Study Demonstrates Ability to Preserve Long-Term Vision for Severe Patients with Uveitis
Research Examines Effectiveness of Leading Treatment Approaches
Researchers comparing leading treatment approaches for patients with severe uveitis have discovered that systemic therapy with oral corticosteroids and immunosuppression can preserve or improve vision in the long term better than regional implant therapy can. The results, published in the May 6, 2017 issue of JAMA, should reassure physicians about the relative safety of this approach, and may lead ophthalmologists to change their treatment protocol for better and safer outcomes.
Douglas Jabs, MD, MBA, Director of the Eye and Vision Research Institute, New York Eye and Ear Infirmary of Mount Sinai, and Professor of Ophthalmology and Medicine, Icahn School of Medicine at Mount Sinai, chaired an international team of researchers as they examined the long-term effects of two treatment approaches for patients with vision-threatening uveitis. Uveitis, the fifth leading cause of vision loss in the United States, is a collection of more than 30 diseases characterized by inflammation inside the eye that damages the tissues; without appropriate treatment, it will often lead to visual impairment or blindness. For more severe cases, treatment generally calls for taking oral corticosteroid and immunosuppressive medications. The alternative is regional therapy, either with repetitive corticosteroid injections or with a surgically placed fluocinolone acetonide implant that releases corticosteroid medication over three years. Since most of the more severe uveitis cases are chronic, long-term therapy is typically needed.
The Multicenter Uveitis Steroid Treatment (MUST) Trial Follow-up Study followed 215 patients from the original MUST Trial for seven years. The MUST Trial and Follow-up Study were conducted at 21 medical centers across the United States, along with two sites in the United Kingdom and Australia. Patients in the Trial had been randomized to receive either systemic treatment with oral corticosteroids and immunosuppression or regional therapy with the fluocinolone acetonide implant. At the seven-year mark, the findings showed that patients taking oral medications had better vision on average, compared to those in the implant group. The results differ from the initial MUST Trial findings and from the earlier five-year results of the MUST Follow-up Study, in which the same patients had similar visual outcomes at both time points.
The MUST Trial and Follow-up Study also showed that there was no significant increase in the risks of systemic side effects for the systemic therapy group compared to implant therapy, with one exception: patients in the systemic group were more likely to receive antibiotics for infections. These outcomes suggest that systemic treatment, if used properly, may be given relatively safely for up to seven years.
“The implication of these data is that oral corticosteroids and immunosuppression may be a preferable initial choice for therapy of the more severe uveitides,” explained Dr. Jabs. They have better visual outcomes long-term, fewer ocular side effects, and no apparent significant increase in the risk of systemic side effects, except for the greater use of antibiotics.”
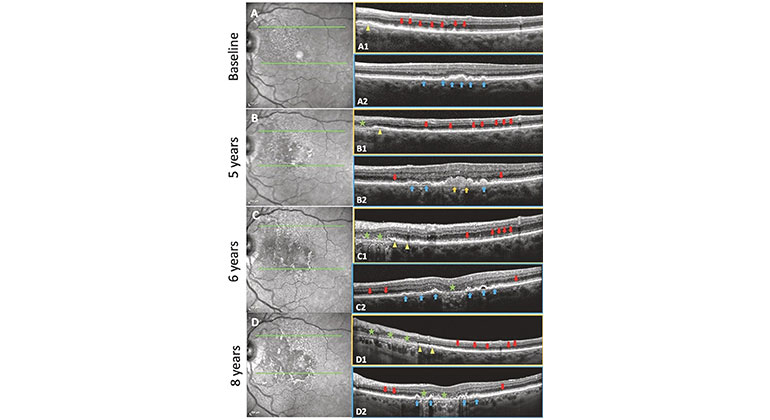
While the large majority of both groups maintained good vision at the end of seven years, some patients with the fluocinolone acetonide implant did worse in terms of visual acuity. Results of the follow-up study show vision loss occurred more often in the implant group due to damage from inflammatory lesions in the back of the eye, which occurred at the time of relapse of the uveitis. Even though the implant is designed to release corticosteroid medication for three years, the study found that the benefit lasted approximately five years, with relapses beginning at that time. Relapses can be treated with an implant exchange or by switching to systemic therapy.
“Although both treatment approaches control the inflammation in the large majority of patients, for the first five years the implant was better than systemic therapy at controlling inflammation. Hence it has value for those patients where systemic therapy cannot control the inflammation or for those patients who cannot tolerate the oral medications,” said Dr. Jabs. He notes the implant has an important role to play in the management of these diseases. “The visual loss that occurred in the implant group with relapse of the uveitis emphasizes the need of sustained control of inflammation in order to optimize visual outcomes in patients. These patients need close follow-up for reactivation of the inflammation, so that appropriate adjustments to treatment can be made.”
The National Eye Institute (NEI), which is part of the National Institutes of Health, supported the MUST Trial and MUST Trial Follow-up Study.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.
Blinding Eye Disease Strongly Associated With Serious Forms of Cardiovascular Disease
Nov 17, 2022 View All Press Releases
High-Tech Imaging Offers New Way to Detect Signs of Early Glaucoma
Aug 02, 2022 View All Press Releases
Blinding Eye Disease Is Strongly Associated With Heart Disease and Stroke
Jul 12, 2022 View All Press Releases