the inflammatory molecules they produce, can be extremely informative and help identify new treatments for many different diseases,” says Dr. Merad.
“Our study demonstrates that immune profiling could help stratify patients according to their disease drivers and identify therapeutic strategies tailored to these drivers,” said Dr. Merad. “In our investigation, a subset of patients could have significantly benefited from restoring reparative lung resident macrophages. The use of immune profiling studies in the clinic would have helped make this call quite early during the disease process.”
“Together with co-senior authors Alex Charney, MD, PhD, and Sacha Gnjatic, PhD we are now following our COVID-19 cohort described in this study and will compare extensive immune profiling of the patients who develop long COVID with those who fully recover, in order to identify drivers and treatment strategies for long COVID.”
The paper is titled, “A shift in lung macrophage composition is associated with COVID-19 severity and recovery.”
This work was funded by National Institutes of Health grants F30CA243210, U24CA224319, U01DK124165, P30CA196521, NCI 75N91020R00055, R33CA263705, U24AI118644-05S1, and P30CA196521-05S2.
About the Icahn School of Medicine at Mount Sinai
The Icahn School of Medicine at Mount Sinai is internationally renowned for its outstanding research, educational, and clinical care programs. It is the sole academic partner for the eight- member hospitals* of the Mount Sinai Health System, one of the largest academic health systems in the United States, providing care to a large and diverse patient population.
Ranked 14th nationwide in National Institutes of Health (NIH) funding and among the 99th percentile in research dollars per investigator according to the Association of American Medical Colleges, Icahn Mount Sinai has a talented, productive, and successful faculty. More than 3,000 full-time scientists, educators, and clinicians work within and across 34 academic departments and 35 multidisciplinary institutes, a structure that facilitates tremendous collaboration and synergy. Our emphasis on translational research and therapeutics is evident in such diverse areas as genomics/big data, virology, neuroscience, cardiology, geriatrics, as well as gastrointestinal and liver diseases.
Icahn Mount Sinai offers highly competitive MD, PhD, and Master’s degree programs, with current enrollment of approximately 1,300 students. It has the largest graduate medical education program in the country, with more than 2,000 clinical residents and fellows training throughout the Health System. In addition, more than 550 postdoctoral research fellows are in training within the Health System.
A culture of innovation and discovery permeates every Icahn Mount Sinai program. Mount Sinai’s technology transfer office, one of the largest in the country, partners with faculty and trainees to pursue optimal commercialization of intellectual property to ensure that Mount Sinai discoveries and innovations translate into healthcare products and services that benefit the public.
Icahn Mount Sinai’s commitment to breakthrough science and clinical care is enhanced by academic affiliations that supplement and complement the School’s programs.
Through the Mount Sinai Innovation Partners (MSIP), the Health System facilitates the real-world application and commercialization of medical breakthroughs made at Mount Sinai. Additionally, MSIP develops research partnerships with industry leaders such as Merck & Co., AstraZeneca, Novo Nordisk, and others.
The Icahn School of Medicine at Mount Sinai is located in New York City on the border between the Upper East Side and East Harlem, and classroom teaching takes place on a campus facing Central Park. Icahn Mount Sinai’s location offers many opportunities to interact with and care for diverse communities. Learning extends well beyond the borders of our physical campus, to the eight hospitals of the Mount Sinai Health System, our academic affiliates, and globally.
-------------------------------------------------------
* Mount Sinai Health System member hospitals: The Mount Sinai Hospital; Mount Sinai Beth Israel; Mount Sinai Brooklyn; Mount Sinai Morningside; Mount Sinai Queens; Mount Sinai South Nassau; Mount Sinai West; and New York Eye and Ear Infirmary of Mount Sinai.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.