Eosinophil count - absolute
Eosinophils; Absolute eosinophil count
An absolute eosinophil count is a blood test that measures the number of one type of white blood cells called eosinophils. Eosinophils become active when you have certain allergic diseases, infections, and other medical conditions.
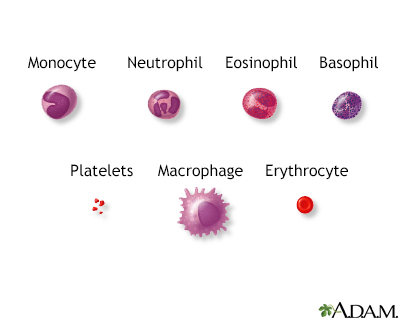
Blood is comprised of red blood cells, platelets, and various white blood cells.
How the Test is Performed
Most of the time, blood is drawn from a vein on the inside of the elbow or the back of the hand. The site is cleaned with an antiseptic. The health care provider wraps an elastic band around your upper arm to make the vein swell with blood.
Next, the provider gently inserts a needle into the vein. The blood collects into an airtight tube attached to the needle. The elastic band is removed from your arm. The needle is then removed and the site is covered to stop bleeding.
In infants or young children, a sharp tool called a lancet may be used to prick the skin. The blood collects in a small glass tube, or onto a slide or test strip. A bandage is put on the spot to stop bleeding.
In the lab, the blood is placed on a microscope slide. A stain is added to the sample. This causes eosinophils to show up as orange-red granules. The technician then counts how many eosinophils are present per 100 cells. The percentage of eosinophils is multiplied by the white blood cell count to give the absolute eosinophil count.
How to Prepare for the Test
Most of the time, adults do not need to take special steps before this test. Tell your provider the medicines you are taking, including the ones without a prescription. Some drugs may change the test results.
Medicines that may cause you to have an increase in eosinophils include:
- Amphetamines (appetite suppressants)
- Certain laxatives containing psyllium
- Certain antibiotics
- Interferon
- Tranquilizers
How the Test will Feel
You may feel slight pain or a sting when the needle is inserted. You may also feel some throbbing at the site after the blood is drawn.
Why the Test is Performed
You will have this test to see if you have abnormal results from a blood differential test. This test may also be done if the provider thinks you may have a specific disease.
This test may help diagnose:
- Acute hypereosinophilic syndrome (a rare, but sometimes fatal leukemia-like condition)
- An allergic reaction (can also reveal how severe the reaction is)
- Cancer
- Early stages of Addison disease
- Infection by a parasite
- Vasculitis
Normal Results
Normal eosinophil count is less than 500 cells per microliter (cells/mcL).
Normal value ranges may vary slightly among different laboratories. Talk to your provider about the meaning of your specific test results.
The example above shows the common measurements for results of these tests. Some laboratories use different measurements or may test different specimens.
What Abnormal Results Mean
A high number of eosinophils (eosinophilia) are often linked to a variety of disorders. A high eosinophil count may be due to:
- Adrenal gland deficiency
- Allergic disease, including hay fever
- Asthma
- Autoimmune diseases
- Eczema
- Fungal infections
- Hypereosinophilic syndrome
- Leukemia and other blood disorders
- Lymphoma
- Parasite infection, such as worms
A lower-than-normal eosinophil count may be due to:
- Alcohol intoxication
- Overproduction of certain steroids in the body (such as cortisol)
Risks
Risks from having blood drawn are slight, but may include:
- Excessive bleeding
- Fainting or feeling lightheaded
- Hematoma (blood accumulating under the skin)
- Infection (a slight risk any time the skin is broken)
Considerations
The eosinophil count is used to help confirm a diagnosis. The test cannot tell if the higher number of cells is caused by allergy or parasite infection.
References
Khoury P, Akuthota P, Weller PF, Klion AD. Eosinophilia and eosinophil-related disorders. In: Burks AW, Holgate ST, O' Hehir RE, Broide DH, et al. eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 73.
Klion AD. Eosinophilic syndromes. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 161.
Roberts DJ. Hematologic aspects of parasitic diseases. In: Hoffman R, Benz EJ, Silberstein LE, et al, eds. Hematology: Basic Principles and Practice. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 154.
Version Info
Last reviewed on: 1/25/2023
Reviewed by: Neil J. Gonter, MD, Assistant Professor of Medicine, Columbia University, NY and private practice specializing in Rheumatology at Rheumatology Associates of North Jersey, Teaneck, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
