Shoulder pain
Pain - shoulder
Shoulder pain is any pain in or around the shoulder joint.

Swelling, damage, or bone changes around the rotator cuff in your shoulder can cause pain that puts a kink in the activities of your life. Let's talk about shoulder pain. The rotator cuff is a group of muscles and tendons that attach to the bones of your shoulder joint. The group allows your shoulder to move and keep it stable. The most common cause of shoulder pain is when rotator cuff tendons become inflamed or trapped in your shoulder. This is called rotator cuff tendinitis, or irritation of these tendons and inflammation of the bursa, small slippery fluid filled sacs that the tendons glide over. A rotator cuff tear, when one of the tendons is torn from overuse or injury, can also cause intense shoulder pain. Other causes of shoulder pain can include arthritis, bone spurs - bony projections, a broken shoulder bone, frozen shoulder, when the muscles, tendons, and ligaments in your shoulder become stiff, and shoulder dislocation. Most of the time, you can take care of your shoulder pain at home. Try putting ice on your shoulder for 15 minutes, then leave it off for 15 minutes, three or four times a day for a few days. Make sure you wrap the ice in cloth, so it doesn't give you frostbite. Take ibuprofen to reduce pain and swelling. Slowly return to your regular activities once you start feeling less pain. Sudden shoulder pain can be a sign of a heart attack. Call Emergency Services if you have sudden pressure or crushing pain in your shoulder, especially if the pain starts in your chest, jaw, or neck. If you fall on your shoulder and feel sudden intense pain, you should see a doctor because you may have torn rotator cuff or dislocated your shoulder. If you have had shoulder pain before, try using ice and ibuprofen after exercising. Learn proper exercises to stretch and strengthen your rotator cuff tendons and shoulder muscles. Also, physical therapy can help. Make an appointment and talk about your options.

Feeling pain in your shoulder when you lift your arm over your head may mean you have a have a problem with your rotator cuff. So, what causes rotator cuff problems? The rotator cuff is a group of muscles and tendons that attach to the bones of your shoulder joint. The group allows your shoulder to move and keeps it stable. Pain in your rotator cuff area usually means you have rotator cuff tendinitis, or inflammation of these tendons and inflammation of the bursa, smooth slippery sacs the tendons glide across; or a rotator cuff tear, when one the tendons is torn from overuse or injury. Rotator cuff tendinitis may be due to keeping your arm in the same position for long periods of time, such as doing computer work or hairstyling. Sleeping on the same arm each night can also cause this problem. You can also get tendinitis playing sports that require you to move your arm over your head repeatedly, such as in tennis, baseball especially pitching, swimming, and weight-lifting. Rotator cuff tears may happen if you fall on your arm while it is stretched out, or after a sudden, jerking motion when trying to lift something heavy. Chronic tears occur slowly over time, particularly in people who have chronic tendinitis. At some point, the tendon wears down and starts to tear. If you have tendinitis, you'll have pain when you lift your arm over your head, such as when you brush your hair and reach for objects on shelves. The pain may be mild at first, but over time you may have pain at rest or at night, especially when you lie on your shoulder. The pain of a sudden rotator cuff tear can be intense. Your shoulder may be weak, and you may hear a snapping sound when you move your shoulder. Chronic symptoms include a gradual worsening of pain, weakness, stiffness or loss of motion. Most people with rotator cuff tears have worse pain at night and when they wake up. To treat your rotator cuff problem, your doctor will check your shoulder for tenderness and lift your arm to see in which position you have pain. X-rays may show a bone spur, a bony projection. If your doctor thinks you have a tear, you may have an ultrasound or MRI. Treatment for rotator cuff tendinitis involves resting your shoulder and avoiding the activities that cause you pain. You can also try applying ice packs 20 minutes at a time, 3 or 4 times a day. Medicines like ibuprofen may help reduce swelling and inflammation. Eventually, you should start physical therapy to learn to stretch and strengthen the muscles of your shoulder. Surgery can remove inflamed tissue and part of the bone that lies over the rotator cuff, which may help relieve the pressure on your tendons. Someone with a partial rotator cuff tear can try rest and exercise, if they don't normally put a lot of demand on their shoulder. But if there's a complete tear, or if the symptoms don't improve with therapy, you may need surgery to repair the tendon. But with rest or exercise, symptoms of most shoulder problems often improve or go away, though it may take months.
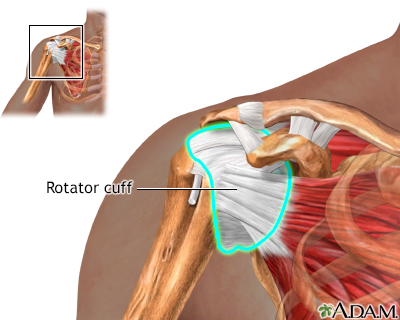
The rotator cuff is a group of muscles and tendons that form a cuff over the shoulder. These muscles and tendons hold the arm in its ball and socket joint and are involved in essentially all shoulder motions.
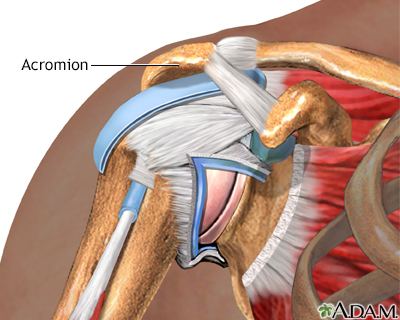
When tendons become trapped under the acromion, the rigid bony arch of the shoulder blade, it can cause shoulder pain called impingement syndrome. The tendons become compressed, damaged, and inflamed leading to rotator cuff tendonitis. This can occur from general wear and tear as you get older, or from an activity that requires constant use of the shoulder like baseball pitching, or from an injury.
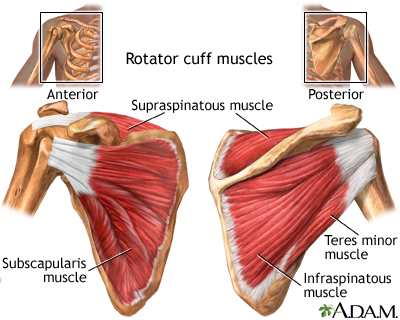
There are four muscle tendons that connect to the shoulder that make up the rotator cuff. Together these four tendons stabilize the upper arm bone to the shoulder socket and allow the wide range of motion in the shoulder.
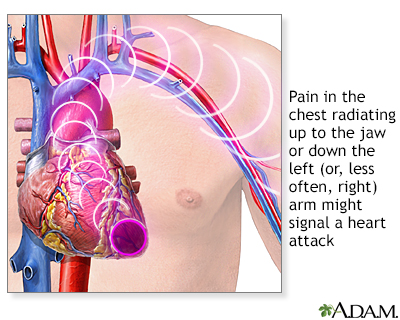
Symptoms of a possible heart attack include chest pain and pain that radiates down the shoulder and arm. Some people (older adults, people with diabetes, and women) may have little or no chest pain. Or, they may experience unusual symptoms (shortness of breath, fatigue, weakness). Women are more likely than men to have symptoms of nausea, vomiting, back or jaw pain, and shortness of breath with chest pain.

Force on a joint can cause a dislocation. The force pushes the bone out of the socket, which may damage surrounding ligaments, tendons, and nerves.
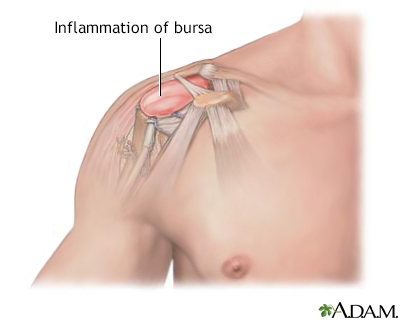
Bursae are fluid-filled cavities located at tissue sites where tendons or muscles pass over bony prominences near joints. Their function is to facilitate movement and reduce friction between moving parts. When a bursa becomes infected, traumatized, or injured it is referred to as bursitis.
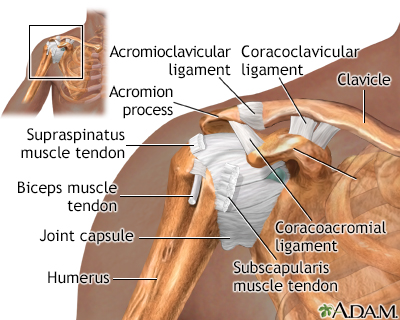
Ligaments hold the shoulder joint together. A disruption or weakening of these connections is a shoulder separation.
Considerations
The shoulder is the most movable joint in the human body. A group of four muscles and their tendons, called the rotator cuff, give the shoulder its wide range of motion.
Swelling, damage, or bone changes around the rotator cuff can cause shoulder pain. You may have pain when lifting the arm above your head or moving it forward or behind your back.
Causes
The most common cause of shoulder pain occurs when rotator cuff tendons become trapped under the bony area in the shoulder. The tendons become inflamed or damaged. This condition is called rotator cuff tendinitis or bursitis.
Shoulder pain may also be caused by:
- Arthritis in the shoulder joint
- Bone spurs in the shoulder area
- Bursitis, which is inflammation of a fluid-filled sac (bursa) that normally protects the joint and helps it move smoothly
- Broken shoulder bone
- Dislocation of the shoulder
- Shoulder separation
- Frozen shoulder, which occurs when the muscles, tendons, and ligaments inside the shoulder become stiff, making movement difficult and painful
- Overuse or injury of nearby tendons, such as the bicep muscles of the arms
- Nerve injury that leads to abnormal shoulder movement
- Tears of the rotator cuff tendons
- Poor shoulder posture and mechanics
Sometimes, shoulder pain may be due to a problem in another area of the body, such as the neck or lungs. This is called referred pain. There is usually pain at rest and no worsening of pain when moving the shoulder.
Home Care
Here are some tips for helping shoulder pain get better:
- Put ice on the shoulder area for 15 minutes, then leave it off for 15 minutes. Do this 3 to 4 times a day for 2 to 3 days. Wrap the ice in cloth. Do not put ice directly on the skin because this can result in frostbite.
- Rest your shoulder for the next few days.
- Slowly return to your regular activities. A physical therapist can help you do this safely.
- Taking ibuprofen or acetaminophen (such as Tylenol) may help reduce inflammation and pain.
Rotator cuff problems can be treated at home also.
- If you have had shoulder pain before, use ice and ibuprofen after exercising.
- Learn exercises to stretch and strengthen your rotator cuff tendons and shoulder muscles. A health care provider or physical therapist can recommend such exercises.
- If you are recovering from tendinitis, continue to do range-of-motion exercises to avoid frozen shoulder.
- Practice good posture to keep your shoulder muscles and tendons in their right positions.
When to Contact a Medical Professional
Sudden left shoulder pain can sometimes be a sign of a heart attack. Call 911 or the local emergency number if you have sudden pressure or crushing pain in your shoulder, especially if the pain runs from your chest to the left jaw, arm or neck, or occurs with shortness of breath, dizziness, or sweating.
Go to the hospital emergency room if you have just had a severe injury and your shoulder is very painful, swollen, bruised, or bleeding.
Call your provider if you have:
- Shoulder pain with a fever, swelling, or redness
- Significant pain even with moving the shoulder with the arm or by someone else
- Pain for more than 2 to 4 weeks, even after home treatment
- Swelling of the shoulder
- Red or blue color of the skin of the shoulder area
What to Expect at Your Office Visit
Your provider will perform a physical exam and closely look at your shoulder. You will be asked questions to help the provider understand your shoulder problem.
Blood or imaging tests, such as x-rays or MRI, may be ordered to help diagnose the problem.
Your provider may recommend treatment for shoulder pain, including:
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Injection of an anti-inflammatory medicine called corticosteroid
- Physical therapy
- Surgery if all other treatments do not work
If you have a rotator cuff problem, your provider will likely suggest self-care measures and exercises.
References
Gill TJ. Shoulder diagnosis and decision-making. In: Miller MD, Thompson SR, eds. DeLee, Drez, & Miller's Orthopaedic Sports Medicine: Principles and Practice. 5th ed. Philadelphia, PA: Elsevier; 2020:chap 37.
Martin SD, Thornhill TS. Shoulder pain. In: Firestein GS, Budd RC, Gabriel SE, Koretzky GA, McInnes IB, O'Dell JR, eds. Firestein & Kelley's Textbook of Rheumatology. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 49.
Version Info
Last reviewed on: 8/12/2023
Reviewed by: C. Benjamin Ma, MD, Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery, San Francisco, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
