Mount Sinai Mobile Interventional Stroke Team Travels to Patients, Resulting in Faster Treatment and Better Outcomes
Study finds stroke patients are nearly twice as likely to be functionally independent if treated by a specialized team that travels to them to perform surgical clot removal
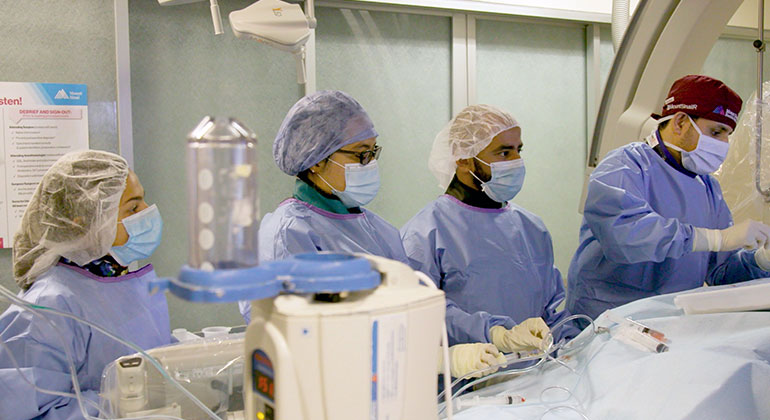
Stroke patients were almost twice as likely to be functionally independent—mobile and able to perform daily tasks—at 90 days post-stroke if they were treated by a specialized mobile stroke team that traveled to them to perform mechanical clot removal, compared to those who were transferred to a thrombectomy stroke center, according to research conducted within the Mount Sinai Health System and published today in Stroke, a journal of the American Stroke Association, a division of the American Heart Association.
The study examines results of a pilot program created by stroke specialists at Mount Sinai in New York City. Through this program, instead of transferring stroke patients to a specialized stroke center, a mobile interventional stroke team (MIST) traveled to the patient to perform endovascular thrombectomy—a surgical procedure used to remove large blood clots in patients with acute ischemic stroke. The MIST team includes a neuro-interventionist, an assistant, and a radiologic technologist. The trial focused on 226 patients who received endovascular thrombectomy at four hospitals within the Mount Sinai Health System between January 2017 and February 2020.
Medications to dissolve large blood clots in vessels in or leading to the brain are effective in about 15 to 20 percent of stroke cases. However, most patients with a large vessel blockage still require endovascular thrombectomy. Nearly 90 percent of strokes are ischemic strokes, caused by blood clots in an artery that blocks normal blood flow and oxygen leading to the brain. Since 2015, endovascular thrombectomy has been the standard of care for stroke therapy. Currently, the biggest barrier for stroke patients is timely access to this potentially life-saving procedure.
“Less than 50 percent of Americans have direct access to endovascular thrombectomy, with the other half needing to be transferred to a thrombectomy-capable hospital for treatment, often losing more than two hours of time to treatment,” said Johanna Fifi, MD, Associate Director of the Mount Sinai Cerebrovascular Center, Co-Director of Pediatric Cerebral Disorders, and Associate Professor of Neurosurgery, Neurology and Radiology at the Icahn School of Medicine at Mount Sinai and co-author of the study. “Every minute is precious in treating stroke, and getting to a center that offers thrombectomy is critically important. The MIST model addresses this loss of time and brain health by providing faster access to this surgical treatment.”
Researchers examined data from 226 patients who received endovascular thrombectomy at four hospitals within the Mount Sinai Health System (one is a certified comprehensive stroke center, and three are thrombectomy-capable stroke centers). Of those, 106 patients were treated by the MIST team, and 120 were treated by the current standard of care at hospitals without expertise in endovascular thrombectomy. Current standards are to treat patients with medications to dissolve the clot and then transfer the patient to a hospital with the expertise to perform endovascular thrombectomy. All patients in the analysis were functionally independent before having a stroke.
To assess outcomes, researchers used the modified Rankin Scale (mRS) and the National Institutes of Health Stroke Scale, two commonly used measures of the degree of disability or dependence in the daily activities of people who have suffered a stroke. They analyzed results of patients who were seen within six hours of stroke onset (early therapeutic window) and after six hours of stroke symptoms (late window).
For patients treated within the early window, the rate for a good outcome (mRS less than 2—mobile and can perform daily tasks) three months after the event was significantly higher in patients from the MIST group (54 percent) compared to the patients in the transferred group (28 percent). However, for patients treated in the late window, outcomes were similar, with 35 percent of patients in the MIST group having a good 90-day outcome, compared with 41 percent in the transferred group.
“Ischemic strokes often progress rapidly and can cause severe damage because as the brain is starved of blood and oxygen, and brain tissue dies quickly, resulting in serious long-term disabilities or death,” said Dr. Fifi. “Assessing stroke patients in the early window means that a greater number of fast-progressing strokes are identified and treated.”
Data for the MIST trial was collected prospectively, however, the analysis was conducted retrospectively. The MIST program continues as more institutions and cities implement the model.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.