Largest Genetic Study of Suicide Attempts Confirms Genetic Underpinnings That Are Not Driven by Underlying Psychiatric Disorders
An international consortium of scientists dissects the shared genetic architecture of suicide attempts, psychiatric disorders, and non-psychiatric risk factors
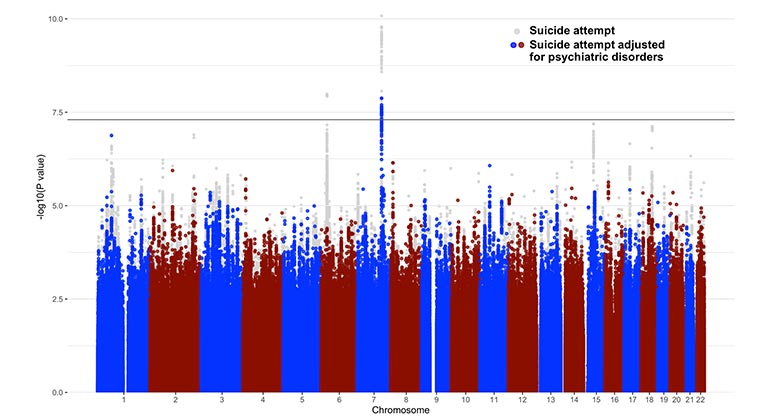
In the largest genetic study of suicide attempts to date, researchers have identified a region of the genome on chromosome 7 containing DNA variations that increase the risk that a person will attempt suicide.
The study also found overlap in the genetic basis of suicide attempts and that of related psychiatric disorders, particularly major depression, and also with that of non-psychiatric risk factors such as smoking, risk-taking behavior, sleep disturbances, and poorer general health. The study results, published November 30 in Biological Psychiatry, suggest that the genetic underpinnings of suicide attempts are partially shared and partially distinct from those of related psychiatric disorders.
Suicide is a worldwide public health problem, accounting for almost 800,000 deaths per year. Non-fatal suicide attempts are estimated to occur more than 20 times for every death by suicide and are a major source of disability, reduced quality of life, and social and economic burden. Suicidal thoughts and behaviors can be reduced with proper mental health support and treatment. Therefore, it is critical to gain insight into the underlying biological pathways involved in suicide attempts or suicidal thoughts, which could provide potential avenues to treatment and prevention strategies.
To help elucidate the underlying biology of suicide attempts, an international consortium of scientists from the International Suicide Genetics Consortium conducted a genome-wide association study. This method involves scanning the DNA of many people, looking for genetic markers that were more common in those who had made a suicide attempt. The team scanned more than 7.5 million common variations in the DNA sequence of nearly 550,000 people, almost 30,000 of whom had made a suicide attempt.
“In addition to identifying the risk location for suicide attempt on chromosome 7, we uncovered a strong overlap in the genetic basis of suicide attempt and that of psychiatric disorders, particularly major depression, as well as some overlap with the genetics of smoking, pain, risk-taking, sleep disturbances, and poorer general health,” said Niamh Mullins, PhD, Assistant Professor of Psychiatric Genomics at the Icahn School of Medicine at Mount Sinai, co-founder and co-chair of the consortium, and lead author of the paper. “This genetic overlap with non-psychiatric risk factors was largely unchanged by adjusting for psychiatric disorders, which suggests that a substantial component of the biological basis of suicide attempt is not simply a byproduct of comorbid psychiatric disease, but instead may be the result of shared biology with non-psychiatric risk factors.”
The association between genetic variations on chromosome 7 and risk of attempting suicide was also not mediated by comorbid psychiatric disorders, and was replicated through an independent analysis of more than 14,000 veterans who had made a suicide attempt from the Million Veterans Program, a national research program to learn how genes, lifestyle, and military exposures affect health and illness.
“This study is an exciting advancement of our understanding of how the genetics of suicide attempt relate to that of psychiatric and non-psychiatric risk factors,” said JooEun Kang, an MD-PhD student at Vanderbilt University Medical Center and co-lead author of this paper.
DNA variations in this region have previously been linked with insomnia, smoking, and risk-taking behavior, and although future work is needed to uncover the underlying biological mechanism, findings like these bring researchers a step closer to understanding the neurobiology of suicidality.
“The study findings also point to the importance of studying the potential direct causal paths between these risk factors and suicide attempt in patients with and without psychiatric illness,” added Douglas Ruderfer, PhD Associate Professor of Genetic Medicine, Psychiatry, and Biomedical Informatics at Vanderbilt University Medical Center, co-founder and co-chair of the consortium, and senior author of the paper.
The International Suicide Genetics Consortium includes more than 260 scientists in more than 20 countries who are dedicated to studying the genetic basis of suicidality. Their work provides the foundation for future larger studies to identify genetic risk factors for suicide attempts in other areas of the genome, as well as additional studies focused on suicidal thoughts. The ultimate goal of this research is to gain insight into the underlying biological pathways involved in suicidality, providing potential avenues to treatments and prevention strategies.
If you are in crisis, please call the National Suicide Prevention 24-hour Lifeline at 1-800-273-TALK (8255), or contact the Crisis Text Line by texting TALK to 741741, or visit their website at: http://suicidepreventionlifeline.org.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.