Tapeworm infection - Hymenolepsis
Hymenolepiasis; Dwarf tapeworm infection; Rat tapeworm; Tapeworm - infection
Hymenolepis infection is an infestation by one of two species of tapeworm: Hymenolepis nana or Hymenolepis diminuta. The disease is also called hymenolepiasis.
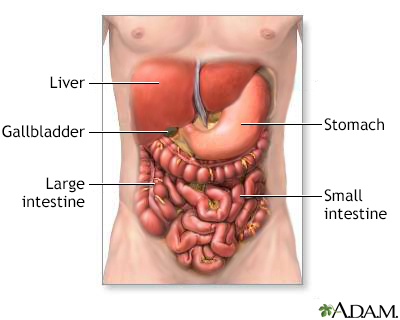
The digestive system organs in the abdominal cavity include the liver, gallbladder, stomach, small intestine and large intestine.
Causes
Hymenolepis worms live in warm climates and are common in the southern United States. Insects eat the eggs of these worms.
Humans and other animals become infected when they eat material contaminated by insects (including fleas associated with rats). In an infected person, it is possible for the worm's entire life cycle to be completed in the bowel, so infection can last for years.
Hymenolepis nana infections are much more common than Hymenolepis diminuta infections in humans. These infections used to be common in the southeastern United States, in crowded environments, and in people who were confined to institutions. However, the disease occurs throughout the world.
Symptoms
Symptoms occur only with heavy infections. Symptoms include:
- Diarrhea
- Gastrointestinal discomfort
- Itchy anus
- Poor appetite
- Weakness
Exams and Tests
A stool exam for the tapeworm and its eggs confirms the diagnosis.
Treatment
The treatment for this condition is a single dose of praziquantel, repeated in 10 days.
Household members may also need to be screened and treated because the infection can be spread easily from person to person.
Outlook (Prognosis)
Expect full recovery following treatment.
Possible Complications
Health problems that may result from this infection include:
- Abdominal discomfort
- Dehydration from prolonged diarrhea
When to Contact a Medical Professional
Contact your health care provider if you have chronic diarrhea or abdominal cramping.
Prevention
Good hygiene, public health and sanitation programs, and elimination of rats help prevent the spread of hymenolepiasis.
References
Alroy KA, Gilman RH. Tapeworm infections. In: Ryan ET, Hill DR, Solomon T, Aronson NE, Endy TP, eds. Hunter's Tropical Medicine and Emerging Infectious Disease. 10th ed. Philadelphia, PA: Elsevier; 2020:chap 130.
White AC, Brunetti E. Cestodes. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 325.
Version Info
Last reviewed on: 8/26/2023
Reviewed by: Jatin M. Vyas, MD, PhD, Associate Professor in Medicine, Harvard Medical School; Associate in Medicine, Division of Infectious Disease, Department of Medicine, Massachusetts General Hospital, Boston, MA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
