Anthrax
Woolsorter's disease; Ragpicker's disease; Cutaneous anthrax; Gastrointestinal anthrax
Anthrax is an infectious disease caused by a bacterium called Bacillus anthracis. Infection in humans most often involves the skin, gastrointestinal tract, or lungs.
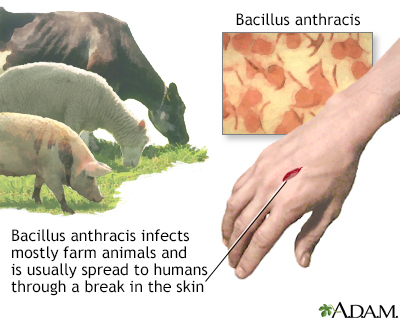
Anthrax is caused by the bacteria Bacillus anthracis. While anthrax commonly affects hoofed animals such as sheep and goats, humans may get sick from anthrax, too. The most common type of anthrax infection is cutaneous anthrax, an infection of the skin.
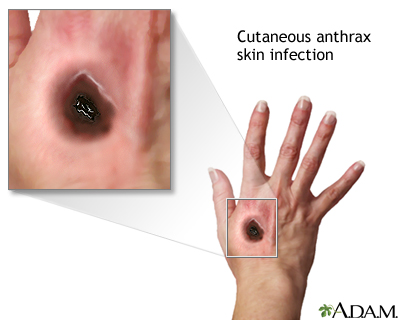
Cutaneous anthrax is an infection of the skin caused by the bacterium Bacillus anthracis. The bacteria causes disease when it comes into contact with non-intact skin. During an infection, an initial skin lesion forms then blisters. The blister breaks down into a black ulcer and nearby lymph nodes may become infected and painful. A scar is often formed which then dries and falls off within two weeks. In 20% of untreated individuals, the infection may spread to the bloodstream and become fatal. Although with proper treatment, death is extremely rare.
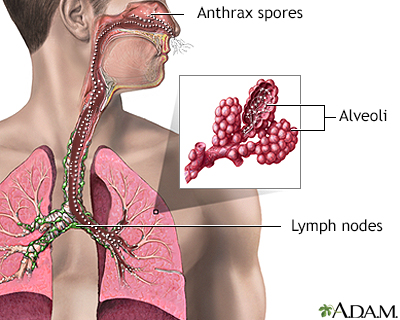
Inhaled anthrax is particularly deadly. Although the spores are dormant when breathed in, they germinate when exposed to a warm, moist environment, such as the lungs. Not all particles are small enough to pass into the alveoli, or air sacs, but those that do begin to multiply and may spread to the lymphatic system. When the spores germinate in the lymph nodes, several toxins are released. Particles illustrated are not to scale.
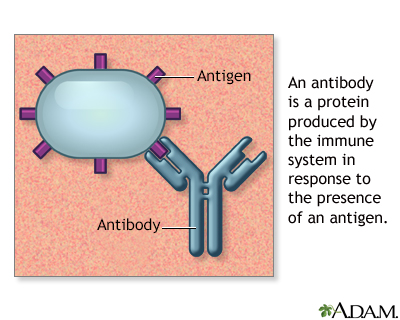
Antigens are large molecules (usually proteins) on the surface of cells, viruses, fungi, bacteria, and some non-living substances such as toxins, chemicals, drugs, and foreign particles. The immune system recognizes antigens and produces antibodies that destroy substances containing antigens.
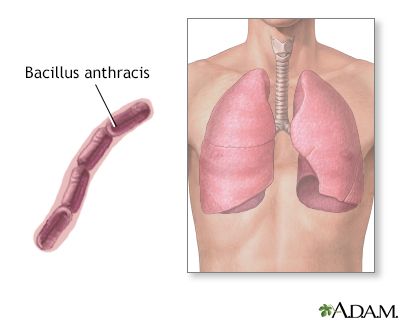
Bacillus anthracis is an aerobic spore-forming bacterium that causes disease in humans and animals. The bacteria is found in two forms cutaneous anthrax and inhalation anthrax. Cutaneous anthrax is an infection of the skin caused by direct contact with the bacterium. Inhalation or respiratory anthrax is an infectious disease caused by inhaling the spores of the bacterium. While anthrax commonly affects hoofed animals such as sheep and goats, humans may acquire this disease as well. Anthrax is a potential agent for use as a biological weapon or bio-terrorism.
Causes
Anthrax commonly affects hoofed animals such as sheep, cattle, and goats. Humans who come into contact with infected animals can get sick with anthrax as well.
There are three main routes of anthrax infection: skin (cutaneous), lung (inhalation), and mouth (gastrointestinal).
Cutaneous anthrax occurs when anthrax spores enter the body through a cut or scrape on the skin.
- It is the most common type of anthrax infection.
- The main risk is contact with animal hides or hair, bone products, and wool, or with infected animals. People most at risk for cutaneous anthrax include farm workers, veterinarians, tanners, and wool workers.
Inhalation anthrax develops when anthrax spores enter the lungs through the airways. It is most commonly contracted when workers breathe in airborne anthrax spores during processes such as tanning hides and processing wool.
Breathing in spores means a person has been exposed to anthrax. But it does not mean the person will have symptoms.
- The bacterial spores must germinate or sprout (the same way a seed sprouts before a plant grows) before the actual disease occurs. This process usually takes 1 to 6 days.
- Once the spores germinate, they release several toxic substances. These substances cause internal bleeding, swelling, and tissue death.
Gastrointestinal anthrax occurs when someone eats anthrax-tainted meat.
Injection anthrax can occur in someone who self-injects drugs (heroin).
Anthrax may be used as a biological weapon or for bioterrorism.
Symptoms
Symptoms of anthrax differ, depending on the type of anthrax.
Symptoms of cutaneous anthrax start 1 to 7 days after exposure:
- An itchy sore develops that is similar to an insect bite. This sore may blister and form a black ulcer (sore or eschar).
- The sore is usually painless, but it is often surrounded by swelling.
- A scab often forms, and then dries and falls off within 2 weeks. Complete healing can take longer.
Symptoms of inhalation anthrax:
- Begins with fever, malaise, headache, cough, shortness of breath, and chest pain
- Fever and shock may occur later
Symptoms of gastrointestinal anthrax usually occur within 1 week and may include:
- Abdominal pain
- Bloody diarrhea
- Diarrhea
- Fever
- Mouth sores
- Nausea and vomiting (the vomit may contain blood)
Symptoms of injection anthrax are similar to those of cutaneous anthrax. In addition, the skin or muscle beneath the injection site may get infected.
Exams and Tests
Your health care provider will perform a physical examination.
The tests to diagnose anthrax depend on the type of disease that is suspected.
A culture of the skin, and sometimes a biopsy, are done on the skin sores. The sample is looked at under a microscope to identify the anthrax bacterium.
Tests may include:
- Blood culture
- Chest CT scan or chest x-ray
- Spinal tap to check for infection around the spinal column
- Sputum culture
- Complete blood count
- Blood chemistries
More tests may be done on fluid or blood samples.
Treatment
Antibiotics are usually used to treat anthrax. Antibiotics that may be prescribed include penicillin, doxycycline, and ciprofloxacin.
Inhalation anthrax is treated with a combination of antibiotics such as ciprofloxacin plus another medicine. They are given by IV (intravenously). Antibiotics are usually taken for 60 days because it can take spores that long to germinate.
Cutaneous anthrax is treated with antibiotics taken by mouth, usually for 7 to 10 days. Doxycycline and ciprofloxacin are most often used.
Outlook (Prognosis)
When treated with antibiotics, cutaneous anthrax is likely to get better. But some people who do not get treated may die if anthrax spreads to the blood.
People with second-stage inhalation anthrax have a poor outlook, even with antibiotic therapy. Many cases in the second stage are fatal.
Gastrointestinal anthrax infection can spread to the bloodstream and may result in death.
When to Contact a Medical Professional
Contact your provider if you think you have been exposed to anthrax or if you develop symptoms of any type of anthrax.
Prevention
There are two main ways to prevent anthrax:
- For people who have been exposed to anthrax (but have no symptoms of the disease), providers may prescribe preventive antibiotics, such as ciprofloxacin, penicillin, or doxycycline, depending on the strain of anthrax.
- An anthrax vaccine is available to military personnel and some members of the general public. It is given in a series of 5 doses over 18 months.
There is no known way to spread cutaneous anthrax from person to person. People who live with someone who has cutaneous anthrax do not need antibiotics unless they have also been exposed to the same source of anthrax.
References
Centers for Disease Control and Prevention website. What is anthrax?
Kortepeter MG, Cieslak TJ. Bioterrorism. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 19.
Martin GJ, Friedlander AM. Bacillus anthracis (anthrax). In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 207.
Version Info
Last reviewed on: 5/19/2023
Reviewed by: Jatin M. Vyas, MD, PhD, Associate Professor in Medicine, Harvard Medical School; Associate in Medicine, Division of Infectious Disease, Department of Medicine, Massachusetts General Hospital, Boston, MA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
