Departments of Neurology and Neurosurgery
Mount Sinai faculty and staff utilize the most advanced technologies, including the combination of presurgical information and surgical navigation, 3D simulation, “heads-up” display, and endoscopy.
Departments of Neurology and Neurosurgery
Mount Sinai Health System’s Departments of Neurology and Neurosurgery are dedicated to rapid advances in technology, pioneering research, and multidisciplinary collaboration to set a new standard for team care to dramatically improve the quality of life for Mount Sinai patients with acute and chronic neurological problems.
This specialty report highlights:
- The Neurosurgery Department’s use of 3D simulation and “heads-up” display to address a patient’s complex brainstem tumor
- Promising surgical techniques that extend the intervention time frame for stroke patients
- The use of a responsive neurostimulation device to decrease seizure activity in epilepsy cases
- Recent strides made in finding treatments for progressive multiple sclerosis
- Clinical trials of stem-cell therapy aimed at extending the lives of patients with glioblastomas
Using Virtual Reality Programs to Help Brain Surgeons Remove Deep-Seated Tumor
In July 2015, a 68-year-old woman with a six-month history of difficulty walking and using her hands, as well as progressive weakness in her arms and legs, was admitted to a hospital in the Philippines after a fall. MRI and CT imaging of the brain and spine showed a large tumor (2.8 cm x 2.0 cm x 1.8 cm) located directly in front of the brainstem, occupying more than 90 percent of the canal, causing severe compression of the brainstem and spinal cord, and enveloping the right vertebral artery.
The case was considered by attending surgeons to be essentially inoperable due to the location of the tumor directly in front of the brainstem, which blocked access. In addition, the tumor appeared to surround the vertebral artery, which limited access from a lateral approach. They recommended, and the patient agreed, to seek surgery in the United States.
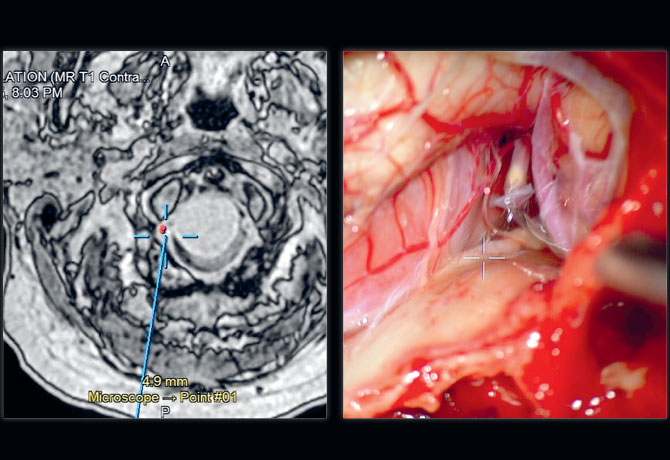
Right: A red dot generated from the microscope marking the location of the vertebral artery.
Shortly after arrival in New York, the patient experienced further worsening of neurological function and was rushed to a major local teaching hospital. With new images of the brain and spinal cord, attending neurosurgeons recommended transfer to yet a third hospital with special expertise in conditions with this level of complexity.
In September, at the request of the family, the patient was transferred to The Mount Sinai Hospital’s Neurosurgery and Neurology ICU. Attending spine neurosurgeon John M. Caridi, MD, Assistant Professor of Neurosurgery, and Orthopaedics, requested a case assessment by Joshua B. Bederson, MD, Professor and Chair of Neurosurgery for the Mount Sinai Health System, an expert in complex brain and spinal tumors, especially those involving the skull base and cerebral vasculature.
Mount Sinai is currently the only site in North America that has the specific combination of integrated neurosurgical tools for preoperative simulation, planning, intraoperative navigation, and microscope integration that were mobilized to help this patient. These include Surgical Theater’s patient-specific 3D simulation platform, coupling intraoperative navigation with 3D virtual reality systems, linked to Brainlab’s newest surgical navigation hardware and software platforms, all integrated into Zeiss’s Pentero® 900 navigation “heads-up” display in the operating room.
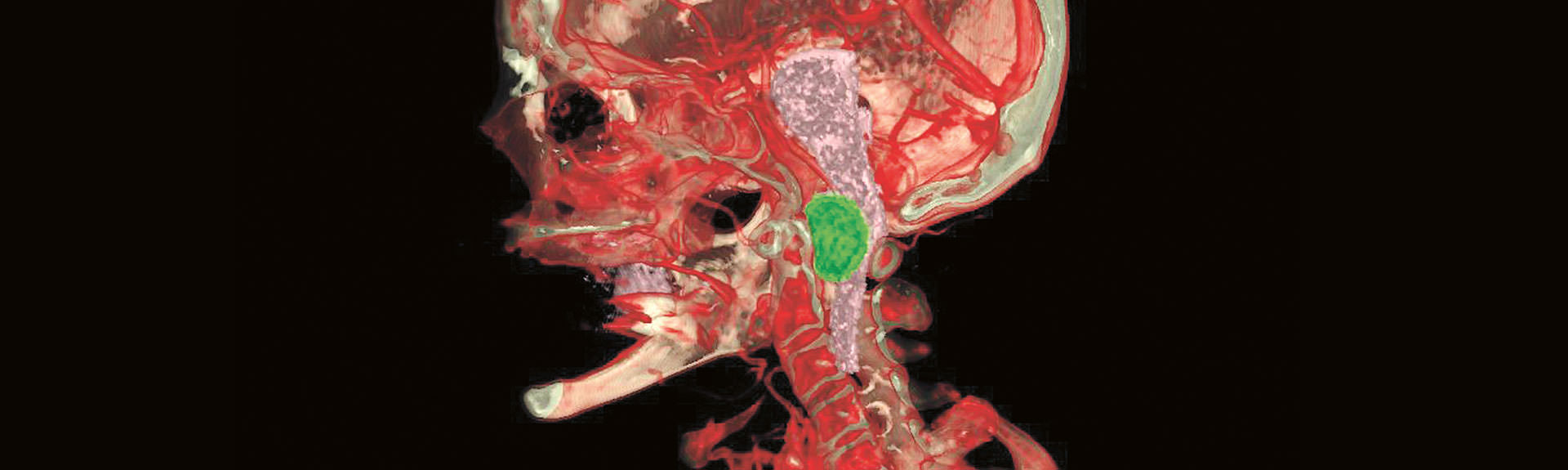
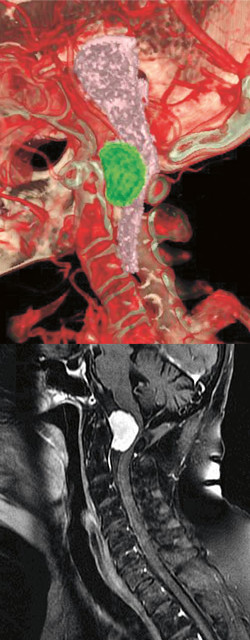 These unique technology platforms provided Dr. Bederson with an interactive 3D visualization of the patient’s craniospinal anatomy generated from MRI and CT imaging, clarifying relationships among critical structures such as the vertebral artery, the tumor, and the skull-base bony structures. Although the vertebral artery was surrounded by tumor, it appeared separable from it, a key factor that was less discernible on standard imaging.
These unique technology platforms provided Dr. Bederson with an interactive 3D visualization of the patient’s craniospinal anatomy generated from MRI and CT imaging, clarifying relationships among critical structures such as the vertebral artery, the tumor, and the skull-base bony structures. Although the vertebral artery was surrounded by tumor, it appeared separable from it, a key factor that was less discernible on standard imaging.
During surgery, the simulations were tied to intraoperative stereotactic frameless navigation and projected into a “heads-up” display within the eyepieces of a Zeiss Pentero 900 neurosurgical microscope. Together, these information modalities provided the surgeon with an “augmented reality” interface that brought enhanced situational awareness throughout the case and contributed to patient safety.
A far-lateral transcondylar suboccipital craniectomy with C1-C2 laminectomy was performed to provide surgical access. The approach was based on the concept of removing bone and mobilizing the vascular structures to permit rotation of the spinal cord and to allow a direct approach to the tumor without undue manipulation of the spinal cord and brainstem. The highly vascular and fibrous tumor was removed using microsurgical techniques and ultrasonic aspiration over a period of several hours.
Postoperative imaging showed gross-total resection of the tumor. The patient was discharged to the acute rehabilitation service for a few days of physical therapy, and then to her home, where she has rapidly regained muscle strength, fine motor coordination, and independent ambulation, and has improved overall function.
Joshua B. Bederson, MD, Professor and Chair of Neurosurgery for the Mount Sinai Health System, owns equity in Surgical Theater, LLC.
Extending Intervention Time Frames for Clot Retrieval with IV tPA Administration and Stenting
A 44-year-old man was treated at a New York City–area hospital with intravenous tPA after the acute onset of dysarthria and a left hemiparesis. His symptoms initially resolved, but during that night he developed a complete left hemiplegia. The patient’s neurologist, a voluntary attending at The Mount Sinai Hospital, contacted the hospital’s stroke team, and arrangements were made to transfer the patient emergently to Mount Sinai’s Neurosurgery and Neurology ICU.
Upon the patient’s arrival at Mount Sinai, a CT scan demonstrated an infarction in the right insular region and thrombus in the right middle cerebral artery (MCA). A CT perfusion scan demonstrated a much larger region of decreased flow in the right hemisphere, indicating that a significant portion of that hemisphere was at risk. CT angiography showed occlusion of the right internal carotid artery in the neck. The patient went directly to the angiography suite where an endovascular neurosurgery team, led by Srinivasan Paramasivam, MD, Assistant Professor of Neurosurgery, performed an angioplasty and stented the carotid artery while administering aspirin, clopidogrel, and abciximab, and then retrieved the clot blocking the MCA. Although treatment with antiplatelet agents is generally withheld for 24 hours after tPA administration, this regimen was required to maintain stent patency. The patient’s hemiparesis resolved gradually, and today he is back at work with only minimal left facial weakness.
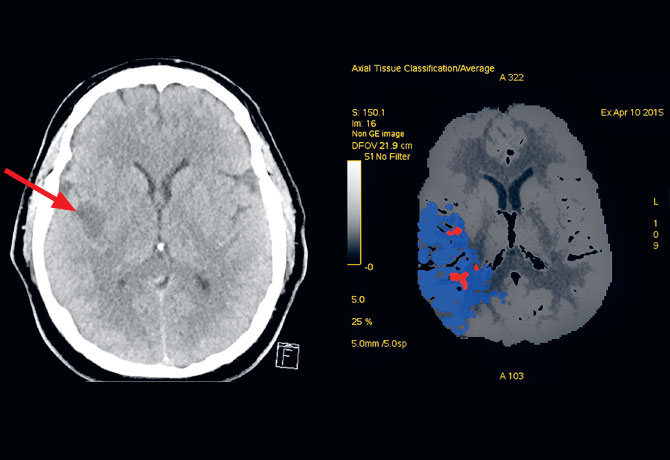
Right: CT Perfusion April 10, 11:01 am, CT perfusion demonstrates a large area of salvageable brain tissue (blue) and small area of established infarct (pink).
Successful outcomes such as this, involving a coordinated team of physicians in Neurosurgery, Neurology, Neurocritical Care, Radiology, and Emergency Medicine, are based on the year-old findings of several studies demonstrating the efficacy of clot retrieval in conjunction with the administration of IV tPA. This case extended the six- to eight-hour time frame suggested by those studies and incorporated the stenting procedure required by the presence of carotid artery occlusion. Much remains to be learned about the limits of acute ischemic stroke interventions. Ongoing national trials led at Mount Sinai by Johanna Fifi, MD; J Mocco, MD, MS; and Stanley Tuhrim, MD, are exploring promising interventions and selection criteria that may extend the time window and improve the success rate for these procedures.
Dr. Fifi is Director of Endovascular Ischemic Stroke and Assistant Professor of Neurology, Neurosurgery, and Radiology; Dr. Mocco is Professor and Vice Chair for Education in the Department of Neurosurgery and Director of the Mount Sinai Health System’s Cerebrovascular Center; and Dr. Tuhrim is Director of the Comprehensive Stroke Center at The Mount Sinai Hospital and Professor and Vice Chair of Clinical Affairs, Department of Neurology.
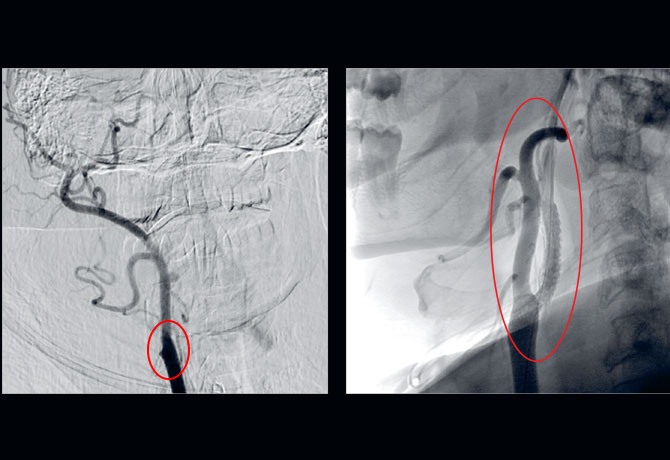
Left: Digital subtraction angiography (DSA) in AP view with injection into the right common carotid artery demonstrates occlusion of the right internal carotid artery (RICA) at its origin (red circle).
Right: DSA in lateral view demonstrates restoration of flow into the RICA after placement of a carotid stent (red circle).
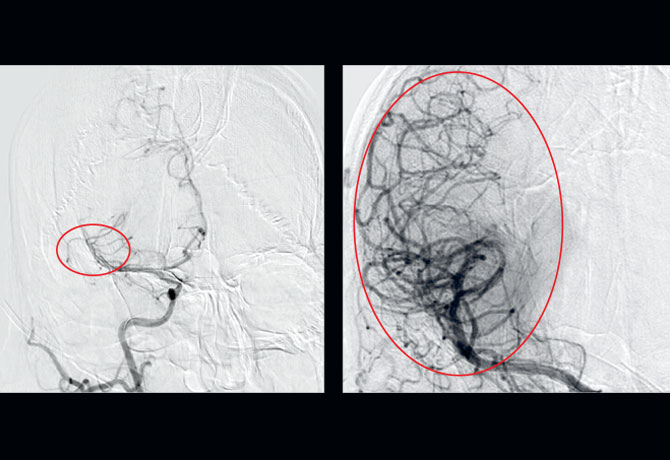
Left: DSA in AP view centered at the head demonstrates a second occlusion of the right middle cerebral artery intracranially (red circle).
Right: DSA in AP view after clot retrieval demonstrates restoration of flow into the middle cerebral artery and its branches (red circle).
Significantly Decreasing Seizure Activity in Youngest Patient to Be Treated With Responsive Neurostimulation Device
Colin is 14 and lives with his family in New Jersey. He was born via normal delivery after a pregnancy complicated by maternal Lyme disease. Development was normal until he developed infantile spasms.
He has tried and failed more than 15 antiepileptic medications, and continued seizures have impacted his development. Colin is unable to walk and has behavioral abnormalities, including episodes of screaming and self-injurious behavior. He is wheelchair-dependent and experiences four to six seizures per day, with his head down and to the left, and with tonic extension of the arms.
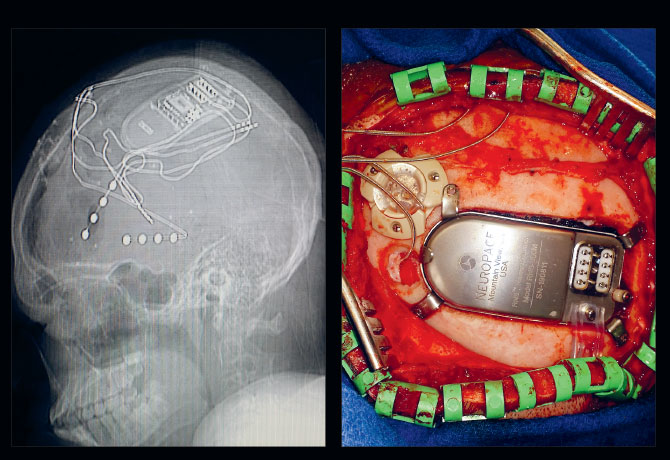
Right: Intraoperative photo of the left side of the skull shows the responsive neurostimulator pulse generator and the leads, including a left frontal strip and left thalamic depth electrode, as well as the two right-sided leads coming from the right thalamus and right temporal lobe.
Colin has undergone five epilepsy surgeries, placement of a vagus nerve stimulator, and placement of a ventriculoperitoneal shunt for hydrocephalus.
His seizures were initially thought to arise from the right frontal lobe, and his first surgery, a right frontal resection, was performed at an out-of-state hospital. He subsequently developed atonic seizures, and a corpus callosotomy was performed at a New York City hospital by Saadi Ghatan, MD, prior to Dr. Ghatan’s move to Mount Sinai. Two years later, Colin underwent an anterior commissurotomy and placement of bilateral strip electrodes at Mount Sinai Beth Israel after the seizures recurred.
After the commissurotomy, it was hoped that there would be clear lateralization of the seizure onset, but, unfortunately, electrographic seizures arose from the right temporal lobe, while clinical seizures arose from the left temporal lobe and occipital lobes. The left temporal lobectomy and occipital disconnect failed to halt the seizure activity, and the family was offered the option for Colin to receive the RNS® System, a responsive neurostimulation device by NeuroPace.
On September 15, 2015, he became the youngest person to be treated with the RNS System. The U.S. Food and Drug Administration had recently approved the device for treatment of refractory complex partial seizures in patients aged 18 and older.
During the surgery, two cortical electrode strips were placed in the right temporal and left frontal lobes, and an additional two electrodes were inserted in the bilateral thalami in anticipation of possible use in the future. The device is programmed every three weeks to detect abnormal epileptiform discharges that may result in a seizure and to stimulate those areas of the brain to prevent the abnormal discharges from resulting in a seizure.
Two months after the procedure, Colin has experienced a significant decrease in seizure activity, from about three to four seizures every morning to only one per morning.
Mount Sinai’s epilepsy team is headed by Steven M. Wolf, MD, Director of Pediatric Epilepsy and of the Comprehensive Pediatric Epilepsy Center, in partnership with co-director Patricia Engel McGoldrick, NP, MPA; and Saadi Ghatan, MD, Chair of Neurosurgery, Mount Sinai West and Mount Sinai St. Luke’s, and Director of Pediatric Neurosurgery at the Mount Sinai Health System. To learn more about the epilepsy program, visit www.nycepilepsyteam.org
A Leading Role in Advancing Research for Progressive Multiple Sclerosis
Treatments for relapsing forms of multiple sclerosis (MS) have been one of this century’s neurotherapeutic triumphs, but to date there has been no approved treatment for progressive MS, the most disabling form of the disease. Finding such treatments remains a priority for investigators around the world and at Mount Sinai, who have made recent strides.
Clinical researchers at Mount Sinai’s Corinne Goldsmith Dickinson Center for Multiple Sclerosis have played a key role in developing a potential breakthrough treatment for progressive MS, and they recently received funding to head an international coalition studying new strategies for treatment development.
The Center was a trial site for the first pivotal Phase 3 study, called ORATORIO, to show efficacy in treating primary progressive MS with a monoclonal antibody, ocrelizumab, produced by Genentech, an affiliate of Roche. Fred D. Lublin, MD, Saunders Family Professor of Neurology and Director of the Corinne Goldsmith Dickinson Center for Multiple Sclerosis, was a member of the steering committee that designed and monitored the study. The study results, presented in October 2015 at the meeting of the European Committee for Treatment and Research in MS in Barcelona, Spain, demonstrated that the molecule significantly reduced the rate of disability accrual in primary progressive MS—a breakthrough, pending regulatory approval, that has the potential to improve the lives of progressive MS patients.
In September 2015, the International Progressive MS Alliance, a consortium of international MS societies dedicated to advancing progressive MS research, awarded its second round of planning grants to collaborative teams of scientists tasked with uncovering and removing the barriers to treatment development. The grants specifically aim to accelerate research progress in three areas: development of preclinical drug candidates; development of meaningful outcomes measures, such as biomarkers, for early clinical integration; and initiation of clinical trials of new interventions.
The Alliance considered 52 applications, involving nearly 500 worldwide investigators, for its 12-month Collaborative Network Planning Awards before selecting the 11 projects. Mount Sinai’s Corinne Goldsmith Dickinson Center
for Multiple Sclerosis, with Dr. Lublin as principal investigator, was funded to assemble a coalition of international MS centers to develop a strategy for diagnosing progressive MS earlier, allowing for more effective therapeutic options. Currently, it takes years to confirm onset of progressive MS.
The multiple sclerosis center at Brigham and Women’s Hospital in Boston, as well as other multiple sclerosis centers in Barcelona, Spain; Rennes, France; and Perth, Australia, are part of the new consortium. Together, these sites will pool their large multiple sclerosis datasets to test potential clinical, MRI, and biomarker predictors of onset of progressive disease.
Ocrelizumab Meets Primary Endpoint for Progressive MS
The ORATORIO study met its primary endpoint, showing treatment with ocrelizumab significantly reduced the risk of progression of clinical disability sustained for at least 12 weeks by 24 percent compared with placebo, as measured by the Expanded Disability Status Scale (EDSS) (p = 0.0321).
Additionally, ocrelizumab was superior to placebo in:
- Significantly reducing the risk of progression of clinical disability for at least 24 weeks by 25 percent (p = 0.0365), and the time required to walk 25 feet (Timed 25-Foot Walk, or T25-FW) over 120 weeks by 29 percent (p = 0.0404).
- Decreasing the volume of hyperintense T2 lesions by 3.4 percent over 120 weeks compared to placebo, which increased T2 volume by 7.4 percent (p < 0.0001).
- Reducing the rate of whole brain volume loss over 120 weeks by 17.5 percent compared to placebo (p = 0.0206).
Manipulating Patients’ Stem Cells to Go After Glioblastomas
As a surgeon skilled in removing tumors from what others would consider inoperable parts of the brain, Isabelle Germano, MD, Professor of Neurosurgery, Neurology, and Oncological Sciences at the Icahn School of Medicine at Mount Sinai and Director of the Comprehensive Brain Tumor Program, is well aware of the grim prognosis her patients face. “Fifty percent or more of patients with glioblastoma will be dead within 11 months,” she says.
Dr. Germano has taken her expertise—and concern—into the laboratory, and by the end of 2016 expects to start clinical trials with an innovative stem-cell therapy she has developed, which, if proven successful, could prolong the lives of people with glioblastoma by several years. Just as important, it could have applicability across a range of neurodegenerative disorders, the most significant one being Alzheimer’s disease.
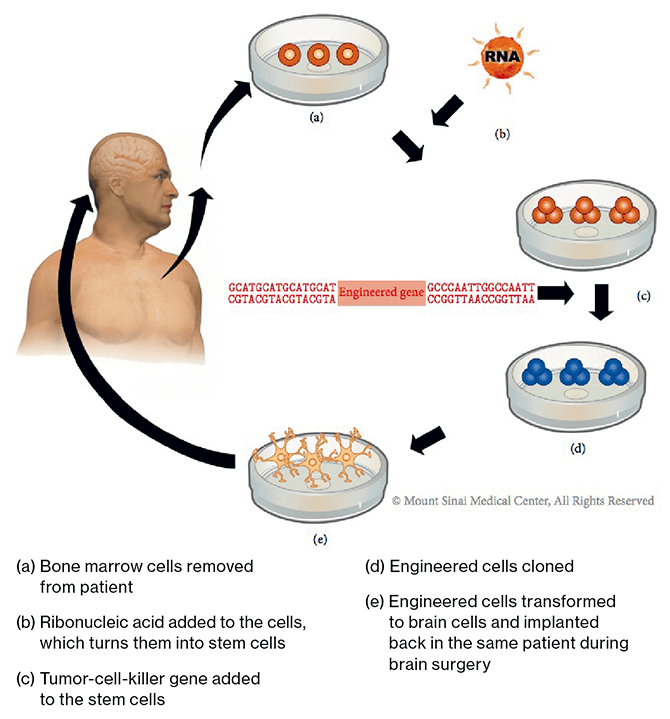
This first-of-its-kind technique involves manipulating the patient’s own stem cells, thereby avoiding potential ethical as well as immunological issues. Skin cells are drawn from the arm or elsewhere and turned into induced pluripotent stem cells (iPSCs)—adult cells that are genetically reprogrammed to replicate embryonic stem cells. These autologous cells are then engineered to express a tumor-cell-killer gene (or Alzheimer’s-fighting gene), cloned, and differentiated into fully formed brain cells (astrocytes). When the tumor recurs, which in the case of glioblastomas is 95 percent of the time, a second surgery is performed and these manipulated stem cells are implanted in the brain, destroying tumor cells only.
While noting that patient-specific iPSCs are “formidable tools for cell-based therapy and drug discovery,” Dr. Germano acknowledges the major challenges that their development posed for researchers. These hurdles included the need to develop iPSCs without the oncogenic genes that were originally used in their reprogramming, so that patients would not be exposed to cancerous genes. Dr. Germano describes this development as a breakthrough for her team. Another technical challenge—insertion of the killer genes into the patients’ stem cells—still remains, although the team is making progress. Dr. Germano is confident that all outstanding issues can be resolved over the next 12 months, clearing the way for clinical trials in humans to begin soon after.
“The future for treating brain tumors and many other neurological diseases is to exploit the strength within our bodies, making the cells ‘smarter’ so they can go back and fight the disease,” she asserts. “In this way we believe we can make a difference, particularly for patients with brain tumors where two or three additional years of life are considered significant.”
Mining a Robust Pipeline
In keeping with its mission to ensure that its discoveries and innovations are translated into health care products and services, Mount Sinai has produced cutting-edge work in a wide range of laboratories. These advances include:
- The discovery of novel small molecules for treating lysosomal storage diseases (LSDs), a group of conditions caused by the most common genetic disorder in humans. In preclinical trials, these compounds have been shown to reverse the toxic lipid buildup in patient cells, which can severely damage tissue and organs.
- Development of a family of noninvasive assays to monitor kidney function both before and after transplantation to predict the likelihood of fibrosis and graft loss in transplant recipients. These unique assays, under the name FractalDx, will be a significant advance over current methods of monitoring transplanted kidneys for failure.
- A first-in-class small molecule that could bring new hope to individuals with the most severe cases of heart failure. The compound activates a protein known as SUMO1, which, in turn, stimulates the activity of SERCA2a, another protein responsible for the pumping action of the heart muscle.
Message from the Chairs: Joshua B. Bederson, MD, and Barbara G. Vickrey, MD, MPH
Digital medicine, rapid advances in technology, pioneering research, and multidisciplinary collaboration that sets a new standard for team care are saving lives and dramatically improving quality of life for Mount Sinai patients with acute and chronic neurological problems.
Mount Sinai faculty and staff utilize the most advanced technologies, including the combination of presurgical information and surgical navigation, 3D simulation, “heads-up” display, and endoscopy. Our expertise in applying these technologies is integrated across Neurology and Neurosurgery, and today we are able to achieve a high quality of technical care—and often extraordinary outcomes—for patients requiring neurosurgical interventions, as in the case we share of a 68-year-old woman with a large, complex brainstem tumor.
We are also pioneering surgical techniques for endovascular treatment of stroke and have been leading the conversation internationally to generate the evidence needed to establish its benefit. For individuals who have a major stroke with a blockage of a large brain artery, there are now clear indications that this time-sensitive therapy can significantly improve the likelihood of recovery, as in the case of a 44-year-old man profiled in this Report.
Still, achieving the highest patient outcomes requires team care that focuses on identifying the information and support needs of patients and their families, and integrating that knowledge with expert medical management from subspecialists and seamless communication with referring providers. Barbara G. Vickrey, MD, MPH, newly named Chair of Neurology and the Henry P. and Georgette Goldschmidt Professor of Neurology, has pioneered research to develop reliable and valid measures of patients’ and caregivers’ health-related quality of life, and to build and test the impact of re-engineered, coordinated team care delivery models for dementia, Parkinson’s disease, and stroke prevention. Central to these models is ensuring access to high-quality technical care and optimizing the patients’ and family members’ experience of care, as well as building their knowledge and self-management skills.
We invite you to read about some of our recent achievements in this Report.
Departments of Neurology and Neurosurgery
Download the Winter 2016 Specialty Report