Tracheal Airway Disease and Tracheal Transplant Program
The Tracheal Airway Disease and Tracheal Transplant Program at the Mount Sinai Health System is world-renowned for advanced disease of the tracheal airway. The Program provides specialized treatments for disorders of the trachea using a multidisciplinary approach. The specialized team includes head and neck surgeons, thoracic surgeons, laryngologists, pulmonologists, pulmonary interventionalists, and experts in airway radiology. Offering patients state-of-the-art diagnostics and management, this program is the first in the world with a Tracheal Transplant Program for patients with severe long segment disease of the tracheal airway.
Our multidisciplinary team is comprised of innovators in tracheal reconstruction and laryngeal reconstruction focused on restoration of the airway and voice.
The program for tracheal airway disease and transplantation is designed to manage patients with all forms of tracheal airway disease including congenital, disease that results from tumors, and acquired disease. Patients can email our program coordinators at ENTheadneck@mountsinai.org for referrals and review.
Our treatment approach is derived from years of basic science and clinical signs programs focused on management of tracheal airway disease. Our team recently performed the world’s tracheal transplant for a patient with extensive long segment tracheal disease.
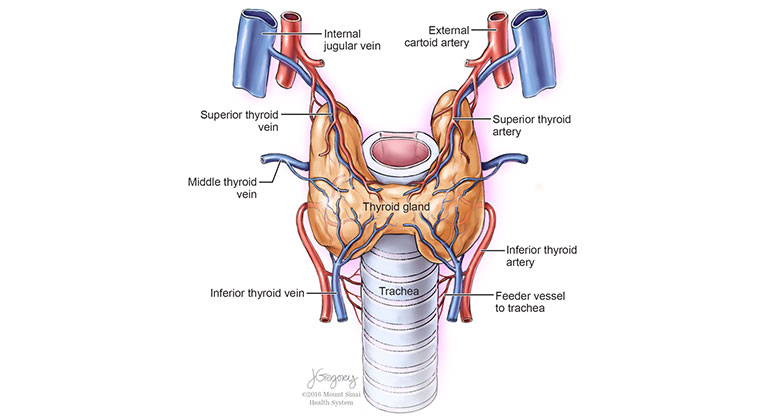
Airway and Trachea Conditions We Treat
Our complex Airway Program treats patients with a variety of disorders that impact breathing and may present as wheezing or shortness of breath. These disorders may be congenital (a young child is born with a tracheal disorder), develop after injury or cancer, or occur after treatment for another condition. Mount Sinai physicians have significant experience in performing surgical procedures to treat complex airway conditions:
- Tracheobronchomalacia
- Tracheal stenosis
- Tracheal or bronchial tumor
- Tracheoesophageal fistula
- Tracheostomy-related problems (granulation tissue, stoma issues)
Patient Care: What to Expect (Evaluation and Management of Airway Disorders)
New patients undergo a comprehensive multidisciplinary evaluation. The team reviews the nature of the disease and establishes a treatment plan in consultation with the patient and the family. While many of the problems that we evaluate can be remedied through our minimally invasive pulmonary interventional program, some patients will require surgery. As one of the most well recognized centers in the world, treatment options span the full range from dilation, to surgical resection, to tracheal transplantation for patients with the most severe disease.
Treatment Options
Airway and tracheal treatments encompass:
- Airway stent
- T-tube
- Bronchial dilation
- Tracheal or bronchial resection and reconstruction
- Tracheoplasty
- Carinal Resection and Reconstruction
- Repair of tracheoesophageal fistula
- Revision of tracheal stoma
- Tracheostomy-related maintenance
The team includes the finest pulmonary physicians and surgical team as well as a team of anesthesiologists who play a critical role in the management of patients with airway problems.