Mount Sinai Scientists Gain New Insight into Hepatitis C Antiviral Resistance
Nature Communications paper offers pivotal new information about how the virus interacts with and evades therapeutics, as well as new clues to its role in cancer development
A team of scientists specializing in genomics and microbiology at the Icahn School of Medicine at Mount Sinai has revealed important new information about the hepatitis C virus (HCV), including its response to targeted therapeutics and new insight about its role in cancer development. The work, published in Nature Communications, focused on microRNA genes — a recently discovered type of regulatory gene —and used whole-genome sequencing of the virus to challenge conventional wisdom about how the virus responds to emerging therapies. The findings may contribute to more effective development of hepatitis C drugs in the future and to more personalized treatment for patients.
According to the Centers for Disease Control and Prevention, HCV is widespread, affecting some 3 percent of the world’s population and more than 3 million people in the United States alone. Recent CDC reports indicate that hepatitis C infections are on the rise among young people and are increasingly the cause of death among baby boomers. The vast majority of people who get HCV will suffer chronic infection, which can lead to liver inflammation, cirrhosis, and liver cancer. Highly effective new treatments have been launched recently, but their high prices have caused public outcry and limited widespread use. There is no commercially available vaccine for hepatitis C.
In this new study, Mount Sinai researchers examined HCV response to an experimental treatment that targets and blocks the supply of a microRNA that the virus needs for infection of human cells. Contrary to expectations, they found that depleting the supply of this microRNA could trigger drug resistance with the emergence of HCV strains able to infect cells with negligible levels of the microRNA. This information could be used for more effective dosing of drugs targeting this gene, as well as for pre-treatment analysis to determine which patients may respond best to this class of drugs.
“This effort, which was made possible by innovative microRNA analysis, offers significant progress toward precision medicine in treating HCV patients,” said Matthew Evans, PhD, Assistant Professor of microbiology at the Icahn School of Medicine at Mount Sinai and a co-author of the study. “There is a critical need for more weapons in our arsenal to fight HCV — particularly for affordable, effective treatment as we try to stay a step ahead of this virus and prevent it from developing the kind of drug resistance we’re seeing in the bacterial realm.”
In another key finding, the scientists uncovered knowledge that may help answer the longstanding question of how HCV leads to cancer. The study demonstrated that HCV hijacks the microRNA gene, diminishing its normal activity in liver cells. Since this microRNA is known to be a potent tumor repressor, it is possible that HCV robs cells of their natural defenses against uncontrolled growth. Such an outcome could contribute to cancers that arise from chronic HCV infection.
“Our study offers broader implications for this class of microRNA genes and their interaction with targets, which may be useful for a number of diseases in addition to hepatitis C,” said Brian Brown, PhD, Associate Professor of Genetics and Genomic Sciences at the Icahn School of Medicine at Mount Sinai and a co-author of the study. “We are also intrigued by this new information that may shed light on the link between HCV and the onset of cancer and look forward to future efforts to explore this theory.”
Paper cited:
Benjamin Israelow, Gavriel Mullokandov, Judith Agudo, Marion Sourisseau, Ali Bashir,
Andres Y. Maldonado, Arvin C. Dar, Brian D. Brown & Matthew J. Evans. “Hepatitis C virus genetics affects miR-122 requirements and response to miR-122 inhibitors.” Nature Communications. DOI: 10.1038/ncomms6408.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
New RNA-based Therapy Combats Melanoma in Mouse Models
Jul 27, 2023 View All Press Releases
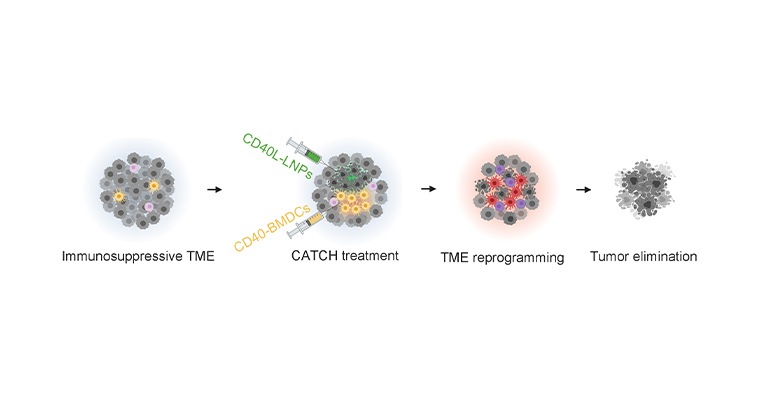
Targeting One Type of Immune Cell With Another Slows Cancer Growth in Preclinical Studies
Oct 25, 2022 View All Press Releases
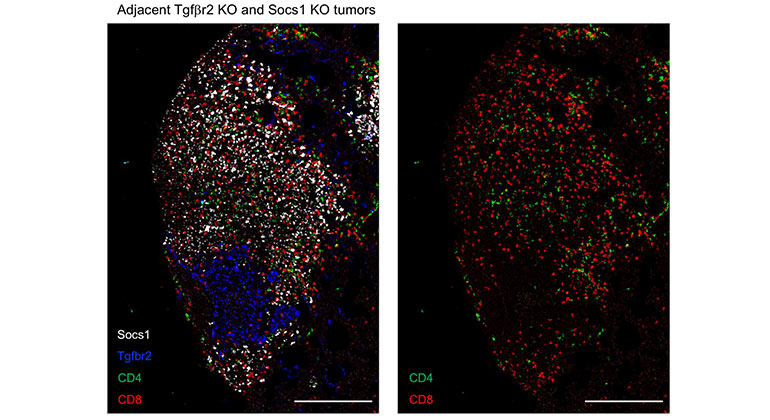
Novel CRISPR Imaging Technology Reveals Genes Controlling Tumor Immunity
Mar 15, 2022 View All Press ReleasesMount Sinai Researchers: Why COVID-19 May Be Less Common in Children Than Adults
May 22, 2020 View All Press ReleasesAirway Microbiome and Host Interact Differently in Children with Severe Asthma
Mar 12, 2020 View All Press Releases