Glaucoma
Open-angle glaucoma; Chronic glaucoma; Chronic open-angle glaucoma; Primary open-angle glaucoma; Closed-angle glaucoma; Narrow-angle glaucoma; Angle-closure glaucoma; Acute glaucoma; Secondary glaucoma; Congenital glaucoma; Vision loss - glaucoma
Glaucoma is a group of eye conditions that can damage the optic nerve. This nerve sends the images you see to your brain.
Most often, optic nerve damage is caused by increased pressure in the eye. This is called intraocular pressure.
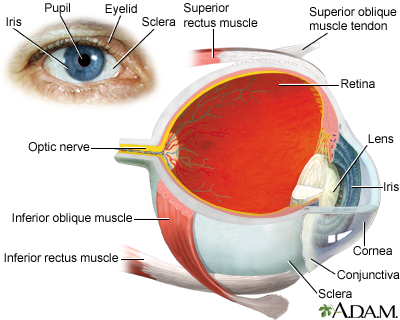
The eye is the organ of sight, a nearly spherical hollow globe filled with fluids (humors). The outer layer or tunic (sclera, or white, and cornea) is fibrous and protective. The middle layer (choroid, ciliary body and the iris) is vascular. The innermost layer (the retina) is nervous or sensory. The fluids in the eye are divided by the lens into the vitreous humor (behind the lens) and the aqueous humor (in front of the lens). The lens itself is flexible and suspended by ligaments which allow it to change shape to focus light on the retina, which is composed of sensory neurons.
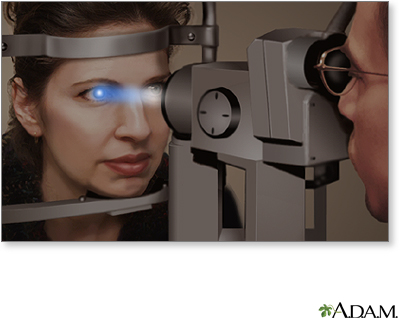
A slit-lamp, which is a specialized magnifying microscope, is used to examine the structures of the eye (including the cornea, iris, vitreous, and retina). The slit-lamp is used to examine, treat (with a laser), and photograph (with a camera) the eye.
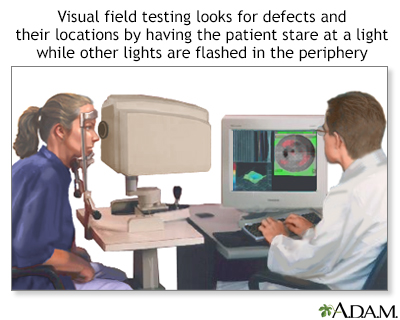
Central and peripheral vision is tested by using visual field tests. Changes may indicate eye diseases, such as glaucoma or retinitis.
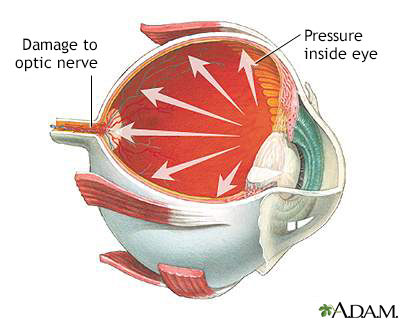
Glaucoma is a condition of increased fluid pressure inside the eye. The increased pressure causes compression of the retina and the optic nerve which can eventually lead to nerve damage. Glaucoma can cause partial vision loss, with blindness as a possible eventual outcome.
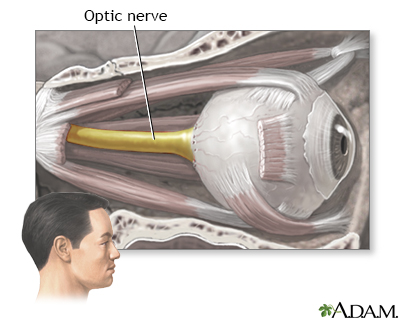
The optic nerve carries the information of vision from the eye to the brain.

Tonometry is a test to measure the fluid pressure inside your eyes. This test is used to screen for glaucoma. It is also used to measure how well glaucoma treatment is working. Applanation tonometry uses a slit lamp with supports for your forehead and chin and a small cone that gently touches your cornea after it has been made numb with eye drops. This cone is used to measure the force (pressure) needed to temporarily flatten a part of your cornea.
Causes
Glaucoma is the second most common cause of blindness in the United States. There are four major types of glaucoma:
- Open-angle glaucoma
- Angle-closure glaucoma, also called closed-angle glaucoma
- Congenital glaucoma
- Secondary glaucoma
The front part of the eye is filled with a clear fluid called aqueous humor. This fluid is made in an area behind the colored part of the eye (iris). It leaves the eye through channels where the iris and cornea meet. This area is called the anterior chamber angle, or the angle. The cornea is the clear covering on the front of the eye that is in front of the iris, pupil, and angle.
Anything that slows or blocks the flow of this fluid will cause pressure to build up in the eye.
- In open-angle glaucoma, the increase in pressure is often small and slow.
- In closed-angle glaucoma, the increase is often high and sudden.
- Either type can damage the optic nerve.
Open-angle glaucoma is the most common type of glaucoma.
- The cause is unknown. The increase in eye pressure happens slowly over time. You cannot feel it.
- The increased pressure pushes on the optic nerve. Damage to the optic nerve causes blind spots in your vision.
- Open-angle glaucoma tends to run in families. Your risk is higher if you have a parent or grandparent with open-angle glaucoma. People of African descent are also at higher risk for this disease.
Closed-angle glaucoma occurs when the fluid is suddenly blocked and cannot flow out of the eye. This causes a quick, severe rise in eye pressure.
- Dilating eye drops and certain medicines may trigger an acute glaucoma attack.
- Closed-angle glaucoma is an emergency.
- If you have had acute glaucoma in one eye, you are at risk for it in the second eye. Your health care provider is likely to treat your second eye to prevent a first attack in that eye.
Secondary glaucoma occurs due to a known cause. Both open- and closed-angle glaucoma can be secondary when caused by something known. Causes include:
- Medicines such as corticosteroids
- Eye diseases, such as uveitis (an inflammation of the middle layer of the eye)
- Diseases such as diabetes
- Eye injury
Congenital glaucoma occurs in babies.
- It often runs in families.
- It is present at birth.
- It is caused when the eye does not develop normally.
Symptoms
OPEN-ANGLE GLAUCOMA
- Most people have no symptoms.
- Once you are aware of vision loss, the damage is already severe.
- Slow loss of side (peripheral) vision (also called tunnel vision) is the main type of vision loss.
- Advanced glaucoma can lead to blindness.
ANGLE-CLOSURE GLAUCOMA
Symptoms may come and go at first, or steadily become worse. You may notice:
- Sudden, severe pain in one eye
- Decreased or cloudy vision, often called "steamy" vision
- Nausea and vomiting
- Rainbow-like halos around lights
- Red eye
- Eye feels swollen
CONGENITAL GLAUCOMA
Symptoms are most often noticed when the child is a few months old.
- Cloudiness of the front of the eye
- Enlargement of one eye or both eyes
- Red eye
- Sensitivity to light
- Tearing
SECONDARY GLAUCOMA
- Symptoms are most often related to the underlying problem causing the glaucoma.
- Depending on the cause, symptoms may either be like open-angle glaucoma or angle-closure glaucoma.
Exams and Tests
The only way to diagnose glaucoma is by having a complete eye exam.
- You will be given a test to check your eye pressure. This is called tonometry.
- In most cases, you will be given eye drops to widen (dilate) your pupil.
- When your pupil is dilated, your eye doctor will look at the inside of your eye and the optic nerve.
Eye pressure is different at different times of the day. Eye pressure can even be normal in some people with glaucoma. So you may need other tests to confirm glaucoma. They may include:
- Using a special lens to look at the angle of the eye (gonioscopy).
- Photographs or laser scanning images of the inside of your eye (optic nerve imaging).
- Laser scanning images of the angle of the eye.
- Checking your retina -- The retina is the light-sensitive tissue at the back of your eye.
- Checking how your pupil responds to light (pupillary reflex response).
- 3-D view of your eye (slit lamp examination).
- Testing the clearness of your vision (visual acuity).
- Testing your field of vision (visual field measurement).
Treatment
The goal of treatment is to reduce your eye pressure. Treatment depends on the type of glaucoma that you have.
OPEN-ANGLE GLAUCOMA
- If you have open-angle glaucoma, you will probably be given eye drops.
- You may need more than one type. Most people can be treated with eye drops.
- Most of the eye drops used today have fewer side effects than those used in the past.
- You also may be given pills to lower pressure in the eye.
If drops alone do not work, you may need other treatment:
- Laser treatment uses a painless laser to open the channels where fluid flows out.
- If drops and laser treatment do not work, you may need surgery. Your eye doctor will open a new channel so fluid can escape. This will help lower your eye pressure.
- Recently, new implants have been developed that can help treat glaucoma in people having cataract surgery.
ACUTE ANGLE GLAUCOMA
An acute angle-closure attack is a medical emergency. You can become blind in a few days if you are not treated.
- You may be given eye drops, pills, and medicine given through a vein (by IV) to lower your eye pressure.
- Some people also need an emergency operation, called an iridotomy. The doctor uses a laser to open a new channel in the iris. Sometimes this is done with surgery. The new channel relieves the attack and will prevent another attack.
- To help prevent an attack in the other eye, the same procedure will often be performed on the other eye. This may be done even if it has never had an attack.
CONGENITAL GLAUCOMA
- Congenital glaucoma is almost always treated with surgery.
- This is done using general anesthesia. This means the child is asleep and feels no pain.
SECONDARY GLAUCOMA
If you have secondary glaucoma, treating the cause may help your symptoms go away. Other treatments also may be needed.
Outlook (Prognosis)
Open-angle glaucoma cannot be cured. You can manage it and keep your sight by following your provider's directions.
Closed-angle glaucoma is a medical emergency. You need treatment right away to save your vision.
Babies with congenital glaucoma usually do well when surgery is done early.
How you do with secondary glaucoma depends on what is causing the condition.
When to Contact a Medical Professional
If you have severe eye pain or a sudden loss of vision, get immediate medical help. These may be signs of closed-angle glaucoma.
Prevention
You cannot prevent open-angle glaucoma. Most people have no symptoms. But you can help prevent vision loss.
- A complete eye exam can help find open-angle glaucoma early, when it is easier to treat.
- All adults should have a complete eye exam by the age of 40.
- If you are at risk for glaucoma, you should have a complete eye exam sooner than age 40.
- You should have regular eye exams as recommended by your provider.
If you are at risk for closed-angle glaucoma, your provider may recommend treatment before you have an attack to help prevent eye damage and vision loss.
References
2019 exceptional surveillance of glaucoma: diagnosis and management (NICE guideline NG81) [Internet]. London: National Institute for Health and Care Excellence (UK); 2019 Sep 12. PMID: 31909934
Gedde SJ, Lind JT, Wright MM, et al. American Academy of Ophthalmology Preferred Practice Pattern Glaucoma Panel. primary open-angle glaucoma suspect preferred practice pattern. Ophthalmology. 2021;128(1):P151-P192. PMID: 34933743
McMillan BD, Gross RL. Current medical management of glaucoma. In: Yanoff M, Duker JS, eds. Ophthalmology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 10.22.
Hood DC, La Bruna S, Tsamis E, et al. Detecting glaucoma with only OCT: implications for the clinic, research, screening, and AI development. Prog Retin Eye Res. 2022;90:101052. PMID: 35216894
Jampel HD, Mahjoub H. Evidence-based medicine in glaucoma. In: Yanoff M, Duker JS, eds. Ophthalmology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 10.32.
Madu A, Rhee DJ. Which therapy to use in glaucoma. In: Yanoff M, Duker JS, eds. Ophthalmology. 5th ed. Philadelphia, PA: Elsevier; 2019:chap 10.23.
Moyer VA; U.S. Preventive Services Task Force. Screening for glaucoma: U.S. Preventive Services Task Force Recommendation Statement. Ann Intern Med. 2013;159(7):484-489. PMID: 24325017
Stein JD, Khawaja AP, Weizer JS. Glaucoma in adults-screening, diagnosis, and management: a review. JAMA. 2021;325(2):164-174. PMID: 33433580
Version Info
Last reviewed on: 8/22/2022
Reviewed by: Franklin W. Lusby, MD, Ophthalmologist, Lusby Vision Institute, La Jolla, CA. Internal review and update on 07/23/2023 by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
