Salivary gland infections
Parotitis; Sialadenitis
Salivary gland infections affect the glands that produce spit (saliva). The infection may be due to bacteria or viruses.
There are 3 pairs of major salivary glands:
- Parotid glands -- These are the two largest glands. One is located in each cheek over the jaw in front of the ears. Inflammation of one or more of these glands is called parotitis, or parotiditis.
- Submandibular glands -- These two glands are located just under both sides of the lower jaw and carry saliva up to the floor of the mouth under the tongue.
- Sublingual glands -- These two glands are located just under the front most area of the floor of the mouth.
All of the salivary glands empty saliva into the mouth. The saliva enters the mouth through ducts that open into the mouth in different places.
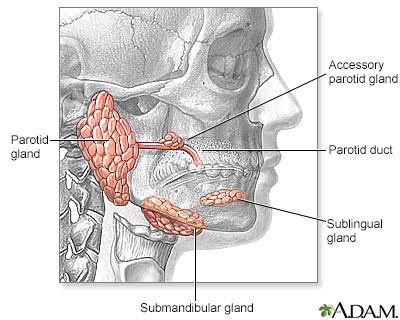
There are several pairs of salivary glands in different locations a major pair in front of the ears (parotid glands); two major pairs on the floor of the mouth (sublingual and submaxillary glands); and several minor pairs within the lips, cheeks, and tongue.
Causes
Salivary gland infections are somewhat common, and they can return in some people.
Viral infections, such as mumps, often affect the salivary glands. (Mumps most often involves the parotid salivary gland). There are fewer cases today because of the widespread use of the MMR vaccine.
Bacterial infections are most often the result of a:
- Blockage from salivary duct stones
- Poor cleanliness in the mouth (oral hygiene)
- Low amounts of water in the body, most often while in the hospital
- Smoking
- Chronic illness
- Autoimmune diseases
Symptoms
Symptoms include:
- Abnormal tastes, foul tastes
- Decreased ability to open the mouth
- Dry mouth
- Fever
- Mouth or facial "squeezing" pain, especially when eating
- Redness over the side of the face or the upper neck
- Swelling of the face (particularly in front of the ears, below the jaw, or on the floor of the mouth)
Exams and Tests
Your health care provider or dentist will do an exam to look for enlarged glands. You may also have pus that drains into the mouth. The gland is often painful.
A CT scan, MRI scan, or ultrasound may be done if the provider suspects an abscess, or to look for stones.
Your provider may suggest a mumps blood test if multiple glands are involved.
A bacterial culture can help identify the organism causing the problem.
Treatment
In some cases, no treatment is needed.
Treatment from your provider may include:
- Antibiotics if you have a fever or pus drainage, or if the infection is caused by bacteria. Antibiotics are not useful against viral infections.
- Surgery or aspiration to drain an abscess if you have one.
- A technique called sialendoscopy uses a very small camera and instruments to diagnose and treat infections and other problems in the salivary glands.
Self-care steps you can take at home to help with recovery include:
- Practice good oral hygiene. Brush your teeth and floss well at least twice a day. This may help with healing and prevent an infection from spreading.
- Rinse your mouth with warm salt water rinses (one half teaspoon or 3 grams of salt in 1 cup or 240 milliliters of water) to ease pain and keep the mouth moist.
- To speed up healing, stop smoking if you are a smoker.
- Drink lots of water and use sugar-free lemon drops to increase the flow of saliva and reduce swelling.
- Massaging the gland with heat.
- Using warm compresses on the inflamed gland.
Outlook (Prognosis)
Most salivary gland infections go away on their own or are cured with treatment. Some infections will return. Complications are not common.
Possible Complications
Complications may include:
- Abscess of salivary gland
- Return of infection
- Spread of infection (cellulitis, Ludwig angina)
When to Contact a Medical Professional
Contact your provider if you have:
- Symptoms of a salivary gland infection
- Salivary gland infection and symptoms get worse
Get medical help right away if you have:
- High fever
- Trouble breathing
- Swallowing problems
Prevention
In many cases, salivary gland infections can't be prevented. Good oral hygiene may prevent some cases of bacterial infection.
References
Elluru RG. Physiology of the salivary glands. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 81.
Jackson NM, Mitchell JL, Walvekar RR. Inflammatory disorders of the salivary glands. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 83.
Version Info
Last reviewed on: 9/10/2023
Reviewed by: Josef Shargorodsky, MD, MPH, Johns Hopkins University School of Medicine, Baltimore, MD. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
