Evaluation of Thyroid Nodules
The initial evaluation of a newly discovered thyroid nodule begins with:
- Assessment by an endocrinologist or thyroid surgeon
- Thyroid function tests (laboratory (blood) tests)
- A thyroid ultrasound
What is a Thyroid Ultrasound?
An ultrasound is a highly accurate tool to visualize your nodule. There is no associated radiation with an ultrasound and it is non-invasive. Ultrasounds are cost-effective as most patients really do not need any other imaging because the ultrasounds are the best way to look at the thyroid, all thyroid nodules present, and the lymph nodes in the neck.
If a Thyroid Nodule is Visualized, What Next?
Typically, nodules that represent a risk of malignancy should be biopsied. That is one way to avoid over-treatment. However, all thyroid nodules do not need a biopsy. For example, nodules that appear completely black on the inside (“anechoic”) are purely cystic, or filled with fluid. The chance of cancer for a cystic nodule is essentially zero and cystic nodules do not require biopsy.
The American Thyroid Association has determined guidelines that we follow in determining if a biopsy is indicated. Findings on the ultrasound that may indicate a risk of cancer or suggest a nodule is suspicious for thyroid cancer, include:
- Nodules that do not have smooth borders
- Nodules that have little bright white spots (micro-calcifications).
If the nodule appears suspicious on ultrasound and is larger than 1 cm, the next step is to perform a thyroid biopsy.
At Mount Sinai, we have a team of cytopathologists who evaluate thousands of samples per year, so we are confident in the accuracy of our biopsies. When a biopsy does not give a clear answer, we automatically use molecular profiling to refine the diagnosis.
How Is a Thyroid Biopsy Performed?
Thyroid biopsy, also called a fine needle aspiration (FNA), uses a small needle to take a little sample of the cells in the thyroid nodule. An ultrasound machine typically guides your doctor or cytopathologist during the biopsy. A topical anesthetic spray is used to make it comfortable for the patient. Once the sample is obtained, the patient usually waits one week for a pathologist to further examine the cellular characteristic of the biopsy sample.
What Will the Biopsy Tell Us?
A biopsy may demonstrate one of FIVE possible outcomes: the biopsy may be “non-diagnostic”, “benign”, “indeterminate”, “suspicious”, or “malignant”.
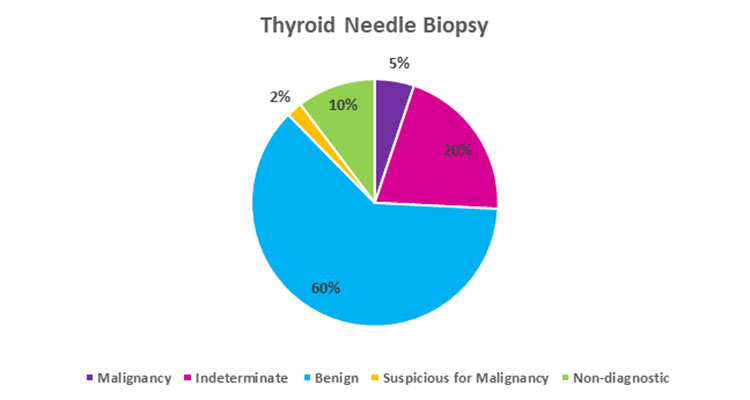
- Non-diagnostic: Non-diagnostic is a technically failed biopsy. This occurs when not enough cells taken during a biopsy so the cytologist was not able to determine anything. These usually need to be repeated.
- Benign: Most thyroid nodule biopsies come back benign. This suggest that the nodule is not cancerous. Patients can almost always avoid surgery with a benign diagnosis unless the nodule is large and pushing on adjacent structures, or the nodule is growing.
- Indeterminate: Indeterminate means there was enough cells taken during the biopsy, but the cytopathologist was not sure if it is benign or malignant. Indeterminate results occur in about 30% of thyroid biopsies. This is a gray zone and means that the risk of cancer is about 10-30%. These nodules require additional work-up such as a repeat biopsy, molecular marker test, or surgical removal. In some cases, we recommend molecular profiling for indeterminate biopsies.
- Suspicious for Malignancy or Malignant: Results categorized in these two categories are a strong indicator that there is cancer present and usually require surgical removal.
If your doctor is reassured that it is benign based on the biopsy result, further work-up is stopped and serial ultrasound surveillance is recommended usually once a year. It is important to remember that although needle biopsies and the practice of cytology is a wonderful medical development, it is not 100 percent specific or sensitive.
While both the sensitivity, the ability to diagnose either benign or malignant disease, and specificity, ability to tell us exactly what type of tumor is within the nodule, is excellent, there is still a false positive and false negative rate that ranges between 1-7 percent, depending on the cytologist’s experience. This is one of the advantages of coming to a tertiary care medical center like Mount Sinai; our pathologists have a wealth of experience and expertise in this area leading to a very low rate of false positive and false negative readings.
What Is Molecular Profiling?
Thyroid nodules with indeterminate biopsies may be assessed for molecular mutations.
Mutational testing is designed to identify mutations within the DNA of the nodules to more accurately determine if the nodule represents a cancer or the risk of developing into a cancer. In the past, to avoid missing a cancer, we recommended thyroid lobectomy to establish a definitive diagnosis. In many cases, mutational testing will provide us with more information. If the genetic profile appears benign, patients can avoid surgery and we simply monitor the nodule with neck ultrasound.