Multiple sclerosis
MS; Demyelinating disease
Multiple sclerosis (MS) is an autoimmune disease that affects the brain and spinal cord (central nervous system).
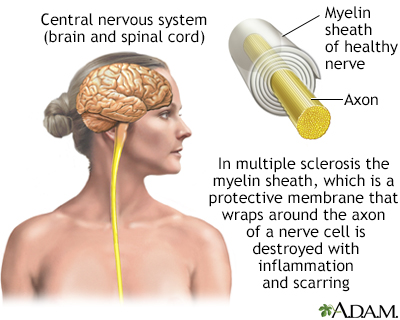
Multiple sclerosis is a central nervous system disorder marked by decreased nerve function with initial inflammation of the protective myelin nerve covering and eventual scarring. Symptoms and severity of symptoms vary widely and may progress into episodes of crisis alternating with episodes of remission.
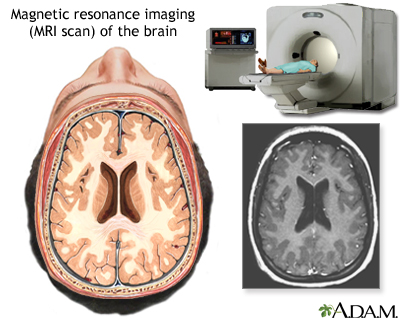
An MRI (magnetic resonance imaging) of the brain creates a detailed image of the complex structures in the brain. An MRI can give a three-dimensional depiction of the brain, making location of problems such as tumors or aneuryms more precise.
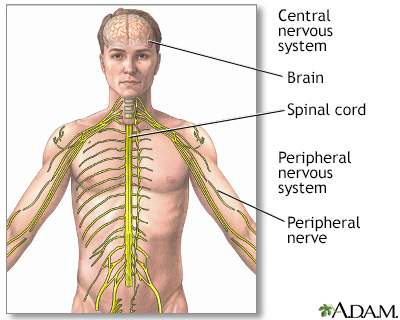
The central nervous system comprises the brain and spinal cord. The peripheral nervous system includes all peripheral nerves.
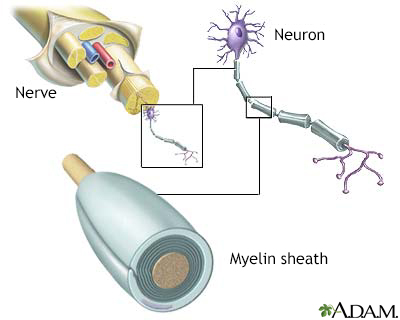
Myelin is the layer that forms around nerve cells. Its purpose is to speed the transmission of impulses along nerve cells.
Causes
MS affects women more often than men. The disorder is most commonly diagnosed between ages 30 to 40, but it can be seen at any age.
MS is caused by damage to the myelin sheath. This sheath is the protective covering that surrounds nerve cells. When this nerve covering is damaged, nerve signals slow or stop.
The nerve damage is caused by inflammation. Inflammation occurs when the body's immune cells attack the nervous system. This can occur along any area of the brain, optic nerve, and spinal cord.
It is unknown what exactly causes MS. The most common thought is that it is caused by a virus, a gene defect, or both. Environmental factors may also play a role.
You are slightly more likely to develop this condition if you have a family history of MS or you live in a part of the world where MS is more common (areas further from the equator).
Multiple sclerosis can be a particularly debilitating disorder because your body essentially attacks itself. But you can learn to cope during attacks. So, what causes multiple sclerosis? Multiple sclerosis, or MS, is a disease in which your body's immune system eats away at the protective sheath that covers your nerves. The disorder disrupts communication between your brain and the rest of your body, meaning your nerve signals slow down or stop. We don't know exactly why this happens. The most common thought is that a virus or gene defect, or both, are to blame. Environmental factors may even play a role. We do know that the disorder affects more women than men, that you may get the disorder if you have a family history of MS, and that you are at higher risk if you live in a part of the world where MS is more common. It's typically diagnosed between the ages of 20 and 40, but we see the disorder at any age. Now you may ask, how do you know you have multiple sclerosis? Symptoms of MS can vary widely from person to person because the location and severity of each attack can be different. Episodes may last for days, weeks, or months. You may even have long periods where you have no symptoms. We call this remission. Because MS may damage nerves in any part of the brain or spinal cord, you may have symptoms in many parts of the body. You may have muscle problems, including loss of balance, muscle spasms, numbness, trouble moving your arms or legs, even trouble walking. You may have bowel and bladder problems, such as constipation, trouble urinating, or a frequent urge to urinate. You may have double vision, eye pain, or uncontrolled eye movements. You will probably be tired a lot, and it's often worse in the late afternoon. And those are just a few of the many possible symptoms of MS. Since symptoms of MS may mimic those of other nervous system disorders, your doctor will want to rule those out. Your doctor may suspect MS if you have trouble with two different parts of your central nervous system (such as abnormal reflexes) at two different times. A neurological exam may show you have reduced function in one area of your body, or it may be spread over many parts of your body. You may have abnormal reflexes, decreased ability to move a part of your body, a loss of sensation. An eye exam might show abnormal pupil responses, changes in your visual field, or trouble seeing. There is no known cure for MS, so your doctor will focus on therapies to slow down the disorder, to control your symptoms and help you maintain a normal quality of life. Your doctor can prescribe different medicines to help with this. You may have to take several medications. Life expectancy with MS can be normal, or almost normal. Most people with MS continue to walk and function at work with minimal disability for 20 or more years. The amount of disability and discomfort can depend on how often you have attacks, on how bad they are, and what part of the central nervous system is affected by each attack. Most people return to normal or near-normal function between attacks. But, over time, many people with MS will need a wheelchair. To help you maintain a normal quality of life, your doctor may suggest physical therapy, speech therapy, occupational therapy, and support groups, depending on your needs. Starting an exercising program early in the course of your disorder, eating right, and getting enough rest can also help.
Symptoms
Symptoms vary because the location and severity of each attack can be different. Attacks can last for days, weeks, or months. Attacks are followed by remissions. These are periods of reduced symptoms or no symptoms. Fever, hot baths, sun exposure, and stress can trigger or worsen attacks.
Nerves in any part of the brain or spinal cord may be damaged. Because of this, MS symptoms can appear in many parts of the body.
Muscle symptoms:
- Loss of balance
- Muscle spasms
- Numbness or abnormal sensation in any area
- Problems moving arms or legs
- Problems walking
- Problems with coordination and making small movements
- Tremor in one or more arms or legs
- Weakness in one or more arms or legs
Bowel and bladder symptoms:
- Constipation and stool leakage
- Difficulty beginning to urinate
- Frequent need to urinate
- Strong urge to urinate
- Urine leakage (incontinence)
Eye symptoms:
- Double vision
- Eye discomfort
- Uncontrollable eye movements
- Vision loss (usually affects one eye at a time)
Numbness, tingling, or pain:
- Facial pain
- Painful muscle spasms
- Tingling, crawling, or burning feeling in the arms and legs
Other brain and nerve symptoms:
- Decreased attention span, poor judgment, and memory loss
- Difficulty reasoning and solving problems
- Depression or feelings of sadness
- Dizziness and balance problems
- Hearing loss
Sexual symptoms:
- Problems with erections
- Problems with vaginal lubrication
Speech and swallowing symptoms:
- Slurred or difficult-to-understand speech
- Trouble chewing and swallowing
Fatigue is a common and bothersome symptom as MS progresses. It is often worse in the late afternoon.
Exams and Tests
Symptoms of MS may mimic those of many other nervous system problems. MS is diagnosed by determining if there are signs of more than one attack on the brain or spinal cord and by ruling out other conditions.
People who have a form of MS called relapsing-remitting MS have evidence of at least two attacks separated by a remission.
In other people, the disease may slowly get worse in between clear attacks. This form is called secondary progressive MS. A form with gradual progression, but no clear attacks is called primary progressive MS.
Your health care provider may suspect MS if there are decreases in the function of two different parts of the central nervous system (such as abnormal reflexes) at two different times.
An exam of the nervous system may show reduced nerve function in one area of the body. Or the reduced nerve function may be spread over many parts of the body. This may include:
- Abnormal nerve reflexes
- Decreased ability to move a part of the body
- Decreased or abnormal sensation
- Other loss of nervous system functions, such as vision
An eye exam may show:
- Abnormal pupil responses
- Changes in the visual fields
- Changes in eye movements
- Damage to the nerve in the eye (optic nerve atrophy)
- Decreased visual acuity
- Problems with the inside parts of the eye
- Rapid eye movements triggered when the eye moves
Tests to diagnose MS include:
- Blood tests to check for other conditions that are similar to MS.
- Lumbar puncture (spinal tap) for cerebrospinal fluid (CSF) tests, including CSF oligoclonal banding may be needed.
- MRI scan of the brain or the spine, or both are important to help diagnose and follow MS.
- Nerve function study (evoked potential test, such as visual evoked response) is less often used.
Treatment
There is no known cure for MS at this time, but there are treatments that may slow the disease. The goal of treatment is to stop progression, control symptoms, and help you maintain a normal quality of life.
Medicines are often taken long-term. These include:
- Medicines to slow the disease
- Steroids to decrease the severity of attacks
- Medicines to control symptoms such as muscle spasms, urinary problems, fatigue, or mood problems
Medicines are more effective for the relapsing-remitting form than for other forms of MS.
The following may also be helpful for people with MS:
- Physical therapy, speech therapy, occupational therapy, and support groups
- Assistive devices, such as wheelchairs, bed lifts, shower chairs, walkers, and wall bars
- A planned exercise program early in the course of the disorder
- A healthy lifestyle, with good nutrition and enough rest and relaxation
- Avoiding fatigue, stress, temperature extremes, and illness
- Changes in what you eat or drink if there are swallowing problems
- Making changes around the home to prevent falls
- Social workers or other counseling services to help you cope with the disorder and get assistance
- Vitamin D or other supplements (talk to your provider first)
- Complementary and alternative approaches, such as acupuncture or cannabis, to help with muscle problems
- Spinal devices can reduce pain and spasticity in the legs
Support Groups
Living with MS may be a challenge. You can ease the stress of illness by joining an MS support group. Sharing with others who have common experiences and problems can help you not feel alone.
Outlook (Prognosis)
The outcome varies, and is hard to predict. Although the disorder is life-long (chronic) and incurable, life expectancy can be normal or almost normal. Most people with MS are active and function at work with little disability.
Those who usually have the best outlook are:
- Females
- People who were young (less than 30 years old) when the disease started
- People with infrequent attacks
- People with a relapsing-remitting pattern
- People who have limited disease on imaging studies
The amount of disability and discomfort depends on:
- How often and severe the attacks are
- The part of the central nervous system that is affected by each attack
Most people return to normal or near-normal function between attacks. Over time, there is greater loss of function with less improvement between attacks.
Possible Complications
MS may lead to the following:
- Depression
- Difficulty swallowing
- Difficulty thinking
- Less and less ability to care for self
- Need for indwelling urinary catheter
- Osteoporosis or thinning of the bones
- Pressure sores
- Side effects of medicines used to treat the disorder
- Urinary tract infections
When to Contact a Medical Professional
Contact your provider if:
- You develop any symptoms of MS
- Your symptoms get worse, even with treatment
- The condition worsens to the point when home care is no longer possible
References
Calabresi PA, Multiple sclerosis and demyelinating conditions of the central nervous system. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 380.
Fabian MT, Krieger SC, Lublin FD. Multiple sclerosis and other inflammatory demyelinating diseases of the central nervous system. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 80.
Rae-Grant A, Day GS, Marrie RA, et al. Practice guideline recommendations summary: disease-modifying therapies for adults with multiple sclerosis: report of the Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology. Neurology. 2018;90(17):777-788. PMID: 29686116
Version Info
Last reviewed on: 1/23/2022
Reviewed by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Internal review and update on 02/23/24 by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
