Conditions We Treat
The liver thrombosis team works diligently to evaluate, diagnose, treat, and manage a wide range of thrombotic disorders, including the following conditions:
Non-cirrhotic portal hypertension
Cirrhosis is scarring of the liver and poor liver function as a result of chronic liver disease. Cirrhosis can sometimes cause high blood pressure in the liver. When patients experience this high blood pressure from non-cirrhosis-related liver dysfunction, it is known as non-cirrhotic portal hypertension. The liver pathologists at Mount Sinai are national experts in making the very difficult diagnosis of non-cirrhotic portal hypertension based on liver biopsy. The condition may be of unknown cause but may also be related to certain medications, as well as collagen vascular and hematologic disorders. Two forms of the condition are nodular regenerative hyperplasia and obliterative portal venopathy.
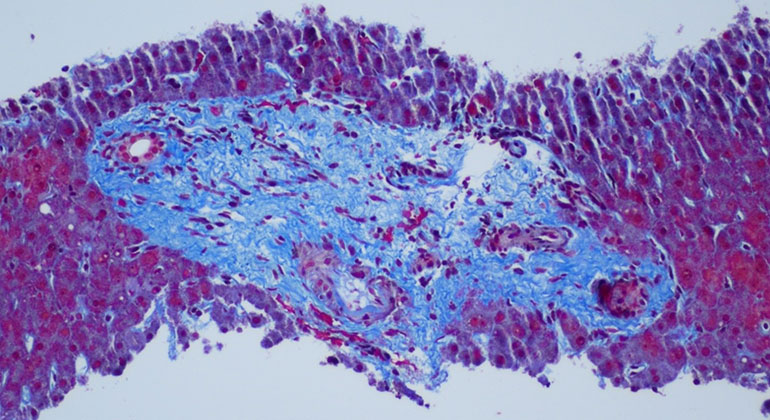
Liver biopsy showing obliterative portal venopathy. This image shows a densely fibrotic portal tract with rounded borders/portal vein lumen is totally obliterated (courtesy of MI Fiel, MD, Pathology, Icahn School of Medicine at Mount Sinai).
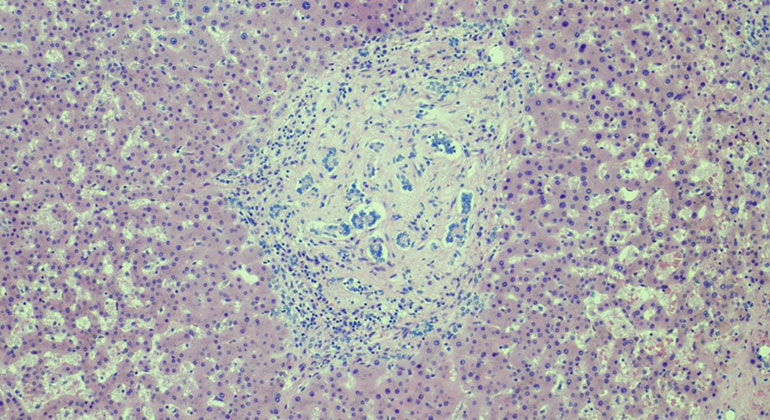
Features of nodular regenerative hyperplasia with reversed lobulation of the architecture (courtesy of MI Fiel, MD, Pathology, Icahn School of Medicine at Mount Sinai).
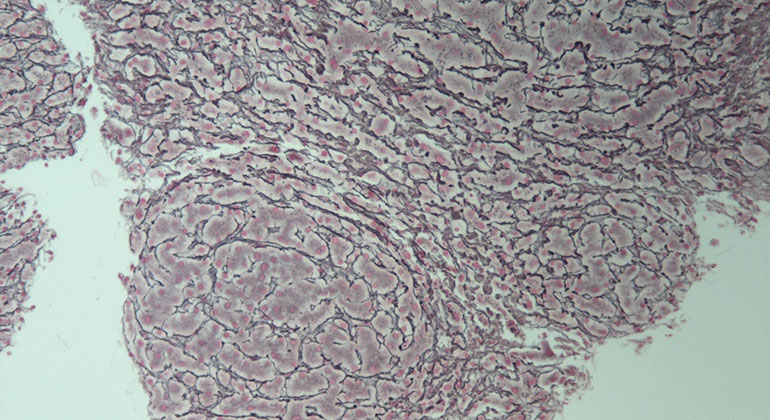
Reticulin stain of an nodular regenerative hyperplasia case showing a nodule composed of thickened cell plates and bordered by atrophic hepatocytes (courtesy of MI Fiel, MD, Pathology, Icahn School of Medicine at Mount Sinai).
Budd-Chiari syndrome
This rare liver disease is develops when the veins that drain blood from the liver are blocked or narrowed. It occurs when a clot completely or partially blocks the large veins that carry blood from the liver (hepatic veins) via the inferior vena cava and back to the heart. Without timely intervention, liver failure and the need for liver transplantation may ensue. Patients often have an underlying clotting disorder that is diagnosed by our hematology colleagues who are national experts in clotting and in the management of myeloproliferative neoplasms.
Acute and Chronic Portomesenteric thrombosis
This form of thrombosis affects the portal vein, splenic vein or superior mesenteric vein. The portal vein carries blood from the digestive organs (mouth, esophagus, stomach, small and large intestines, pancreas, gallbladder and spleen) to the liver. If blood cannot reach the liver, it can result in the patient experiencing high blood pressure in and reduced blood supply to the liver. Our highly skilled liver surgeons are sometimes able to treat portomesenteric thrombosis without a transplant, especially in children, by performing certain surgical procedures.
Refractory Portal Hypertensive Bleeding
Patients who have bleeding from varices in the esophagus and stomach which cannot be stopped by medical or endoscopic treatment need urgent intervention with transjugular intrahepatic portosystemic shunt (TIPS) or balloon- retrograde transvenous occlusion (BRTO). In the setting of a pre-existing portal vein thrombosis (portal cavernoma), our experienced interventional radiology team will be able to re-establish blood flow, and have long-standing success and excellence in performing complicated TIPS in the setting of portal vein thrombosis.
Ectopic Variceal Bleeding
Varices in unusual places, such as the small intestine, colon, rectum, mesentery, or around stomas are difficult to treat medically and endoscopically. Patients may require transjugular intrahepatic portosystemic shunt or embolization of the feeding vessels of the varices; procedures are performed by the interventional radiology team.
Mesenteric Ischemia
Mesenteric ischemia can be related to acute thrombosis either due to atherosclerotic disease, an abdominal surgical procedure, spontaneous arterial dissection, or thrombophilia. Timely management with thrombolytic therapy or stenting is necessary to prevent intestinal necrosis and loss of bowel.
Embolization of Aneurysms
Aneurysms occurring in portomesenteric and hepatic arterial vessels occur rarely, but may have catastrophic consequences. Treatment requires embolization by an experienced interventional radiology team in order to achieve an optimal result without complications.
Diagnosis and Treatment of Hypercoagulable States (Thrombophilia)
The multidisciplinary team includes hematologists who have experience in clotting and who utilize cutting-edge diagnostics in establishing the cause of underlying hypercoagulable states. This diagnosis then allows for the initiation of appropriate medical therapy to prevent further thrombosis.
Familial and Uncommon Vascular and Aneurysmal Diseases
Vascular medicine specialists will help diagnose such infrequently seen but complicated diseases. The non-invasive vascular diagnostic laboratory in the Zena and Michael A. Wiener Cardiovascular Institute at Mount Sinai performs non-invasive arterial and venous duplex ultrasonography of the abdominal vessels, including the vena cava, mesenteric arteries, and veins. Ultrasound imaging provides the multidisciplinary care team with vital information on blood flow through the arteries or veins of interest. Duplex ultrasonography is often used to monitor patients that have undergone revascularization procedures and can thus guide therapy. The exams are interpreted by our vascular medicine and vascular surgery physicians, who work in parallel for the betterment of our patients.