Balloon Sinuplasty at Mount Sinai
Approximately 15 percent of adults in the U.S. suffer from the debilitating symptoms of chronic sinusitis, which often include difficulty breathing, congestion, and facial pain. Far fewer, however, seek the advice of a physician. As the largest Division of Rhinology in New York City, Mount Sinai’s ear, nose, and throat surgeons are experts in a wide variety of innovative options that significantly improve the quality of life for tens of thousands of patients each year. From medical management to a variety of surgical techniques performed both in the office and operating room — including several minimally invasive options — our specialists partner with patients to develop an individualized treatment plan based on their unique anatomy, symptoms, procedure tolerance, and medical history.
Balloon sinuplasty is a minimally invasive endoscopic procedure that has been successful in treating chronic sinusitis for fifteen years. Commonly thought of as an angioplasty for the nose, the surgical technique opens up inflamed and blocked sinus passageways without an incision—offering numerous benefits such as faster recovery time and fewer side effects. Long-recognized as international experts in the field, our surgeons perform hundreds of balloon sinuplasty procedures each year.
About Chronic Sinusitis - How Balloon Sinuplasty Can Help
Most of us have had a runny or stuffy nose, known as acute sinusitis, at some point in our lifetime. But chronic sinusitis occurs when the sinuses passages — four pairs of hollow cavities in the nose and head — swell and are unable to properly drain for a period of three months or longer. When mucus gets stuck, it causes swelling and can become infected leading to symptoms like congestion, headache, or difficulty smelling and tasting. Patients are usually candidates for surgical intervention for chronic sinusitis if they have four or more sinus infections in one year. Balloon sinuplasty provides relief by opening up these passageways, flushing the sinus and allowing the mucus to drain.
How Balloon Sinuplasty is Performed
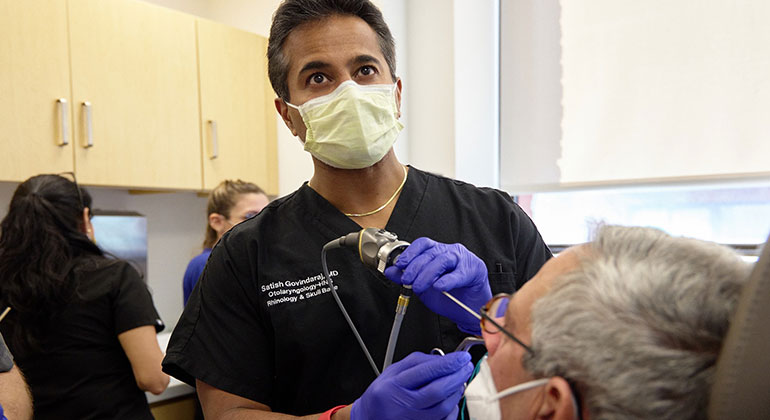
During a balloon sinuplasty, a wire or probe with an attached balloon is guided through the nasal opening into the affected sinus cavity. At Mount Sinai, surgeons use image-guided CT scans to precisely navigate these tiny instruments through the nasal passageways. When the balloon is in the correct spot, it is inflated and dilates the blocked passageway—similar to the way a stent is used to open up a clogged artery. The sinus cavity is then irrigated or flushed with salt water to allow the trapped mucus to drain out.
Read more about the advanced balloon sinuplasty navigation technology used at Mount Sinai.
Benefits of Balloon Sinuplasty
For patients who are appropriate candidates, research shows numerous advantages to having a balloon sinuplasty, compared to traditional sinus surgery. These include:
- Faster recovery time — patients report fewer missed days of work or school
- Use of local sedation rather than general anesthesia — the procedure is performed in a doctor's office rather than an operating room using numbing agents and IV sedation when necessary
- Shorter operating time — depending on how many sinus cavities are affected, the procedure typically takes one hour
- Comparable outcomes to more invasive sinus surgeries in patients with mild to moderate chronic sinusitis
- Fewer side effects including pain, soreness, and congestion — the surgery does not require an incision or any tissue or bone to be removed
- Minimal follow-up care — there is no nasal packing after the operation
Candidates for Balloon Sinuplasty
Medical management is always the best and first option for any patient experiencing chronic sinusitis. If several treatments such as oral or nasal corticosteroids and nasal saline nasal irrigation do not offer any relief, patients should consider surgical treatment.
Since we manage such a high volume of cases, Mount Sinai’s ear, nose, and throat physicians are experts in identifying the right candidates for balloon sinuplasty. Patients who have mild to moderate sinusitis, and have failed conventional therapies, typically benefit the most from the balloon sinuplasty procedure. In addition to detailed CT scans, our surgeons use a quality of life questionnaire called SNOT-22 to objectively measure the impact sinusitis has on their quality of life.
To perform the procedure, the surgeon has to be able to move the balloon freely through the opening of the nostril and into the sinus cavity. As a result, individuals with severe chronic sinusitis, or anatomical issues like nasal polyps or a severely deviated septum, often benefit from more traditional surgical approaches. Sometimes, balloon sinuplasty is performed in tandem with other techniques.
Mount Sinai’s Advantage in Balloon Sinuplasty
As a large, tertiary medical center reputable for managing complex cases, we have vast experience in treating all aspects of sinus disease. Many of our ear, nose, and throat physicians are fellowship-trained in sinus surgery and receive additional education specifically in the balloon sinuplasty procedure. With access to countless specialties across the medical center, patients can feel safe knowing there is a multidisciplinary team at every surgeon's fingertips. We also have multiple locations throughout New York City, making it easy to find care close to home. Physicians performing this procedure include:
- Dr. Daniel Alicea
- Dr. David Culang
- Dr. Anthony Del Signore
- Dr. Satish Govindaraj
- Dr. Sam Huh
- Dr. Alfred Marc Iloreta
- Dr. Isaac Namdar
- Dr. Madeleine Schaberg
- Dr. Edward Shin
- Dr. Gregory Tsai
- Dr. Benjamin Tweel
About the Procedure - Follow-up Care and Recovery Time
A balloon sinuplasty procedure causes minimal disruption to daily life—most patients return to work the next day. In an abundance of caution, we recommend that individuals who have sinus surgery do not exert themselves physically for a few days. Follow-up appointments are typically made in one to two weeks. Complications are minimal and comparable with other sinus procedures.
The overwhelming majority of patients who have balloon sinuplasty notice a significant improvement in their symptoms. The length of time individuals are expected to experience benefit depends on the severity of their disease and whether or not they have other compromising disorders such as allergies or immune system conditions. To ensure success, it is important that patients continue to take their medication regularly after surgery and properly irrigate their sinuses with nasal rinses.
Safety Protocols
Our Division of Rhinology has strict protocols in place to protect patients and staff. We have stand-alone offices for outpatient procedures that receives minimal foot traffic. Every patient is tested for COVID-19 prior to the procedure. Staff wear personal protective equipment, rooms are sterilized and cleaned after every patient, and proper social distancing practices are followed in the waiting room. Your safety is our top priority.