Mount Sinai Researchers Receive $13 Million NIH Grant to Study Connection Between Stress-Associated Brain Activity and Cardiovascular Risk
Project aims to provide new guidelines for clinicians and researchers to provide more comprehensive risk assessment in patients
Researchers at the Icahn School of Medicine at Mount Sinai have been awarded $13 million from the National Heart, Lung, and Blood Institute of the National Institutes of Health (NIH) for a five-year research program that aims to uncover the mechanisms by which stress contributes to cardiovascular risk. The program aims to improve our understanding of how the effect of stress on the brain can directly impact the immune system and cardiovascular disease, and to provide a scientific platform for clinicians and researchers to integrate this knowledge into patient care.
While abundant epidemiological data exists describing severe chronic stress as a risk factor for cardiovascular disease, the mechanism by which stress contributes to cardiovascular events is not fully understood. Preclinical preliminary data from the program's investigators describe a direct causal link between psychosocial stress, neural signals, and atherosclerosis, the chronic inflammatory disease that is the underlying cause of heart attacks and strokes. To better characterize risk of future cardiovascular events as affected by psychosocial stress, researchers will study the levels of macrophages—key immune cells contributing to the inflammation that characterizes atherosclerosis—within the arteries, blood, and organs of the immune system.
The program consists of three distinct studies. The first will use mouse models to explore how the brain reacts to stress and affects the immune system to increase cardiovascular disease risk. The second study will translate discoveries from the first to develop non-invasive imaging methodologies, such as combined MRI and PET scans, in order to study these same processes in larger mammals and humans. The third study will then use these imaging technologies to examine the link between increased emotional stress and increased cardiovascular risk in human subjects diagnosed with post-traumatic stress disorder.
“A better understanding of non-traditional risk factors to cardiovascular disease, such as psychosocial stress, allows for a more comprehensive risk assessment in patients,” says Zahi A. Fayad, PhD, Mount Sinai Endowed Chair in Medical Imaging and Bioengineering, Professor of Radiology and Medicine (Cardiology), and Director of the Translational and Molecular Imaging Institute (TMII) at the Icahn School of Medicine at Mount Sinai, and the Principal Investigator of the study. “The development of non-invasive imaging technology to assess cardiovascular risk in relationship to brain and immune system activation opens new opportunities for early diagnosis and treatment of cardiovascular disease.”
“The findings from this pioneering study will have significant impact on current and future research in cardiovascular disease, psychiatry, and imaging,” says Dennis S. Charney, MD, Anne and Joel Ehrenkranz Dean, Icahn School of Medicine at Mount Sinai, and President for Academic Affairs, Mount Sinai Health System. “We appreciate the NIH recognition of our efforts and are excited to be part of this groundbreaking endeavor.”
The research team from the Icahn School of Medicine at Mount Sinai is composed of Dr. Fayad (overall PI, PI Project 3 and Administration/data Core); Willem Mulder, PhD, Professor, (PI Project 2); Venkatesh Mani, PhD, Assistant Professor (PI Imaging Core); Cheuk Tang, PhD, Associate Professor; Claudia Calcagno, MD, PhD; James Murrough, MD, Assistant Professor; Dr. Charney; Valentin Fuster, MD, PhD, Director, Mount Sinai Heart; Emilia Bagiella, PhD, Professor; and Helena Chang, MS, Senior Biostatistician. Other institutions involved in this program include New York University and Massachusetts General Hospital. The research team includes multidisciplinary investigators in cardiac and neuroimaging, psychiatry, psychology, neuroscience, neurology, cardiology, immunology, and nanotechnology.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 47,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and leading schools of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care from conception through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes more than 6,400 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals,” “Best in State Hospitals,” “World’s Best Hospitals,” and “Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.
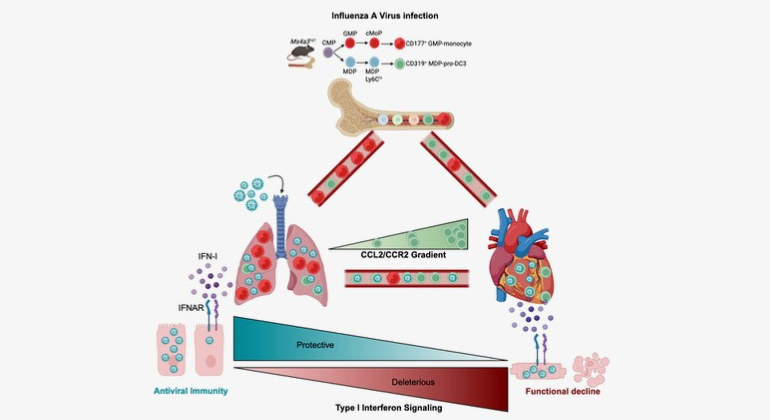
Mount Sinai Scientists Uncover Link Between Influenza and Heart Disease
Feb 09, 2026 View All Press Releases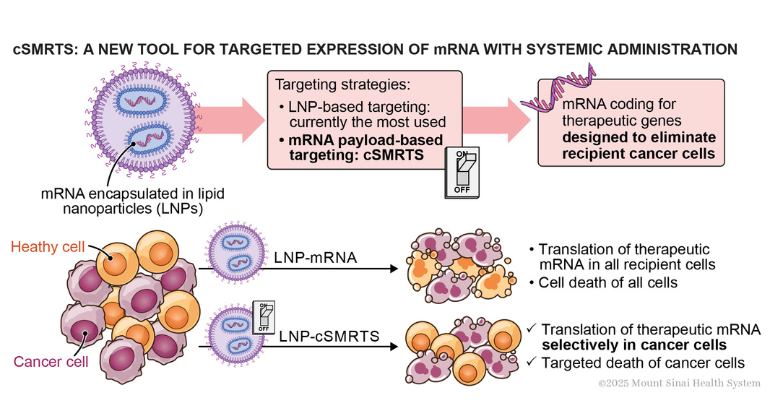
Scientists Develop a Smarter mRNA Therapy That Knows Which Cells to Target
Dec 15, 2025 View All Press Releases
A Specific Human Gene Can Help the Heart Repair Itself From Heart Attack or Heart Failure
Nov 03, 2025 View All Press Releases