Mount Sinai Study Reveals New Genetic Link to Heart Disease
Findings may help improve risk prediction tools for cardiovascular disease
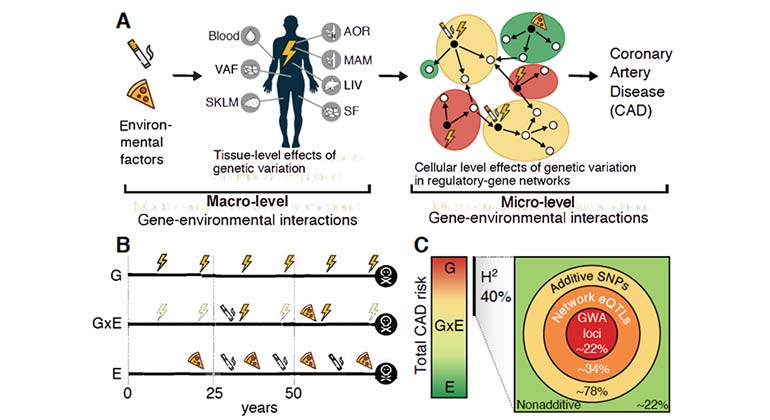
How "environmentally triggered" genetic variants of cellular gene networks contribute to heart disease heritability. (A) Schematics of the macro- and micro levels of gene-environmental interactions. Macro-environmental factors (e.g., lifestyle, food intake and smoking) interact with genetic variants in organs to change the micro-environment in cellular networks leading to heart disease.
A collaboration involving the Icahn School of Medicine at Mount Sinai, the German Heart Center Munich, AstraZeneca, and Karolinska Institutet in Sweden has demonstrated that more than 30 percent of heart disease risk stems from genetic factors, much more than was previously understood. The study findings, published June 18th in the Journal of the American College of Cardiology, introduce the biology of gene networks as means to better understand the heritability and genetic underpinnings of heart disease.
Coronary artery disease (CAD), the most common type of heart disease and one of the leading causes of death worldwide, forms plaque in the walls of the arteries that supply blood to the heart. A complete blockage of these arteries can lead to a heart attack or stroke.
Before this study, more than a decade of genome-wide-association studies (GWAS)—the analysis of genetic risk codes found more frequently in people with a particular trait, such as heart disease—had indicated that less than a quarter of CAD was considered inheritable. Meanwhile, the heritability contribution (if any) of genetic variants in gene regulatory networks (GRNs)—a set of genes that interact with each other to control a particular cell function—was unknown. In light of this, researchers used tissue data from two separate studies of individuals with CAD to determine whether genetic variants that regulate GRNs make independent contributions to the risk of heart disease.
Across vascular and metabolic tissue data, researchers identified and replicated 28 independent GRNs active in CAD and determined that the genetic variation in these networks contributed to the inherited risk of the heart disease by an additional 11 percent—adding to the 22 percent attributable risk previously identified by GWAS. This newfound contribution boosts the heritability of CAD to approximately 32 percent, spotlighting the important role played by interactions between internal environments and genetic variants—mediated by regulatory networks—in the development of heart disease.
“The results of this study demonstrate that the risk of heart disease is a concerted result of interactions between genetic variants and biological environments,” said Johan LM Björkegren, Professor of Medicine (Cardiology), and Genetics, at the Icahn School of Medicine at Mount Sinai. “By understanding the complex relationship between the two, we’ve created a framework for identifying new risk genes in disease-relevant tissues leading to heart disease, which in turn will allow for more effective risk prediction, clinical intervention, and eventually, opportunities for novel and more effective therapies.”
Another researcher involved in the study, Heribert Schunkert, MD, Professor of Cardiology at the German Heart Center in Munich, added, “A mystery of recent research was the fact that many genes contributing to the genetics of coronary artery disease affect mechanisms that were not expected in this context. The present study leads to a much better understanding of how these genes work together in precipitating or preventing the disease.”
Li-Ming Gan, Vice President of Early Clinical Development, Cardiovascular, Renal and Metabolism, R&D BioPharmaceuticals, AstraZeneca, commented that this study “provides new insight into the heritability of coronary artery disease, adding a substantial number of genetic variants contributing to its heritability. Further analysis may help explain the disease’s etiology and give novel insights on how to prevent its development.”
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.