
The Recanati/Miller Transplantation Institute (RMTI) is proud of its success record. More than 5,500 people have received a new lease on life through the RMTI’s organ transplant services. Here are some of their stories:
A Student at Icahn School of Medicine Saves Her Father’s Life by Becoming a Living Organ Donor

When school bus driver Edward Allen, 67, found out his rare liver cancer had reached a critical stage, his daughter Ashanay Allen, 27, stepped in to donate part of her liver—both have made a full recovery.
A Mount Sinai Patient Is First in New York State to Receive a Triple Organ Transplant

23 years after a successful transplant at Mount Sinai, in 2024, Mack Godbee’s heart started to fail last year—he needed a liver, kidney and heart transplant to survive.
A Grateful Kidney Transplant Patient Meets Care Team for Ice Cream

9 year old McKalya De Long received a life-saving kidney transplant in 2022. Two years later, the Make-A-Wish Foundation granted her wish to return to New York City to “do all the things I couldn’t do when I was here for my transplant.” She also fulfilled her wish to meet her transplant surgeon, Vikram Wadhera, MBBS, Associate Professor, Surgery and Renal Transplant and to share an ice cream with him. They were joined by Rafael Khaim, DNP, ANP-BC, FNP-BC, Clinical Senior Operations Manager, Pediatric and Adult Renal Transplant.
Ornithologist Is the First to Receive a Liver Transplant at The Mount Sinai Hospital Using a Donor Liver Enhanced by Pump Technology

Eduardo E. Iñigo Elias, 63, had waited more than six years when the call came from the Recanati/Miller Transplantation Institute at Mount Sinai that a donor liver was available for transplant
Mount Sinai Patient Receives a Life-Saving Liver Transplant Just in Time

After many years of living with primary biliary cholangitis (PBC), a chronic autoimmune disease, in 2021 Sharon Speer’s condition had developed into end stage liver disease and left her in urgent need of a liver transplant.
From Son to Father—the Gift of a Kidney and the Gift of Life

When 56-year-old Jose Calixto needed a life-saving kidney transplant, his son Jonathan, age 30, quickly offered to donate one of his kidneys.
Sister Saves Her Brother’s Life Through Liver Transplant at the Recanati/Miller Transplantation Institute at Mount Sinai
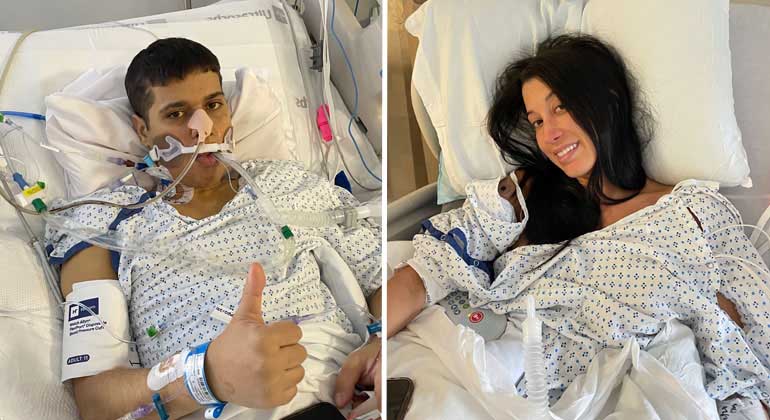
In his late teens, Zachary Castro was diagnosed with a debilitating bile duct disease called primary sclerosing cholangitis (PSC). By his mid-20s he needed a liver transplant. His elder sister Kayla offered to be a live donor - and saved his life.
Daughter Gives Lifesaving Gift To Dad
Two years ago, Steven Frey, of Long Island, gathered his three children to tell them that his liver was failing and he would need a transplant. After tests showed his daughter Marielle was a match, the two underwent surgery so she could donate part of her liver to him. Sander Florman, MD, director of the Recanti and Miller Transplant Institute at Mount Sinai, and team at The Mount Sinai Hospital performed the complicated hour’s long surgery. “As soon as we start cutting the liver in half, the liver starts to regenerate, and within six weeks 90 percent of it grows back,” said Dr. Florman. It has been almost a year since the transplant and both Marielle and Steven are doing great.
- Sander Florman, MD, Director, Recanti and Miller Transplant Institute, Professor, Surgery, Icahn School of Medicine at Mount Sinai
A Pioneering HIV-Positive Transplant Success Story

Kenneth Teasley, HIV-positive with end-stage renal disease, had been on a waiting list for a kidney transplant for five years. He learned from The Mount Sinai Hospital in the spring of 2016 about his eligibility for an organ from another HIV-positive patient. Mount Sinai was the first hospital in New York State and only the second in the country approved to perform kidney and liver transplants from a deceased HIV-positive donor to an HIV-positive recipient.
Unique Liver Transplant at The Mount Sinai Hospital Restores a Patient's Quality of Life

Jennifer Long is only person in the United States to have had a liver transplant due to porphyria-a disease that occurs when porphyrins-chemicals that help form many substances in the body, including hemoglobin, the protein in red blood cells-affect the nervous system and/or skin. An estimated one in 20,000 people carry the disease, which is actually comprised of nine separate disorders, but only 10 percent of people will experience symptoms.
Over several years, Ms. Long's acute form of porphyria had become so extreme that her nausea, the constant pain in her back, stomach, and legs, and attacks of paralysis forced her to be hospitalized for months at a time. In 2012, after a series of failed treatments and being rejected as a liver transplant candidate at two other medical facilities, Ms. Long, a resident of Maryland, was referred to Lawrence Liu, MD, Assistant Professor of Medicine, a specialist in porphyria and liver transplantation at The Mount Sinai Hospital. Dr. Liu and a team of medical researchers at Mount Sinai believed the best course of action for Ms. Long was, indeed, a liver transplant.
As Ms. Long moved up the waiting list for liver transplants, she was transferred by ambulance from Johns Hopkins Medical Center in Baltimore to The Mount Sinai Hospital for several months of testing and preparatory treatments.
"A transplant had never been done in the United States for a patient with porphyria and there was no precedent," says Dr. Liu. "It had been done in the United Kingdom and the early results that were published were more favorable then detrimental." Using the results from the procedures in the United Kingdom as a guide, Dr. Liu and his team were able to proceed successfully and avoid major setbacks.
Today, Ms. Long is free of the excessive porphyrins in her body that impeded her quality of life and is grateful for her remarkable gift. "The medical team at Mount Sinai did a wonderful job of taking care of me," says Ms. Long, who has written a letter of thanks to the family of her liver donor. For routine health care needs, she sees specialists at Johns Hopkins, and for annual follow-ups Ms. Long returns to her doctors at Mount Sinai's Recanati/Miller Transplantation Institute.
My Life is Yours, and Also, My Kidney

Carlos was unable to find a kidney donor for his wife Elena. He could not find one in his home country of Ecuador nor here the United States. For many years, Elena had been suffering greatly: She had anemia; she was not eating; and she was, according to Carlos, at the end stage of her life. A friend of his referred them to Mount Sinai because he thought that they would be able to help find a suitable donor. Carlos remembered their introduction to Mount Sinai and went on to say, “Since the first day we were treated well,” and that, “when we went to the hospital, we found an answer.”
The process of finding a donor took around three nerve racking months which included several meetings with various medical personnel, and numerous tests to see if perhaps Carlos was a potential donor. At the end of three months, and the end of test after test, Carlos received a call that confirmed he was compatible.
“I received the news from the hospital on my phone. I was at work,” he remembers. “They told me, ‘Carlos, you are compatible, congrats! Share the good news with your wife at home.’ My wife was not working at the time so I called her at home and we began to cry. Even now I feel like crying from such a joy. Thank God. When I told my wife the news, she asked me, ‘My love, are you sure you want to give me your kidney?’ And I said, ‘Of course, my love. My life is yours, and also, my kidney.’”
On June 27, 2013, the transplant was a success thanks to the team at Mount Sinai. Elena’s life was saved, she was able to return to her normal lifestyle, and she has been diligent in going to her regular follow up appointments. Carlos went on to say that he was fine as well, but didn’t want to talk about himself as much as he wanted to emphasize how amazing it was that his wife Elena had now, “come back to life.”
On the first anniversary of the surgery, the couple traveled to Ecuador to share the good news with family, and also went to church to thank God for the miracle. At the two-year anniversary, together with the family, Carlos and Elena continued with the tradition and went to the Catholic Church to thank God, followed by a great meal. Among all the changes in Elena, post-surgery, Carlos noticed her returned appetite more than anything. At the restaurant, Carlos marveled at the site of Elena stating, “My wife was eating and enjoying the things that she couldn’t eat before.” This moment, among others, still brings a tear to his eyes.
“My wife had kidney failure. Since we weren’t able to find a donor, with all of my love and care, I donated my kidney in order to save her life,” says Carlos. “Thanks to The Mount Sinai Hospital and the fact that we were compatible, we were able to restore my wife’s health. Now she is fine, thank you. “
Carlos no podía encontrar un donante para su esposa Elena. El no pudo encontrar uno en Ecuador, su país, tampoco en los Estados Unidos. Por muchos años Elena estaba sufriendo bastante: ella tenía anemia; no comía; y de acuerdo con Carlos, ella estaba en la etapa final de su vida. Un amigo lo refirió a Mount Sinaí porque él pensaba le podrían ayudar a conseguir un donante. Carlos recuerda su introducción a Mount Sinaí and comento “desde el primer día fuimos tratado muy bien” y “cuando fuimos al hospital encontramos las respuesta”
El proceso de encontrar un donante tomo alrededor de tres desesperado meses que incluyeron varias reuniones con varios personales médicos y numerosos exámenes para ver si talvez Carlos era un donante potencial. Al final de los tres meses, y después de terminar exámenes tras exámenes, Carlos, recibió una llamada que confirmo que él era compatible.
“Yo recibí la buena noticia del hospital en mi teléfono. Yo estaba en el trabajo,” el recuerda. “Ellos me dijeron, ‘Carlos tu eres compatible, felicidades! Comparte la noticia con tu esposa en tu casa.’ Mi esposa no estaba trabajando en ese tiempo entonces le llame a la casa y comenzamos a llorar. Inclusive ahora sentimos querer llorar de tanta alegría. Gracias a Dios. Cuando le dije a mi esposa las buenas noticias, ella me pregunta, ‘Mi amor, tu estas seguro de que me quieres dar tu riñón? Y yo le dije, ’claro que si mi amor’. Mi vida es tuya y también mi riñón.’”
En Junio 27 del 2013, el trasplante fue un éxito gracias al equipo de Mount Sinaí. La vida de Elena fue salvada, ella pudo retornar a su estilo de vida normal y ella es muy diligente con sus citas regulares de seguimiento. Carlos también dijo que él se sentía bien, pero no quiso hablar tanto acerca de el mismo tanto como quería enfatizar que maravilloso era que su esposa Elena ahora “volvió a vivir.”
En el primer aniversario después de la cirugía, la pareja viajo al Ecuador para compartir las buenas noticias con la familia y también fueron a la iglesia a agradecer a Dios por el milagro. A los dos años de aniversario, juntos con la familia, Carlos y Elena continuaron con la tradició n y fueron a la iglesia católica para agradecer a Dios seguido de gran almuerzo. Dentro de todos los cambios en Elena después de la cirugía, Carlos ha notado el regreso de su apetito más que todo. En el restaurante, Carlos admira a Elena diciendo “Mi esposa estaba comiendo y disfrutando las cosas que no podía comer anteriormente.” Este momento, sobre todo, todavía le traen lágrimas a sus ojos.
“Mi esposa tenia deficiencia de riñón. Como no pudimos encontrar un donante, con todo mi amor and cuidado, yo le done mi riñón para salvar su vida,” dice Carlos. “Gracias al Hospital Mount Sinaí y al hecho de que fuimos compatibles, pudimos restaurar la salud de mi esposa. Ahora ella está bien, Gracias.”
A Son’s Selfless Love

Just two months after donating his liver, Brian Clemente was in Upstate New York with his fiancé, Jessica, and friends for their joint bachelor/bachelorette party. He took a moment from the celebration to speak about his liver donation process, his current state, and the state of the liver recipient, his mother Pamela. With the surgery behind them, Brian now describes his mother as, “vibrant,” a remarkable change from the debilitated state she was in months prior. Clemente feels the two of them haven’t looked or felt this good in some time, stating that neither was experiencing any complications following the transplant procedure, thanks largely to the “angels” at Mount Sinai.
In 2013, Pamela had been diagnosed with Nonalcoholic Steatohepatitis (NASH), liver inflammation and damage caused by a buildup of fat in the liver. Pamela’s condition was not life threatening at the time, but over the years her disease had progressed at an alarming rate and the liver transplant required to treat it would have to be done sooner than expected.
It was Brian’s sister-in-law Deborah who gave the family their first glimmer of hope in the form of a blood test kit. As a Health Education Teacher at Felix V. Festa Middle School in Rockland County, Deborah was familiar with and had access to the tools needed to determine if there was a blood match within the family, which could potentially lead to a liver donor. Unfortunately, Brian’s father was ruled out as a donor due to his age. Brian and his two brothers Mike and Paul had no hesitation when it came to testing their blood types. After Deborah tested all three brothers it turned out that Brian, the youngest, was the only match. The family understood that complications could arise at any time between then and the operating table, but for the time being they were able to breathe a sigh of relief.
Brian recalls being at the hospital on April 15, 2015. They had both arrived early that morning and Brian was pacing nervously until his procedure began at 8:00 am. Pamela had just celebrated her 72nd birthday, and surgery had already been delayed a week by a fever that afflicted her. It was then that the two found comfort in the Mount Sinai transplant team—the “Angels,” that guided them through the nerve-racking process, holding their hands and reassuring them that everything was going to be okay.
Brian awoke around 3:00 pm, feeling great and completely surprised by his large torso scar. According to Brian, he was pleased at the sight of the scar because it wasn’t about vanity to him. He had given a part of himself to his mother, the woman who had been the rock for him and his brothers all their lives. His joy is best described in a Thank You note he had written to the transplant team, which included Marcelo Facciuto, MD, Sander S. Florman, MD, and Leona Kim-Schluger, MD. The note said: “My brothers and I have always looked at our mother as our guiding light, and we were in no way prepared to lose her. Thanks to the doctors and nurses at Mount Sinai, we get to keep her for a while—hopefully a long one.”
Pamela woke up in the early evening, and was met with tears of joy by Brian, who came into her room waiting to embrace her. Brian remembered her telling him about the angels she saw watching over her on the operating table, and thinking that the morphine must have been working its way through her system. However, evidence of such a miracle was further demonstrated when the family was shown a picture of Pamela’s removed liver, described by Brian as looking like, “hamburger meat.” Relief came over the family as they learned that they were lucky to have had the transplant done sooner rather than later, as Pamela might have had less time than originally anticipated.
Today Brian is eager to express his eternal gratitude to the transplant team members for doing their job or, more accurately, giving the “gift of saving lives and giving families hope.”
The Difference a Decade Makes

One of the things I remember best is how many friends he had,” says Brian Patton of his father William, a lifelong resident of Rumson, NJ. “We’d be driving in the car and my dad’s hand would constantly be going up waving to people driving by because he knew everyone in the town—and probably the next three towns over.” Brian also remembers “Willie” as the life of the party whose 69 years included joining the United States Navy, serving on the Rumson police force for 26 years, working security for Bruce Springsteen, and filling the roles of husband and father for his former wife Pegeen and Brian’s siblings Stephanie and Eric. “He was the guy who was out playing catch with you, taking us knee boarding on a friend’s boat; He coached my little league baseball team,” Brian says. “Even if he was working during my high school baseball games, I’d see the cop car out in left field, and there he was watching me play.”
But by the time Willie and his then wife Pegeen, along with Stephanie and Eric, attended Brian’s graduation from Arizona State University in 1996, things were changing. “I remember my mom looking at him and saying he just didn’t look right. His color was different and he was retaining a lot of fluid,” Brian says, adding that a subsequent visit to the doctor resulted in the diagnosis that would change everything: cirrhosis of the liver. In the coming years as Willie waited for a new liver to become available for transplant, his condition worsened with symptoms ranging from extreme fatigue and weight loss to mental confusion. “He was being admitted to our local hospital every two to three months because he would slip into a coma due to the high levels of toxins in his blood and brain,” Eric remembers.
“I remember him comparing himself to Walter Payton,” Brian says of the Chicago Bears running back whose own liver disease prompted him to become a spokesperson for organ donation. “He told me when he realized things were getting really bad he looked down at his wrist and his watch was so loose … He even said he’d take a shower then realize he’d already taken a shower before because his towel was still wet—he knew he was too young to be going through all that.”
Twelve More Years

In May 2000, Willie was admitted to Mount Sinai Hospital under the care of his transplant hepatologist Leona Kim-Schluger, MD, so he would be on-site should a liver become available. About a month into his stay, Brian called to talk to his dad and was told he was being wheeled into surgery; a liver had just been identified, and the Patton family was en route to the hospital. And almost immediately after the transplant procedure, Willie seemed to be returning to his old lively self. “My dad said he woke up after the transplant and the two people over him were my mom—then his ex-wife—and my grandmother who’s his ex-mother in law,” Brian remembers. “And the first words out of his mouth were: Now I know I’m not dead.”
And what Willie woke up to was another 12 years of life, which were packed with irreplaceable memories, experiences, and new arrivals. “We got our dad back,” Brian says, launching into a list of the things Willie would have missed were it not for the gift of a new liver. “My brother and I getting married, all seven grandchildren being born, the Yankees winning the World Series, the Giants winning the Super Bowl. I sent a letter to Dr. Kim-Schluger thanking her for everything and I put in all the things my dad got to experience over those extra 12 years.”
A Foundation Is Formed
Over a decade later in March 2012, Willie was again ill enough to be admitted to the hospital, and Brian—now living in Colorado—flew home for a week (which father and son dubbed “Spring Break 2012: Mount Sinai Hospital”) to be with him. Back in Colorado that April, Brian had a dream about his dad then couldn’t get back to sleep. While checking emails on his cell phone, he received a call from his brother Eric at 5:30 am saying the doctors thought the end was coming. Brian rushed for a flight, arriving at Mount Sinai the same afternoon. “At the very end, he opened his eyes, so he saw all of us around,” Brian remembers. “You’d think we’d be crying, but we were just happy we were all there.”
It was while Brian was writing the obituary on the plane on the way home (an unorthodox obituary that was printed in a local paper and later recognized by Reader’s Digest) that the idea of forming a foundation to honor their father and help other families of transplant patients began to take shape. “You hear about paying it forward; our idea was to pay it back,” Brian says. “He got those extra twelve years—how do we pay people back for that?”
The Patton family formed The Willie Patton Foundation with the goal of raising money that would be gifted to institutes such as the Recanati-Miller Transplantation Institute to help families of transplant patients. “We called on friends for donations and on local restaurants where the owners had known my dad for 60 something years,” Brian says. “It was amazing the number of people and companies who were willing to make a donation on my dad’s behalf.”
The Foundation’s largest fund raiser to date was a 2014 silent auction that resulted in a $10,000 check Brian and his sister personally presented to Sander S. Florman, MD, and Dr. Kim-Schluger over lunch in March 2015. “Our goal is to help the families and patients going through the transplantation process with a focus on housing,” Brian says. As a result, the Foundation’s contribution has helped cover the cost of staying at the Transplant Living Center, a “home away from home” with 10 bedrooms maintained by RMTI for patient families. “We grew up in Rumson, which is 50 miles from Sinai, so we could come up in the morning, go home at night and sleep in our own bed. But other families can’t do that. So we wanted to make sure they had a place to stay that wasn’t part of their worries and it was hopefully an escape that could feel like home.”
During that lunch, Dr. Kim-Schluger suggested framing Willie’s photo and story to hang in the Transplant Living Center, and Brian hopes seeing the display might be encouraging to other families who could find hope in learning about the 12 years a transplant gave to his father.
“My dad would be so proud of the Foundation,” Brian says, adding that his family plans to continue raising more money to help RMTI families. “He was always somebody who cared about everybody else, and I think he’d be very happy that we’re doing the same.”
A Grateful Mom Gives Back

After Kelly and Tyler Smith suffered a string of shocks in the first week of their newborn Matilda’s life—her lethargy and vomiting a few days after birth, the diagnosis of liver failure, the ambulance dash to Mount Sinai—the couple entered another world of living in the hospital and watching their daughter’s deterioration while waiting for a liver to become available for transplant.
“We knew she was slipping away, and there was nothing I could do for her—I couldn’t even change her diaper or feed her,” Kelly remembers. “Before this I had been completely naïve to the world of pediatric organ donation—I’d honestly never even thought about babies needing baby-sized organs for transplant.”
During that dark time of relentless worry—during which the couple was also missing their small son, Parker, who was staying with relatives—it was the little things that kept Kelly going, including knitting and crafting supplies given to her by Mount Sinai’s Child Life Program, which supports young, hospitalized patients and families using art and other media.
“When I was able to do something and say to the doctors and nurses who came in, ‘Look what I made,’ then they would smile, and the air became lighter,” Kelly says. “And I think little things like that impacted Matilda because she could sense that energy and feel whether her parents were sinking into despair or if we were able to lift out of it.”
Matilda received her new liver November 2, 2012, and was soon responding so well her hopeful parents were able to take her home—after having spent 72 days in the hospital. And the gift of life that had launched Matilda’s journey to health is something that Kelly found both astonishing and humbling. “During what I would imagine was the most painful part of somebody’s life where they lost a child,” she says, imaging the donor family’s perspective, “they were able to give someone else a chance—to give me the opportunity to be Matilda’s mother and to give Matilda the opportunity to grow and shine. And that is absolutely beautiful.”
Repaying a Priceless Gift

While in the hospital, doctors had prepared the Smith’s for the possibility that Matilda may not develop as a normal child. That reality was with the family as they settled into life back in Canton, NY, where caring for Matilda would involve a strict medication regimen, routine blood work, Mount Sinai visits every three months, and additional considerations like the need to keep Matilda’s environment especially clean.
But at five months, Kelly was thrilled to see her daughter sit up—then go on to meet all major milestones. Now, 19 months after her life-saving transplant, Matilda is a thriving, beaming toddler, spending her days playing with big brother Parker.
With such an opportunity to celebrate life, Kelly had felt inspired to give back to the world that had spared her daughter. She started a blog, Cloudy Day Gray, on which she shares episodes of Matilda’s stay at Mount Sinai, as well as current updates on both children, and an assortment of colorful crafting ideas. And it was memories of the crafts that had helped her cope in the hospital that prompted her to embark on a whole new project.
“My premise for the blog is that we all have cloudy days—it’s what you do with those clouds that defines who you are,” says Kelly. “Since leaving the hospital and doing the blog I’d really been wanting to start making craft packs for the parents of the PICU at the hospital.”
Kelly’s idea was to assemble bags of crafting supplies—each with the components of a different project—and donate them to families currently in the Pediatric Intensive Care Unit (PICU). With the help of Provo Craft (makers of the Cricut ExploreTM ) and three other bloggers, the project steamed ahead, and after weeks of preparation Kelly had 15 completed packs consisting of a stenciled canvas bag containing the supplies needed to make a pinwheel, finger puppets, or colorful bunting. With the plan of bringing a supply of craft packs to Mount Sinai for each of Matilda’s three-month visits, Kelly brought the first “shipment” of packs to the PICU in March.
“I really believe that when you can smile and be joyful in the hospital room, it changes everyone’s outlook,” Kelly says. “Crafting gave us the chance to talk about something that wasn’t so heavy, which also helped us see the people taking care of our child in a different way, and the dynamic became warmer. And that’s what I want for other people—to bring happiness into their hospital rooms.”
In addition, Kelly hopes the involvement of the other blogs—Kids Stuff World, The Proper Pinwheel, and You Are My Fave—will help spread awareness about pediatric organ donation to wider audiences who may be as naïve to the struggle of children waiting for new organs as she once was.
Spreading Smiles

Not long after Kelly’s first delivery, the craft packs had been very well received. “I have worked with many families who have commented on how the projects have brightened up the room,” says Angela Koeneker, Creative Arts Therapy Manager of the Child Life Program. “I have also seen many kids using the pinwheels when they are completed.”
And Koeneker is mindful of the spirit of giving behind those brightened rooms. “We are so grateful for Kelly's generosity and creativity,” she adds. “What a wonderful gift to use her own experience in the hospital setting to improve the stay for other patients and families.”
When Life Gives You the Blues, Eat Blueberries
Richie Rubin’s positive attitude is an inspiration to those coping with waiting for an organ transplant.
Richard “Richie” Rubin is currently waiting for a life-saving liver and kidney transplant at Mount Sinai. Because he has kidney failure, Richie, 57, must undergo hemodialysis treatments three times each week for approximately four hours each treatment. Because of his liver cirrhosis, he must be admitted to The Mount Sinai Hospital, almost two hours from his home, to undergo paracentesis (a process to remove the fluid that builds up in his belly). Just prior to being diagnosed with liver and kidney failure, Richie had beaten liver cancer and was successfully treated for hepatitis C.
Given his circumstances, one would assume Richie would be feeling depressed—overwhelmed by his health condition and limitations. On the contrary, Richie considers himself to be one of the luckiest men alive.
Why Richie Feels Lucky
Richie will tell you he has the best family and community surrounding him. His wife, Joann, takes exceptional care of him, happily driving him to appointments and making sure he eats well and has learned how to cook delicious foods even with his restrictions. He gushes about his children: a son, Justin, who helps run the family electronics business, and a step-daughter, Danielle, who just brought his beautiful granddaughter, Giovana, into the world. The list of those who love and support Richie is very long—and he appreciates each and every person. My brother, Gene and my sister, Adrienne, have been by my side through this journey. Whatever I have needed, they have provided it.
Richie also feels lucky to be so confident in his medical care. Leading his team of providers at Mount Sinai is Thomas Schiano, MD, whom Richie calls “heaven on earth,” adding: “Dr Schiano’s team has been so supportive of me physically, emotionally, and spiritually. I couldn’t have asked for a more knowledgeable and committed team of individuals.”
Richie also says he is grateful that he has gained wisdom and inner strength and can see his own resilience: “I have learned to appreciate the things most take for granted in the everyday.” He now enjoys a cold glass of water (which has been restricted due to his kidney disease) and anything with blueberries. “It’s the simple things in life that make me happy now,” he says.
Looking Ahead
With so many people currently helping him to cope and prepare for transplant, Richie is looking forward to his life following his transplant when he can redouble his efforts to help others. “It is important people know my story. I made mistakes when I was younger, but I am now 11 years sober with Alcoholics Anonymous,” he says. “I want to help others avoid what I am going through now by learning from my lessons. I want to make a difference.”
Whether Richie knows it or not, he has already made a huge difference. By his powerful example, he is showing us all how to cope head-on with life’s challenges; how to maintain hope, dignity, and joy; and how to allow loved ones to be there for you—and how to enjoy blueberries, even when you may have the blues.
A Long Wait

Irene and Melvin renewed their marriage vows on their 31st wedding anniversary. Four months later “Poppy,” as Melvin was lovingly called by Irene, died of liver failure at age 64.
Theirs was a true love story. They met as co-workers at a nursing home in the 1980s; Irene was an LPN and Melvin was a custodian. He wooed her with his sense of humor and his kindness. Irene affectionately says: “Poppy was the first to give you the shirt off his back…he would help anyone in need.” They married, had three children (Anthony, Justin, and Ann Marie), and lived a very full life in Lawrence, New York. Melvin seemed to devour life. He was an avid fisherman and gardener, had many friends and community connections, and was a former marine and volunteered as a firefighter for 22 years. He also worked as a custodian at the St. Joachim’s Church in Cedarhurst in Long Island.
A Troubling Diagnosis
The year 2012 proved to be the beginning of a very difficult time for the Pereira family. Melvin was diagnosed with cirrhosis and started a regimen of medications that stabilized his condition. Then “Superstorm Sandy” struck and virtually destroyed their home. Irene, who was being treated for a medical condition, needed to move in with family in another state to recover. While she was away, Melvin and their son Justin worked tirelessly to rebuild their home, and Melvin’s health seemed to buckle under the stress. He became too weak to work so he retired early. He required regular paracentesis (a procedure to remove fluid that has collected in the belly). He was in and out of the hospital due to infections and had many complications.
By Christmas 2012, Melvin was told by his trusted physician, Thomas Schiano, MD, that his liver condition was end stage and he would need a liver transplant within a year. Irene becomes teary when talking about her husband’s physician. “Dr. Schiano was compassionate, caring, and honest with us from the beginning. Melvin had such a great relationship with him. They knew how to communicate with each other.”
The Wait Begins
Melvin was placed on the national wait list for a liver, and the Pereira’s knew Melvin’s only chance to live was to receive a transplant. They had to learn to cope with the uncertainty of when or if an offer would come. Unfortunately, New York State has a very low donor registration rate—one of the lowest in the country—therefore many patients do not survive what can be a long wait for an organ to become available.
To add to the challenge of waiting and coping with the symptoms of Melvin’s illness, the Pereira’s home was still under construction. Melvin and Irene were confined to living in one room, preparing home cooked meals with a toaster. Although the situation could have been disastrous a strong community and support from friends, church, their local fire department, and the Ladies Auxiliary kept them from feeling alone. “So many have been kind and gracious and kept us going.”
Melvin was called in twice for a potential transplant; they were so close that they packed bags and came to hospital. However, both times they returned home due to issues of compatibility and matching. Those were the most difficult times, and Irene credits Dr. Schiano for encouraging Melvin to keep going.
Unfortunately, Melvin did not receive a third offer for a transplant and died waiting on December 30, 2013.
Irene and her children want to tell Melvin’s story. They want to keep his spirit alive. Their pain and sense of grief is palpable. They are clearly proud of him and the battle he fought. As Melvin’s son Justin says, “Many wars are fought in this world. They bring pain and sorry to many. My father for a year fought a war within himself. He stood tall and fought til the end. It might not have been in a fire or overseas, but he fought to keep his life and be with his family.”
The Pereira’s also feel compelled to tell the more difficult side of the story of organ donation. They are the faces of the wait—the faces of grief as a result of the shortage of organ donors. While they can’t save their loved one they can hopefully help save someone else’s “Poppy” by sharing their story and encouraging more interest in organ donation.
Saved by a Selfless Gift

When Akil Thomas started vomiting every day in the spring of 2011, he initially thought he had the flu. But when the problem continued for weeks, his wife Toya insisted they go to The Mount Sinai Hospital emergency room, where doctors ran tests that resulted in a shocking diagnosis: Akil was in end stage renal failure with only three percent of his kidneys functioning. He was admitted to the hospital for a week of testing then sent home to follow a regimen of blood pressure medication and regular nephrologist visits with the understanding that he would soon have to start dialysis.
“It was a lot to take in,” says Akil, a 41-year-old husband and father living in New York City. “But I knew I had to stay strong for my wife and son. What I told them was: This is not going to be our life; we’re going to defeat this.”
But staying strong proved challenging throughout the fall as the vomiting persisted and fatigue intensified. Finally in November Akil’s doctor decided it was time to start dialysis, and the Thomas’s were given a choice between hemodialysis (which would involve visiting a center three days a week for four-hour sessions) or peritoneal dialysis (which would involve being connected to an at-home system for 10 hours each day while he slept). Akil chose hemodialysis and began coming to Mount Sinai every other day for therapy.
“And that was when our journey really started,” says Toya of the treatment schedule and the draining effect it had on her husband, who frequently felt fatigued and sick. “It was like I was looking through glasses that didn’t belong to me because I was seeing something that couldn’t be my life. We went from being active parents with a thriving teenager and traveling all the time to everything changing so drastically. I’d have to wake up in the mornings and tell myself: ‘This is my today; not my forever.’”
When the hemodialysis schedule and dietary restrictions proved too difficult, Akil switched to peritoneal dialysis. Although it was a relief to reclaim some control by doing therapy in the comfort of home, the Thomas’s had to juggle medical equipment and monthly deliveries of supplies.
Toya was tested to determine if she could donate a kidney to her husband, but she wasn’t a match. And with the wait time for a new kidney through the New York Organ Donor Network estimated at 7-9 years, the Thomas’s assumed this would be their life until an organ became available.
Another Option Emerges
In September 2011 Akil and Toya were at Mount Sinai for an exam when Scott Ames, MD, made an unexpected suggestion: “Did you know you could be part of the ‘swap program?’” Dr. Ames explained that in cases where a patient needing a kidney has a loved one who is willing to donate but isn’t a match, both patient and loved one can be entered into the National Kidney Donation Registry, a system that tracks other unmatched donors and recipients throughout the country. The Registry vets all those people to identify chains of “swaps,” so that Akil, for example, could receive a kidney from a stranger matching him, and Toya would in turn donate her kidney to a stranger matching her.
“I was ecstatic,” Akil says of the opportunity. “I thought our prayers had been answered.” In May 2013, after meeting certain safety guidelines, Akil and Toya were entered into the system. At the end of August, a Mount Sinai transplant coordinator called to say matches had been identified for each of them, and their surgery date would be October 8.
In the coming weeks as arrangements solidified, Akil and Toya would learn about their respective donor and recipient. Akil’s donor was a wife and mother from San Diego, whose husband had altruistically donated a kidney (meaning offering up an organ for donation to a stranger) the previous year, and she was inspired by his gift to also offer her kidney. Toya’s recipient was a patient at Johns Hopkins who had been “in the system” waiting for a compatible donor for two years, and Toya was the first person to match. “It hit me that if I’m the one person to be a match, after everything we’d gone through I was supposed to be here,” Toya says.
The Turning Point
“The morning of the surgery I was actually excited to be at the hospital,” says Akil of the few hours before his procedure on Tuesday, October 8. “I felt like my life was about to go back to normal—going to the park with my son and traveling with my family. Plus I had a lot of trust in Dr. Ames.”
“I was petrified,” counters Toya, who was waiting for her own procedure in the room next door. “I had always been the one waiting for Akil to come out of a procedure—this time we were both going in.” But Toya was committed and began her surgery with Juan Pablo Rocca, MD, at 7:30, while Akil’s procedure with Dr. Ames started at 10:00. Both came through with flying colors, with Akil, especially, having a very positive response.
“It was like he jumped out of bed running,” Toya says, “while I was like the turtle trying to get into the race.” With the help of the Mount Sinai staff, husband and wife progressed well in the four days before their discharge. “Everybody on that 9th floor—the nurses, the guys who delivered the meals—everybody was just wonderful,” says Toya. “And that new donors wing is something to talk about—I had a suite!”
It was the day after surgery that Dr. Ames told Akil the full story about his donor: The husband and wife had altruistically given their kidneys despite the fact that their two children suffer from rare medical conditions that had required years of surgeries and intense care.
“People keep telling me what a good thing I did for Akil, but of course I’ll do anything to save my own husband,” says Toya. “It was his donor who did a truly great thing—and I will never be able to thank her enough. The fact that she gave something up to whoever was in need so selflessly is a kind of humanity you don’t find in 2013. And if anybody who has that much humanity in them is now a part of Akil, we’re going to be ok.”
A New Life
Although Toya’s recovery at home involved initial challenges like fatigue, gas, and “tolerable” pain, Akil was immediately thriving. “He has a spring in his step and his eyes are brighter,” Toya reports. “Everything about him looks so different.”
For Akil, the journey back to health has filled him with a profound sense of gratitude. “I live for my wife and son, and I think this was put in front of us to make us stronger as a family,” he says. “I’d always told them we were going to get over this. And on October 8 we defeated it; our lives went back to the way we knew it, and I feel so blessed.”
And Akil adds one more thing: “One day I would love to talk to or even meet my donor—just to give my thanks and hug the person who literally saved my life.”
A Donor Family Story - Knitting to Heal and Give Back

To watch Andrew Max Davis work his magic on the small screen is to step back in time. In the 1990s, the child actor was in multiple TV shows and commercials, including, memorably, General Mills’ ‘KIX are for kids’ campaign. With presence beyond his years, he had the makings of a future star. But it wasn’t to be. In 2007, Andrew was killed in a car crash. He was 17 years old.
For Andrew’s mother, Sharon Jones, now an employee of Mount Sinai, it was a defining moment. Though initially uncomfortable with the idea of organ donation, when asked, she agreed. Upon getting home from the hospital she found an organ donor card in Andrew’s wallet – affirming for her that it was the right thing to do.
Six years later, that decision – and the knowledge of the 90 lives that Andrew thus helped heal or save – remains a major source of solace. But it was hardly enough to blunt the pain. For that reason, three years ago, Sharon took up knitting. It proved to be powerful therapy. “When you lose a child, it doesn’t go away,” says Sharon. “The knitting keeps me thinking about something else.”
Realizing that knitting was something others could benefit from as well, a year and a half ago, Sharon decided to begin an informal class. She hung up posters around the hospital and more than 30 people showed up. Many of them meet daily still.
Today, the group’s purpose has grown beyond propagating the craft to making blankets for donor families as part of an initiative called “Sean’s Gift.” Named for a 24-year-old Iraq War veteran who died after getting hit by a car in his hometown, the project was started by his mother, Marie LaPersonerie, whose friend gave her a blanket to wrap Sean in before his organs could be recovered. Finding that blanket to be a source of comfort and connection after Sean’s death, she started the project to provide blankets to families in similar situations.
For Sharon, it was only a natural initiative to get involved with. The group has already made five blankets specifically for families at Mount Sinai and is working on their sixth. Adding extra poignancy to effort, for Sharon, is the fact that Mount Sinai is where Andrew as born. “He was born here, so I’m trying to continue his story here,” says the halcyon mom. “I’m just trying to do my part to keep his story going – but also to help other people.”
For Pediatric Patient, Family is the Best Medicine

A visit by six-year-old Raymond Leedy to Mount Sinai is a looked-forward-to event. Even beyond the nurses' and doctors' pride at "Ray Ray" doing so well, he's known for being an affectionate, lovable kid. He gives high fives and hugs whenever he comes in, and always has a big smile on his face. What makes his positivity all the more poignant is that, for a six-year-old kid, Raymond has already had more than a lifetime's worth of challenges. It's a continual reminder for everyone that it could easily have turned out differently.
A sick baby boy, abandoned at birth
Raymond's story begins in September 2006 at the University of Medicine and Dentistry of New Jersey, where he was born to a mother with drug problems, two months premature. Weighing a mere two pounds, Raymond was found to have necrotizing entercolitis (intestinal failure) almost immediately. Raymond's mother abandoned him shortly after giving birth. It was the nurses and doctors who would become Raymond's parents for his first two years of life.
His case file from there tells the story of an incredibly sick baby boy. Weeks after being born, Raymond underwent surgery to remove most of his intestines, a procedure that involved inserting a central line so that nutrients could be administered directly to his blood stream. This intervention came with high costs, however; central lines are prone to infection and delivering high concentrations of nutrients directly to a child's bloodstream can often cause liver damage. Raymond encountered both.
In June 2008, however, things began looking up. Under the care of Kishore Iyer, MD, intestinal surgical director at the Recanati/Miller Transplantation Institute at Mount Sinai, Raymond received an intestinal transplant. Finally stabilized, he was released to a foster family the following fall. Soon after, he was placed with a second. Although it was a positive environment for a special needs kid, given his foster mom's age and the fact that she was already looking after multiple children, there was no guaranteeing the length of his stay.
A nurse goes the extra mile
The first time Christine Chamberlain met Raymond was in 2008, shortly after he left Mount Sinai to live with his first foster family. As Christine tells it, he endeared himself immediately. "He was just a sweet, lovable kid," she says. As she continued to watch him grow, that easy-going spirit – in spite of his difficult circumstances – continued to impress. "He walks into the office and hugs everyone and says hello to everyone," she says, describing a typical visit. "It's infectious. You see him and just want to hug him."
But there were other reasons Christine felt compelled to take a personal interest in his case. As a nurse, Christine knew that Raymond would have the best long-term prognosis with parents who could look after his developmental and medical needs. At the same time, closer to home, Christine thought of her father, who himself was raised by good foster parents and the difference it made for him. With 40,000 kids already in foster homes in the Tristate region though, Christine also recognized the odds. Finding a home for any foster kid is hard. Who could take care of – and love – such a special needs child?
Fortunately for Raymond, Christine had another patient, Sierra. Sierra was transplanted at a very young age (following a liver and intestinal transplant) and was also adopted by a family in central New Jersey. Since then, Christine watched as Sierra grew from a quiet little girl into a "sweet and polite" young lady. It reflected good parenting, Christine thought. She knew it was a long shot, and wondered if it was even right to ask. But Sierra's parents had adopted kids with special medical needs before; could they do it again?
An act of kindness becomes a calling
Raymond wouldn't be the second – or even the third child– that Patty and Chip Leedy adopted. The first time they'd opened their home to a child was more than a decade earlier, shortly after getting married. Patty was working at Children's Specialized Hospital in Mountainside, New Jersey, and expecting her first child. It was there that she met Andy, a patient in need of a home. Having been adopted herself, Patty's heart went out to the boy. After talking it over with Chip, they decided to take Andy in – one month after giving birth to her daughter Shannon. Shortly after giving birth to her second child, Casey, Patty met Trevor, a pediatric liver transplant recipient also in need of a family. They took him as well, bringing their burgeoning family to four. In the following years, they would adopt two more: Dylan, Trevor's half brother, and Sierra, Christine's other patient.
It was about eight years after adopting Sierra that Patty got Christine's call. She was standing in her kitchen and the kids were off at school. "I was a little anxious," Christine confesses, thinking back to that conversation. "It's not an easy phone call to make."
Patty told Christine that she'd have to talk it over with Chip and the kids; Raymond would be their seventh child. With the oldest two off at college, though, they had the space to provide. Plus, by now, what began as an act of kindness had become something of a calling. "You hate to see kids who don't have somebody," Patty explains.
A few days later, Patty called back to say they'd love to meet Raymond. It took almost a year, but Patty, Chip, Dylan, and Sierra went to Ray's foster family's home finally meet. Next, Raymond's foster family came to visit the Leedys. Then there were some overnights before Raymond came to live with the Leedys full time.
Raymond moved into the Leedy home in August, 2012 (he's pictured above with the Leedy Clan on the day of his legal adoption). "When he first came, I thought ‘Oh, he's going to have some trouble sleeping.' But he went right up to his room," Patty recalls. They'd put up fresh sheetrock in Trevor's old room and filled it with toys. They also hung a picture of Raymond's former foster family so that he'd feel more connected and at home. "Periodically he'll point it to and declare, ‘my family!'" Patty says. "Then he'll point to his new brothers and sisters and declare again, ‘my family!'"
"He likes it here," Patty says, 10 months after first taking Raymond in. "From the first day he was here he was calling us ‘mom' and ‘dad.' … He's seldom upset, unless he's not feeling good. He's easy going. The way his life started out, he had to learn to adapt to change." The affection in Patty's voice is evident.
Last fall, Raymond was enrolled in Montgomery Township schools, where a devoted team of teachers is helping with his education and development. Patty is also actively involved, contributing frequently to PTA efforts. As for Shannon, Casey, Trevor, Dylan, and Sierra, they've taken in Raymond as one of their own.
"[Sierra] is very affectionate with him," Christine says, reflecting on seeing them in clinic. "She holds his hand. … You can tell she really likes having him around, too."
A happy ending and new beginning
When asked what would have happened if she hadn't connected Raymond with the Leedys, Christine pauses. "He would have wound up in foster care," she says. In the foster system, he likely would have gone from home to home. Upon turning 18, he probably wouldn't have been able to live independently, since a difficult childhood is especially handicapping for a child with developmental and medical needs. "A kid like Raymond is going to do really well with parents like Patty and Chip because they teach him; he goes to school; they're interactive; and there are other children there with him," Christine says.
As for Patty, when asked what it means to know the difference she and Chip can make for Raymond, she answers simply: "It's just nice to be able to help out." She quickly changes the focus to Raymond: "I think he'll do well so long as he can stay healthy, so long as his medications keep doing what they're doing, and he has a good support system."
Particularly on that last point, by all indications he does. Six years after being left in the hospital at birth, Raymond is receiving long-term care from his Mount Sinai team and settling into a good home where he is beginning to thrive. It bears out the old adage: sometimes family is the best medicine.
A New Father Weathers the “Perfect Storm”

Unable to sleep, Kevin Pugh grabbed his phone from his bedside and started composing a letter to his unborn child:
“The day I learned of your existence and pending arrival … the world I lived in crashed down and a new reality was upon me. … What kind of father will I be? What do I want to teach you? The world is a beautiful place and so many wonders await you. I can’t wait to show them all to you and see them for the first time again through your eyes…”
For Kevin, it was an introspective time. Almost a decade after being diagnosed with primary sclerosing cholangitis (PSC), a slow-progressing disease of the bile ducts that leads to cirrhosis of the liver and eventually liver failure, the condition was finally catching up to him. He was still able to work from home, but chronic fatigue and sleep deprivation, common symptoms of PSC, were increasingly taking their toll. It was clear that he needed a new liver. But in New York State, where the wait time can be as long as seven years, there was no telling when one might come. Would he be there for his daughter’s birth? What about being there to watch her grow?
If that wasn’t enough to worry about, in October—just as Kevin’s condition was worsening—Hurricane Sandy came barreling down, flooding his hospital, closing it for weeks.
“It’s a stressful process as it is to wait for a transplant and not know when you’re going to get the call,” Kevin says. Add to that a deteriorating condition and expectant wife, and you might say it was a perfect storm.
Upon the advice of his NYU doctor, Kevin transferred to Mount Sinai’s Recanati/Miller Transplantation Institute. It proved a good match. “When I first met with [the team at] Sinai, I had a good feeling. … I felt like it was the right place,” Kevin says. At Mount Sinai, Kevin was followed closely by his clinical coordinator, Ramon Kapoor and his hepatologist, Leona Kim-Schluger, MD, associate director of the RMTI. Within days, they arranged to have his wait time transferred over. They were also able to get him additional points towards his wait list rank, improving his odds of getting an organ sooner.
Within weeks, the team’s efforts paid off. In the middle of a February night, “the call” finally came. An organ had been identified in Buffalo.
“The call was surreal,” Kevin says. “I wasn’t expecting it to happen that quickly.”
The following day, as Kevin waited for surgery, his thoughts were with his wife and child, and how the stress of the situation would affect them. As for himself, ironically, he felt a degree of relief. “I was so nervous about getting the call the week my child was born,” he says. “That became one of my biggest fears. I wasn’t necessarily scared of what could happen in the surgery—I was really more concerned about whether I would get this call when my wife is giving birth and has to do it alone.”
That night, Kevin was finally taken in for surgery. Jami waited down the hall. Afterwards, she barely left his side. “My wife was amazing throughout the process,” Kevin says. “She is such a strong woman.”
A New Beginning
Just a few weeks post-surgery, Kevin found himself waiting in a hospital room again—this time as Jami went through labor before giving birth to a healthy baby girl. He was healthy enough to sit bedside the entire time, like Jami did for him. He wouldn’t have had it any other way.
The couple named their daughter Delaney, after Kevin’s grandmother.
“I want to be healthy and share in your happiest moments,” Kevin wrote to her in that letter last fall. With his daughter just two weeks old, he reiterated that desire, adding how invigorated he’s been since her birth. “Since the week of my daughter’s birth, my energy levels have been so much better—I’ve been feeling so much better,” he says. Underscoring the sincerity of the point, when asked how much sleep he is getting with a newborn in the house, he chuckles. “Not much,” he says.
Having navigated the storms of the past year successfully, Kevin looks forward to the adventures of fatherhood ahead.
Paying it Forward: Connecting Lives to Save Lives

For ten years, Dennis Bligen, the former New York Jets running back, kept his health problems a secret. Through tests and treatments, weight gain and hair loss, the last thing he wanted was for his family to worry.
“They would always look at me like something was strange, but they didn’t force the issue too much,” he says with a laugh. “I never really filled them in on what was going on, mainly because my mother is a worrywart.” But while Dennis kept his game face, beneath he was scared.
The first signs that something might be wrong had become apparent during a summer league basketball game around 2002. As Dennis ran down the court, the former pro running back felt sluggish and heavy. He looked at his ankles: They were size of his thighs. The next day his doctor told him to go straight to the hospital. But that was the last thing Dennis wanted. He was coaching football at St. John’s University, his alma mater, while being involved with multiple community and business ventures. Besides, he still thought of himself as young and invincible. As he puts it: “Life was going on.”
But as his symptoms got worse, Dennis was forced to confront them. So began his ten-year odyssey of tests, misdiagnoses, and treatments for conditions he turned out not to have. In 2011, he finally saw a nephrologist who got the call right: focal segmental glomerulosclerosis (FSGS), a hereditary condition that leads to the formation of scar tissue in the kidney and, eventually, organ failure.
By that point, there was no way around it: Dennis needed a new kidney.
The Farmer’s Daughter from Iowa
When Jill Christensen’s flight touched down in New York City in 1989, she could never have imagined the way her life would become forever entwined with five others – Dennis’s included – 25 years later. That year, she was a newly minted University of Iowa grad, and after landing a plum job as an athletics trainer at St. John’s University in Queens she decided to leave the farms of her native Iowa behind for a chance to make it big in New York.
When Dennis – then just returning from five years in the NFL to coach at St. John’s – heard a farmer’s daughter from Iowa would be joining the staff, he imagined she’d be in over her head. Sure enough, there were times early on when Jill was seemingly lost. Dennis, a coach by instinct, took her under his wing.
“He kind of showed me the ropes,” says Jill. “We became dear friends.”
As Dennis’s health deteriorated over the subsequent years, Jill – like Dennis’s family – knew something was wrong. But Dennis remained stoic. Thus, when Dennis made a passing remark that he was going to need a new kidney, Jill was hardly surprised.
“I just knew that I’d get tested,” she says, thinking back to that conversation. It was the least she could do for her mentor and friend. “I’m a true believer that if it’s meant to be, it’s meant to be. So I put it in God’s hands and thought if it’s supposed to happen, it would,” she says.
But as fate would have it, Jill didn’t match.
The Father of Two from Virginia
Around the same time that Dennis was undergoing tests to be placed on the wait list for a kidney, 600 miles away in Virginia, John Detwiler got an email. It was from a colleague in New York whose seven-year-old daughter needed a new kidney. Born with a rare kidney disease, it would be her second. Her mother had already donated with 18 months of giving birth.
Though John had never met this man or his daughter, as the father of two young kids himself – a son and daughter – the message hit a chord. Seeing he was the right blood type for the little girl, he got tested. “What’s another kidney going to be worth to you? What are you giving up, and what is someone else going to be able to gain from it?” John recalls thinking at the time. “Someone else could be gaining years of life.”
When John learned that, although he would make an excellent donor, he wasn’t a suitable match, he remained undaunted. Doctors in Virginia asked him if he’d be willing to participate in a possible kidney swap – a chain of donations between people in need of kidneys who have willing donors who don’t match. Having come this far already, after talking it over with his family, John decided to say yes.
There was no way to know that around that same time, Jill Christensen had said the same thing to the same question herself in New York.
Kidney Swaps: Connecting Lives to Save Lives
Kidney swap chains are not easy to arrange. In addition to the dozens and sometimes hundreds of staff required for the screenings and eventual surgeries, computer data bases are often required to find strings of donors and patients throughout the country. And that’s the easy part. Finding willing and eligible donors remains the biggest challenge. Although the procedure today is extremely safe, it’s no small task for a person to put their work and life on hold – let alone to do so for someone they might not ever meet.
In a kidney swap, as the name implies, living donors give a kidney to help a friend or loved one indirectly. Because they’re willing to donate, but don’t match their desired recipient, they are connected with another donor-recipient pair in a similar situation. Each donor gives to the other donor’s intended recipient. In this way, both recipients get kidneys that match, and both donors see their loved one’s life spared.
Such chains can grow from four people to many. Moreover, considering the deceased donor kidneys made available for others on the wait list thanks to the swap process, the number of lives saved quickly multiplies.
The heroes in all this are the living donors who make it possible. But for Jill and John, that was the last thing on their minds. For them, it was just the right thing to do.
The Surgery: Friendships Formed and Solidified
The many moving pieces finally came together in August 2012. Two weeks after completing the screening, Jill received a call informing her that a recipient had been found. John by that point had been matched to Dennis, and another donor was found for the seven-year-old girl that inspired John to begin his quest initially.
While it’s normally rare for swap donors and recipients to meet, John, Dennis, and Jill all wound up in rooms next to each other at Mount Sinai. Within a day they were going between them, trading stories, talking about their families and telling jokes.
“I just remember laughing and talking about absolutely nothing,” says Dennis, recalling those days in the hospital fondly. “We were all just thrilled to be in that situation. You’d think I’d be the most thrilled. But you know, it seemed like those two were just as thrilled and happy to give an organ as I was to receive one.”
Dennis’s surgery, performed by RMTI Director Sander Florman, MD, went well, and his recovery was made easier by having Jill and John nearby to share in the experience.
The family of the little girl that John donated his kidney to save also came by. It was only the second time he’d met them. The first was on his way to the operating room.
“Dennis will tell me, ‘Oh, Jill, you’re so amazing,’” for doing this, Jill says. “But John is really amazing. … When he didn’t match the little girl, most people at that point would have said, ‘I’ve done my part.’ But not John – he continued into the swap program. He got into it for her, and he’d never even met her.”
If you ask John, he’ll say humbly that it’s no big deal. But he and the girl’s family continue to remain in touch, trading texts and Facebook messages often. The same is true for him and Dennis. They exchanged cards over the holidays and ‘Happy New Year’ texts on New Year’s Eve.
Paying it Forward: The Dennis Bligen Kidney Foundation
The morning after Dennis got out of the hospital, he was back on the field coaching football. “The kids thought it was cool. The parents thought I was crazy. Most of them were looking at me and shaking their heads,” says Dennis with a laugh. But he wasn’t about to put the experience behind him completely.
As Dennis had been readying for surgery, his family – who for so long had known something was wrong, but not known how to help – had begun making plans to form a new foundation in Dennis’s honor, as well as an inaugural gala to raise awareness and funds for kidney donation. “The original idea came from my siblings,” explains Dennis. “Not many of them could help as donors, so they were trying to find other ways to help.”
In November 2011, the family members had settled on the idea of a foundation and threw themselves into scheduling a walk-a-thon, seminars, workshops, lectures, and the gala. In addition to raising awareness of kidney disease in general, the program is also committed to raising awareness of kidney swaps. “Most people are amazed at how rampant chronic kidney disease is around the world,” says Dennis. In spite of this, “Most people I speak to have not heard of the swap program. I had never heard of it until I came to Mount Sinai. That’s critical – that’s crucial right there. If I hadn’t learned of it, I’d still be on the list right now.”
At the Dennis Bligen Kidney Foundation’s inaugural gala, Susan Lerner, MD, of Mount Sinai spoke of the reasons why swaps are not more common: “A lot of times people have a hard time giving to someone if they don’t know who it is. They look at it differently.”
Reflecting on that, Jill put it this way: “There are so many people in the world, there are so many people who can give. … You only need one kidney to live. A lot of people don’t understand that. I kind of just look at it like: God was bored that day so he threw two in.” She laughs.
As Dennis, Jill, and John move on with their lives, it’s a message they hope to carry forward.
For more information on the Dennis Bligen Kidney Foundation, visit the foundation’s Facebook page.
Family, Faith, and a New Kidney Give Blind Musician a Second Act

Ask Larry about music and the troubadour waxes poetic. “I’m eclectic in my tastes,” he says, listing Steely Dan, Elvis Costello, the Beatles, and Earth, Wind & Fire among his favorites. He has a recording studio in his home; he’s put out an album, and he writes, plays, and sings original compositions for his church. In addition to being an avid musician, he’s also an author – the first book in a trilogy he’s writing is already in Barnes & Noble and he is working on a book of poems. He also used to teach acting to at-risk kids, and before losing his eyesight, was a dedicated painter as well.
But in December 2011 all that creative energy came to a halt. After years of “gluttonous” habits (as Larry puts it), in spite of his end stage renal disease and need for dialysis, one day he collapsed on the floor of his apartment. Siblings found him hours later and rushed him to the hospital.
He would spend the next four weeks unconscious in a hospital bed.
“From December 15 to January 15 my mind is blank. I was knocked out, hospitalized – they thought I was going to pass away,” Larry says. Doctors warned family members that his condition was grave. But eventually they were able to bring him back. When Larry finally awoke a month later in Kings Brook nursing home, where he was sent for long-term care, he found himself in despair. He had lost his remaining eyesight and was in terrible shape physically. Normally jovial and good-natured, he was angry and depressed. As he puts it, “I wasn’t myself.” Proving the point: Larry had lost all drive to make music.
But if Larry had given up, his brother and doctor didn’t. Over the following six months, both coaxed him to get better. His brother, Stanley, started taking him on trips back to his apartment. After months away, his first homecoming was bittersweet. “When I first came to my apartment, it was very foreign for me,” Larry says. “I had been gone for six or seven months, so I was lost.” Against the advice of others – but believing in his brother – that first visit, Stanley let Larry go into the house for half an hour alone. It was a galvanizing moment. Says Larry: “All I did was sit on the steps and cry.” Over the following weeks, Stanley let his brother stay longer with each visit, before returning him to Kings Brook each night. The visits helped focus Larry’s mind and rebuild his resolve. After years of neglecting his health, and particularly his kidney disease, Larry became determined to turn the page. He would get a kidney transplant.
The Musician’s Second Act
Getting a new organ is not as simple as taking the old one out and putting the donated one in. For starters, in the case of kidney transplants, the old kidneys are kept in place. But more relevantly for Larry, new organs require lifelong care. Patients must be incredibly diligent about the anti-rejection medication regimens, checking in with doctors, and staying healthy overall. Qualifying for a transplant therefore requires more than tests of physical wellbeing; doctors must be convinced of a patient’s willingness and ability to take care of the organ over time.
For Larry, who wound up in a hospital and nursing home in part by not managing his kidney disease properly, the first hurdle to a new kidney was convincing doctors he would take the transplant seriously. Fortunately for Larry, in addition to new resolve, he also had the support of his brother, brother’s girlfriend, and other siblings to help reassure the medical team. And after meeting with Susan M. Lerner, MD, MD, a renal surgeon at Mount Sinai Medical Center, he found an advocate in her as well.
In November 2012, almost a year after collapsing in his home, Larry underwent surgery for a new kidney. He came through with flying colors. Though he found aspects of the initial recovery at times painful, he appreciated the attention he received from hospital staff. “I know I’m difficult; I know that for a fact,” says Larry with a laugh. “The one thing about the nurses at Mount Sinai – they must take a courtesy course – they are so nice and cheerful.”
Several months after surgery, Larry has recovered and reports doing well. Most indicative of a successful recovery: his passion for making music has returned. In late March, he performed at his first major gig in over a year, a women’s benefit concert at the King Cultural Arts Center.
A spiritual man, Larry says his favorite passage of scripture is Proverbs 3:5-6, which counsels putting faith in God, even when things seem grim. In addition to the family members, doctors, and nurses who saw him through, Larry credits that faith with helping him persevere. In addition, he’s particularly appreciative of his surgeon, Dr. Lerner: “She was a life changer,” says Larry.
In his second act, Larry looks forward to making a difference for others through his music. “There is so much chaos, so much confusion in the world … there is a little room and a little space for someone to bring some comfort, some compassion,” Larry says. “I want to do it through music. I want people to have their lives changed through music. And not through Larry Banks; but through the music that God has gifted me to share with the human race.”
After a Midnight Dash and Neonatal Liver Transplant, a Sunny Outlook for Baby Matilda

For Kelly Smith, it was the longest drive of her life: four hours in an ambulance from Syracuse to New York City beside her nine-day-old daughter, fighting for her life.
As the driver tore down I-81, heading south through Pennsylvania before cutting back into New York, Kelly found herself alone, battling thoughts. “Where would we have a funeral? What would we do? How would we get past it as a family?” she recalls now. She thought of her son: “How are we going to explain that you had this sister and now she’s gone? How as a family are we going to deal with that loss?”.
Though she tried to stay positive, like any new mother, she couldn’t help but fear the worst, she says. “That [first] night I didn’t have any hope.”
A week earlier it had been a joyous occasion. After a smooth pregnancy she gave birth to a seemingly healthy baby girl, and in those first few days all seemed well. But suddenly Matilda became lethargic; it was taking more effort to get her to nurse. Then she started throwing up after eating. Assuring herself that it was just new mother jitters, Kelly called the doctor anyway. Take her to the ER, the pediatrician counseled. Neither imagined just how serious the situation was.
Acute liver failure in neonates is so rare that its precise incidence is unknown. It can be caused by a number of factors. And in most cases, it’s fatal.
When doctors at the local emergency room ran tests, that’s precisely what they found: Matilda’s liver was essentially non-functioning. Recognizing the severity of the situation, they sent Kelly—with nothing more than the clothes on her back and the diaper bag she grabbed on her way out the door—to the regional medical center two hours away in Syracuse. After six hours and more tests it was clear the situation was dire. Matilda needed the help of doctors in New York City—and she needed it now.
For Kelly, the experience was surreal: “I just kept telling myself that it was ok, it was ok. But it was a huge shock when we found out it was something really serious,” she says.
Trailing her in the ambulance was her husband, Tyler, mother, and two-year-old son.
Arriving at Mount Sinai, doctors moved swiftly to assess Matilda’s status, initiate life support, and begin the process for possible transplantation. Given her age and the severity of the case, within days she was at the top of the pediatric list.
In the Care of Mount Sinai
Over the ten weeks that followed, Ronen Arnon, MD, head of pediatric transplant medicine, and the rest of the care team took strides to keep Kelly and Tyler abreast of their daughter’s status and also to check in on their emotional wellbeing. For Kelly, in retrospect, it was the little things that made the ordeal most bearable: cups of coffee brought by nurses; “normal” conversations with residents who were around the couple’s same age; and outside the hospital, a “meal train” of food made possible by Kelly and Tyler’s friends. As for their two-year-old son, Kelly and Tyler’s families were fortunately able to look after him in Montana for a few months.
“We were living in the PICU with nothing, not even a toothbrush, and the nurses there really took us in, and the doctors were so kind,” Kelly says. “We felt really good and really taken care of.”
Five weeks after arriving at Mount Sinai, doctors came to the young parents with urgent news: A liver from a recently-passed, two-week-old infant in Michigan had become available. Extracting it would be difficult, and Mount Sinai surgeon Jang Moon, MD, would fly to Michigan to assist. Even if successful, they warned, the risks remained abundant. But with Matilda’s condition deteriorating, it was her best shot at life.
“When the team came to us and said they had a possible match, we both just looked at each other and said, ‘yeah go for it.’” Kelly says of her and Tyler. “It was really clear and obvious that she needed a liver … and she needed it now.”
It turned out that Matilda needed a new liver even more than any of them knew. When doctors successfully completed the surgery, they told Kelly that less than 1 percent of Matilda’s original liver was still functioning and alive.
A Hopeful Outlook
The days following the transplant were harrowing, but with the new liver, Matilda quickly began to improve. After 72 days in the hospital—but only slightly more than a week after the transplant —she was discharged in mid December. Three months later, at time of writing, she is happy, healthy, bubbly and doing incredibly well. She loves to laugh and smiles with every kiss from her big brother, says a thankful mom, Kelly. “I don’t want to say we’re out of the woods yet, but I’m feeling confident,” she says.
Most recently, Kelly started a blog to share the family’s experience and Matilda’s continued recovery. In addition to commentary from Kelly, it features colorful photos of a proud older brother, a thankful dad, and a beautiful baby girl. Recently, Kelly posted about Matilda sitting up by herself for the first time. The pictures of a smiling Matilda, bright blue eyes, blue bow on her head and pink flower on her dress say it all. Of all that happened leading up to that milestone, Kelly writes: “It is nice to think that I can forget about all of that, even for just a moment, and consider her to be a normal healthy baby.”
Months after that harrowing dash to New York City, the thankful mom looks forward to the journey ahead.
A Lifetime of Pain Transformed by Transplantation

Anthony Neal describes himself as a “veteran” of pain. His war wounds are surgical scars; they tell the story of years of bodily trauma brought on by chronic intestinal disease. Now 46 years old, Anthony says, “I was literally born with pain.” He was premature and underwent emergency surgery at two weeks of age to untwist his intestines. Issues around his intestines would plague him for years.
Anthony’s doting mother closely watched over him. She made sure he ate well and often. He was a “chunky” child, so when he would go to the doctor with complaints of stinging belly pain, he was always told he was fine and sent home—undiagnosed.
Living with Chronic Pain
Anthony learned to cope by developing a high tolerance for pain. “My need to fit in and feel like everyone else enabled me to shut the pain out,” he says. “I even played football and basketball in school.”
In high school, Anthony was diagnosed with ulcers and colitis, and given heavy medicines to manage the symptoms. He also changed his diet and lifestyle and was able to cope with the periodic bouts of pain on his own. As a young adult, he got a job with the postal service and became a father. However, he always suspected the underlying problem related to his health was not resolved. His way of coping with this uncertainty was to block it out and avoid going to the doctor.
In 2006, however, Anthony got very sick. He started to lose weight rapidly, his skin became discolored, and his blood pressure would fall so low he had fainting spells. His former tactics if distracting himself from the pain were of no use. He was hospitalized and finally given a definitive diagnosis of Crohn’s disease (a chronic condition causing inflammation in the lining of the digestive tract, which leads to severe abdominal pain and malnutrition).
Surgeries were performed to fix his intestines, but they failed, leaving him even worse off. In fact, Anthony was near death following one procedure that left him in a coma for 30 days. He became so malnourished that he was requiring daily Total Parenteral Nutrition (TPN) through a shunt in his chest. It became clear that an intestinal transplant would be required to save Anthony’s life, and he was transferred to Kishore Iyer, MD, and the Mount Sinai Intestinal Transplant team for an evaluation.
Finding the Road to Recovery
By the time he arrived at Mount Sinai, Anthony was beaten down mentally and physically. Due to the complications and scarring resulting from his prior surgeries, he would need to undergo many more surgeries to “stretch” his skin with tissue expanders so he could be safely closed after transplant. After several months of preparations and waiting, the call for a transplant came in November of 2012. The surgery went exceptionally well, and Anthony recovered so quickly he was discharged several months earlier than expected.
Today Anthony says he takes nothing for granted. He is back to enjoying the simple joys of life: food, exercise, and time with his 9-year-old son Antoine. He is looking forward to returning to work. Anthony is the epitome of a survivor; he has tenacity, grit, and resilience. He is grateful for the “Gift of Life” granted to him by an organ donor and for the exceptional care provided to him by the members of the RMTI team. “The team is wonderful,” he says. “They are so kind and caring. I felt I was safe and in competent hands. We inspired each other.”
While he was once a “veteran” of pain, who nearly died of malnutrition and infection, Anthony now appears a picture of health (the photo accompanying this story was taken approximately 1 ½ years after his transplant). The RMTI team wishes for Anthony a long life free of pain and many years of good health.
Young Liver Transplant Recipient Committed to Raising Awareness about the Need for Living Donors
At Matt Rosiello’s baptism, someone remarked that he appeared yellow. His mother Randy took him to the pediatrician the next day and things moved rapidly from there. Matt’s pediatrician had seen one case of Biliary Atresia during his residency and had a strong sense that this was the cause of Matt’s jaundice. The pediatrician had recently read a paper on Biliary Atresia and made a quick call to the author, Dr. Keith Benkov, Chief of Pediatric Gastroenterology and an Associate Professor of Pediatrics, at Mount Sinai. The next day Matt Rosiello began a relationship with Mount Sinai that has lasted 23 years.
Biliary Atresia is a serious liver disorder that occurs before or shortly after birth when a baby's bile ducts (the tubes that carry bile from the liver) become blocked. The body needs bile to aid digestion and carry wastes from the liver out of the body. When blocked ducts prevent bile from being excreted, the liver becomes damaged. Left untreated, it leads to liver damage and eventually liver failure. The disease affects an estimated one in 10,000 newborns. When Matt was two months old, he had his first surgery at Mount Sinai. This surgery was called a Kasai procedure which attempts to create bile drainage from the Liver to the Intestines. His family was told that although the surgery was successful there remained a strong possibility that Matt would need a liver transplant in the future.
In 2007, after many liver infections and hospitalizations, Matt’s liver started to fail. Four years later, in early 2011, Matt was listed for transplantation. His family and friends first looked to Living Donation, but there were no viable matches among them. As Matt’s health deteriorated, the hope for a donor liver in the New York area seemed bleak. Eventually Matt had to consider traveling to another region of the country where the wait time for a new liver was shorter. Thanks to an incredible amount of support from family and friends, including a great fundraising effort, Matt was able to travel outside of N.Y. to another Region which had a shorter waiting list. Matt and his family traveled to Ohio, and he was placed on the Transplant list in March of 2011. Matt was fortunate and received his Transplant on July 7, 2011.
After his successful surgery, and after spending almost 4 months away from home, Matt returned to New York and to the RMTI at Mount Sinai and Dr. Kim Schluger for his follow up treatment. Matt still considers Mount Sinai his hospital. Today, he is working full time and continuing to grow his DJ business, (DJ little Matt Entertainment). He is committed to educating people about the importance of organ donation, speaking about the need for living and deceased Organ Donors and participating in fundraising efforts whenever possible.
“If more people were Organ Donors, there wouldn’t be so many people waiting on the list and dying each day,” says Matt with obvious conviction.
His Father adds, “It was only through the efforts of Matt’s doctors and the entire hospital staff, that Matt was able to overcome the odds and make it to adulthood. Mount Sinai has been an invaluable part of Matt’s journey.”
His mother adds, “It does indeed take a village – in this case, an entire hospital staff – to raise this child and give him the gift of life – real life – that is what Matthew has because of Mount Sinai.”
One day - One family - Two liver transplants: Sisters share a very special day
The joy of welcoming a baby daughter into the world was short-lived when Rachel Golombeck's daughter, Devorah, stopped opening her eyes and slipped into a coma within days of her birth in March 2001. Tests revealed that Devorah had a rare, potentially fatal disease known as maple syrup urine disease (MSUD). The disease is named for the maple syrup scent of the urine in untreated babies. Passed down through families, MSUD affects the body's ability to break down certain amino acids found in protein, leading to a dangerous buildup if untreated.
Rachel was referred to a team of metabolic disease specialists at Mount Sinai and a relationship began between Rachel, her infant daughter, and the group of Mount Sinai physicians– a relationship so caring that Rachel could only describe it as "incredible."
Almost unbelievably, soon after Devorah's condition was stabilized, Devorah's 15 month-younger sister, Esther, received the same diagnosis. Now the team at Mount Sinai was treating both girls, monitoring them while they were on a carefully controlled diet, undergoing constant lab tests, and so many hospitalizations that Rachel lost count.
Rachel was desperate for a cure that would allow her girls to lead a normal life. She inquired about liver transplantation, an optional treatment for people with MSUD, but was told by the girls' doctors they didn't need liver transplants – not yet. A donated liver from a person who does not have MSUD would provide enough of the enzyme necessary to metabolize protein and cure the disease's symptoms. Within a few years, however, Esther had become quite ill. Devorah grew increasingly ill as well. It was apparent that transplantation was now the only answer.
Devorah and Esther were put on the liver transplant waiting list in the spring of 2009. The call came that a match for Esther was available first. The Golombeck family came to Mount Sinai from their home in New Jersey and waited for the liver to arrive. As the hours ticked by Rachel wondered what the future would hold. That afternoon while she was waiting, Dr. Kishore Iyer, Surgical Director of the Pediatric Liver/Liver Transplant Program at Mount Sinai's Recanati/Miller Transplantation Institute, approached her and told her something she could have never anticipated: Another liver had become available that was a match for Devorah. Both girls' transplants were performed within the next 24 hours.
Together, they recovered from surgery with the help of the staff, who Rachel described as "warm, accommodating, approachable people who listen to you, sympathize with you, and care for you." She said, "Bedside manner makes a world of difference for the child and the parent. They (the staff) took something so difficult and made it so much easier... Times two!"
Today, the sisters, ages 11 and 10, keep a very busy schedule. They excel in school, are active in sports, and are enjoying life to the hilt, said Rachel.
Avoiding a Liver Transplant: Noa’s Story

Noa Oelsner was born on August 31, 2011 by C-section weighing 9 pounds 12 ounces. Her parents Amalia and Dan could not have been more delighted with their beautiful, bouncing baby girl.
Then, within less than a week of Noa’s birth, red spots began to appear on her body. Noa’s pediatrician examined them but was unconcerned. The red spots continued to appear and after a few more visits to the pediatrician, Amalia and Dan decided to take Noa to a dermatologist to have the spots checked. The dermatologist immediately wanted to perform a biopsy. Noa’s father was not ready for that, and at a Friday Shabbat dinner, a friend, who is also a pediatrician, at Mount Sinai recommended calmly but firmly that they take Noa on Monday to a doctor she knew. She said she would arrange the appointment herself.
Still unalarmed, Noa’s parents followed their friend’s advice and met with the doctor. The doctor ordered an ultrasound test and during the test, the technician’s face said it all. Afterward, a parade of doctors filed in to confer with Amalia and Dan. The bad news was that there was a tumor on Noa’s liver, but the good news was that it was a hemangioma (a noncancerous tumor) and it was treatable. The Oelsners were then referred to Dr. Ronen Arnon, Medical Director of the Pediatric Liver Disease and Liver Transplantation Program at Mount Sinai, who they were told had successfully treated a similar case a year earlier.
Coming to Mount Sinai
When the Oelsners met with Dr. Arnon, he began by reviewing the results of Noa’s ultrasound. He then ordered an MRI (magnetic resonance imaging) test, a painless, non-invasive test, on Noa to gather more information about the tumor. The MRI revealed not one but multiple vascular tumors on Noa’s liver. Dr. Arnon explained to Amalia and Dan that there was a treatment available for their daughter’s condition – a treatment with almost no side effects -- discovered by doctors in France that used the medication propranolol (Inderal®), a drug normally prescribed for high blood pressure. The French doctors had stumbled upon the possible efficacy of propanolol for treating conditions such as Noa’s when they gave a patient with high blood pressure, who coincidentally had hemangiomas, the drug. The patient took the blood pressure medication and the hemangiomas disappeared.
Dr. Arnon and his team at Mount Sinia followed suit by successfully treating another baby with the same type of tumor as Noa’s with propranolol.Their experience, one of the first 10 published cases in the world, was documented in the Journal of Pediatric Gastroenterology in 2012.
Dr. Arnon recommended a similar course of treatment for Noa in the hope of helping her and avoiding a liver transplant later on. Children like Noa, and others with similar conditions, sometimes need liver transplantation as the vascular tumor grows and compresses other organs, he explained. The only treatment option prior to propranolol was high- dose steroids which have many side effects; furthermore, response to this treatment is generally not so good, Dr. Arnon said. The Recanati/Miller Institute was one of the first centers in the world to start using propranolol to treat pediatric liver hemangiomas and to publish its experience with the new therapy in the medical literature.
Moving Forward with Hope
Coping with their infant daughter’s illness and having to make decisions about what was best for her was extremely difficult for the family. But Dr. Arnon’s confidence and his willingness to answer every question, no matter how complicated or minute in detail, helped them move forward with hope, the Oelsners said.
And move forward they did. Noa will soon celebrate her first birthday. She is a beautiful, precocious child. As the hemangiomas on her body have shrunk more than 50 percent and the tumors on her liver have almost completely disappeared, the family is forever grateful to Mount Sinai and to Dr. Arnon and a treatment that has made all the difference for their little girl.
Little Girl’s Drawings Express Boundless Joy and Gratitude

One look at Karol Cardenas’ drawing “Me and My New Liver”and it’s hard not to be struck by the strength, optimism and gratitude it conveys. In the center of the drawing is a heart and in the heart is a little girl with curly brown hair (Karol) standing next to her father with the words “Thanks Dad” written in very careful script.
Anyone who knows Karol knows that this sweet, spirited nine-year-old has gone through more than most people do in a lifetime. Karol, the daughter of parents from Columbia, was born at Flushing General Hospital in Queens, NY. Just moments after her birth, her pediatrician had to give her parents Carolina and Edison (Ed) very disturbing news. Their infant daughter had biliary artesia, a rare, congenital disease of the liver that has no known cause and occurs in approximately one in 10,000 children. The immediate tell-tale sign was baby Karol’s jaundiced eyes.
Despite her diagnosis, Karol thrived as a baby under the care of her pediatrician and progressed normally in her development. At one year of age, she came to Mount Sinai and was seen by doctors here every three to six months. Although the family’s use of the English language was limited, Mount Sinai used Spanish-language interpreters and Karol’s condition was followed uneventfully for seven years. It was during a routine visit in September 2011 that Karol’s doctor noticed she had very low oxygen saturation (low oxygen levels in the blood). Tests were done for hepatopulmonary syndrome, an uncommon conditions that occurs when liver disease has advanced to the lungs. Shortness of breath is one of the signs of the syndrome. Karol was diagnosed with hepatopulmonary syndrome in September 2011 and listed for liver transplant.
Her mother volunteered to donate a portion of her liver but she was not a match. Karol’s father did match, but he had a condition known as fatty liver and would have to diet in order to qualify as her donor. Diet he did, and in March 2012, Ed was able to donate a portion of his liver to his daughter.
Today, Karol and her family revel in the simple pleasures of just being alive. Dr. Ronen Arnon, Medical Director, Pediatric Liver Disease and Liver Transplantation at the Recanati/Miller Transplantation Institute at Mount Sinai, beams at the mention of Karol and other children who have received transplants at Mount Sinai. He calls them “my heroes.”
Fraternity Brothers Bonded Forever

David and Bob met more than 30 years ago as college roommates. They hit it off immediately, became fraternity brothers and enjoyed their college years together. After college, Bob asked David to be the godfather to one of his children and they were in each others' weddings. Indeed, their bond was special.
Although David knew that Bob suffered from kidney disease, he did not know what the cause was or much about Bob's condition. He did know that Bob had received a kidney from his brother. Unbeknownst to Bob, David had spoken with a urologist friend about donating one of his kidneys to his friend.
Thirteen years later, David got a phone call from Bob. During the course of the conversation, Bob told him that he needed another kidney transplant. At that moment, without a second’s hesitation, David said, "I’ll give you one." Bob said that he appreciated his friend's quick and generous response but that this was something David really needed to think about and discuss with Jamie, his wife. David replied that he had been thinking about it for 13 years. He related the story of his conversation with the urologist many years earlier. Bob consented to David being screened to be his donor. David also said that his wife, Jamie, loves Bob and had also immediately said "you got to do it."
The screening process began and Bob and David proved that they were indeed an incredible match. "Are you sure you’re not related?" the doctor who performed the screening test asked. Amazingly, Bob and David had the same match score as Bob had with his brother years before.
The surgery was performed in 2010 at Mount Sinai, and although there were difficult days, their friendship, determination and shared sense of humor saw them through.
For David, being a living donor for his friend was one of the greatest experiences of his life. "It was one of the best things I have ever done in my life — without equivocation. Other than my wife and my kids – to be able to step up and help a friend was incredible."
Dr. Juan Rocca, Surgical Director of the Live Donor Kidney Transplantation Program, and his team were incredible, David said, "I think the world of Dr. Rocca and my anesthesiologist. It’s my pleasure to support this program and these doctors in any way I can."
In the summer of 2011, more than 30 years after meeting and one year after David donated one of his kidneys to Bob, the two celebrated their friendship with a hiking trip in Colorado. They are pictured below at the summit of Mount Lincoln at 14,293 feet.
Saving “the Big Sister I Never Had"

For Jennifer, it was the most difficult call of her life: asking her perfectly healthy younger cousin, Nina, to consider donating part of her liver. With the odds of finding a deceased donor against her, and time running out – after wrestling with the decision for two days – she picked up the phone and dialed.
After choking back tears, she finally asked. For Nina though, it was never really a question. “Absolutely,” she told her cousin. Jennifer again started crying. “She said thank you a million times,” Nina would later recount, several weeks post surgery.
Once she said yes, “I knew it was guaranteed I was going to live,” Jennifer would later tell the North Jersey Record, in a profile of the cousins. “But [at the same time], I felt horrible because I … just didn’t want her to have to go through all this.”
For living donors, liver transplants can be especially involved, requiring major abdominal surgery, months of recovery and a life long scar. For that reason, the procedure is somewhat uncommon. According to the Health Resources and Services Administration, only 247 out of 6,342 liver transplants performed in 2011 were from living donors.
For recipients though, receiving a liver from a living donor offers a new lease on life, freeing them from the otherwise long wait for the right deceased donor’s organ to become available.
A month after Jennifer’s call, Nina went in for the screening, which included a physical, blood tests, and imaging to ensure her liver was large enough. While initially she didn’t have any real doubts, upon learning she was a match reality began to set in. Given the risks, New York State law requires donors to take two weeks before committing to the decision.
“During my two week cool down period, I was fluctuating back and forth,” Nina would later confess. “It was a life changing decision on my part. It was a toss-up.” In the end though, she decided the chance to save her cousin’s life was worth it. “She’s my cousin; she’s my family and I love her,” she says.
On July 31, the cousins went for surgery. Ever upbeat, Nina joked with the doctors and nurses right up to receiving anesthesia. After coming through, her support team was still by her side. “Everyone in the hospital was absolutely awesome. Dr. Facciuto was awesome. He’s funny. He came to see me and would always look at the incision. Tara my coordinator was the same way. The nurses were absolutely excellent. … Everyone was great, so nice and caring. They treated you with respect, like you’re a person and not a thing.” Jennifer shared similar sentiments.
After a week in the hospital, Nina got to go home. A month later, she started feeling more like her old self, but it would still be a few more weeks before she could get back to work -- or back to what she looked forward to most: hitting the gym.
Jennifer’s recovery has also been strong. “My eyes are white. My skin is clear. It’s just amazing,” she said. Though still on oxygen for a related condition, in time she should be able to come off that too. With further improvement, she’s most looking forward to getting back to gardening – and hopefully becoming a mom.
As much as the experience brought Jennifer and Nina closer together, and for all their appreciation of how it saved Jennifer’s life, both stressed that perhaps the most important part of living donation is that it saves not just one life – but two.
“Because of her doing what she did, now somebody else can have the liver that [would have gone] to me,” Jennifer stressed. Of Nina: “We’re all very proud of her.”
“[Living donation] gives you an opportunity to do something that not everyone has a chance to do,” Nina said. “You have an opportunity to find out what kind of person you are. You are saving multiple people’s lives – you’re saving not just one, but two lives at least.”
A Gift Between Friends

Although Harold Engel had been diagnosed with polycystic kidney disease in his twenties, it wasn't until 2010 that his creatinine level was found to be dangerously high and the related decline in his kidney function began to take its toll. A New Jersey husband and father, and president of the advocacy group The Rights of the Child, which maintains orphanages in Thailand, Engel had always been an active person, who slept only four hours each night and traveled constantly. But as his kidney function worsened he started sleeping twenty hours each day and feeling physically drained and emotionally depressed. As the possibility of dialysis began looming larger, a string of relatives and friends—including his wife and sister—were tested as candidates to donate a kidney, but no one was a match.
“Then,” Engel remembers, “along came Angela.”
Angela Diaz, MD, MPH, Director of the Mount Sinai Adolescent Health Center, had done her pediatric residency at Mount Sinai with Engel's wife, Paula Elbirt, MD, and the two friends had remained close for over thirty years. As a result, Dr. Diaz had long been aware of Engel's declining health, and one night in the spring of 2012, during an ordinary phone call, she asked how he was doing.
“I knew he was going through a clearance for transplant so at the end of the conversation I asked where things were,” Dr. Diaz remembers. Upon hearing of Engels' dwindling options, Dr. Diaz responded with an amazing, spur-of-the-moment offer: “I said I would be tested and if I was a match, I would donate.”
"Engel was moved beyond words with gratitude and hope, and after subsequent conversations Dr. Diaz began the thorough process of being evaluated as a potential kidney donor. Unfortunately a very strong family history of diabetes—including her mother and a hemoglobin A1c at a level that made the surgical team uncomfortable about moving forward—meant that Dr. Diaz was an unsuitable candidate. When she shared this news with her then 30-year-old son, he replied that he would like to be considered as a possible donor. But Dr. Diaz was undeterred: She made lifestyle changes such as diet modifications and increased exercise to bring her levels within a healthier range, and re-testing a month later revealed that she was now able to donate. With the clearance official, arrangements moved very quickly, and the surgery date was set for July 24.
Asked why he thinks Dr. Diaz showed such tenacious follow-through in order to give him such a gift, Engel admits his inability to find words that would do justice to her kindness. “You don't ask ‘why' because there is no ‘why'—I have no way to express it,” he says. “Someone once told me the only reason God gave you two kidneys was to teach you to be generous. And I suppose that's true.”
The Turning Point
Engel vividly remembers arriving at Mount Sinai at the “ungodly hour” of 5:30 am on the morning of surgery. His wife and Dr. Diaz's three children and ex-husband also came and waited nervously through the pair of operations that were made longer due to complications from an underlying hernia condition that had been troubling Engel for years. But in the care of highly skilled surgeons, within five hours Dr. Diaz then Engel emerged from the OR after the successful completion of their procedures.
While Engel and Dr. Diaz were recovering in adjacent hospital rooms, their relieved families started ping-ponging back and forth between them sharing hugs, food, and updates. Then came one of the most joyous moments of Engel's journey: “About 48 hours after surgery, my creatinine level went from 8.1 to 1.8,” he says. “It's amazing how quickly the body cures itself.”
“Yes, that kidney was working right away,” Dr. Diaz adds. “It just took off.”
Dr. Diaz was feeling so well after her procedure, she was in the hospital for only one night and returned to work two days later—and on the way home from work she visited Engel in the hospital. Engel, dealing with significant pain from the hernia portion of his procedure, stayed for 8-9 days, but he is grateful for the staff that helped him through. “I had a great relationship with everyone at Mount Sinai,” he says. “It was a really wonderful experience.”
Looking Ahead
Dr. Diaz's generosity that year didn't end with the donation of her kidney. As director of the Mount Sinai Adolescent Health Center, which offers free care to young people between the ages of 10 and 24, she is tirelessly searching for money to provide services to the 12,000 patients they serve every year. Since 2010, she has been running the New York City Marathon to raise funds, and as soon as her surgeon cleared her after transplant surgery that August, she started training for the 2012 race. Although it was cancelled due to Hurricane Sandy, Dr. Diaz was pleased to run the 2013 marathon along with other team members from Mount Sinai and the community, and to raise almost $80,000.
Today Dr. Diaz continues to benefit from the healthy lifestyle changes she adopted in preparation for surgery, and she is very gratified by the transplantation experience itself. “It's just wonderful to see Harold the way he is now—he's doing well, he's traveling again, and he's full of life.” Plus, Dr. Diaz adds another observation. “It's interesting—he's a Jewish man from Europe, and I'm from the Caribbean, so our ancestry is quite diverse. But as it turned out, I was a closer match than even his sister. So I think it was very special to be able to do this.”
In return, Harold's gratitude is so enthusiastic that he surprised Dr. Diaz with a testament to her generosity at a holiday party: a tattoo on his hand of a heart with the initials “A” and “D” for the friend who saved his life.
“This entire experience has been phenomenal—better than any roller coaster ride you've ever been on,” Engel says. “And I wonder if everything worked out because life has a bigger purpose for me than it did in the past. I mean, Angela has devoted her life to the welfare of kids, and now I'm more devoted than ever to my work for children. And since the surgery we have such a bond—because now, every morning when I wake up, it's thanks to Angela.”
Arriving at the Right Place, with the Right Doctor

Edwin Rivera was 40 years-old in 2007 when he learned that he had familial polyposis coli, or FAP, a hereditary colorectal cancer syndrome associated with the development of hundreds to thousands of polyps in the large intestine (colon) and rectum – polyps that could become cancerous. He said the doctor who gave him the diagnosis never really explained what the condition was. Over the next several years, he had three surgeries to remove the polyps.
After his last surgery, Edwin was given a clean bill of health and told by his physician that everything would be fine. Yet his medical problems persisted. As the days and months dragged on, he became increasingly angry about his condition. But he did not know where to turn. In May 2010, he was admitted to the emergency room at Mount Sinai a very sick man. Tests revealed that he had multiple polyps typical of FAP’s progression. He says his previous physician never told him that the tumors would indeed return and multiply and that he needed to have X-rays regularly performed.
Edwin says his life changed dramatically when he was introduced to Dr. Kishore Iyer, Surgical Director of the Recanati/Miller Transplantation Institute’s Intestinal Rehabilitation and Transplantation Program. At their meeting, described by Edwin as a deep, honest conversation, Dr. Iyer told Edwin that his case was challenging. He said he needed an intestinal transplant and that the surgery would be complicated. But Dr Iyer also told him in no uncertain terms, “I will take your case, and I will see it through.” A spiritual man, Edwin knew that he had finally arrived “at the right place, with the right doctor and that this was the right time.” He told Dr Iyer that we will get through the transplant procedure “together.” And together they have.
Today, Edwin is enjoying good health and a full, active life with his family. He is grateful to Dr. Iyer and Mount Sinai for giving him "a second chance at life."
A Man Honored for Improving the Lives of Many New Yorkers Credits Mount Sinai

By the time Paul Navarro had his kidney transplant at Mount Sinai in 1998 at the age of 48, he had already had a long and distinguished career as a public servant and community activist in New York City. Despite struggling with chronic high blood pressure and being on dialysis for kidney failure in the early 1990s, Paul had continued his community service, receiving numerous accolades for his work along the way. But it was the kidney transplant he received at Mount Sinai that enabled him to “operate at a different speed” and do his best work in the years that followed, he said.
Born and raised in the South Bronx, Paul began his career in the 1980s as a community activist aspiring to end the urban blight and poverty in the neighborhoods he’d grown up in. He worked on local governing boards to renovate the derelict buildings of the South Bronx and improve the quality of its neighborhoods. He later joined the Koch administration’s Division of Labor Services monitoring equal employment opportunities and prevailing wage rates in the construction industry. He then moved on to help tenants with rent and repair issues in the City’s Department of Housing Preservation and Development (HPD).
In 2006, he was awarded the prestigious Isaac Lieberman Award for outstanding public service by New York City’s Police Commissioner Raymond Kelly. In June 2009, New York Congressman Charles Rangel on the floor of the U.S. House of Representatives paid special tribute to Paul, calling him a “a courageous New Yorker and exceptional human being, for his commitment, and tireless efforts, in improving the lives of so many…”
Unfortunately, around the same time, Paul began to show symptoms of chronic kidney rejection, and in 2009, he returned to dialysis in New Jersey where he now lives. Although he was forced to retire due to his poor health, he was eager to be listed for transplant.
One Saturday afternoon in June 2012, while celebrating his heritage and enjoying the Puerto Rican Day parade with his family (he has two daughters, six grandchildren and four great grandchildren) Paul received a call from Mount Sinai informing him a kidney that was a good match had become available for transplant. He hurried to the hospital and the transplant operation was performed successfully.
From his room at Mount Sinai, he said, “Mount Sinai is my hospital. Going to Mount Sinai so many years ago was the best decision I have made. I have great, great doctors and I am improving everyday!”
Kidney Donation: Sister to Sister
Davinya Avery looks both younger and older than her 30 years. Younger, when she’s joking and laughing with her sister and kidney donor, Damitra Avery-Parker; older, when she’s talking about the monthly doctor visits she has endured since she was diagnosed at 19 with glomerulonephritis, a chronic kidney disease.
“I used to get a physical once a year so I could play sports in high school,” Davinya says. “Then after I was diagnosed, it was doctor’s visits every month, sometimes every two weeks, constant blood work, medication, hospitalization.” Just speaking about the grueling regimen seems to tire her out. “A lot of stuff hit me all at one time,” she says. Damitra nods her head in silent support.
As soon as she was diagnosed, Davinya’s three sisters volunteered to become donors. Yet she waited 10 years before going through with it. “At first, I was scared,” she admits. “But as time passed, I knew I wanted to marry and have children—to move on with my life.”
All three sisters were tested, and two came back as a match. Damitra—the oldest sister, and a mother of three—settled the question of who would be the donor with the same pragmatic, irrefutable logic that a big sister might use to stake her claim to ride in the front seat of the car. “”I’m the oldest, I’ll go,” she said.
Less than six months later—after a whirlwind of MRIs, ultrasounds, blood work, nutrition work, as the RMTI team prepared both sisters for what to expect—the two surgeries took place in March 2012. (Davinya’s surgeon was Michael J. Goldstein, MD, Surgical Director of Kidney Transplantation; Damitra’s was Juan Rocca, MD, Surgical Director of Live Donor Kidney Transplantation.)
Two weeks after the surgery, both sisters were recovering well. “I thank Damitra every day from the bottom of my heart,” she says, turning to her sister. “It’s a powerful thing. I want to thank you for giving me a second chance.”
Davinya shrugs off the notion that she did anything special. “I would do it again,” she says. “I would never second-guess my choice.”
A Four-Year-Old Girl Resumes Her Active Life with Cousin’s Liver

Madison Blumenthal was a typical preschooler – picking up common illnesses during her childhood but otherwise healthy. However, one Monday morning when her babysitter picked her up from preschool, Madison’s teacher commented that Madison had been sleeping an unusual amount during the day. For the next two days her lethargy continued until her mother Michelle Rodriquez insisted that she take a shower. Out of pure exhaustion, Madison urinated in the shower and her mom saw that her urine was the color of rust.
At the doctor’s office that afternoon, Madison’s examination was unremarkable. Just when the doctor stepped out of the office, Madison’s eyes shifted as she looked peripherally at a cartoon on the wall. That was what mom described as her “oh, no” moment, as she saw the yellowing in the corners of her daughter’s eyes. She called the doctor back in and from there things moved incredibly fast.
Madison was admitted to the hospital and tests began. By the next morning, she was going into liver failure and was transferred to the intensive care unit. Her mother was told that Madison needed a liver transplant and that she had acute hepatitis and liver disease. Although her mom immediately volunteered to donate a portion of her liver, she did not qualify as a donor. Madison was listed on the organ transplant waiting list. The hope was that her condition would stabilize in time for a liver donor to be found.
Within a few days, her condition had rapidly worsened. Friends and family started calling and coming in to be screened as potential donors. Miraculously, of the five relatives visiting one day, three were a match. Based on her overall health, one cousin, Katherine Franco, was chosen to be the donor. Mom reassured her cousin that she didn’t have to do this. But Katherine insisted that she wanted to make this difference.
Co-Workers' Bond of Friendship Grows Through Living Donation

Teresa Ferreri knew she wanted to be an organ donor. She just assumed she would become one upon her death. But life often takes mysterious turns.
Teresa met Christine Stile-Mazzeo at work. They immediately felt a special connection and became close friends. It was only natural that Teresa was very concerned when she learned that Christine had a chronic kidney disorder known as polycystic kidney disease (PKD), a genetic disorder that often leads to kidney failure.
One day in 2007, Christine’s doctor informed her that her condition was deteriorating and that, in time, she would need to start either dialysis or receive a kidney transplant. When Christine told Teresa of this, Teresa asked Christine if she could be considered as her potential living kidney donor. Christine was overwhelmed by her friend’s generous offer. Very soon afterward, they both came to Mount Sinai for organ transplant testing and evaluation. Teresa had the full support of her family in her desire to become a living donor for her friend.
On Good Friday, which as a Catholic, Teresa believed was truly a sign, a transplant coordinator at Mount Sinai informed her that the test results indicated she was a good transplant match for Christine, and that she could move forward with the donation. When Teresa called to share the good news with her friend, Christine’s husband answered and was elated by the news. He asked Teresa to call his wife on her cell phone to let her know. Christine was in the grocery store shopping for Easter Sunday dinner when Teresa reached her.
On December 29, 2009, Teresa donated one of her kidneys to Christine. The special bond they shared has since multiplied in ways they never imagined. Teresa now loves getting text messages and emails from Christine because they are filled with details of her very active life -- a life that would never have been possible without Teresa’s living donation.
“It is so hard to express how fulfilling this experience has been. I am often overcome with emotion when I hear how active Christine is with her family, her husband’s business and keeping her home,” Teresa said. “Being a donor and being able to help someone I love like a sister has definitely been the WOW experience of my life!”
A Gift of Life for the Tiniest of Patients
Born with a rare, life-threatening liver disease, Ariz Gadit received a life-saving liver transplant at Mount Sinai in 2011 when he was less than a month old and weighed less than seven pounds. Today, he is thriving.
When Ariz Gadit was born in October 2011, he seemed like a healthy baby. But a routine test showed that little Ariz had low blood sugar and a low blood platelet count. Further testing revealed that he had neonatal hemochromatosis, a rare and often fatal liver disease that causes “iron overload,” or toxic amounts of iron to build up in a baby’s body. When several treatments failed, his parents Samreen and Hussain Gadit turned to the liver transplant specialists at Mount Sinai Medical Center’s Recanati/Miller Transplantation Institute (RMTI) to save their son’s life.
Ariz’ dad Hussain begged the team at RMTI to let him donate to his son. However, Ariz was only three weeks old and needed a smaller-size donor liver. If someone living were to donate, they had to weigh less than 120 pounds. No one in their family met those requirements.
Unexpectedly, a donor liver, from a deceased infant, became available within a matter of days. As Dr. Sander Florman explains in the video, “A Life-Saving Liver Transplant: Baby Ariz,” this surgery was particularly challenging given Ariz’s age and size (less than a month old and only seven pounds). But the liver transplant was successful. “Only one or two liver transplant surgeries are done a year in the United States on babies less than two months of age,” says Dr. Florman, who is Director of the Recanati/Miller Transplantation Institute at Mount Sinai and who performed Ariz’s surgery with a team of specialists at Mount Sinai. Ariz is now growing fast. He is healthy and energetic and enjoying the simple pleasures of everyday life with his two brothers.
The Pediatric Liver Transplant Program at Mount Sinai is one of the largest and most successful in the United States. The first pediatric living-related liver transplant and the first pediatric liver/intestinal transplant in New York State were performed at Mount Sinai. We provide comprehensive, multidisciplinary care, before, during, and after transplantation. In addition, we offer comprehensive counseling and medical care to people considering living donation through the Zweig Family Center for Living Donation, which is part of RMTI. The Zweig Family Center for Living Donation is one of the largest living donor programs in the United States.
For the Win: When a Daughter Saves Her Mother’s Life
When Roberta Gorman first told her daughter that she had been diagnosed with primary biliary cirrhosis and needed a liver transplant, 19-year-old Sammi Gorman was on a team bus on her way back to Fitchburg State University, where she was a sophomore, from a lacrosse game. Night was falling and the two were talking by cell phone. “I sat there and was like, ‘I could help you,’” Sammi says, recalling the conversation. Roberta, who goes by Bobbi with her family, dismissed the idea out of hand. She had five brothers and sisters, a husband and older son; certainly one of them would be a possible donor.
“You’re supposed to be taking care of your kid, not your kid taking care of you,” she explains. Plus, Sammi was too young; liver living donors typically need to be at least 21. For all of those reasons, even when Sammi persisted, “We kept telling her no,” Bobbi says.
But over the subsequent months, as family members were one-by-one disqualified as possible donors, Bobbi’s condition deteriorated significantly. Not one to watch from the sidelines, Sammi pleaded to get evaluated. For Bobbi and her husband, Barry, it was an agonizing decision. “Do we want to [let Sam] do this, or don’t we? What if the end results aren’t good? What if something happens?” Bobbi recalls.
Sammi thought about it differently: “The entire time, I felt pretty confident that everything was going to be fine. Where my mom thought she was putting her daughter in danger, I thought: I’m healthy; I’m going to bounce back and my liver is going to grow back.” There were more sentimental considerations as well: “I know it sounds corny, but I’m about to head into the adult world. I still need my mom.” She laughs.
For Bobbi, it would ultimately take a conversation with her physician, Leona Kim-Schluger, MD, associate director of the Recanati/Miller Transplantation Institute at Mount Sinai, to get her to feel comfortable with Sammi’s decision to become her donor. “Dr. Kim said something very important: ‘As a mother, I understand your feelings, and I would say no in a heartbeat as a parent. But as a person, you can’t take this away from her.’” The advice resonated. This was something her daughter wanted to do. That drive was part of who she was. Thus, with tremendous trepidation, Bobbi agreed.
Evaluation, Surgery, and Recovery
Sammi underwent the evaluation in November 2011. She remembers finding out she was a qualified match shortly afterwards vividly: “I was walking down the [dormitory] hall, when I got the call,” Sammi says. Her transplant coordinator told her the news. “I was like, ‘So wait, I’m a match?’” She was thrilled. “My friends were all jumping out into the hallway and hugging me and getting all excited. It was a very exciting day.”
The seriousness of the situation didn’t fully sink in for Sammi until a day after returning home from finals. That morning, Sammi woke up to find Bobbi unresponsive. An ambulance rushed her to the ER, where she was admitted to the ICU. Although they had hoped to schedule surgery for after the spring semester when it would it be least disruptive to Sammi’s studies, it was becoming clear that there wasn’t time to waste.
Surgery was scheduled for February 7, 2012. It was a “textbook” case, Sammi says. For mom and daughter, it couldn’t have gone more smoothly.
Bobbi was never so excited to see her daughter as after surgery. “When they wheeled her in, if I hadn’t been so groggy, I would have jumped up and down,” she says. “She came over and hugged me. The people behind her were all crying. But she was smiling. She was in her glory.” She looked like an “angel” Bobbi adds, and confesses that even a year later, she still dwells on that memory often.
For Sammi, the first thing she noticed upon seeing her mother was how much her complexion improved; second, was how much more like her old self she was. “A complete 180, it was amazing. I didn’t expect, in all honesty, to see results that quickly,” Sammi says. She told her mom how good she looked. Bobbi, with spirits clearly improving, quipped: “I didn’t think I looked that bad before.”
Last fall, Sammi returned to Fitchburg State University, where she resumed her studies towards a degree in communications media, as well as lacrosse. She also started a charity, Endless Cradle, through which she is working to raise awareness and funds for liver disease treatment and research. When she graduates next week—on-time with honors, despite the semester she took off for surgery—most of her classmates will see the occasion as a milestone connoting their passage to full adulthood. Whether Sammi realizes it or not, it’s a transition she made already.
“The whole thing has definitely changed my life,” Sammi says. “It has shown me a side of things that I hadn’t seen before and allows me to put things in perspective. And I’m very glad that everything worked out. Those first minutes of seeing my mom with her color was like having my mom back. That was the most rewarding thing of all. I was like ‘she’s back!’”
Kidney Transplantations Foster Bright Hopes

In August 2011, Michael J. Goldstein, MD, Director of Kidney and Pancreas Transplantation, and Associate Professor of Surgery, performed life-saving transplants on two 13-year-old girls who each received a kidney from the same donor on the same day at The Mount Sinai Hospital.
Today, the girls, Lizbeth Irizarry and Joseline De Los Santos – eighth graders who enjoy math and dancing to pop songs by Lady Gaga and Rihanna – share their hopes for the future as well.
Prior to receiving her kidney, “Lizbeth was on dialysis for 18 months,” says her mother, Claudia Irizarry. “It felt as though our lives had stopped. Now we are going back to normal. I feel like I have my baby back.”
Organ donation from a living relative is the best way for children to receive timely kidney transplants, according to Dr. Goldstein. But that was not possible for Jocelin or Lizbeth, who waited for kidneys from deceased donors through the United Network for Organ Sharing. Read full story
The Gift of Reading Leads to the Gift of Life

An avid reader, Tom Naylor had always been a fan of author and cultural critic Virginia Postrel. In 2005, while reading her blog, he discovered that Postrel was going to donate one of her kidneys to a fellow author, Sally Satel. Virginia Postrel’s description of this experience and her friend’s challenges living with kidney failure touched him deeply.
Tom had no friend or loved one who needed his kidney. But he knew there were countless other people’s loved ones suffering with kidney failure whose lives could be vastly improved if they were lucky enough to get a kidney transplant. At that moment, Tom Naylor decided to be an altruistic donor.
Altrustic donation (seeking to donate to a stranger) was still a new concept to many transplant programs and few were equipped to assist Tom in pursuing this selfless gift. Tom learned about the living donor transplant program at Mount Sinai‘s Recanati/Miller Transplantation Institute from a friend who had a family member being treated at Mount Sinai. He contacted the Zweig Family Center for Living Donation at RMTI. He was impressed by the knowledge, the care and the attentiveness of the staff. He eventually was able to realize his goal and donate.
On April 4, 2011, five years after reading Virgina Postrel’s blog, Tom Naylor donated a kidney to someone he had never met before. Before he left the hospital, Tom briefly met the recipient of his kidney – a 34-year-old man. He was glad to know the surgery went well but does not need to know more, he says. Tom is content that he fulfilled his objective of helping another human being through living donation and feels a tremendous amount of satisfaction in doing so.
An Intestinal Transplant Recipient's Mission to Help Others Like Her

In 2008 Noa Walsky was in the best shape of her life, but something felt off. Now and then, she felt a lump in her belly that she affectionately called “her grapefruit.” Because it wasn't always noticeable, she didn't worry much about it. But six months later, she felt it again, and her parents—a surgeon and nurse— also felt the lump.
An MRI revealed a desmoid tumor in June 2009. Desmoid tumors develop in the body's fibrous tissue and can become very large. They are considered benign because they don't metastasize like cancerous tumors do, but they can cause serious damage to internal organs because they often attack adjacent muscle tissue.
Noa’s tumor had to be removed – but in order to do so, surgeons needed to remove her entire small bowel. As a result, Noa needed to receive an intestinal transplant and was placed on the national wait list. In December 2009,she received her transplant at Mount Sinai Medical Center.
Noa requires a lifetime of follow-up care to make sure her body doesn't reject her new intestines. While she was tremendously grateful for the gift of transplantation – Noa had to cope with the stress of maintaining the high costs of staying healthy. She was out of work for long periods of time, and the cost of her medications was exorbitant.
Last November, Noa (pictured above, 2nd from the right) turned 30. She chose to celebrate her birthday and her transplant by helping others. She contacted the National Foundation for Transplants (NFT) to see how she could help other small bowel transplant patients. This call led to the creation of the NFT's Small Bowel Fund. She asked her friends to make a donation to this fund in lieu of giving her a birthday gift. About 50 people attended the party, raising nearly $6,000. Noa has relied on the help of her family and friends during her long recovery process, and she's grateful for their support. She wanted to begin this fund to help others who may not have the same kind of support system. And she has done just that. To contribute to this fund please contact the NFT.
Newborn Receives Living Donor Partial Liver Transplant, Happy and Healthy 10 Years Later

Adalyn was diagnosed with a choledochal cyst, a developmental condition in newborns, where the common bile duct between the liver and the small intestine is blocked, resulting in liver damage. Despite all efforts to save her liver, she became so sick that the only remaining option was a liver transplant. She underwent a successful living donor partial liver transplant at Mount Sinai when she was 10 months old. Her mom, Annette, was her donor.
Adalyn is now 10 years old. She is very happy, healthy, and adventurous. She enjoys skateboarding, surfing, and rollerblading with her three sisters Angelia, Avraelle, and Aylexis. She has achieved a brown belt in karate and loves to shoot hoops, swim, and travel. Indoors, she loves to draw, paint, and build with Legos.
Adalyn was nicknamed “boo” by her father, Yuan, because when she used to cry she would hold her breath and puff out her cheeks and release a sound like “boo.” Now Boo no longer sheds few tears and has been living a happy and active life.
We are partners in this journey

Sam Goldman appears to be a happy and bright "typical" 14-year old. He is a soccer enthusiast; he "loves, loves, loves" the Yankees; he enjoys watching the Discovery Channel; and he wants to be a geologist when he grows up.
One would never guess that Sam has travelled a rough road to get to this point. At age 6, Sam was diagnosed with primary sclerosing cholingitis—a chronic inflammatory disorder of the bile ducts. By age 13, this condition irreversibly damaged his liver and Sam began to feel very weak and debilitated.
Instead of experiencing a special summer trip to Italy with his mom, Lisa, he was preparing for a life-saving liver transplant. Lisa wanted to be Sam's living donor.
On August 3rd, 2010, Lisa donated a piece of her liver to her son. As she says: "We are partners in this journey."
Mount Sinai's Recanati/Miller Transplantation Institute has partnered with more than 5,500 patients like Sam, whose life depends on a new liver, pancreas, or kidney. And our continuum of care philosophy means we are there for you and your loved one before, during, and after the surgery to ensure your wellbeing.
A few months following surgery, Lisa was back to her exercise regime of biking and hot yoga. And Sam is now back to routing for his beloved Yankees, some of whom he recently met.
Both are looking forward to their rescheduled summer trip Italy in 2011. And both have their eye on the ball of a bright future together.
Find out more about how you can save a live by becoming an organ donor.
A Brother's Living Kidney Donation Enables His Sister to Continue Outstanding Community Service

Soon after the birth of her daughter Rebecca in 1985, Ellen Skolnick was diagnosed with the connective tissue disease, "Diffuse Scleroderma." Holding her newborn was nearly impossible due to the swollen joints and daily nausea and vomiting caused by this disease. Scleroderma eventually destroyed her kidneys. By the time Rebecca was three years old, Ellen required life-sustaining kidney dialysis treatments.
In 1992, Ellen received her first kidney transplant from a deceased donor. For many years she enjoyed a feeling of wellness and independence from dialysis. When Ellen's transplanted kidney stopped working, it was her younger brother, David, who volunteered to give her one of his kidneys.
"Every anniversary of my transplant I send a "thank you" lunch to the kidney staff. These kidneys were my gift, but all of the staff at Mount Sinai enabled me to get it and keep it. I always send my brother a delivery of bagels and lox from Barney Greengrass on "our anniversary," and my family in New Mexico celebrates together!"
Today, Ellen continues to visit dialysis patients and provide information and hope about transplantation, as she has done for more than two decades. She is the team captain and a major fundraiser for the annual National Kidney Foundation Walk. In 2011, she received the "Humanitarian of the Year" Award from the American Kidney Fund for all of her community service and outreach efforts.
Ill Toddler Grows Up Healthy with Mother’s Liver

Robbie Stratakos was an active, healthy toddler until one day in March 2002, when his skin suddenly turned yellow. His parents, Allison and Peter, brought him immediately to the doctor.
Robbie was diagnosed with fulminant liver failure. An unknown virus had permanently damaged Robbie’s liver. The toddler urgently needed a life-saving liver transplant.
It took two days for Allison to be evaluated and cleared as Robbie’s living donor. The liver transplant surgery took place just four days after Robbie was diagnosed.
"Robbie is now a healthy, normal 11 year old," Allison said. "He loves to play the drums. He excels at sports. And he wants to be a professional golfer. We are back to being the three musketeers — four if you count our beloved puppy, Frosty!
Now that Robbie is getting older, he is starting to understand how fortunate and special he is, she said. "We as a family want to help educate the public about the importance of organ donation.
"Everybody gives all of the credit for getting through the transplant to Robbie and me, but I feel that my husband, Peter, had the toughest job of all. He had to sit by waiting while the two people he loved the most were in the operating room. He kept our world together throughout the entire process. He is our hero," Allison said.
Desire to Donate Spurs Lifestyle Change

At age 14, Tatiana Caceres was diagnosed with Lupus — an autoimmune disease that caused tremendous pain in her joints and legs. Eventually the disease attacked her kidneys, and Tatiana became dependent on a kidney machine three-times-a-week to survive.
Tatiana needed to find a kidney donor. Her mother and siblings were tested but ruled out medically. Carlos, her father, was a good match — but doctors said he would need to lose weight and get his blood pressure under control before he could be cleared as a living donor.
Carlos was determined. He changed his diet and took long walks with his dogs. After 8 months, he had lost more than 40 lbs and was cleared to donate.
Tatiana was 32 when she had her living donor kidney transplant,. She now teaches first grade at PS 97 in Queens, N.Y. She shows her students the "battle wounds" from dialysis on her arms and hopes she conveys the importance of resilience, gratitude and family love.
"It was painful to pick Tatiana up from dialysis," Carlos said. She would say, ‘Poppy I can’t do this anymore.’ To see her so happy makes me happy…I felt peaceful for donating."
Dual Organ Transplant Saves Man Whose Brother Died of Same Disease

John McGowan had known for a long time about his diagnosis of hemochromatosis — a disorder that interferes with the body’s ability to absorb iron and can sometimes lead to organ failure. John’s brother Eugene had succumbed to the same illness.
Over time, John’s liver and kidney function deteriorated. He became so ill that doctors felt he would need a dual liver-kidney transplant in order to survive. John was placed on the transplant list at Mount Sinai and within four days received three calls regarding potential organ donors. The third call was "the call" that gave him his new lease on life. John, an attorney, returned to work just one month after the transplant surgery.
Thanks to an organ donor, John and his wife, Peggy, can enjoy their daughter Caroline’s upcoming high school graduation and celebrate many more milestones together. John’s donor is always in his thoughts. He writes a thank you letter to his donor family every year around his "second birthday," the day he received his transplant.
"Having a second chance at life changes how you think about the gift of life, John said. "Your family, friends, job, and yourself — enjoy them every day, because no one knows what tomorrow will bring."
Baby Girl Receives Part of Her Father’s Liver

"We were absolutely shocked with this diagnosis," said Lia’s mother, Carolina. "Our lives were turned upside down."
Doctors attempted to delay the need for transplant with the surgical "Kasai procedure" — a way to bypass the blocked bile ducts. However, it was clear that Lia would still need a liver transplant in order to survive. The months leading up to the transplant were very difficult, and Lia required frequent and lengthy hospital stays.
Lia’s father,Kevin, wanted desperately to be the donor for his daughter. After an extensive evaluation — he got his wish. Lia was 1 year and 7 months old when she received her liver transplant.
"January 20, 2009, will forever be the greatest day of my life," Kevin said.
"Lia has kept that same feisty spirit that helped her when she was ill," Carolina said. "She has grown up so much in the past few months. She loves to do everything with her 5-year-old brother, Dylan. She loves music, plays the guitar with her dad, takes dance lessons and loves all babies. She is wonderful, healthy and we appreciate every minute together."
Kidney-Intestine Recipient Regains Independence

Andrea "Andi" Slover at age 63 is finally enjoying her retirement. Despite having Crohn’s disease — a chronic inflammatory disease of the intestines — for more than 40 years, Andi has lived an active life.
For 23 years she worked for the federal government and was a classification specialist for the National Guard. However, five years ago, Andi’s disease became debilitating.
"I couldn’t eat so I relied on TPN (intravenous nutrition)," Andi said. "I was very weak, I felt confined since I always had to be near a bathroom. It was awful."
After many surgeries that failed to help, Andi lost hope of having a higher quality of life. But after meeting with the intestinal transplant team at The Recanati/Miller Transplant Institute (RMTI), Andi, her husband, Pete, and their three children decided that transplantation could give her a chance at a better life.
In the summer of 2009, Andi received a small intestine, a large intestine and a kidney transplant at The Mount Sinai Medical Center. She was the first person to receive a large intestine at Mount Sinai. This summer she plans on enjoying fresh fruits, babysit her grandchildren and go on boating trips with her family.
"I now have my independence," Andi said. "I am enormously grateful to the Sinai team. I am going to write a letter to my donor family and thank them for giving me my independence and my life back."
