Department of Orthopaedic Surgery
By combining medical care with meaningful research in both clinical and basic science areas, we will improve the practice of orthopaedic surgery.
Department of Orthopaedic Surgery
The Leni and Peter W. May Department of Orthopaedic Surgery is recognized for its depth of expertise and personalized patient care.
This report highlights:
- Studying transformative treatments for intervertebral disc repair
- Rotator cuff repair with iliac crest bone graft
- Resection of thigh sarcoma involving the sciatic nerve
- Helping to identify—and protect—nerves during surgery
- Revision hip surgery in a patient with multiple diseases
Studying Transformative Treatments for Intervertebral Disc Repair
Lumbar discectomy is the most common procedure for patients with intervertebral disc (VD) herniation, a common condition affecting the spines of the young and middle-aged. While discectomy, which accounts for more than 300,000 operations each year in the United States, provides favorable outcomes in many cases, in others—such as large disc protrusions with minimal disc degeneration—a significant gap in treatment persists.
“Discectomy is a great procedure for addressing the acute pain and disability that come from herniation, but it leaves the defect unrepaired,” says James Iatridis, PhD, Professor of Orthopaedic Surgery, and Neurosurgery, and Director of Spine Research for the Mount Sinai Health System. “We now have the potential to significantly improve long-term outcomes with safe, minimally invasive injections of cells or other bioactive factors. These could be transformative for the field of annulus repair.”
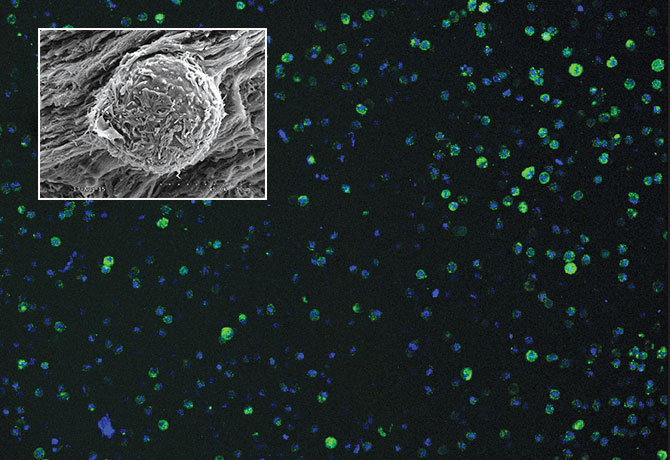
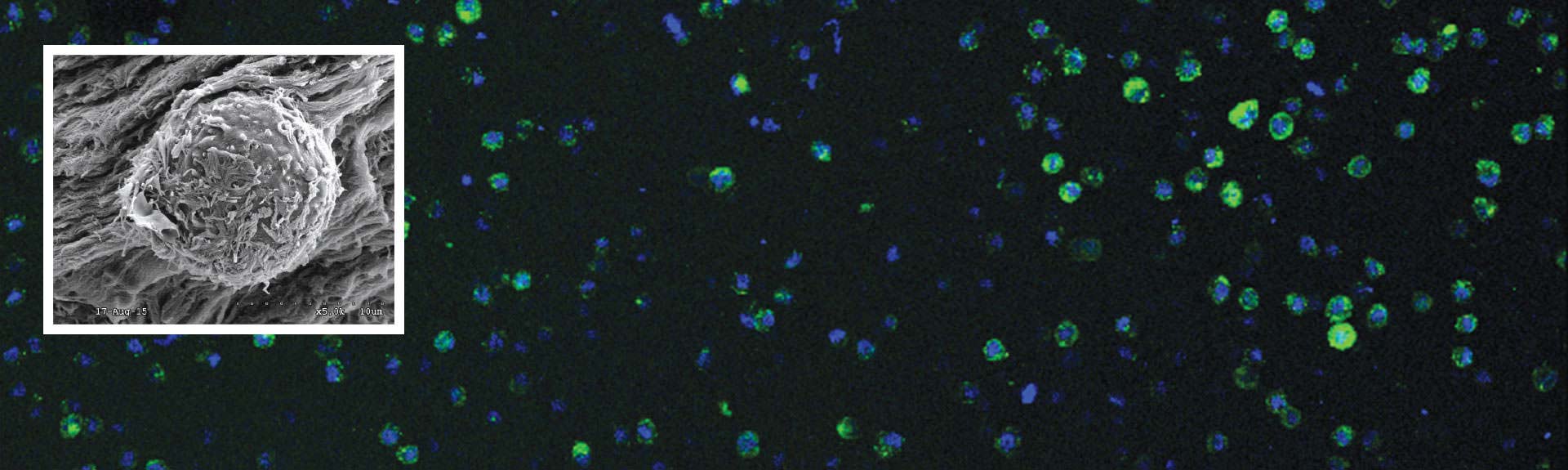
Mount Sinai’s Department of Orthopaedics has emerged as a global leader in innovative biomaterial strategies for repairing the annulus fibrosus (AF), the tough circular exterior of the intervertebral disc composed of a ring of ligament fibers that is involved in almost all degenerative spine pathologies.
One promising area of study involves a naturally occurring biomaterial, fibrin, a sealant derived from the patient’s blood, that is modified using genipin, a natural cross-linking agent, for use in intervertebral discs. This hydrogel can serve as a sealant for tears and fissures in the AF, which, if not repaired, can lead to protrusion of the gelatinous, highly hydrated nucleus pulposus. This cell-free injectable, developed in Dr. Iatridis’s lab, would not only close the defect and allow natural healing, but also restore many of the mechanical behaviors of a healthy intervertebral disc. This project is currently in large-animal trials in Switzerland as part of Mount Sinai’s participation in an international consortium funded by the AO Foundation, a nonprofit organization that is supporting research on innovative tissue engineering approaches to AF repair.
Other approaches, directed at cell delivery, have engaged a variety of Mount Sinai researchers working under the scientific umbrella of the Spine Hospital at Mount Sinai. Cell delivery addresses the problem of increased cell death, senescence, and lack of paracrine factors in the degenerative disc. Newly recruited cells are intended to repopulate the region where native cells and the extracellular matrix (ECM) of collagens and proteoglycans have been lost. The arrival of cells and biologically active compounds to the degenerative disc not only promotes ECM production, but also new tissue formation. The seminal work that is under way is expected to soon move from the cell-culture to organ-culture stage.
Among the deficiencies in the AF field that Mount Sinai is addressing is what Dr. Iatridis calls “the fragmented and often narrowly focused” research efforts of the past. The Spine Hospital’s response is an interdisciplinary collaboration of basic scientists, biologists, bioengineers, orthopedic surgeons, neuroradiologists, pain specialists, and physiatrists—each focused on the same clinical problem from different perspectives. “We believe we are on the verge of developing, over the next several years, effective new treatments for biological annular repair, and our diverse team of scientists and clinicians are excited about these collaborative and possibly transformative areas of research,” says Dr. Iatridis.
Rotator Cuff Repair With Iliac Crest Bone Graft
The patient is a 14-year-old otherwise healthy right-hand-dominant male who in 2014 presented with left shoulder pain to the orthopedic clinic and was attended to by Ilya Iofin, MD, Chief of Orthopaedic Oncology Service, The Mount Sinai Hospital, and Assistant Professor of Orthopaedics, Icahn School of Medicine at Mount Sinai.
Except for shoulder pain, his clinical examination was unremarkable. Radiographs showed a lucent epiphyseal lesion of the proximal humerus with well-demarcated borders that did not appear to be aggressive in nature. The patient’s MRI revealed a high T2, low T1 proximal humerus epiphyseal lesion. He was diagnosed with chondroblastoma and underwent excision of lesion, cryotherapy, iliac crest bone grafting, and cement augmentation. Given his age and his physis still being open, the excision of the lesion was performed after takedown of the supraspinatus muscle, which was repaired at the end of the case.
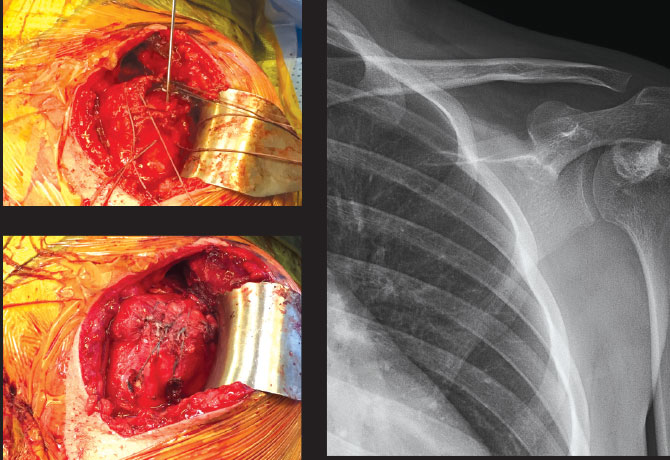
One year postoperative, the patient presented to the orthopedic clinic with shoulder pain and an inability to raise his left arm. He was seen by Bradford Parsons, MD, Associate Professor of Orthopaedics, Icahn School of Medicine at Mount Sinai, and Residency Program Director, Leni and Peter W. May Department of Orthopaedic Surgery. On physical examination, his left shoulder range of motion was 80 degrees of forward flexion, 60 degrees of external rotation, and internal rotation to T8.
Passively, his shoulder would forward flex to 170 degrees. He was neurovascularly intact with good deltoid tone. Radiographs revealed no evidence of recurrent lesion with bone cement in place. An MRI was obtained, which revealed a rotator cuff tear of the supraspinatus. After the risks and benefits of new therapies were discussed with the patient and his family, it was collectively decided that in order to give him the best function of his left shoulder, a surgical procedure would be required.
At surgery, he was found to have a supraspinatus tear with previous bone cement visible. The cement was removed, which created a void at the footprint of the rotator cuff. To increase healing potential of the rotator cuff, iliac crest bone graft was obtained and placed at the footprint. The rotator cuff muscle was then repaired on top of the bone graft in a double row fashion. At his postoperative visit three months later, he had no shoulder pain and was able to forward flex his left shoulder to 170 degrees.
Resection of Thigh Sarcoma Involving the Sciatic Nerve
The patient, a 31-year-old father of two young children, had been living with a mass in his right thigh for more than two years. He initially thought it was a growing muscle, but when the mass started to grow quickly and cause shooting pains into the foot, he suspected that something was wrong. An MRI was obtained showing a very large mass in the thigh that was suspicious for a cancer. The tumor was encasing the sciatic nerve and abutting the popliteal vessels (Figure 1).
The patient was referred to Ilya Iofin, MD, Chief of Orthopaedic Oncology Service, The Mount Sinai Hospital, and Assistant Professor of Orthopaedics, Icahn School of Medicine at Mount Sinai. Dr. Iofin performed a needle biopsy and made the diagnosis of myxoid liposarcoma, a very rare cancer. Staging studies showed that the cancer had not spread and was localized to the thigh.
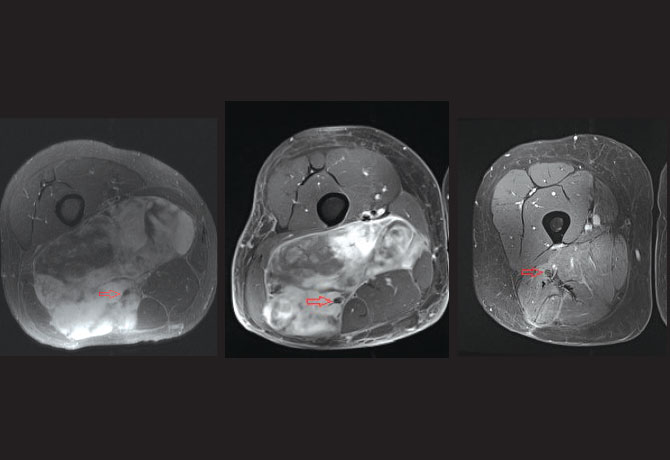
Dr. Iofin discussed with the patient the possibility of having to remove the nerve with the tumor to rid the patient of his cancer, which would lead to numbness in the foot and the need to wear a brace. However, because myxoid liposarcoma is very sensitive to radiation, the patient was referred for radiation prior to surgery in an attempt to shrink the cancer and free up the sciatic nerve. After five weeks of radiation, the tumor got smaller, and an MRI showed that the sciatic nerve was at the edge of the tumor rather than running through it (Figure 2).
The decision about whether to save or remove the sciatic nerve would be made during surgery. At the time of surgery, Dr. Iofin carefully explored the sciatic nerve and its branches and found that the radiation had shrunk the tumor sufficiently and the nerve was free of cancer. The tumor was removed in its entirety.
The patient recovered well after the surgery. His sciatic nerve functions without a problem, he has returned to his job and family life with his wife and children, and he follows up regularly with Dr. Iofin. As seen on the most recent MRI (Figure 3), the patient has been cancer-free for more than a year.
Helping to Identify—and Protect—Nerves During Surgery
The patient is a young athlete who had five shoulder dislocations. Eventually, he underwent a Latarjet procedure to stabilize the shoulder at an outside hospital. Unfortunately, when he awoke, he was unable to move his arm due to accidental injury to the brachial plexus, the group of nerves that control the muscles of the arm. The patient was referred to Michael R. Hausman, MD, the Dr. Robert K. Lippmann Professor of Orthopaedics at the Icahn School of Medicine at Mount Sinai and Chief of Hand and Upper Extremity Surgery for the Mount Sinai Health System. Dr. Hausman has special expertise in microsurgery and peripheral nerve reconstruction.
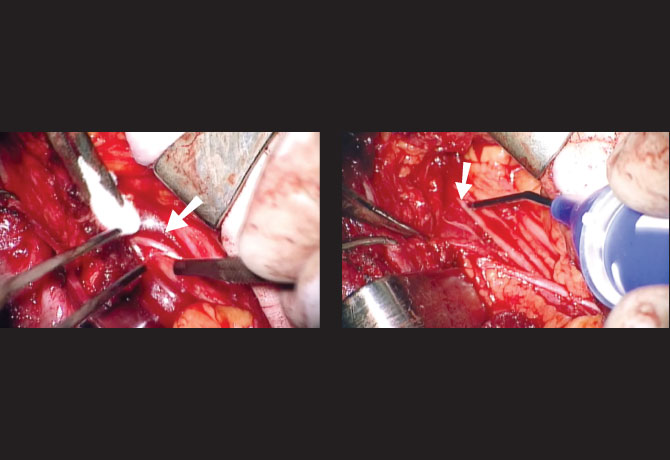
Right:The Checkpoint Stimulator is used to stimulate and assess the function of the nerve fibers, seen as the long, cord-shaped structures (arrow). The presence of a response in the biceps with stimulation of the nerve means that the prognosis for recovery is good.
Accidental injury to nerves during surgery is a very serious complication, frequently resulting in paralysis and loss of sensation. Neuroprotective surgery techniques developed by Dr. Hausman at Mount Sinai can help prevent and, in some cases, treat these injuries. Challenged by complex reconstructive cases with distorted anatomy that can put nerves at increased risk, Dr. Hausman created technology now embodied in the Checkpoint Nerve Locator/Stimulator. The hand-held instrument is used to help identify and protect nerves during surgery to prevent accidental injury. It also allows the surgeon to assess the condition and function of a damaged nerve intraoperatively to decide if a damaged nerve segment can recover or if it needs to be replaced by a nerve graft. Preservation of the native, original nerve can lead to better outcomes, as it did in this patient’s case.
Using the Checkpoint Stimulator to probe the nerve as he dissected it under the high magnification of the operating microscope, Dr. Hausman determined that a thorough “cleaning” procedure—an internal neurolysis—would likely be beneficial and yield a much better outcome in strength and mobility than nerve grafting, which would take a year or more to show any improvement. As the viable nerve elements were painstakingly freed from the scar, the stimulator showed improved function of the nerve in the damaged segment, indicating a high probability of recovery. Within days, the patient was able to bring his hand to his face, and by six weeks after surgery, his strength had returned to near normal.
Protection of nerves during surgery has become the standard of care, and these techniques are increasingly utilized not only in orthopedics, but also in many surgical fields, including otolaryngology, plastic surgery, urology, and general surgery, among others, to help prevent injuries as well as to repair damaged nerves and restore function to arms and legs. For example, difficult hip or knee replacements, nerve-sparing tumor resections, trauma surgery and vascular procedures, and even transplant surgery can be performed more safely using Mount Sinai’s neuroprotective techniques.
Michael R. Hausman, MD, owns equity in Checkpoint Surgical.
Revision Hip Surgery in Patient With Multiple Diseases
The patient is an 84-year-old male with a previous medical history of advanced cardiac disease (ejection fraction 15 percent), stage 4 chronic kidney disease, and a history of multiple myeloma and thyroid cancer, both now in remission. He fell off his bicycle in 1976 and underwent open reduction/internal fixation of right hip fracture. Ten years later, he underwent a total hip replacement followed by revision surgery in 2006.
About two years prior to his referral to Calin S. Moucha, MD, Chief of Adult Reconstruction and Joint Replacement Surgery, The Mount Sinai Hospital, and Associate Professor of Orthopaedics, Icahn School of Medicine at Mount Sinai, the patient began having progressively worsening right groin pain that reached 9/10 in intensity, difficulty ambulating without a walker, as well as significant pain putting on his shoes.
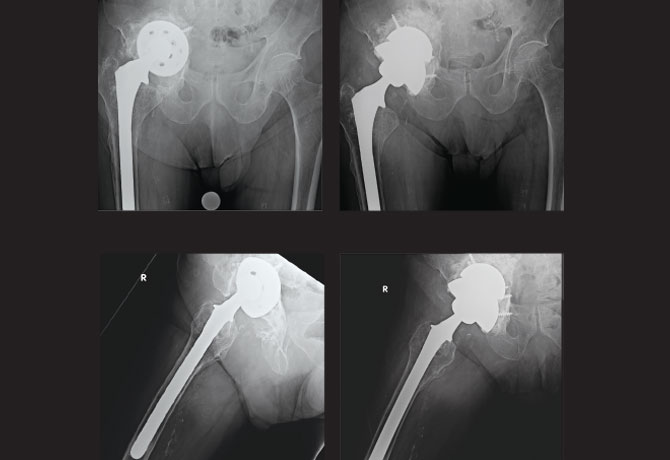
His physical exam was significant for an antalgic gait, limited motion throughout the right hip, and a flexion/external rotation contracture. Stinchfield test and Trendelenburg sign were both positive. Shortening of the affected limb was noted. Pulses were palpable and neurological function was fully intact.
Radiographs showed a well-fixed cementless revision femoral component. Loose revision acetabular component was visualized with complete destruction of the teardrop, violation of Kohler line, and migration > 3 cm superior to the obturator line. Superior-medial migration of the acetabular component was visualized on radiographs defining a Paprosky Type IIIB defect. CT scan confirmed no lytic lesions or periosteal formation suggestive of multiple myeloma or metastatic thyroid disease. Infection workup was negative.
The complexity of the case from an orthopedic and medical standpoint was explained in detail to the patient and his family. The patient was taken to the operating room for revision surgery under general anesthesia and an epidural.
The femoral stem was well-fixed and well-positioned. The acetabular bone stock, as predicted, was creating pelvic discontinuity. Dr. Moucha reconstructed the pelvis using a 62mm revision trabecular metal shell press fit into the superior defect, bone grafting using cancellous bone, followed by an 80mm revision trabecular metal shell placed inferiorly in distraction. Multiple screws were placed including into the ischial spine as well as in remaining areas of bone. The shells were unitized using antibiotic loaded cement. The liner was cemented into appropriate anteversion (a few degrees more than the shell), and a 40mm head was used to optimize stability.
His postoperative course was uneventful. The patient was allowed to bear weight as tolerated with a walker for eight weeks, followed by unassisted weight bearing as tolerated thereafter. At the latest 19-month follow-up, the patient’s radiographs showed a stable construct. He was ambulating pain-free without any assistive devices and enjoyed getting back to gardening.
Chair’s Message from Leesa M. Galatz, MD
I am extremely pleased to report on the outstanding performance of the Department of Orthopaedic Surgery at the Mount Sinai Health System, which is recognized for its depth of expertise and personalized patient care.
Leesa M. Galatz, MD, Mount Sinai Professor in Orthopaedics and Chair, Leni and Peter W. May Department of Orthopaedic Surgery
We are now ranked among the top Orthopaedic Surgery programs by U.S. News & World Report. Additionally, The Joint Commission recently recognized two of our institutions as centers of excellence in total hip and knee replacement, joining only a few programs nationwide that have received this distinction for quality and safety.
The Health System reaches across the New York City area with networks that extend throughout the region, giving our physicians and investigators unique opportunities to advance medical care through meaningful research in clinical and basic science areas. Additionally, through a culture of collaboration within the Health System—combining the talents and resources of the Icahn School of Medicine at Mount Sinai and our seven hospital campuses—we expect to gather robust data on our large and diverse group of patients and grow our Orthopaedic Research Laboratory.
I am fortunate to welcome several new faculty members of various subspecialties who will help us build on the great work of our clinicians, researchers, and staff.
It is our outstanding faculty that drives our Department’s commitment to offer restorative treatments that can have a dramatic impact on patients’ lives.
The next several years hold great promise as the Department grows, and we realize our academic potential through first-rate patient care and breakthrough research initiatives.
Department of Orthopaedic Surgery
Download the Winter 2017 Specialty Report
