
The Hilda and J. Lester Gabrilove Division of Endocrinology, Diabetes and Bone Disease
We provide the highest quality care to patients and are at the forefront of research on endocrine diseases and diabetes.
Endocrinology, Diabetes and Bone Disease
The Hilda and J. Lester Gabrilove Division of Endocrinology, Diabetes and Bone Disease provides the highest quality care to patients and is at the forefront of research on endocrine diseases and diabetes. This report highlights the work of our physicians and scientists in the following areas:
- Cutting-edge research that is reshaping our understanding of thyroid diseases and setting the stage for long-overdue new therapies in areas like Graves’ disease and Hashimoto’s thyroiditis
- Characterizing the complexity of the type 2 diabetes patient population by parsing the electronic medical records and genotype data of more than 11,000 patients included in Mount Sinai’s massive data warehouse
- A study on the prevalence of primary aldosteronism in an urban hypertensive population that found a much lower prevalence of PA than other studies but confirmed PA screening is essential for patients with resistant hypertension
- The opening of the Center for Transgender Medicine and Surgery in Manhattan, among the first of its kind in the country and the first in the New York metropolitan area affiliated with a major academic medical center
From Stem Cells to Thyroid Cells
Lab Work Yields Insights Into Many Diseases
By focusing his career on one gland, the thyroid—and, more specifically, mostly on one molecule, the thyroid-stimulating hormone (TSH) receptor—Terry Davies, MD, is making a difference in the field of hormonal disorders, which afflict up to 10 percent of the population. Cutting-edge research by Dr. Davies, Director of the Thyroid Research Unit in the Division of Endocrinology, Diabetes and Bone Disease and the Florence and Theodore Baumritter Professor of Medicine at the Icahn School of Medicine at Mount Sinai, and his lab team is reshaping our understanding of thyroid diseases and setting the stage for long-overdue new therapies in areas like Graves’ disease and Hashimoto’s thyroiditis.
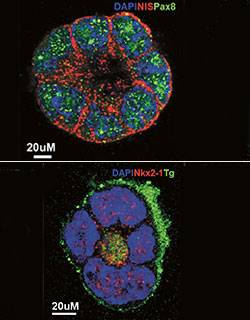
In a major new development, the Mount Sinai researchers are now able to make thyroid cells without overexpressing transcription factors. It is done through chemical induction—exposing the human stem cells or IPS cells to activin A, ethacridine, and TSH. And, as another important step toward turning working thyroid follicles into an actual gland, the team is exploring structural supports to grow thyroid tissue in culture for transplantation—initially into mice.
Dr. Davies’s laboratory is also breaking new ground through its investigation of other promising areas that play a role in thyroid dysfunction, including:
• The role of thyroid antibodies in Graves’ disease. Mount Sinai produced the first monoclonal antibody that stimulates the thyroid TSH receptors as seen in Graves’ disease, a condition caused by an overactive thyroid. Researchers also found that TSH receptors group together in complexes called multimers, which appear to be important to the normal functioning of the receptor. Most recently, they characterized a form of TSH receptor antibody that binds to and actually kills thyroid cells rather than stimulating them.
• Identification of small molecules with therapeutic potential that activate or inhibit the TSH receptor. In the course of screening more than 100,000 molecules through a new high-throughput system that they developed, researchers found two lead candidates with high specificity and potency that activate the receptor, leading to the upregulation of thyroglobulin and TSH receptor expression in mice. The hope is that these molecules can be developed into cheaper treatments for patients, particularly those with thyroid cancer who rely on expensive recombinant TSH.
• Characterization of new variants of TSH that act as bone protectors. TSH impacts not only the thyroid gland, but also other bodily systems like the bones, which it protects from thyroid hormone excess. While TSH is normally triggered by a signal from the pituitary to the thyroid gland, Dr. Davies’s lab uncovered for the first time “local TSH” produced in macrophage cells in the bone. Researchers are now attempting to produce a recombinant version that could act as a bone protector, safeguarding against bone breakdown and osteoporosis. 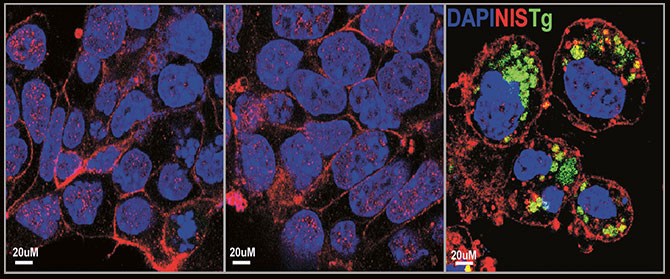
Using Big Data to Redefine Diabetes
Three Clinically Distinct Subtypes Identified
Endocrinologists have long suspected that type 2 diabetes is a heterogeneous disease that could be better treated if patients were grouped by clinically distinct subtypes. By marshaling the power of precision medicine and “big data,” biomedical informatics investigators at the Icahn School of Medicine at Mount Sinai have taken a giant step in that direction, redefining the topography of the disease through research that could lead to more precise diagnosis and treatment strategies.
Led by Joel Dudley, PhD, Director of Biomedical Informatics, the team has characterized the complexity of the type 2 patient population by parsing the electronic medical records and genotype data of more than 11,000 patients included in Mount Sinai’s massive data warehouse. Using computational analysis, the group constructed patient networks based on the similarity of clinical features. From that groundbreaking work, published in Science Translational Medicine in October 2015, three distinct clusters (or subtypes) became apparent. Patients in subtype 1 were most likely to develop diabetic nephropathy and diabetic retinopathy; those in subtype 2 were most at risk for cancer and cardiovascular diseases; and the third subtype was associated with both cardiovascular and neurological diseases, allergies, and HIV infections. Next, through a genetic association analysis of subtypes 1, 2, and 3, the research team identified 1,279, 1,227, and 1,338 single nucleotide polymorphisms, respectively, which in turn mapped to 425, 322, and 437 unique genes.
Mount Sinai researchers hope that from this unique and wide-ranging data analysis will emerge clinical and genetic biomarkers for each subtype, paving the way for tailored treatment regimens instead of the current one-size-fits-all approach to diabetes.
“Our study showed that diabetes is not a homogeneous disease,” Dr. Dudley emphasizes. “Through a precision medicine approach, we demonstrated that we now have the methods and visualization tools to get a handle on the complexity of the disease and start identifying other subtypes among patients who have diabetes along with varying levels of comorbidity expression.” Those comorbidities could include NASH (nonalcoholic stage of hepatitis)—a fatty liver disease linked to metabolic dysfunction—and mental health disorders whose pharmaceutical treatment leads to metabolic problems in many patients who are then referred to endocrinologists.
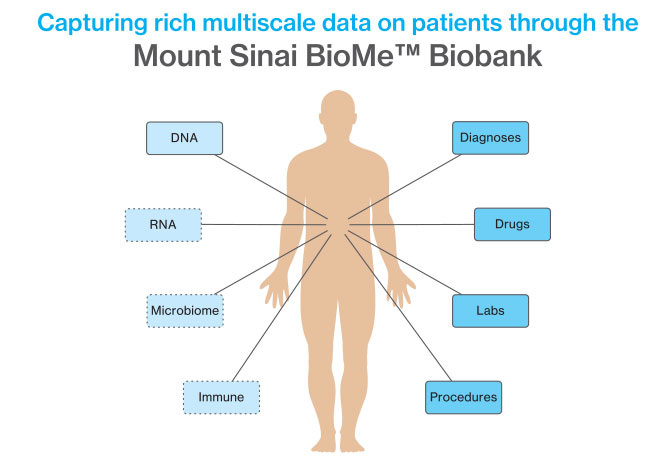
The precision-medicine approach—defined by Dr. Dudley as redefining patient populations and disease through data—has been confined in the past mainly to cancer. But the rapidly growing trove of patient-specific information from electronic-medical-record systems like Mount Sinai’s BioMe™ Biobank is now making it possible to broaden precision medicine to many other complex, multifactorial diseases. “In the case of rheumatoid arthritis, for example, it might tell us that what we’ve always thought of as a single disease is in fact four different diseases, and understanding where patients live on this new map is critical to how they’re treated.”
Indeed, it could result in patients no longer being treated by their disease at all, but by their “coordinates” on a patient population map. “A disease like diabetes doesn’t end in a neat little bordered space and another disease begins,” he says. “These diseases overlap.” And that simple notion, he adds, “could help us reimagine the whole taxonomy of human disease and how it’s treated.”
A Search for Primary Aldosteronism
Screening Is Essential in Resistant Hypertension

A Mount Sinai Hospital study on the prevalence of primary aldosteronism (PA) in an urban hypertensive population found a much lower prevalence of PA than did other studies involving certain at-risk populations. But it confirmed that PA screening is essential for patients with resistant hypertension, defined as taking four or more drugs for hypertension or taking three drugs with hypertension still uncontrolled. Furthermore, although excessive aldosterone can cause low levels of potassium in the blood, the majority of patients in the study had normal potassium levels.
“We wouldn’t recommend screening everybody, but it could have a significant impact on an individual’s medical regimen and life expectancy, and it is an easy, cost-effective screening to do,” says Alice C. Levine, MD, Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at the Icahn School of Medicine at Mount Sinai (ISMMS) and Co-Director of the Adrenal Center at The Mount Sinai Hospital.
The study, published online in August 2016 in the journal Endocrine Practice, was launched in August 2012 and concluded in May 2013. It involved 296 hypertensive patients (BP ≥ 140/90) over the age of 18 who were treated at the primary care clinic at The Mount Sinai Hospital. Participants were considered positive for PA if their aldosterone-to-renin ratio (ARR) was ≥ 20 ng/dL with a plasma aldosterone concentration of ≥ 10 ng/dL and a suppressed plasma renin activity of < 1 ng/ml/hr. Patients with results that suggested PA subsequently underwent an oral salt loading test (OSLT) to confirm the disorder. Dr. Levine, the senior author of the article, says that 14 of the 296 patients participating in the study were positive on initial screening for PA—an overall prevalence of 4.7 percent. Six of the 14 confirmed PA patients underwent confirmatory testing with an OSLT, with two of the six confirmed positive—a prevalence of 0.7 percent. The prevalence of PA in the Mount Sinai study was much lower than in other international studies, in which as many as 22 percent of subjects were found to have PA. But Dr. Levine notes that those studies were conducted in specialty clinics that focused on patients with resistant hypertension. “We were looking at a mixed group of patients with hypertension, some of whom had conditions that were very easily controlled on one or two drugs, and that’s why we had a lower rate,” she says. “It is worth noting that the patients who did screen positive had resistant hypertension.”
Given the prevalence of hypertension nationwide, Dr. Levine says it is important to identify PA if it is an underlying cause, since high aldosterone levels are also associated with increased cardiovascular morbidity and mortality, osteoporosis, and insulin resistance. She says patients who have resistant hypertension should be screened even if they do not have low potassium levels (hypokalemia). “Most recent studies, including ours, demonstrate that only a minority of patients who screen positive for PA have any issues with potassium deficiency in the bloodstream,” Dr. Levine says. “That’s important, because most MDs have been taught to look for PA only in patients with hypokalemia, despite the fact that it is not a necessary component to dictate screening.”
The study was led by Sandi-Jo Galati, MD, who at the time was a second-year endocrine fellow at The Mount Sinai Hospital, with assistance from Khadeen Cheesman, MD, Assistant Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at ISMMS. Dr. Levine anticipates that this study will be followed by collaborations with medical systems worldwide to look for new markers for PA that might be useful in different hypertensive populations and might help to determine the best treatment modalities.
Transgender Care, Under One Roof
A New Endocrinology Subspecialty Emerges
The barriers that transgender men and women confront in society extend to the field of medicine, where they say it can be hard to find physicians, including endocrinologists, who are sensitive to and knowledgeable about their therapeutic needs. Mount Sinai Health System has taken a giant step toward closing that gap with the opening this summer of the Center for Transgender Medicine and Surgery in Manhattan, among the first of its kind in the country and the first in the New York metropolitan area affiliated with a major academic medical center.
The team of 20 professionals providing compassionate and comprehensive health care services to transgender patients includes specialists in endocrinology, behavioral health, plastic surgery, urology, and gynecology. These multidisciplinary skills make the Center uniquely equipped to guide patients in their journeys from initial assessment and screening through hormonal therapy, surgical procedures, and post-transition care.
“We have a lot to offer transgender patients who want access to all the services they need under one roof,” says Tamar Reisman, MD, an endocrinologist at the Center who specializes in transgender hormone therapy and an Assistant Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at the Icahn School of Medicine at Mount Sinai. “We’re a Center where patients can find physicians with deep experience in hormone-replacement therapy as well as world-class surgeons in the field of gender-affirming procedures like vaginoplasties, phalloplasties, and top (chest reconstruction) surgery.”
Even with rising public awareness, this degree of specialization is rare. (One expert in the field called the number of endocrinologists practicing transgender medicine “shockingly small.”) For physicians who might feel intimidated or uncomfortable treating the transgender population, Dr. Reisman points out that transgender medicine abides by the same guidelines as normal endocrine practice: “If you care for cisgender men and women, you already understand the physiology along with the therapeutic options and risks. In the case of a trans woman, for example, you’re trying to suppress the testosterone and elevate the estradiol level to that of a natal female. This requires careful monitoring to ensure that hormone levels are neither too high nor too low— which is the responsibility of endocrinologists regardless of whom they’re treating.”
Providers to the transgender community must also be able to marry therapeutic practice with unwavering sensitivity. The 2011 National Transgender Discrimination Survey reported that 28 percent of respondents from all 50 states had delayed care due to past discrimination, and 19 percent were denied care outright. Fifty percent reported having to instruct their providers about delivering their health care.
“People who come to our Center know they’re entering a welcoming and tolerant environment where they won’t be discriminated against,” emphasizes Dr. Reisman, who is professionally committed to providing care to the LGBT community. “We understand the terminology and know how to approach patients so they feel comfortable.” The Mount Sinai Center for Transgender Medicine and Surgery further excels through its collaborations with international experts in transition surgery. Vaginoplasty surgery, for example, is performed by a team led by Jess Ting, MD, a plastic surgeon at Mount Sinai, in partnership with renowned surgeon Marci Bowers, MD, Professorial Lecturer at the Icahn School of Medicine at Mount Sinai, who is transgender herself. Dr. Ting also works with internationally known specialist Miroslav Djordjevic, MD, PhD, of Belgrade, Serbia, to perform metoidioplasty, a type of female-to-male genital surgery.
The Center provides outpatient care services at Mount Sinai’s Institute for Advanced Medicine at 275 Seventh Avenue, and surgical services at various sites across the Mount Sinai Health System.

A Team Effort on Adrenal Cases
Pooling Expertise to Address Rarely Seen Diseases
The Mount Sinai Adrenal Conference, a unique team effort at The Mount Sinai Hospital, offers physicians access to multidisciplinary expertise and insights on endocrine diseases that are rarely encountered in common-day practice.
“We look at what are generally referred to as orphan diseases, where it is impossible for an individual specialist to know all of the nuances involved in establishing the diagnosis, localizing the problem, and determining treatment,” says Alice C. Levine, MD, Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at the Icahn School of Medicine at Mount Sinai and Co-Director of the Adrenal Center at The Mount Sinai Hospital. “By approaching these cases as a team, we are able to have a more significant impact than we could if we attempted to treat them as individual practitioners.”
Dr. Levine says the Conference, which is usually held on the third Monday of each month, is similar to a tumor board, reviewing cases submitted by doctors in the Mount Sinai Health System and referrals made by specialists in the tristate area. The submissions are reviewed initially by Dr. Levine and the Endocrine Surgery Team, headed by William B. Inabnet III, MD, and Gustavo G. Fernandez-Ranvier, MD, and any cases that cannot be resolved easily are prepared and added to the Conference patient roster. Many of the cases involve pheochromocytomas (rare adrenal gland tumors that cause the release of excessive epinephrine and norepinephrine), the localization of aldosteronism, and mild hypercortisolism.
“Most practicing endocrinologists will see one or two instances of these diseases in their careers,” Dr. Levine says. “We discuss, on average, three pheochromocytomas, aldosteronomas, and adrenocarcinomas at each Conference, and given that sheer volume, we’re able to be smarter not just in how we treat those diseases but also how we sequence that treatment.”
On average, as many as 11 cases may be reviewed in each hour-long session by about 30 specialists, including endocrine surgeons, hypertension specialists, radiologists, nuclear medicine doctors, pathologists, oncologists, and fellows in all of those fields. Each session ends with recommendations for treatment, with followups conducted at the next monthly Conference. There are no specific data demonstrating success rates, but Dr. Levine says the increasing volume of patients being referred for discussion is encouraging. More important, those patients are benefiting from the Conference’s wide-ranging expertise.
“We had one patient in whom a new, small adrenal mass was noted on imaging done as routine monitoring for the patient’s diagnosis of lymphoma. On initial review, the adrenal nodule was thought to be from lymphoma. However, since the patient’s lymphoma was well controlled, with no evidence of disease elsewhere, the team recommended follow-up blood testing and imaging in three months,” Dr. Levine says. “The review at three months demonstrated clear-cut growth of the tumor, again with no evidence elsewhere of worsening lymphoma, so surgical removal was recommended. The final pathology was an adrenal cortical carcinoma, not a lymphoma. That is one example where we have had success by working as a multidisciplinary team.”
Endocrinology and Cancer
Clinic Focuses on Hormonal Effects of Chemotherapy
Emily Gallagher, MD, PhD, could see that something was wrong the moment she met Joan, a 50-year-old undergoing treatment for multiple myeloma at The Mount Sinai Hospital. Joan had been having episodes of heavy sweating and low blood pressure, and she was unable to sit up without dizziness.
“She had a complicated medical history and had been diagnosed with a pulmonary embolism,” says Dr. Gallagher, Director of the OncoEndocrinology Clinic at Mount Sinai. “It was thought her low blood pressure was related to the embolism, but cardiac tests had been conducted, and there was nothing abnormal on the echocardiogram.”
Joan told Dr. Gallagher that she had been taking dexamethasone intermittently for years as part of her treatment for multiple myeloma. Suspecting that Joan might have an adrenal insufficiency as an unintended consequence, Dr. Gallagher started her on steroid hormone replacement, and within 48 hours Joan’s low blood pressure, sweating, and dizziness were resolved.
Launched in April 2015, the OncoEndocrinology Clinic provides endocrinology evaluations, diagnoses, and treatments for patients who have had a cancer diagnosis, or who are undergoing cancer treatments such as chemotherapy. The goal, says Dr. Gallagher, Assistant Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at the Icahn School of Medicine at Mount Sinai, is to prevent cancer treatments from exacerbating conditions like diabetes and causing needless suffering and hospital stays. Dr. Gallagher estimates she sees 20 patients each week.
“I see a lot of patients who have diabetes and are on chemotherapy, in addition to patients who have osteoporosis after being on anti-estrogen therapy for breast cancer,” Dr. Gallagher says. “I also see patients who have adrenal insufficiency after withdrawal of long-term steroid therapy. Recently, I have been seeing a number of patients with endocrine complications of novel immune therapies. I also see cancer survivors with endocrine issues such as bone or metabolic side effects resulting from the cancer treatment.”
The innovative clinic addresses a need that has arisen for at least two reasons: more people are surviving a cancer diagnosis, and new therapies targeting the immune system are causing endocrine problems like diabetes or thyroid and pituitary diseases. The clinic’s approach challenges the prevailing mindset—that if a patient has cancer, all other conditions are of less importance.
Dr. Gallagher is planning a one-day conference on April 7, 2017, at Mount Sinai to raise awareness about the diabetes- and endocrine-related side effects of targeted cancer therapies. She has been in contact with other health systems about setting up similar clinics and has noted a growing realization among oncologists that there is a value to controlling diabetes and recognizing endocrine dysfunction during cancer treatments. Dr. Gallagher is also consulting with the bone marrow transplant team at Mount Sinai about establishing pretransplant care for diabetes or prediabetes, with the goal of eventually making such assessments and treatments the standard for all oncology patients. “If we can prove the concept with bone marrow transplant patients by demonstrating that proactively diagnosing and treating diabetes improves outcomes and reduces hospitalizations and complications, then we can expand it into other types of cancer,” Dr. Gallagher says.
In the case of Joan, Dr. Gallagher says, the adrenal insufficiency caused by her cancer medication was confirmed with a cosyntropin stimulation test. The patient was prescribed replacement hydrocortisone and was doing well, with no recurrence of symptoms.

Endocrinology, Diabetes and Bone Disease
Download the Winter 2017 Specialty Report