Restless legs syndrome
Willis-Ekbom disease; Nocturnal myoclonus; RLS; Akathisia
Restless legs syndrome (RLS) is a nervous system problem that causes you to feel an unstoppable urge to get up and pace or walk. You feel uncomfortable unless you move your legs. Moving stops the unpleasant feeling for a short time.
This disorder is also known as restless legs syndrome/Willis-Ekbom disease (RLS/WED).
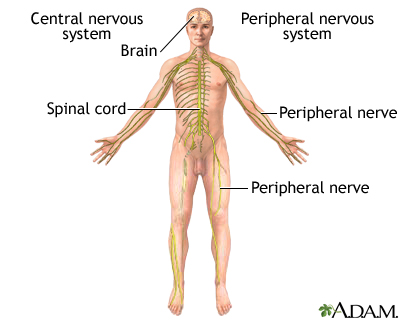
The central nervous system is comprised of the brain and spinal cord. The peripheral nervous system includes all peripheral nerves.
Causes
No one knows exactly what causes RLS. It may be due to a problem with the way brain cells use dopamine. Dopamine is a brain chemical that helps with muscle movement.
RLS may be linked to some other conditions. It may occur more often in people with:
- Chronic kidney disease
- Diabetes
- Iron, magnesium, or folic acid deficiency
- Anemia (often due to iron deficiency)
- Parkinson disease
- Peripheral neuropathy
- Pregnancy
- Multiple sclerosis
RLS may also occur in people who:
- Use certain medicines such as calcium channel blockers, lithium, or neuroleptics
- Are stopping sedative use
- Use caffeine, alcohol, or nicotine
RLS occurs most often in middle-aged and older adults. Women are more likely to have RLS than men.
RLS is commonly passed down in families. This may be a factor when symptoms start at a younger age.
Symptoms
RLS leads to unpleasant feelings in your lower legs. These feelings cause an unstoppable urge to move your legs. You may feel:
- Creeping and crawling
- Bubbling, pulling, or tugging
- Burning or searing
- Aching, throbbing, or pain
- Itching or gnawing
- Tingling, pins and needles in the feet
These sensations:
- Are worse at night when you lie down to the point that it may interfere with sleep and keep you awake
- Sometimes occur during the day
- Start or get worse when you lie down or sit for long periods of time
- May last for 1 hour or longer
- Sometimes also occur in the upper legs, feet, or arms
- Are relieved when you move or stretch as long as you keep moving
Symptoms can make it difficult to sit during air or car travel, or through classes or meetings.
Stress or emotional upset can make symptoms worse.
Most people with RLS have rhythmic leg movements when they sleep. This condition is called periodic limb movement disorder.
All of these symptoms make it hard to sleep. Lack of sleep can lead to:
- Daytime sleepiness
- Anxiety or depression
- Confusion
- Difficulty thinking clearly
Exams and Tests
There is no specific test for RLS. Your health care provider will take your medical history and do a physical exam. You may have blood tests and other exams to check for conditions that can cause similar symptoms. Your provider may order blood tests to look for iron deficiency anemia and other medical problems.
Sleep studies may be done to check for other conditions.
Usually, your provider will determine whether you have RLS based on your symptoms.
Treatment
RLS can't be cured. However, treatment can help relieve symptoms.
Certain lifestyle changes may help you cope with the condition and ease symptoms.
- Get enough sleep. Go to bed and wake up at the same time every day. Make sure your bed and bedroom are comfortable.
- Try using hot or cold packs on your legs.
- Help your muscles relax with gentle stretches, massage, and warm baths.
- Take time out of your day to just relax. Try yoga, meditation, or other ways to ease tension.
- Avoid caffeine, alcohol, and tobacco. They may make symptoms worse.
Your provider may prescribe medicines to treat RLS.
Some medicines help control symptoms:
- Pramipexole (Mirapex)
- Ropinirole (Requip)
- Low doses of narcotics
Other medicines can help you sleep:
- Sinemet (combination carbidopa-levodopa), an anti-Parkinson medicine
- Gabapentin and pregabalin
- Clonazepam or other tranquilizers
Medicines to help you sleep may cause daytime sleepiness.
Treating conditions with similar symptoms such as peripheral neuropathy or iron deficiency can also help relieve symptoms.
Outlook (Prognosis)
RLS is not dangerous. However, it can be uncomfortable, making it hard to sleep and affecting your quality of life.
Possible Complications
You may not be able to sleep well (insomnia).
When to Contact a Medical Professional
Contact your provider for an appointment if:
- You have symptoms of RLS
- Your sleep is disrupted
- Symptoms get worse
Prevention
There is no way to prevent RLS.
References
Allen RP, Montplaisir J, Walters AS, Hogl B, Ferini-Strambi L. Restless legs syndrome (Willis-Ekbom disease) and periodic limb movements during sleep. In: Kryger M, Roth T, Goldstein CA, Dement WC, eds. Principles and Practice of Sleep Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 121.
Avidan AY. Sleep and its disorders. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 101.
National Institute of Neurological Disorders and Stroke website. Restless legs syndrome.
Winkelman JW, Armstrong MJ, Allen RP, et al. Practice guideline summary: treatment of restless legs syndrome in adults: report of the Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology. Neurology. 2016;87(24):2585-2593. PMID: 27856776
Version Info
Last reviewed on: 8/28/2023
Reviewed by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. Editorial update 01/19/2024.
