Nuclear stress test
Sestamibi stress test; MIBI stress test; Myocardial perfusion scintigraphy; Dobutamine stress test; Persantine stress test; Thallium stress test; Stress test - nuclear; Adenosine stress test; Regadenoson stress test; CAD - nuclear stress; Coronary artery disease - nuclear stress; Angina - nuclear stress; Chest pain - nuclear stress
Nuclear stress test is an imaging method that uses radioactive material to show how well blood flows into the heart muscle, both at rest and during activity.
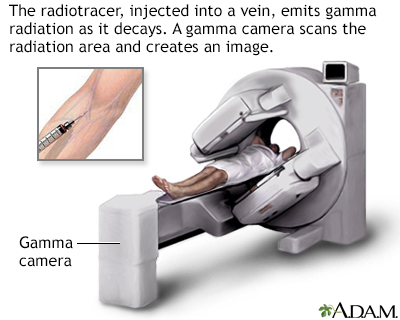
A radiotracer is injected into a peripheral vein. As the radiotracer decays, gamma radiation is emitted and is detected by a Gamma camera. When the tracer has collected in the target organ the area is scanned. Radionuclide scans can detect abnormalities such as fractures, bone infections, arthritis, rickets, and tumors that have spread, among other diseases.
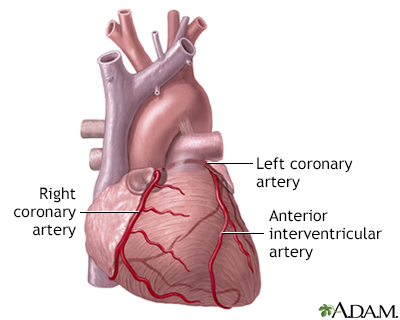
The coronary arteries supply blood to the heart muscle. The right coronary artery supplies both the left and the right heart; the left coronary artery supplies the left heart.
How the Test is Performed
This test is done at a medical center or health care provider's office. It is done in stages:
You will have an intravenous (IV) line started.
- A radioactive substance, such as thallium or sestamibi, will be injected into one of your veins.
- You will lie down and wait for between 15 and 45 minutes.
- A special camera will scan your heart and create pictures to show how the substance has traveled through your blood and into your heart.
Most people will then walk on a treadmill (or pedal on an exercise machine).
- After the treadmill starts moving slowly, you will be asked to walk (or pedal) faster and on an incline.
- If you are not able to exercise, you may be given a medicine called a vasodilator (such as adenosine or dipyridamole [persantine]). This medicine widens (dilates) your heart arteries.
- In other cases, you may get a medicine (dobutamine) that will make your heart beat faster and harder, similar to when you exercise.
Your blood pressure and heart rhythm (electrocardiogram - ECG) will be monitored throughout the test.
When your heart is working as hard as it can, a radioactive substance is again injected into one of your veins.
- You will wait for 15 to 45 minutes.
- Again, the special camera will scan your heart and create pictures.
- You may be allowed to get up from the table or chair and have a snack or drink.
Your provider will compare the first and second set of pictures using a computer. This can help detect if you have heart disease or if your heart disease is becoming worse.
How to Prepare for the Test
You should wear comfortable clothes and shoes with non-skid soles. You may be asked not to eat or drink after midnight. You will be allowed to have a few sips of water if you need to take medicines.
You will need to avoid caffeine for 24 hours before the test. This includes:
- Tea and coffee
- All sodas, even ones that are labeled caffeine-free
- Chocolates, and certain pain relievers that contain caffeine
Many medicines can interfere with blood test results.
- Your provider will tell you if you need to stop taking any medicines before you have this test.
- Do not stop or change your medicines without talking to your provider first.
How the Test will Feel
During the test, some people feel:
- Chest pain
- Fatigue
- Muscle cramps in the legs or feet
- Shortness of breath
If you are given the vasodilator medicine, you may feel a sting as it is injected. This is followed by a feeling of warmth. Some people also have a headache, nausea, and a feeling that their heart is racing.
If you are given medicine to make your heart beat stronger and faster (dobutamine), you may have a headache, nausea, or your heart may pound faster and more strongly.
Rarely, during the test people experience:
- Chest discomfort
- Dizziness
- Palpitations
- Shortness of breath
If any of these symptoms occur during your test, tell the person performing the test right away.
Why the Test is Performed
The test is done to see if your heart muscle is getting enough blood flow and oxygen when it is working hard (under stress).
Your provider may order this test to find out:
- How well a treatment (medicines, angioplasty, or heart surgery) is working.
- If you are at high risk for heart disease or complications.
- If you are planning to start an exercise program or have surgery.
- The cause of new chest pain or worsening angina.
- What you can expect after you have had a heart attack.
The results of a nuclear stress test can help:
- Determine how well your heart is pumping
- Determine the proper treatment for coronary heart disease
- Diagnose coronary artery disease
- See whether your heart is too large
Normal Results
A normal test most often means that you were able to exercise as long as or longer than most people of your age and sex. You also did not have symptoms or changes in blood pressure, your ECG or the images of your heart that caused concern.
A normal result means blood flow through the coronary arteries is probably normal.
The meaning of your test results depends on the reason for the test, your age, and your history of heart and other medical problems.
What Abnormal Results Mean
Abnormal results may be due to:
- Reduced blood flow to a part of the heart. The most likely cause is a narrowing or blockage of one or more of the arteries that supply your heart muscle.
- Scarring of the heart muscle due to a previous heart attack.
After the test you may need:
- Angioplasty and stent placement
- Changes in your heart medicines
- Coronary angiography
- Heart bypass surgery
Risks
Complications are rare, but may include:
- Arrhythmias
- Increased angina pain during the test
- Breathing problems or asthma-like reactions
- Extreme swings in blood pressure
- Skin rashes
Your provider will explain the risks before the test.
Considerations
In some cases, other organs and structures can cause false-positive results. However, special steps can be taken to avoid this problem.
You may need additional tests, such as cardiac catheterization, depending on your test results.
References
Balady GJ, Ades PA. Exercise physiology and exercise electrocardiographic testing. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 15.
Dorbala S, DiCarli MF. Nuclear cardiology. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 18.
Gulati M, Levy PD, Mukherjee D, et al. 2021 AHA/ACC/ASE/CHEST/SAEM/SCCT/SCMR Guideline for the evaluation and diagnosis of chest pain: a report of the American College of Cardiology/American Heart Association Joint Committee on clinical practice guidelines. Circulation. 2021;144(22):e368 e454. PMID: 34709879
Morrow DA, de Lemos JA. Stable ischemic heart disease. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 40.
Virani SS, Newby LK, Arnold SV, et al. 2023 AHA/ACC/ACCP/ASPC/NLA/PCNA guideline for the management of patients with chronic coronary disease: a report of the American Heart Association/American College of Cardiology Joint Committee on Clinical Practice Guidelines. Circulation. 2023;148(9):e9–e119. PMID: 37471501
Version Info
Version: 2.0
Last reviewed on: 7/14/2024
Reviewed by: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
