
Department of Ophthalmology
We are continuing to build on the commitment of New York Eye and Ear Infirmary of Mount Sinai (NYEE) and the Mount Sinai Health System to set new standards in ophthalmic clinical care, medical education, and clinical research.
Department of Ophthalmology
Our long-term goal is to advance new diagnostic and therapeutic innovations while continuing our longstanding commitment to providing the highest quality, compassionate, and patient-centric care as well as training and educating the next generation of leaders in eye care and research.
This report highlights:
- A patient story: Despite traumatic injury, her sight is saved
- Describing the basic biological mechanisms by which defective cells cause exfoliation glaucoma
- A new approach to address NAION: Use a synthetic RNA to protect neurons
- A drainage implant device that shows promise as an alternative to trabulectomy for glaucoma
- Two uveitis fellowship programs combined
- A novel microcatheter used for pediatric glaucoma
- OCT angiography transforms imaging for many common retinal diseases
Stabbed 27 Times, but Her Sight Is Saved
When 32-year-old Julissa Marquez sustained 27 stab wounds to the head, face, and eyes in December 2013, she was told by the trauma specialist who saw her at a New York City-area hospital that she would never see again. She had suffered bilateral open globe injuries and subsequent bilateral retinal detachments. The consulting plastic surgeon proposed removing her left eye, but with no sign of infection, Ms. Marquez rejected that recommendation.
The next day she went to the Emergency Department of New York Eye and Ear Infirmary of Mount Sinai (NYEE), where she was referred to Ronald Gentile, MD, FACS, FASRS, Professor of Ophthalmology at the Icahn School of Medicine at Mount Sinai and Chief of Ocular Trauma Service (Posterior Segment) at NYEE. Dr. Gentile agreed that her prognosis was extremely poor. “I thought the chances of her ever being able to see again were less than 10 percent,” he says. Despite the odds, he promised Ms. Marquez that he would do whatever he could to restore her vision. “That’s what made Dr. Gentile stand out from all the doctors who examined me,” she says.
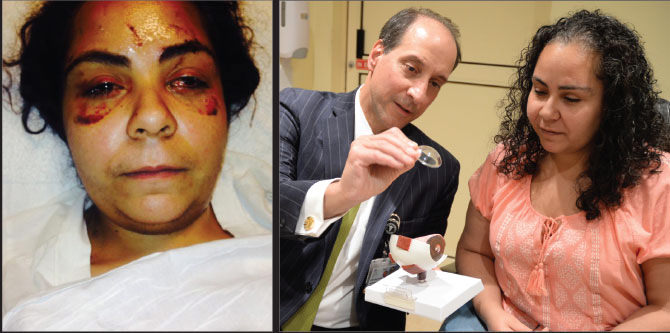
Right: Ronald Gentile, MD, with Ms. Marquez during a follow-up visit three years later.
Ms. Marquez had sustained a 15 mm scleral laceration zone 3 in her right eye resulting in choroidal hemorrhage and total retinal detachment with incarceration. Her left eye suffered a 20+ mm scleral laceration resulting in retinal detachment, minimal remaining retina, and no light perception. Based on her Ocular Trauma Score (OTS), which is used to assess patients after open-globe ocular trauma and predict their visual outcome following treatment, Dr. Gentile thought the likelihood that she would regain as much vision as she has was about 3 percent. Today, nearly three years and approximately 10 surgeries later, her vision has been restored to 20/100 with glasses in her right eye, enough to give her independence.
After performing external choroidal drainage on the right eye, Dr. Gentile and his team were able to identify the site of retinal incarceration. They then performed a pars plana lensectomy (PPL), leaving the anterior lens capsule intact. After removing preretinal and subretinal membranes, they opened and flattened the retina using perfluorocarbon liquid. Endolaser was applied 360 degrees, followed by direct perfluorocarbon liquid-silicone oil exchange. Six weeks later, they performed a capsulotomy after removing the silicone oil. They removed extensive proliferative vitreoretinopathy (PVR) membranes and suprachoroidal silicone oil. This was followed by endolaser and silicone oil injection after fluid air exchange (FAX).
Following PPL surgery in her left eye, Perfluoro-N-octane (PFO) was used to reattach the small amount of retina still present. Additional procedures included endolaser, suture pupilloplasty, and silicone oil injection. Over the next seven weeks, the patient developed PVR. As a last resort, the surgical team removed her preretinal and subretinal membranes, followed by an endolaser procedure and direct perfluorocarbon-silicon oil exchange. She also had two strabismus surgeries to correct the alignment of her eyes, performed by Anthony Panarelli, MD, Associate Adjunct Surgeon at NYEE, and Steven Rosenberg, MD, Interim Director of Pediatric Ophthalmology and Adult Strabismus at NYEE. She has no vision in her left eye, though she can perceive hologram-type images.
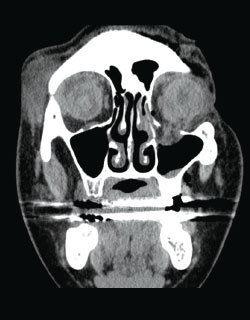
At the present time, it appears that her vision has stabilized, but Dr. Gentile is alert to new technologies that may become available to improve her vision further. He continues to monitor her regularly because she remains prone to additional eye ailments as a result of the trauma.
“I give credit to our entire team of retina surgeons who defied the odds and gave Julissa sight,” says Dr. Gentile. “Ocular trauma is very complex, not only medically, but also emotionally, for the patient and family, and not all eye surgeons are willing to take on some of these cases.” Other surgeons who were part of the team included Gennady Landa, MD, Assistant Professor of Ophthalmology at the Icahn School of Medicine at Mount Sinai, and Khushboo K. Agrawal, MD, who trained with Dr. Gentile at NYEE before going to North Mississippi Medical Center in Tupelo, where she is the region’s first full-time retina surgeon.
Despite near-constant pain, Ms. Marquez is pleased with her outcome. “I tell everyone my story,” she says. “I was told by four different doctors that I would never see again and now I can read from my iPad. There’s always hope.”
Describing the Basic Biological Mechanisms by Which Defective Cells Cause Exfoliation Glaucoma
Glaucoma research took a major leap forward in 2007 with the discovery by a genetic consortium in Iceland of two distinct mutations in the LOXL1 (lysyl oxidase-like gene, which codes for a family of enzymes involved in the synthesis and maintenance of elastic tissues. Nearly a decade later, a team in the Department of Ophthalmology at the Icahn School of Medicine at Mount Sinai is again pushing the boundaries of research by describing for the first time the basic cellular mechanism of a major type of glaucoma.
Exfoliation syndrome (XFS) is the most common recognizable cause of open-angle glaucoma worldwide, accounting for the majority of glaucoma cases in some countries.
“I’ve been saying for years that this is a potentially preventable, reversible, and even curable disease,” says Robert Ritch, MD, Shelley and Steven Einhorn Distinguished Chair and Director of Glaucoma Research at NYEE, as well as founder and Scientific Advisory Board chair of The Glaucoma Foundation.
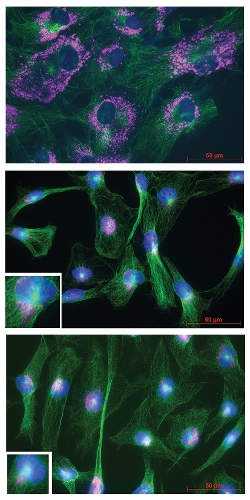
To those ends, he decided about six years ago to “go for broke” by pouring Foundation resources and funding into studying exfoliation syndrome, an age-related systemic disease characterized by the production and accumulation of a whitish, flaky material in ocular and non-ocular tissues. In addition to organizing the annual Optic Nerve Rescue and Regeneration Think Tank, which bring together scientists and clinicians from around the world to focus on exfoliation syndrome, Dr. Ritch helped launch at Mount Sinai with private grant money a project to explore cellular defects that lead to exfoliation glaucoma.
Cell biologists Audrey Bernstein, PhD, Associate Professor of Ophthalmology, and J. Mario Wolosin, PhD, Professor of Ophthalmology at the Icahn School of Medicine at Mount Sinai, began collecting tissue samples from the eyes of exfoliation glaucoma patients. After culturing these tissue samples in their labs, the researchers compared their results from exfoliation patient-derived cells to other neurodegenerative diseases, like Alzheimer’s and Parkinson’s.
This led to an important discovery: discernable defects in the autophagy system, which cells employ to rid themselves of toxic aggregates, and in the lysosome, the end-point organelle that acts as the “garbage disposal.” Explains Dr. Bernstein: “Our hypothesis is that if you don’t degrade the garbage, this trash or exfoliation material gets thrown outside the cell and into the outflow pathway of the eye, thereby contributing to elevated intraocular pressure.”
While allowing that researchers are “extremely excited” about their findings so far, Dr. Bernstein acknowledges they are at an early stage. “We’re working toward the goal of reversing exfoliation, and our next steps are to mechanistically figure out why these cellular defects are occurring and to more specifically target the pathways.” Another priority is to use the human-derived exfoliation cells to begin screening drug libraries in search of corrective agents.
Dr. Ritch is no less optimistic about new cellular and genetic approaches to a disease with no known means of prevention. “Nanotechnology could be a way to disaggregate and dissolve the exfoliation material, while fixing the genes could be a way to prevent the disease from ever developing,” he says. “We’re definitely making progress toward a cure.”
New Approach to Address NAION: Use a Synthetic RNA to Protect Neurons
For Rudrani Banik, MD, Associate Professor of Ophthalmology at the Icahn School of Medicine at Mount Sinai, nothing is more frustrating than having to inform patients with nonarteritic anterior ischemic optic neuropathy (NAION) how little she can do to help them. “These patients come to me with a devastating loss of vision in one or both eyes, and I’m not able to give them much hope,” she laments. “Even though many drugs, even surgery, have been tried, nothing has really proven to work.”
Giving Dr. Banik some comfort is the fact that she is playing an active role in the search for a solution. She is a site investigator at New York Eye and Ear Infirmary of Mount Sinai (NYEE) for the largest study ever undertaken to address NAION. The phase 2/3 trial just getting underway will test a highly promising small interference RNA (siRNA) developed by Quark Pharmaceuticals that acts as a neuroprotective agent for the treatment of the disease, as well as other optic neuropathies, (e.g. glaucoma), resulting in the death of retinal ganglion cells. The global study is being conducted through NORDIC (Neuro-Ophthalmalogy Research Disease Investigator Consortium), a Mount Sinai Health System-directed clinical trials research network. NORDIC has been awarded nearly $2.3 million to co-direct the trial with Quark.
“Quark needed someone to fine-tune their study and provide the sites and know-how to get a trial of this size done,” notes NORDIC chair Mark Kupersmith, MD, Chief of the Division of Neuro-Ophthalmology at NYEE. “What NORDIC offers is a network of certified sites equipped to provide strong organizational and operational support to researchers, including single data coordination and a biostatistics center.”
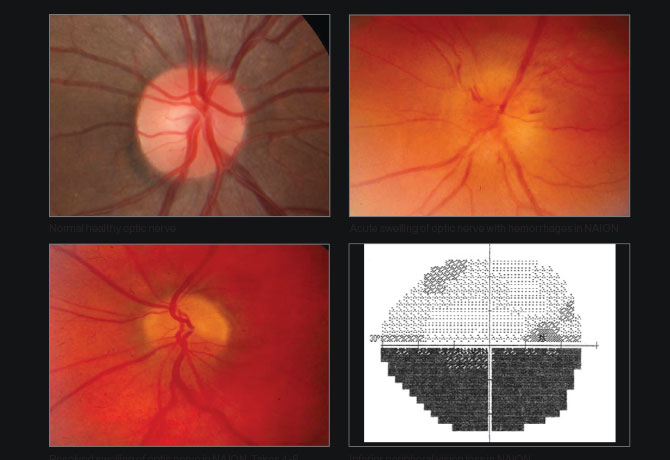
The Quark/NAION study will tap into NORDIC’s grid of 50 sites across the United States and Canada, as well as others In Europe, Israel, Australia, and Asia.
In targeting NAION, the partnership between Quark Pharmaceutical and Mount Sinai is addressing the most common acute optic nerve injury in individuals over age 50, which strikes 12,000 people annually in the United States and is caused by a sudden decrease in the blood circulation to arteries supplying the optic nerve. There are no approved therapies for the disorder, which appears in a single eye and in 20 percent of cases strikes the other eye at a later date. There is a risk of permanent blindness.
This clinical trial represents the first use of a neuroprotective drug for a major neuro-ophthalmic problem. Specifically, the siRNA under investigation inhibits expression of the caspase 2 gene, a key enzyme in the apoptosis cycle which causes the death of retinal ganglion cells following ischemic damage to the optic nerve. Scientists have shown that by blocking caspase 2, the drug—which is delivered through an intravitreal injection—can provide protection to the optic nerve.
Why has NAION been so resistant to treatment over the years? “Like the brain and the spinal cord, the optic nerve can’t heal itself once an ischemic injury occurs,” explains Dr. Banik, who was a site investigator for phase 1 of the Quark drug trial.
“Treatments to date have all been rescue therapies that don’t address the real problem, which is cells dying off due to a lack of oxygen to the optic nerve. This drug is the first specifically aimed at stopping that cascade of events which leads to programmed cell death, and it will hopefully result in a positive treatment strategy for patients.”
Drainage Implant Device Shows Promise As Alternative to Trabulectomy for Glaucoma
Glaucoma specialists are optimistic about an implant device that has the potential to transform glaucoma surgery. In a unique prospective, randomized, controlled, single-masked, multicenter trial with two-year follow-up, the InnFocus MicroShunt™ is being compared to trabeculectomy, the gold standard of glaucoma filtering surgery.
The MicroShunt uses a micro-tube to shunt aqueous fluid from the eye’s anterior chamber to a subconjunctival/sub-Tenon’s space. The shunt is made of the same material used in cardiac stents and has a long history of stability after implantation.
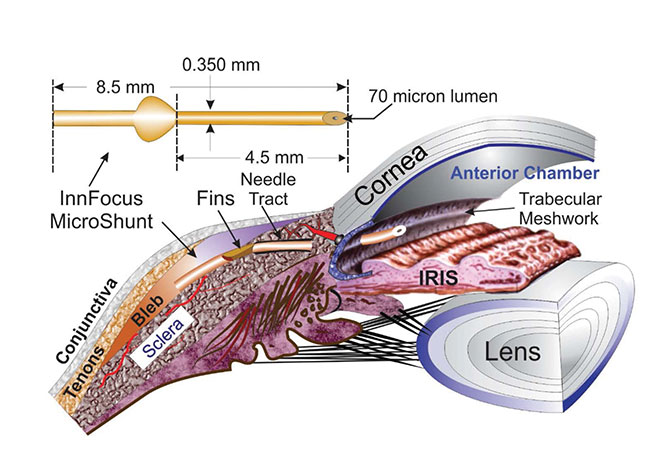
The 8.5mm-long shunt, which conforms to the curvature of the eye, was designed to maintain a level of intraocular pressure in the mid to low teens. Implantation of the MicroShunt takes approximately 15 minutes. It is placed in the anterior chamber through an ab externo scleral needle track tunneled posterior to the limbus.
The subjects in both study groups have primary open angle glaucoma and are inadequately controlled on maximum tolerated medical therapy with intraocular pressures between 15mm Hg and 40mm Hg. The treatment group consists of subjects who receive the InnFocus MicroShunt with mitomycin C (MMC). The control group consists of subjects who receive trabeculectomy with MMC. Phase 1 enrollment of 102 subjects has been completed and the Food and Drug Administration has approved the study to move forward into phase 2/3. The device has been approved in Europe since 2012.
The study is being conducted at 12 sites in the United States, Europe, and the Dominican Republic. New York Eye and Ear Infirmary of Mount Sinai (NYEE) is the only site conducting the trial in the New York area. The NYEE study is being led by Joseph F. Panarelli, MD, Assistant Professor of Ophthalmology at the Icahn School of Medicine at Mount Sinai and Glaucoma Fellowship Director at NYEE, as well as Paul A. Sidoti, MD, Professor of Ophthalmology at the Icahn School of Medicine at Mount Sinai and Director of the Glaucoma Service at NYEE.
Preliminary results are encouraging: there has been a reduction of intraocular pressure of over 50 percent; over 80 percent of eyes treated with the MicroShunt have an IOP of less than 14 mm Hg; there has been more than an 85 percent reduction in glaucoma medication use; and no long-term sight-threatening adverse events have been reported.
Two Uveitis Fellowship Programs Combined
Training the next generation of uveitis specialists is getting a boost from the creation of the Mount Sinai Health System. Separate uveitis fellowship programs at The Mount Sinai Hospital and New York Eye and Ear Infirmary of Mount Sinai (NYEE) are now being combined into one to help physicians master the clinical skills, medical knowledge, and judgment they need to manage the inflammatory eye disease, the fifth leading cause of vision loss in the United States. Specialists in the field manage not just the various types of uveitis, but mucous membrane pemphigoid, and the ocular complications associated with immunosuppression and immunodeficiency, such as AIDS.
“The trick is managing the more severe forms of the disease, which require the use of medications not normally taught to ophthalmologists in residency,” observes Douglas Jabs, MD, MBA, Professor of Ophthalmology and Chair Emeritus of the Department of Ophthalmology at the Icahn School of Medicine at Mount Sinai, who established the Mount Sinai uveitis fellowship program upon joining the hospital 10 years ago. “Our program has an intellectual rigor which teaches fellows how to handle the most complicated and difficult to manage patients.”
Two fellows will be accepted each year into the joint fellowship program, one of only eight in the country. They will spend four or five days a week in outpatient settings seeing patients with attending physicians. Rounding out their education are monthly divisional conferences where fellows present cases, and the Uveitis Journal Club, which also involves second-year residents and uveitis faculty.
The integration of the two fellowship programs was begun as part of the 2013 combination of the Mount Sinai Medical Center and NYEE’s former parent organization, Continuum Health Partners, to form the Mount Sinai Health System. The program merger will be completed in 2017. Leading this effort are Dr. Jabs at Mount Sinai and C. Michael Samson, MD, Assistant Professor of Ophthalmology at the Icahn School of Medicine at Mount Sinai and Co-Director of Uveitis and Ocular Immunology at NYEE.
Novel Microcatheter Used for Pediatric Glaucoma
Childhood glaucoma is relatively rare, but when it occurs, if not detected and treated early, it can cause significant and permanent vision loss.
Fortunately for three-month-old Meagan Charles, her perceptive parents noticed that their newborn’s eyes were getting progressively larger and hazier. They took her to their pediatrician, who referred her to a pediatric ophthalmologist. They could not find a specialist who could see her quickly at two other area hospitals, so they came to New York Eye and Ear Infirmary of Mount Sinai (NYEE).
Meagan’s intraocular pressure was 54 mm Hg in both eyes when she presented. She promptly underwent an examination under anesthesia and had surgery performed by Joseph Panarelli, MD, Assistant Professor of Ophthalmology at the Icahn School of Medicine at Mount Sinai and Glaucoma Fellowship Director at NYEE. The following week, he operated on her second eye. He reports that both surgeries were successful and Meagan’s prognosis is excellent.

High pressure in developing eyes can lead to optic nerve damage, corneal damage, progressive myopia, and amblyopia. Early pressure-induced changes on the optic nerve can be reversed and permanent damage prevented.
Dr. Panarelli performed a 360° trabeculotomy with the iScience microcatheter. This treatment, performed in only a few eye centers nationwide, provides a new, more effective spin on an existing procedure and has enhanced the treatment of pediatric glaucoma. Using the illuminated, flexible microcatheter, the surgeon is able to open the entire length of the Schlemm’s canal.
The illuminated red diode indicator of the probe tip alleviates the problem of the “blind pass” and avoids the potential complications resulting from misdirection of the catheter. It also features a central channel for injecting viscoelastic agents to expand the canal during catheter advancement. The procedure takes approximately 30-45 minutes to perform.
Until recently, when congenital glaucoma patients did not respond to conventional angle surgery, they often required additional procedures to treat the remainder of the angle. With this technique, subsequent surgeries are usually unnecessary if the canal is fully opened.
Dr. Panarelli doesn’t expect Meagan to need additional surgeries. Her eyes have shown a marked improvement a week after surgery. Her corneas are clear, changes in the optic nerves have reversed, and her intraocular pressure is around 12 mm Hg in both eyes. “This is the best outcome we could have hoped for,” he said. For now, drops are not needed and he will continue to monitor her progress closely over the next several months.
“Pediatric glaucoma is one of the most challenging conditions that I treat, but it is also one of the most rewarding aspects of my practice,” says Dr. Panarelli. “I feel privileged to be able to help restore sight to children at a crucial stage in their intellectual and social development. As the father of two, I appreciate the impact of visual stimulation on a child’s maturing mind and I want every child I treat to be able to expand their understanding of the world through sight.”
Next Generation for Corneal Transplants
Since New York Eye and Ear Infirmary of Mount Sinai (NYEE) ophthalmologists David Ritterband, MD, and John Seedor, MD, became the earliest adapters of endothelial keratoplasty (EK) in New York ten years ago, outcomes for their corneal transplant patients have been superb. Most now experience uncorrected vision of 20/30 or better; their visual recovery is quicker and their eyes remain stronger compared to traditional full-thickness corneal transplants.
The procedure they currently use–DSAEK (Descemet’s Stripping Automated Endothelial Keratoplasty)–selectively replaces only the diseased layer of the cornea with healthy donor tissue for patients with endothelial cell disorders like Fuchs’s dystrophy, post-cataract corneal surgery edema, and keratoconus. DSAEK has continued to improve through smaller incisions, better tissue preparation, and improvements in how the graft is placed inside the eye, says Dr. Ritterband, Professor of Ophthalmology and Assistant Director of Cornea and Refractive Surgery at NYEE.
Drs. Ritterband and Seedor, who perform nearly 400 transplants a year at NYEE and have been part of numerous clinical studies, have begun transitioning to the next iteration of EK, DMEK (Descemet’s Membrane Endothelial Keratoplasty), in which the patient’s endothelium is replaced with a single cell layer donor corneal endothelium and Descemet membrane without additional stromal tissue. The graft tissue is merely 10-20 microns thick. On the horizon is another technique—pure endothelial cell transplantation using patient cells grown in a petri dish—which could eliminate corneal surgery altogether.
“Corneal transplantation is a dynamic process that keeps producing better vision with less surgical trauma for patients,” points out Dr. Ritterband. And by now being part of the Mount Sinai network, he adds, his busy ophthalmic practice enjoys both a clinical and research advantage as it seeks to remain on the leading edge of the science.
OCT Angiography Transforms Imaging For Many Common Retinal Diseases
A transformation is underway in the field of ophthalmic imaging as fluorescein angiography—the standard of care for diagnosing vascular disorders since its introduction in 1961—gives way to optical coherence tomography (OCT) angiography. By allowing for enhanced visualization of blood flow in the retina and the choroid capillary network and the detection of abnormal blood vessels, OCT angiography is becoming a powerful tool in the hands of ophthalmologists for treating such common retinal diseases as diabetic retinopathy, age-related macular degeneration, and choroideremia.
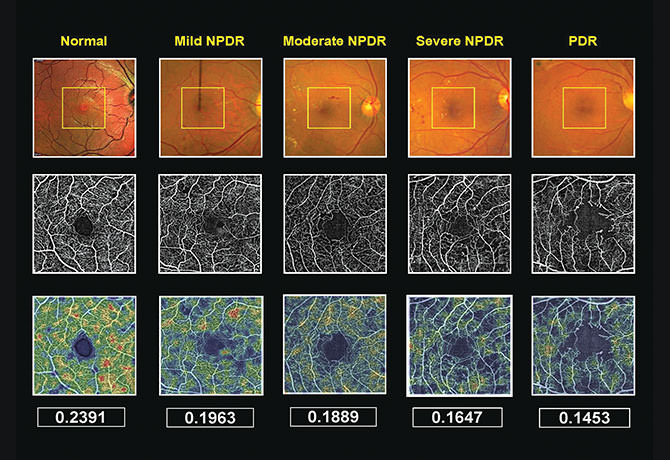
At the Retina Center of New York Eye and Ear Infirmary of Mount Sinai (NYEE), OCT angiography is being used for a growing number of high-value research and clinical applications, such as capillary perfusion density mapping, monitoring the activity of choroidal neovascular membranes, and studying parts of the eye previously undetectable, like the retinal radial paripapillary capillaries and the choriocapillaris, and the retinal nerve fiber layer. A new generation of ophthalmologists is now being trained at NYEE on state-of-the-art systems which allow high-resolution visualization and the ability to detect vascular flow using motion contrast processing (which highlights only features that change) instead of traditional fluorescein dye.
“OCT angiography gives you the ability to study the capillaries in real time and get very precise measurements of change so you can see areas where there is no blood flow,” says Richard Rosen, MD, Director of Ophthalmology Research and Chief of Retinal Services at NYEE. “This technology is helping clinicians to identify progression early and perhaps prevent patients from reaching more advanced stages of the disease without first having adequate imaging.”
An example is diabetic retinopathy, which can take 10 to 20 years to develop in patients with type 1 diabetes. Dr. Rosen’s adaptive optics lab is developing software tools to study perfusion densities (the number of capillaries per cubic millimeter) as a way to scale the progression of the disease. These tools include OCT angiography perfusion density maps and average perfusion density values as an instantaneous way to grade progressive vascular change over a period of months or years.
Glaucoma is another disease where the ability of OCT angiography to assess multiple capillary layers within the retina—including the superficial layer which figures prominently in glaucoma–is raising the prospect of earlier diagnosis and treatment. Dr. Rosen points out that elevated intraocular pressure is not always a marker for glaucoma. “Another group of patients appear to have normal pressure but just lose blood vessels,” he notes. “One of the studies we’ve conducted looks at the different patterns of blood vessel loss—and that may turn out to be very significant in identifying early on which patients have what we call low tension glaucoma before they lose a significant amount of retinal tissue.”
The transition to OCT angiography has taken a decade, but Dr. Rosen feels the science is now poised to overtake fluorescein angiography. “It will continue to grow because it offers quantitative tools we didn’t have before,” he says. And because OCT angiography does not require intravenous administration of dyes, Dr. Rosen adds, “it can be done faster and without any discomfort to patients. This technology clearly has the potential to transform the field of ophthalmology.”
Chair’s Message: Building a New Legacy for NYEE
The merger of the nationally ranked Department of Ophthalmology at New York Eye and Ear Infirmary of Mount Sinai (NYEE) with the storied Department at The Mount Sinai Hospital and at Icahn School of Medicine at Mount Sinai (ISMMS) presents an exciting opportunity to advance eye care throughout the New York metropolitan area, nationally, and internationally. The enormous clinical breadth and depth at NYEE allows for natural synergies with the translational research and educational initiatives of the ISMMS Department of Ophthalmology.

We will continue to focus on clinical research and medical education at NYEE, anchored by the existing Shelley and Steven Einhorn Clinical Research Center and the Jorge N. Buxton Microsurgical Education Center.
We see exciting opportunities in the planned Mount Sinai Downtown campus, which will modernize and enhance our ability to serve patients through the creation of a state-of-the-art Clinical Eye Institute. Our new clinical institute will stimulate the development and advancement of innovative diagnostic technologies and medical therapies through closer collaboration between our leading clinicians and basic scientists at ISMMS and its newly planned Vision Research Institute.
At the same time, the Department is striving to make its clinical research more scientifically rigorous, thereby furthering our translational efforts and focusing on areas such as stem cell/regenerative cell biology, tissue science and bioengineering, optical imaging and functional correlation, and genetics/genomics for ocular diseases. These combined clinical and research efforts will provide a rigorous and superlative training environment for residents, clinical fellows, medical students, graduate students, and postdoctoral fellows.
In the ensuing years, we will continue to build on NYEE’s legacy and set new standards in ophthalmic clinical care, medical education, and clinical research.
James C. Tsai, MD, MBA
President, New York Eye and Ear Infirmary of Mount Sinai
Delafield-Rodgers Professor and System Chair, Department of Ophthalmology, Icahn School of Medicine at Mount Sinai
Department of Ophthalmology
Download the Fall 2016 Specialty Report