Hilda & J. Lester Gabrilove Division of Endocrinology, Diabetes & Bone Disease
Research under way at the Icahn School of Medicine at Mount Sinai has the potential to revolutionize the management of type 1 diabetes (T1D), freeing patients from repeatedly testing their sugar with finger sticks and having to adjust their insulin regimens.
Hilda & J. Lester Gabrilove Division of Endocrinology, Diabetes & Bone Disease
This report highlights the work of Mount Sinai physicians and scientists in the following areas:
- New approaches in adrenal care
- Artificial pancreas research that may revolutionize the management of type 1 diabetes
- Two rare cases of insulinoma, seen by the same physician in just one year
- How our clinicians discovered an undiagnosed case of acromegaly in a patient initially seeking bariatric surgery
Mount Sinai Advances Artificial Pancreas Research
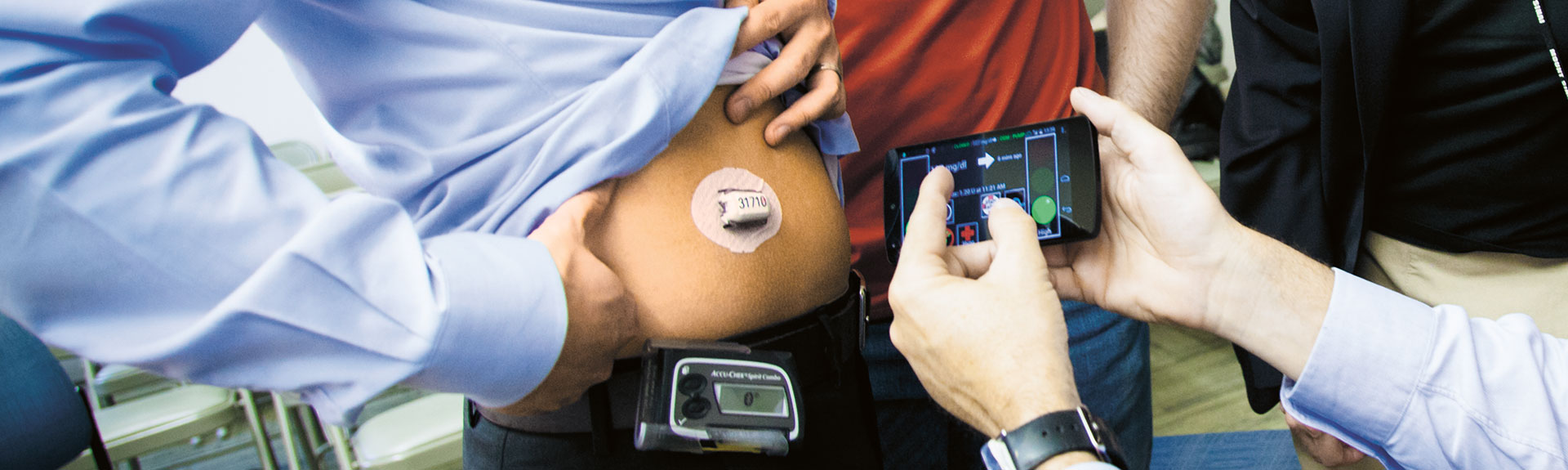
Research under way at the Icahn School of Medicine at Mount Sinai (ISMMS) has the potential to revolutionize the management of type 1 diabetes (T1D), freeing patients from repeatedly testing their sugar with finger sticks and having to adjust their insulin regimens.
The clinical research study, funded by JDRF, is the first outpatient study of artificial pancreas (AP) systems in New York State. A joint effort among ISMMS, the University of Virginia (UVA), and the Mayo Clinic, the study followed 10 patients with T1D for five days, during which the UVA-developed AP system provided them with continuous glucose monitoring and insulin pump therapy at night. The AP system runs a software algorithm on a smartphone that communicates with a standard insulin pump and glucose sensor to maintain each participant’s sugar levels within a designated range to avert nighttime hypoglycemia and ensure a goal glucose level in the morning.
“The goal is for people with type 1 diabetes using the AP system to show superior glucose control, reduced hypoglycemia overnight, and overall reduced risk of sugar imbalances for significantly longer periods, compared with standard therapy,” says Carol Levy, MD, Associate Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at ISMMS and lead investigator of the study.
“The five-night study showed that patients achieved stable glucose levels between 80 and 140 mg/dl during the night, and that the AP system led to improved blood-sugar control throughout the next day as well.”
Dr. Levy, who has T1D herself, believes that, if approved by the U.S. Food and Drug Administration, the AP system is likely to be used widely because it is user-friendly and regulates only a single hormone: insulin. Other, more complex systems currently in development may take longer to implement.
The study is part of a larger artificial pancreas research program at Mount Sinai. Collaborations have taken place with many institutions in addition to UVA and the Mayo Clinic, including Rensselaer Polytechnic Institute, Stanford University, and the Barbara Davis Center for Childhood Diabetes at the University of Colorado, Denver.
In December 2015, Dr. Levy and her team received notification of NIH funding for a nine-center international multisite study in which the Icahn School of Medicine will be one of the primary sites. In these studies, subjects will bring the AP system home with them while researchers monitor the system remotely.
New Approaches to Care In the Adrenal Center
The Adrenal Center at Mount Sinai, under the co-directorship of William B. Inabnet III, MD, Chair of Surgery at Mount Sinai Beth Israel and the Eugene W. Friedman Professor of Surgical Oncology at the Icahn School of Medicine at Mount Sinai, and Alice C. Levine, MD, Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at the Icahn School of Medicine, has become one of the leading programs for adrenal referrals on the East Coast in only five years. Here are updates from the Center:
360-Degree Treatment of Pheos
The results of an international retreat of 15 experts held at Mount Sinai to improve the diagnosis and management of pheochromocytomas (pheos) were published in the November 2014 issue of Endocrine Practice. This was the first publication aimed at developing a comprehensive clinical pathway for the management of pheos. The outcome of the retreat was a consensus for the diagnosis, perioperative management, and postoperative management of pheos, with specific recommendations from our team of adrenal experts, which includes adrenal surgeons, endocrinologists, nuclear medicine doctors, radiologists, clinical laboratory experts, anesthesiologists, oncologists, and genetics counselors. Our clinical pathway model can be applied by other institutions, with many medical centers already expressing interest in using it.
Using Mifepristone in a New Way
A poster presented at the Endocrine Society annual meeting in San Diego in March 2015 showed that the drug mifepristone, which blocks the action of the hormone cortisol, produces positive effects on glucose parameters and insulin sensitivity as well as beneficial effects on depression scores and quality of life in patients with mild overproduction of cortisol due to adrenal incidentalomas. This was the first time the drug had been studied in patients with this type of adrenal tumor.
Top Recruits
This year we welcomed two impressive fellowship-trained endocrine surgeons to the Adrenal Center:
- Gustavo Fernandez-Ranvier, MD, Assistant Professor of Surgery (Metabolic, Endocrine, and Minimally Invasive) at the Icahn School of Medicine at Mount Sinai
- Hyunsuk Suh, MD, Assistant Professor of Surgery at the Icahn School of Medicine at Mount Sinai
Newly Published
Alice C. Levine, MD, Co-Director of the Adrenal Center, was editor of a recent book, Adrenal Cortical Neoplasia, Endocrine Clinics of North America Series, Volume 44, Number 2, June 2015
One Insulinoma Cure Begets Another
Many doctors never see a true case of insulinoma in their entire careers. One Mount Sinai physician saw two in just one year.
Many physicians spend their entire careers without finding a true case of insulinoma. Ronald Tamler, MD, PhD, MBA, Director of the Mount Sinai Clinical Diabetes Institute and Associate Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at the Icahn School of Medicine at Mount Sinai, cured two separate insulinoma cases in just one year.
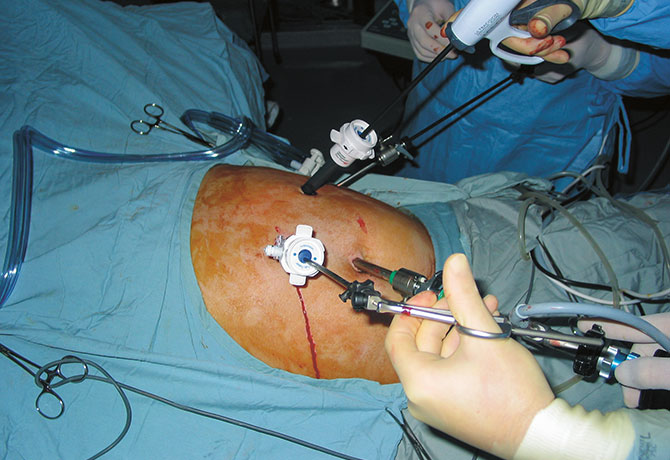
In 2014, a 53-year-old woman from Rockland County, New York, had been experiencing sudden drops in blood sugar (down to a disconcerting 14 mg/dl) that left her incoherent and with gaps in memory. The patient’s endocrinologist was stumped by the normal lab workup and CT, so he referred her to Dr. Tamler at The Mount Sinai Hospital.
Despite the patient’s completely normal lab workup, Dr. Tamler began to suspect an insulin-producing tumor. He noticed that glucose-level and C-peptide tests had never been conducted at the same time, so he ordered a repeat fasting test that showed a blood glucose level of 31 mg/dl with a C-peptide of 2.5. The case was closed: the patient had an insulin-secreting tumor. Once blood glucose drops below 60 mg/dl, insulin production should shut off. An endoscopic ultrasound located a one-centimeter tumor in the pancreas. Shortly thereafter, the patient underwent successful laparoscopic removal of the tumor by William B. Inabnet III, MD, Chair of Surgery at Mount Sinai Beth Israel and the Eugene W. Friedman Professor of Surgical Oncology at the Icahn School of Medicine at Mount Sinai.
A few months later, The New York Times Magazine featured the case in its column “Think Like a Doctor,” in which the magazine challenges its readers to solve a diagnostic mystery.
Hundreds of miles away in Florida, a teacher read the article and felt as though she were reading about her own case. Told by her endocrinologist that she did not have an insulinoma and that she was imagining things, she caught a plane to New York City to see Dr. Tamler. After reading her original workup, Dr. Tamler cut the visit short. “I recognized the same constellation as in my prior insulinoma patient, remembering that ‘normal’ is sometimes abnormal. Her insulin output during hypoglycemia should have been zero. We immediately sent her for an endoscopic ultrasound, which revealed a 12-millimeter insulinoma in the head of the pancreas,” Dr. Tamler recalls.
What should have been a quick referral for timely surgery touched off a three-month battle with the patient’s insurance company, which endorsed the care of a Florida surgeon who recommended an open laparotomy with a Whipple procedure. During this period, the teacher experienced near-daily hypoglycemia and had to begin taking diazoxide.
“Insulinoma enucleation (or removal) is always preferred unless malignancy is suspected. More invasive procedures such as the Whipple procedure are pursued if enucleation is not feasible or safe,” says Dr. Inabnet. “In most cases, insulinomas are benign and ideally suited for laparoscopic and minimally invasive approaches, as was the case here.”
Finally, the patient won her fight with the insurance company and proceeded to have surgery with Dr. Inabnet. She left The Mount Sinai Hospital two days after the surgery, cured.
Solving an Undiagnosed Case Of Acromegaly
V. Brown, a retired nurse, age 59, went to a New York City hospital in 2014, complaining of chest pain. A sufferer of lifelong medical problems, she was diagnosed with hypertrophic cardiomyopathy. After alerting her cardiologist to recent weight gain, she was referred to an endocrinologist.
 In November 2014, Ms. Brown developed a sudden, severe headache, which prompted her to revisit her primary hospital. Along with the headache, she was experiencing nausea and double vision. Her blood pressure was found to be elevated, so her doctor increased her prescription dosage of losartan—one of five medications she was taking. Due to her multitude of serious ailments, she was forced to retire early on disability.
In November 2014, Ms. Brown developed a sudden, severe headache, which prompted her to revisit her primary hospital. Along with the headache, she was experiencing nausea and double vision. Her blood pressure was found to be elevated, so her doctor increased her prescription dosage of losartan—one of five medications she was taking. Due to her multitude of serious ailments, she was forced to retire early on disability.
After seeing a news program that featured Donald Smith, MD, Associate Professor of Medicine (Cardiology) and Preventive Medicine at the Icahn School of Medicine at Mount Sinai, she made an appointment to discuss whether she qualified for bariatric surgery.
Dr. Smith, an endocrinologist who sees cardiac patients, suspected acromegaly after reviewing Ms. Brown’s history of spinal stenosis, sciatica, carpal tunnel, and sleep apnea, and hearing her concerns about recent weight gain and swelling in her face, hands, and feet. She also reported the appearance of widely spaced teeth, an enlarged jaw, and a shoe size that had increased from 8.5 to 13. Dr. Smith ordered labs, which came back showing an elevated insulin-like growth factor-1, or IGF-1. He immediately referred Ms. Brown to Eliza Geer, MD, Medical Director of the Pituitary Care and Research Center and Associate Professor in Endocrinology and Neurosurgery.
Dr. Geer confirmed that Ms. Brown’s IGF-1 level was elevated, at 566 ng/ml, with a growth-hormone level of 3.36 ng/ml, confirming Dr. Smith’s suspicion: the patient had been battling undiagnosed acromegaly, missed by her original physicians, for many years.
Dr. Geer again tested Ms. Brown’s growth-hormone levels after an oral glucose tolerance test: the paradoxical increase in growth hormone from 4.9 to 5.6 ng/ml confirmed the diagnosis of acromegaly. Dr. Geer then viewed her MRI and saw a pituitary tumor, which, based on the previous test results, she knew was a growth-hormone-secreting tumor and the cause of the acromegaly.
She referred Ms. Brown to Kalmon Post, MD, Surgical Co-Director of the Pituitary Care and Research Center and the Leonard I. Malis, MD/Corinne and Joseph Graber Professor of Medicine and Professor of Neurosurgery, who in July 2015 performed transsphenoidal surgery to remove the pituitary tumor. Immediately after surgery, Ms. Brown’s growth-hormone level dropped to approximately 1.5 ng/ml with an IGF-1 level of 348 ng/ml. After three months, her IGF-1 had decreased to 300 ng/ml, and her growth-hormone level was 1.53 ng/ml.

Ms. Brown continues to improve today through a multimodal course of care at Mount Sinai. If needed in the future, she has access to new medications that can aid in lowering her IGF-1 and growth-hormone levels through ongoing clinical trials at the Mount Sinai Pituitary Care and Research Center. She will be attending a monthly support group offered at Mount Sinai for patients with Cushing’s disease and acromegaly. The group—the only one of its kind in New York City—provides emotional support, education, and stress-relief techniques to patients with these rare conditions.
A Nurse Practitioner Solves a $72,000 Mystery
Sometimes it’s the simple solutions that solve problems. Such was the case for a 77-year-old male with type 2 diabetes seen at the Mount Sinai Diabetes Center with curiously uncontrollable sugar levels.
Living with type 2 diabetes for the previous eight years, the patient had maintained his health through a controlled diet and meticulous record-keeping of his blood glucose levels. One day, mysteriously, his sugar levels began to skyrocket.

The patient’s private endocrinologist put him on a difficult and expensive regimen of medications and restrictive diets that lasted two years but never helped his high sugar levels. Over time, his endocrinologist reached the point of prescribing 250 units of insulin. The patient was using one pen a day and still his sugar levels were too high.
In addition to the risks that this treatment posed to his health, it came at a cost: he used roughly $72,000 worth of insulin alone while his endocrinologist tried to diagnose why his sugar levels could not be controlled.
Knowing he needed a second opinion, the patient sought out David W. Lam, MD, Assistant Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at the Icahn School of Medicine at Mount Sinai, and the expertise of the diabetes team at the Mount Sinai Diabetes Center. On his second visit to Mount Sinai, the patient met with Cynthia Esrig, a nurse practitioner who is brought in to consult on cases in which a patient is experiencing high blood glucose levels. By the time Ms. Esrig met with the patient, his A1C test measured nearly 12 percent—almost double the target recommended by the American Diabetes Association for people with diabetes.
Ms. Esrig and the patient discussed his daily habits surrounding his diabetes care, focusing on his nutrition and insulin routines. She asked him to show her how he injected insulin. Observing him, Ms. Esrig discovered the root cause of the patient’s problem: he wasn’t removing one of the caps on the two-cap needle, therefore never injecting any insulin whatsoever into his bloodstream. The insulin would move through the first cap but not the second. The patient had never been shown how to use the pen properly before he met Ms. Esrig at Mount Sinai.
After receiving proper injection training from Ms. Esrig, the patient’s A1C levels normalized. Today he is meeting his A1C goal of around 7 percent and injects only 20 units of insulin per day—a 92 percent reduction in insulin from what had been prescribed before he came to Mount Sinai.
“Cynthia’s discovery is a perfect example of Mount Sinai’s practice of truly listening to a patient—a lost art in some medical centers,” says Dr. Lam.
A Rich Pipeline Offers Promise Against an Array of Diseases
Cutting-edge research by Mount Sinai Health System physician-scientists in a wide range of fields is helping the Health System uncover bold new therapies to meet the urgent needs of patients and society. The Health System, one of the largest in the nation, includes the Icahn School of Medicine at Mount Sinai, with 34 departments and more than 23 multidisciplinary institutes that are designed to facilitate breakthrough science.
Scientists and researchers benefit not only from extensive resources and talent inside the laboratory but also from the expertise of Mount Sinai Innovation Partners, a group that works across the entire system to attract critical funding and shape the newly developed technologies for application and commercialization.

In the field of lysosomal storage diseases (LSDs), for example, the development of small molecules—shown effective in early trials to reverse the toxic buildup of lipids in patients’ cells—holds promise for a new treatment paradigm for these disorders. Collectively, LSDs comprise the most common genetic disorder in humans. Although enzyme replacement therapy has been the standard of care for some LSDs, the inability of proteins to cross the blood-brain barrier renders this approach ineffective for about 90 percent of the 60 known lysosomal storage disorders.
Yiannis Ioannou, PhD, Professor of Genetics and Genomic Sciences at the Icahn School of Medicine at Mount Sinai, has developed a series of small molecules that can penetrate the blood-brain barrier and correct lipid-metabolism dysfunction in patient cells for at least eight LSDs. “We’re very excited by the results of animal studies for Fabry disease, and by an 85 percent decline in cholesterol accumulation for Niemann-Pick Type C,” two types of LSDs, he notes.
In kidney-transplant patients, physicians currently use measures of creatinine in the blood to monitor the transplanted organ’s status. But this method has a critical flaw: by the time increased levels of creatinine are detected, fibrosis has already developed and the kidney has been irreversibly damaged. Indeed, chronic fibrosis is the primary reason that 17 percent of kidney transplants fail by the third year, and fewer than half still function by the tenth year.
Barbara Murphy, MD, the Murray M. Rosenberg Professor of Medicine, System Chair of the Department of Medicine, and Dean for Clinical Integration and Population Health, is developing a portfolio of assays to monitor kidney function before and after transplantation. These noninvasive assessments, known as FractalDx assays, identify genetic signatures from simple blood tests to predict the likelihood that transplant recipients will develop fibrosis and graft loss. “Instead of being reactive and limiting the damage,” Dr. Murphy explains, “we’re developing a monitoring tool that can identify problems before damage occurs.”
Brain tumors, among the most aggressive cancers, consign roughly half of patients to an average life expectancy of 11 months following surgery. By the end of 2016, Isabelle Germano, MD, Director of the Comprehensive Brain Tumor Program and Professor of Neurosurgery, Neurology, and Oncological Sciences, expects to start clinical trials on a breakthrough stem-cell therapy she has developed, which, if proven successful, could prolong the lives of people with glioblastoma by several years. The approach delivers to the disease site autologous stem cells engineered to express a tumor-cell-killer gene that is activated once the tumor returns, which is 95 percent of the time.
Although some technical issues in cell manipulation remain, lab results have validated Dr. Germano’s work with induced pluripotent stem cells. “The future for treating brain tumors is in making the body’s own cells ‘smarter’ so they can fight the disease,” she says.
Top Recruit: Daniel S. Donovan, Jr.
We are proud to announce the recruitment of Daniel S. Donovan, Jr., MD, MS, CDE, as Director of Clinical Research in the Diabetes, Obesity and Metabolism Institute at the Icahn School of Medicine at Mount Sinai. He will also serve as a Professor of Medicine (Endocrinology, Diabetes and Bone Disease) at the Icahn School of Medicine.
 Dr. Donovan was formerly the Director of the Irving Diabetes Research Unit at Columbia University College of Physicians and Surgeons, and Associate Professor of Medicine at the Columbia University Medical Center in New York City.
Dr. Donovan was formerly the Director of the Irving Diabetes Research Unit at Columbia University College of Physicians and Surgeons, and Associate Professor of Medicine at the Columbia University Medical Center in New York City.
A top clinical investigator and expert on type 2 diabetes, Dr. Donovan has successfully administered industry-sponsored, foundation-supported, and NIH-funded projects focused primarily on improving the quality of care for patients with type 2 diabetes, especially in the primary care setting; developing new drug therapies; and improving cardiovascular outcomes. He is now also developing a program in Patient-Centered Outcomes Research at Mount Sinai.
Dr. Donovan obtained his medical degree from the Mount Sinai School of Medicine in 1986. Today he is a Fellow of the American Association of Clinical Endocrinologists and a certified diabetes educator, and has supplementary interests in the areas of neuroendocrinology, obesity, and bone disease.
Founded in 2008, the Mount Sinai Diabetes, Obesity and Metabolism Institute is the research counterpart to Mount Sinai’s nationally ranked Diabetes Center. Created in response to the rise of obesity, diabetes, and metabolic syndrome, the Institute endeavors to cure these disorders by developing better therapeutic and prevention strategies through basic and clinical research.
Endocrinology, Diabetes and Bone Disease
Download the Winter 2016 Specialty Report