Breakthrough Technology Used to Discover Eye Damage from Repeated Intravitreal Injections
Findings may lead to new treatment approaches to counteract this problem
In a first of its kind study, Mount Sinai researchers are using optimal coherence tomography angiography (OCTA) to measure potential retina damage from long-term use of intravitreal eye injections. The findings, published in the April issue of Retina, suggest that repeated use of these injections, a popular therapy for common eye conditions—could contribute to progressive vision loss after many years. The results may also lead to changes in the way eye conditions are treated.
Intravitreal injections are the most widely performed procedure for a variety of eye diseases, including macular degeneration, diabetic retinopathy, and retinal vein occlusion that largely affect the Medicare population. Ophthalmologists perform millions of these procedures each year in the United States, and patients often receive these injections monthly or bi-monthly for the rest of their lives to manage their chronic eye conditions. Since the use of these injections to treat eye diseases is fairly new, (before the year 2000 they were used occasionally to deliver antibiotics for severe infections) doctors do not yet understand the long-term consequences of this delivery method. This is what prompted the study.
“These injections cause eye pressure to temporarily go up three times normal levels, and while patients typically recover within minutes, we wanted to know the immediate impact on blood flow to the eye,” said senior investigator Richard Rosen, MD, Deputy Chair for Clinical Affairs in the Department of Ophthalmology at the Icahn School of Medicine at Mount Sinai, who is also the Belinda Bingham Pierce & Gerald G. Pierce Distinguished Chair of Ophthalmology, and Director of Retina Services at New York Eye and Ear Infirmary of Mount Sinai (NYEE). “Recently, we have become aware that repeated mild trauma to central nervous system structures, such as minor head bumps in athletes, can lead to degenerative brain injury with devastating results, decades later. We wanted to better understand any potential risk for similar kinds of injury to the eye.”
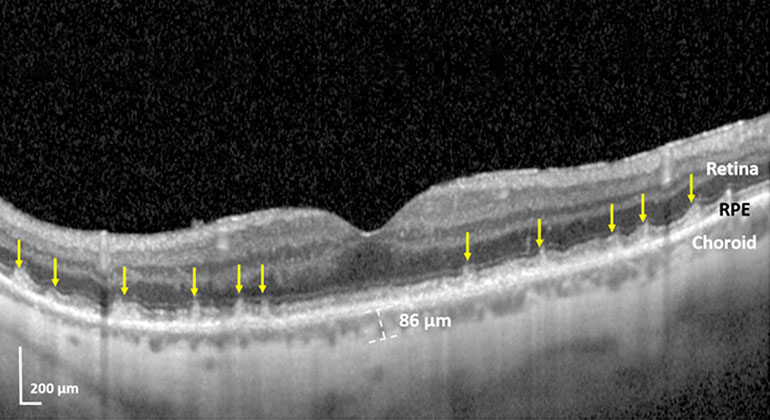
OCTA is an advanced imaging system that captures the motion of red blood cells in blood vessels noninvasively, as opposed to traditional angiography, which uses dye injections Using OCTA, Dr. Rosen and his team analyzed the eyes of 39 patients over age 18 after they received intravitreal bevacizumab or aflibercept injections for diabetic retinopathy, macular degeneration, choroidal neovascular membrane, retinal vein occlusion, or radiation retinopathy. Minutes after the injections, the researchers measured blood flow in different areas of the macula and optic nerve. On average, they found a significant and temporary spike in eye pressure along with a significant and temporary reduction of blood flow that eventually resolved. They discovered that some areas of the macula and nerve were stressed more than others, and this newfound information can lead doctors to use advanced imaging and visual field testing to look for early signs of damage.
“This study is important because we know that high eye pressure leads to tissue damage in glaucoma. If patients are receiving monthly injections that repeatedly stress the eye, we may have to start looking for signs of cumulative damage,” explained lead author Alexander Barash, MD, Clinical Assistant Professor of Ophthalmology at The New York Eye and Ear Infirmary of Mount Sinai. “As doctors, we always have to weigh the benefits of any treatment with risks to the patient. If we are inadvertently causing damage to ocular structures with our injections we should make sure that all physicians performing the procedure are aware of possible side effects so they can discuss these with patients and work to minimize the risks of these treatments.”
This study could pave the way for doctors to pre-treat patients with medications to reduce their spikes in eye pressure after getting injections to protect them from possible long-term damage. The findings may also lead doctors to more carefully consider the risks in patients with advanced glaucoma (who already have high levels of eye pressure) before treating them with injections.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.
Blinding Eye Disease Strongly Associated With Serious Forms of Cardiovascular Disease
Nov 17, 2022 View All Press Releases
High-Tech Imaging Offers New Way to Detect Signs of Early Glaucoma
Aug 02, 2022 View All Press Releases
Blinding Eye Disease Is Strongly Associated With Heart Disease and Stroke
Jul 12, 2022 View All Press ReleasesThree Mount Sinai Ophthalmologists Receive Prestigious Achievement Awards
Dec 01, 2020 View All Press Releases