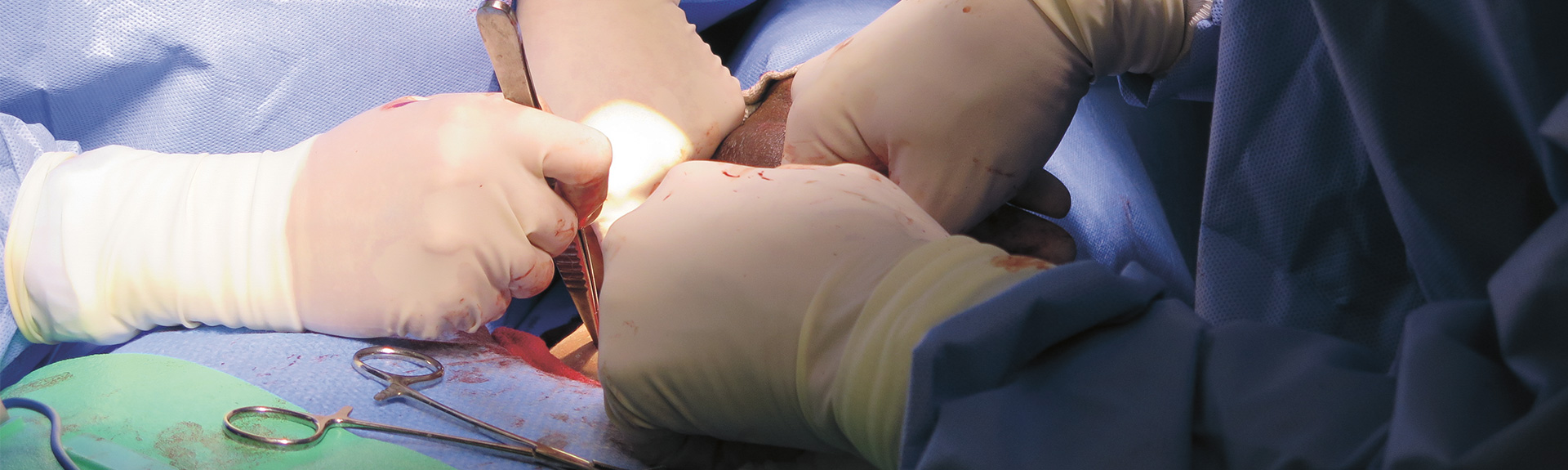
ENT/Head and Neck Surgery Specialty Report
We are committed to our patients, faculty, and referring physicians to shape the landscape of otolaryngology for an even greater future.
ENT / Head and Neck Surgery
Mount Sinai Health System’s Department of Otolaryngology–Head and Neck Surgery is internationally recognized for conservation laryngeal surgery, head and neck reconstruction, and accomplishments in the diagnosis and management of HPV-associated disease and robotic head and neck surgery. This specialty report highlights:
- Successful treatment of a rare and complicated case of adenoid cystic carcinoma.
- The Division of Sleep Surgery’s FDA-approved Inspire™ therapy implant device for obstructive sleep apnea patients
- The pioneering, noninvasive CT/MRI fusion diagnostic technique for cerebrospinal fluid leaks developed by the Division of Rhinology and Skull Base Surgery
- The Division of Facial Plastic and Reconstructive Surgery’s surgical approach of cranial nerve 5 and 7 transfer for facial paralysis
An 11-Hour Operation Successfully Treats “Untreatable” Cancer
Susan Chandler’s salivary cancer journey began in 2005 when she went to the doctor for an earache. After several tests, a lump was discovered under her jaw. Six days after surgery to remove the mass, the pathology revealed that she had adenoid cystic carcinoma—a very rare salivary gland cancer.

After a second operation, it was discovered that her cancer had spread. She next had radiation and chemotherapy concurrently, and was deemed “cancer free” for the next 15 months. Two more surgeries followed in 2007 and 2008. Ms. Chandler continued to see her surgeon and medical oncologist in Florida, where she lives. In fall 2009, several nodules were found in her lungs, so she underwent two additional surgeries in 2009 and 2010 to remove them. In spring 2010, Ms. Chandler’s surgeon told her that the next surgery would leave her “horribly disfigured.” As a flight attendant, she knew that this would end the career that she loved.
In fall 2009, several nodules were found in her lungs, so she underwent two additional surgeries in 2009 and 2010 to remove them. In spring 2010, Ms. Chandler’s surgeon told her that the next surgery would leave her “horribly disfigured.” As a flight attendant, she knew that this would end the career that she loved.
She continued surveillance with CT scans and PET scans, and eventually she was selected to participate in a chemotherapy drug trial. Twenty months later, when it was found that the drug hadn’t worked, she was taken off the trial. She was devastated.
Referred from Florida to Mount Sinai
In the summer of 2014, Ms. Chandler and her husband sought a second opinion. Her oncologist in Tampa referred them to The Mount Sinai Hospital to see Marshall Posner, MD, Director of Head and Neck Medical Oncology, who concluded that chemotherapy would not work for her. Dr. Posner introduced them to Eric Genden, MD, Dr. Isidore Friesner Chair of Otolaryngology at Mount Sinai, who is widely recognized for his head and neck cancer and microvascular reconstruction expertise. “He told us that my jaw was being held together by a large tumor in the bone. He said that he wanted to do surgery right away,” Ms. Chandler says.
Dr. Genden describes the case as unusually complicated, but he was able to assure Ms. Chandler that she would not be permanently disfigured.
“Deemed ‘untreatable,’ Susan Chandler presented to Mount Sinai with an advanced salivary gland cancer that had invaded through her mouth and jaw and left this professional flight attendant with unrelenting pain and an open wound,” Dr. Genden says. “Because of her history of prior surgery and radiotherapy, her case was exceptionally complex. Removing the tumor could leave her with a defect of the tongue, jaw, and external skin, with an opening between the mouth and the external skin. Her prior radiotherapy meant that tissue healing was compromised.”
After performing an 11-hour surgery to remove the tumor, surgeons at Mount Sinai used skin and bone from Ms. Chandler’s shoulder blade to reconstruct her tongue, jaw, and cheek. She is now living a normal life, disease free.
Ms. Chandler calls the surgery a miracle. “There will be one more surgery to perfect my jaw, but already my family and friends are amazed. I look like I did before!” she says. “Thank you, Dr. Posner and Dr. Genden, for giving me my life back so I can live to see my family grow!”
New Device Offers Alternative For Obstructive Sleep Apnea
Obstructive sleep apnea (OSA) affects more than 18 million Americans. It is characterized by breathing pauses, ranging from 5 to 30 times or more per hour, during a single night of sleep. These frequent interruptions can lead to morning headaches, reduced attention spans, excessive daytime sleepiness, and even depression.
More alarming, untreated OSA is associated with cardiovascular and metabolic disorders, such as hypertension, stroke, and diabetes, as well as dementia and cancer.
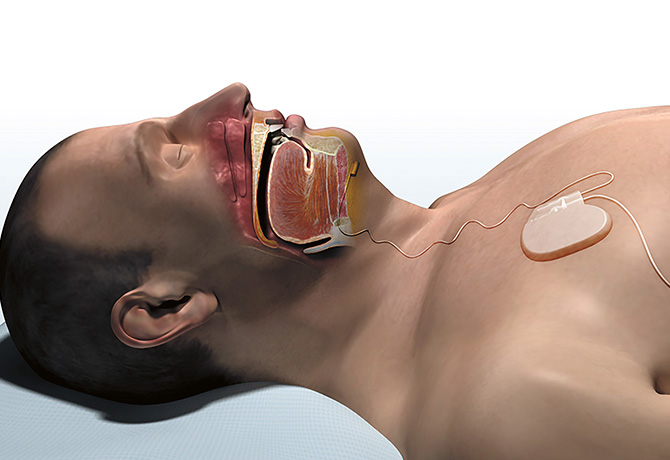
Patients diagnosed with OSA are usually prescribed continuous positive airway pressure (CPAP) machines; however, studies have shown that up to 50 percent of OSA patients do not adhere to this treatment. For these patients, The Mount Sinai Hospital and Mount Sinai Beth Israel are among the first New York City hospitals to offer Inspire™ therapy—an implantable device, placed under the skin of the upper right chest, that connects an electrode to the tongue nerve.
“The Inspire implant is a revolutionary therapy, because it stimulates the base of the tongue, offering a wider airway for patients’ intake of oxygen when they would otherwise obstruct,” says Boris Chernobilsky, MD, Director of Sleep Surgery at Mount Sinai Beth Israel. “It’s also unique in that it is implanted, so patients no longer need to apply masks that cover the nose and mouth at night. Patients struggling with CPAP now have an exciting new therapeutic choice.”
Inspire therapy, approved by the U.S. Food and Drug Administration in 2014, comprises three implantable components: a small programmable pulse generator, a breathing sensor lead, and a stimulator lead. Patients have full control of this device by using a remote control; they simply turn it on at night before bed and then off after awakening in the morning.
Implantation and Follow-up Care
Implantation of the Inspire system is conducted in the operating room under general anesthesia. The outpatient procedure takes about two to three hours. A physician makes three small incisions for the two leads and pulse generator: one on the neck under the jaw, one on the upper right chest, and one in the mid-thorax. Patients experience some swelling but are able to return home within one day of the procedure. Once the incisions have healed, patients return for device activation and to learn how to operate the remote. After a few weeks, they undergo a titration study at the sleep lab to optimize the device settings. Finally, patients return once a year for simple device checks.
Results of the STAR (Stimulation Therapy for Apnea Reduction) trial, published in The New England Journal of Medicine in January 2014, demonstrated that Inspire therapy could significantly reduce sleep apnea events and improve quality-of-life measures. Specifically, there was a 68 percent mean reduction in sleep apnea episodes, and 85 percent of bed partners reported little or no snoring.
Innovative Surgical Approach for Bell’s Palsy: Transferring Cranial Nerves 5 and 7
Bell’s palsy affects about 40,000 Americans each year and can result in long-term eye closure and smiling challenges. For decades, physicians have been able to compensate for eye closure issues with several treatment options; however, the loss of the ability to smile has remained a devastating problem for many patients.
Highly specialized surgeons have recently embraced a new surgical approach to restore a natural smile. Joshua Rosenberg, MD, and Grigoriy Mashkevich, MD, of the Division of Facial Plastic and Reconstructive Surgery at The Mount Sinai Hospital and New York Eye and Ear Infirmary of Mount Sinai, are among the few using this innovative technique. The procedure, called cranial nerve 5 and 7 transfer, helps to ameliorate the disfiguring effects of severe Bell’s palsy and, to a lesser extent, certain head and neck cancers. It involves rerouting the robust masseter nerve—which activates the chewing muscles—to power the facial nerves and restore facial-muscle function, specifically of the muscles involved in smiling.
The surgery is typically performed on an outpatient basis. The approach is similar to a facelift in that the incision is hidden in the hairline by the front of the ear. Small branches of the facial nerve (cranial nerve 7) that stimulate the smile muscles and the nerve that stimulates a muscle involved in closing the jaw (the masseteric branch of cranial nerve 5) are then sewn together. The new nerve connections heal over time, and regeneration occurs over a period of 6 to 12 months, restoring the patient’s ability to smile, eat, and speak.
“Smiling is a universal form of human communication, and it affects our emotional state,” says Dr. Rosenberg. “When patients lose this ability, they lose a basic human function and find it harder to feel engaged with others. This novel facial-nerve procedure can transform the lives of patients who previously suffered the social and professional effects of the loss of smile due to Bell’s palsy. It has given patients new opportunities at work and in relationships that otherwise might not have been obtainable.”
Dr. Rosenberg says that due to the limited number of surgeons who perform this procedure, patients have been coming to Mount Sinai from across the Northeast.
Rachel Lewis, a special-education teacher from Chester County, Pennsylvania, who lost the use of the left side of her face to Bell’s palsy three years ago, experienced improvement after her surgery at The Mount Sinai Hospital in December 2014. “This surgery has given me a sense of hope—something I haven’t felt in years. I always come to office visits with a long list of questions, which Dr. Rosenberg answers thoroughly.”
Novel Diagnostic Technique for Cerebrospinal Fluid Leaks
Mount Sinai is at the forefront of minimally invasive treatment of cerebrospinal fluid leaks (CSF) that originate from the nose. Our multidisciplinary approach and expertise in managing these leaks have produced a very high success rate in treating this condition, with minimal complications.
CSF leaks classically present as watery drainage from the nose, typically on one side. Drainage tends to increase during bending over or straining. Some patients may present with unexplained meningitis or headache when sitting upright.
The first step in making the diagnosis is to collect a small sample of fluid and test it in the lab for beta-2 transferrin— a substance present only in cerebrospinal fluid or the vitreous humor of the eye. Once the fluid is confirmed to be cerebrospinal, the next step is to locate the site of the leak. In some cases, a CSF leak in the nose may originate in the ear through the eustachian tube.
Localization of a CSF leak is conducted through imaging studies, such as CT scan or MRI. In the past, the diagnostic technique required placing a needle in the patient’s back, where a contrast agent was injected into the subarachnoid space and then imaged to determine the site of the leak. This procedure can be difficult for obese patients, who tend to manifest spontaneous CSF leaks, because of their anatomy and the pain of needle insertion in the back.
However, at Mount Sinai’s Skull Base Surgery Center, our physicians have pioneered and perform a novel technique in which they superimpose the CT and MRI scans to find the site of the leak. Working with Bradley Delman, MD, in the Department of Radiology and the Department of Neurosurgery, Satish Govindaraj, MD, has forged a novel high-resolution CT/MRI fusion technique that enables them to identify the site of the CSF leak and any other potential leakage sites. At Mount Sinai, this technique has averted the need for traditional, more invasive localization studies, which often cause patients exceptional discomfort and pain. Among hospitals in the New York City region, only The Mount Sinai Hospital offers this technique.
Treatment of CSF Leaks
The treatment of CSF leaks requires surgical closure of the communication between the brain and nasal cavity. At Mount Sinai, all patients with CSF leaks receive full consultations. Because Mount Sinai is a multidisciplinary center specializing in the treatment of skull base pathology, we can arrange consultations with neurosurgeons and at times neuro-ophthalmologists as needed. Imaging studies are coordinated and at times can be arranged prior to the consultation with our Center. The optimal treatment for CSF leaks is endoscopic surgical CSF leak closure, which has a 97 percent success rate and a complication rate of less than 1 percent. We perform a two-surgeon, minimally invasive technique that avoids the need for facial incisions. Tissue from within the nose is used to seal the defect, and the sinuses adjacent to the area are opened to avoid future problems with chronic sinusitis. Patients are discharged home in one to two days and are followed closely in the physician’s office to ensure that their nasal cavities heal well.
Sinai Robotic Surgery Trial in HPV-Positive Oropharyngeal Cancer
Patients with human papilloma virus-positive oropharyngeal squamous cell carcinoma (HPV-OSCC) are generally curable, young, and will live for many years. However, they are at high risk for long-term toxicity and mortality from their therapy.
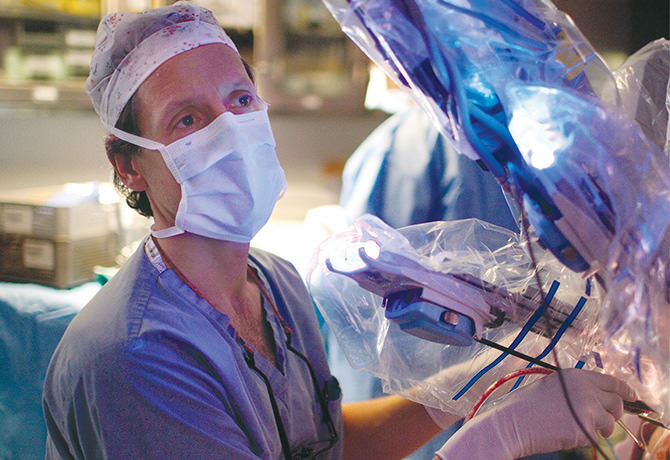
High-dose radiotherapy and chemoradiotherapy substantially affect the local tissues and organ function and result in a significant rate of late mortality and morbidity in patients. Currently, there are few trials examining the role of de-escalation using surgery alone in intermediate and early T-stage HPV-related disease. New surgical techniques have increased the numbers of patients who undergo complete resection, and functional outcomes in such patients are outstanding. Current studies such as the ECOG-E3311 and the Sinai Robotic Surgery Trial aim to evaluate the oncologic efficacy and functional morbidity when TransOral Robotic Surgery is employed to stratify patients for appropriate adjutant therapy.
Patients with intermediate-stage HPV-positive oropharyngeal cancer will be screened for prognostic features and undergo robotic surgery. Patients in whom pathology demonstrates good prognostic features will then be followed without postoperative radiotherapy. Patients with poor prognostic features, such as extranodal extension, perineural invasion, and lymphovascular invasion, will receive reduced-dose radiotherapy or chemoradiotherapy based on their pathologies. It is expected that surgery will produce a cure in more than 50 percent of patients treated, that 25 to 30 percent will avoid radiation therapy entirely, and that the long-term survival of patients with good prognoses will not be changed by withholding postsurgical radiation therapy.
The sensitivity of HPV-OSCC to chemotherapy and radiotherapy suggests that delayed or rescue-therapy treatment in early-stage patients could be highly effective and result in similar survival outcomes, and that radiotherapy could be applied to a much smaller population than current standards prescribe. Moreover, the need for postoperative radiotherapy in this younger, HPV-positive, and highly functional population has not been validated in clinical trials to date. The Sinai Robotic Surgery Trial and similar trials, such as the ECOG-E3311, are being conducted specifically to answer these questions about the role of robotic surgery and pathologic staging for HPV-related oropharyngeal cancer.
A Rich Pipeline Offers Great Promise Against an Array of Diseases
Cutting-edge research by Mount Sinai Health System physician-scientists in a wide range of fields is helping the Health System uncover bold new therapies to meet the urgent needs of patients and society.
The Health System, one of the largest in the nation, includes the Icahn School of Medicine at Mount Sinai, with 34 departments and more than 23 multidisciplinary institutes that are designed to facilitate breakthrough science. Scientists and researchers benefit not only from extensive resources and talent inside the laboratory but also from the expertise of Mount Sinai Innovation Partners, a group that works across the entire system to attract critical funding and shape the newly developed technologies for application and commercialization.
 In the field of lysosomal storage diseases (LSDs), for example, the development of small molecules—shown effective in early trials to reverse the toxic buildup of lipids in patients’ cells—holds promise for a new treatment paradigm for these disorders. Collectively, LSDs comprise the most common genetic disorder in humans. Although enzyme replacement therapy has been the standard of care for some LSDs, the inability of proteins to cross the blood-brain barrier renders this approach ineffective for about 90 percent of the 60 known lysosomal storage disorders.
In the field of lysosomal storage diseases (LSDs), for example, the development of small molecules—shown effective in early trials to reverse the toxic buildup of lipids in patients’ cells—holds promise for a new treatment paradigm for these disorders. Collectively, LSDs comprise the most common genetic disorder in humans. Although enzyme replacement therapy has been the standard of care for some LSDs, the inability of proteins to cross the blood-brain barrier renders this approach ineffective for about 90 percent of the 60 known lysosomal storage disorders.
Yiannis Ioannou, PhD, Professor of Genetics and Genomic Sciences at the Icahn School of Medicine at Mount Sinai, has developed a series of small molecules that can penetrate the blood-brain barrier and correct lipid-metabolism dysfunction in patient cells for at least eight LSDs. “We’re very excited by the results of animal studies for Fabry disease, and by an 85 percent decline in cholesterol accumulation for Niemann-Pick Type C,” two types of LSDs, he notes.
In kidney-transplant patients, physicians currently use measures of creatinine in the blood to monitor the transplanted organ’s status. But this method has a critical flaw: by the time increased levels of creatinine are detected, fibrosis has already developed and the kidney has been irreversibly damaged. Indeed, chronic fibrosis is the primary reason that 17 percent of kidney transplants fail by the third year, and fewer than half still function by the tenth year.
Barbara Murphy, MD, the Murray M. Rosenberg Professor of Medicine, System Chair of the Department of Medicine, and Dean for Clinical Integration and Population Health, is developing a portfolio of assays to monitor kidney function before and after transplantation. These noninvasive assessments, known as FractalDx assays, identify genetic signatures from simple blood tests to predict the likelihood that transplant recipients will develop fibrosis and graft loss. “Instead of being reactive and limiting the damage,” Dr. Murphy explains, “we’re developing a monitoring tool that can identify problems before damage occurs.”
Brain tumors, among the most aggressive cancers, consign roughly half of patients to an average life expectancy of 11 months following surgery. By the end of 2016, Isabelle Germano, MD, Director of the Comprehensive Brain Tumor Program and Professor of Neurosurgery, Neurology, and Oncological Sciences, expects to start clinical trials on a breakthrough stem-cell therapy she has developed, which, if proven successful, could prolong the lives of people with glioblastoma by several years. The approach delivers to the disease site autologous stem cells engineered to express a tumor-cell-killer gene that is activated once the tumor returns, which is 95 percent of the time.
Although some technical issues in cell manipulation remain, lab results have validated Dr. Germano’s work with induced pluripotent stem cells. “The future for treating brain tumors is in making the body’s own cells ‘smarter’ so they can fight the disease,” she says.
Message from the Chair
It gives me great pleasure to present an overview of the impressive achievements and innovative advances of the Mount Sinai Health System’s Department of Otolaryngology–Head and Neck Surgery. The Department is internationally recognized for conservation laryngeal surgery, head and neck reconstruction, and accomplishments in the diagnosis and management of HPV-associated disease and robotic head and neck surgery.

In 2015, the Department launched a Same-Day Appointment Program—the first of its kind on the East Coast. Additionally, the Division of Sleep Surgery introduced the FDA-approved Inspire™ therapy implant device for obstructive sleep apnea patients struggling with the use of CPAP machines. The Division of Rhinology and Skull Base Surgery pioneered a CT/MRI fusion diagnostic technique for cerebrospinal fluid leaks, which supplants invasive alternatives. And the Division of Facial Plastic and Reconstructive Surgery adopted the surgical approach of cranial nerve 5 and 7 transfer for facial paralysis.
Our institutional tradition of excellence in clinical care, education, and research is alive and evident in all of our efforts—some of which keep us up at night and others that allow us to deliver our patients back to their referring doctors earlier than expected. We are committed to our patients, faculty, and referring physicians to shape the landscape of otolaryngology for an even greater future
Department of Otolaryngology Head and Neck Surgery
Download the Winter 2016 Specialty Report